Abstract
Background
There is no consensus on the necessity of endoscopic sphincterotomy (ES) to prevent post-endoscopic retrograde cholangiopancreatography pancreatitis (PEP) after endoscopic stenting in patients with malignant biliary obstruction. We investigated the incidence of PEP after endoscopic biliary stenting for malignant biliary obstruction with or without ES in a multicenter prospective cohort study.
Methods
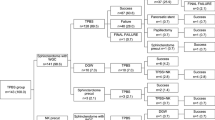
We enrolled 807 patients who underwent endoscopic biliary stenting for malignant biliary obstruction with a native papilla at 36 hospitals between April 2017 and March 2018. The incidence of PEP in patients with or without ES was compared for subgroups based on stent type, placement method, and patient background. Univariate and multivariate analysis was performed to investigate the incidence of PEP in all stenting patients.
Results
Plastic and metal stents (MS) were inserted in 598 and 209 patients, respectively. The incidence of PEP in patients with or without ES was 7.9% and 7.4%, respectively among all stenting patients. The incidences of PEP with or without ES in plastic stent insertion patients, patients with MS insertion, stent insertions across the papilla, stent insertions across the papilla in patients without main pancreatic duct obstruction, and fully covered MS insertions across the papilla were compared. There was no overall significant difference in the incidence of PEP between those with or without ES. Multivariate logistic regression analysis for the incidence of PEP in all stenting patients revealed obstruction of the main pancreatic duct at the pancreatic head and epinephrine spraying on the papilla were significant factors; there was no significant difference in the incidence of PEP between patients with or without ES.
Conclusion
Endoscopic sphincterotomy may not contribute to the prevention of PEP after endoscopic biliary stenting for malignant biliary obstruction, even in cases of insertion with a fully covered MS across the papilla.


Similar content being viewed by others
References
Simmons DT, Petersen BT, Gostout CJ, Levy MJ, Topazian MD, Baron TH (2008) Risk of pancreatitis following endoscopically placed large-bore plastic biliary stents with and without biliary sphincterotomy for management of postoperative bile leaks. Surg Endosc 22:1459–1463. https://doi.org/10.1007/s00464-007-9643-8
Tarnasky PR, Cunningham JT, Hawes RH, Hoffman BJ, Uflacker R, Vujic I, Cotton PB (1997) Transpapillary stenting of proximal biliary strictures: Does biliary sphincterotomy reduce the risk of postprocedure pancreatitis? Gastrointest Endosc 45:46–51. https://doi.org/10.1016/S0016-5107(97)70301-8
Kato S, Kuwatani M, Hayashi T, Eto K, Ono M, Ehira N, Yamato H, Sano I, Taya Y, Onodera M, Kubo K, Ihara H, Yamazaki H, Sakamoto N (2020) Inutility of endoscopic sphincterotomy to prevent pancreatitis after biliary metal stent placement in the patients without pancreatic duct obstruction. Scand J Gastroenterol 55:503–508. https://doi.org/10.1080/00365521.2020.1749879
Dumonceau JM, Kapral C, Aabakken L, Papanikolaou IS, Tringali A, Vanbiervliet G, Beyna T, Dinis-Ribeiro M, Hritz I, Mariani A, Paspatis G, Radaelli F, Lakhtakia S, Veitch AM, Van Hooft JE (2020) ERCP-related adverse events: European society of gastrointestinal endoscopy (ESGE) guideline. Endoscopy 52:127–149. https://doi.org/10.1055/a-1075-4080
Martins FP, Kahaleh M, Ferrari AP (2015) Management of liver transplantation biliary stricture: Results from a tertiary hospital. World J Gastrointest Endosc 7:747. https://doi.org/10.4253/wjge.v7.i7.747
Kato S, Kuwatani M, Onodera M, Kudo T, Sano I, Katanuma A, Uebayashi M, Eto K, Fukasawa M, Hashigo S, Iwashita T, Yoshida M, Taya Y, Kawakami H, Kato H, Nakai Y, Kobashigawa K, Kawahata S, Shinoura S, Ito K, Kubo K, Yamato H, Hara K, Maetani I, Mukai T, Shibukawa G, Itoi T (2021) Risk of pancreatitis following biliary stenting with/without endoscopic sphincterotomy: A randomized controlled trial. Clin Gastroenterol Hepatol 20:P1394-1403. https://doi.org/10.1016/j.cgh.2021.08.016
Zhou H, Li L, Zhu F, Luo SZ, Cai XB, Wan XJ (2012) Endoscopic sphincterotomy associated cholangitis in patients receiving proximal biliary self-expanding metal stents. Hepatobiliary Pancreat Dis Int 11:643–649. https://doi.org/10.1016/S1499-3872(12)60238-0
Cui PJ, Yao J, Zhao YJ, Han HZ, Yang J (2014) Biliary stenting with or without sphincterotomy for malignant biliary obstruction: A meta-analysis. World J Gastroenterol 20:14033–14039. https://doi.org/10.3748/WJG.V20.I38.14033
Di Giorgio P, De Luca L, Rivellini G, Cassandro R, Lizza M, De Luca B (2000) A comparison of the outcomes of treatments with plastic stent (PS) with and without endoscopic sphincterotomy (ES) for inoperable malignant common bile duct obstruction. Dig Liver Dis 32:A61. https://doi.org/10.1016/s1590-8658(00)80422-3
Margulies C, Siqueira ES, Silverman WB, Lin XS, Martin JA, Rabinovitz M, Slivka A (1999) The effect of endoscopic sphincterotomy on acute and chronic complications of biliary endoprostheses. Gastrointest Endosc 49:716–719. https://doi.org/10.1016/S0016-5107(99)70288-9
Nakahara K, Okuse C, Suetani K, Michikawa Y, Kobayashi S, Otsubo T, Itoh F (2013) Covered metal stenting for malignant lower biliary stricture with pancreatic duct obstruction: Is endoscopic sphincterotomy needed? Gastroenterol Res Pract 2013:12–15. https://doi.org/10.1155/2013/375613
Hayashi T, Kawakami H, Osanai M, Ishiwatari H, Naruse H, Hisai H, Yanagawa N, Kaneto H, Koizumi K, Sakurai T, Sonoda T (2015) No benefit of endoscopic sphincterotomy before biliary placement of self-expandable metal stents for unresectable pancreatic cancer. Clin Gastroenterol Hepatol 13:1151-1158.e2. https://doi.org/10.1016/j.cgh.2015.01.008
Artifon ELA, Sakai P, Ishioka S, Marques SB, Lino AS, Cunha JEM, Jukemura J, Cecconello I, Carrilho FJ, Opitz E, Kumar A (2008) Endoscopic sphincterotomy before deployment of covered metal stent is associated with greater complication rate: A prospective randomized control trial. J Clin Gastroenterol 42:815–819. https://doi.org/10.1097/MCG.0b013e31803dcd8a
Shimizu S, Naitoh I, Nakazawa T, Hayashi K, Miyabe K, Kondo H, Yoshida M, Yamashita H, Umemura S, Hori Y, Ohara H, Joh T (2013) Predictive factors for pancreatitis and cholecystitis in endoscopic covered metal stenting for distal malignant biliary obstruction. J Gastroenterol Hepatol 28:68–72. https://doi.org/10.1111/j.1440-1746.2012.07283.x
Andriulli A, Loperfido S, Napolitano G, Niro G, Valvano MR, Spirito F, Pilotto A, Forlano R (2007) Incidence rates of post-ERCP complications: A systematic survey of prospective studies. Am J Gastroenterol 102:1781–1788. https://doi.org/10.1111/j.1572-0241.2007.01279.x
Fujita K, Yazumi S, Matsumoto H, Asada M, Nebiki H, Matsumoto K, Maruo T, Takenaka M, Tomoda T, Onoyama T, Kurita A, Ueki T, Katayama T, Kawamura T, Kawamoto H (2021) Multicenter prospective cohort study of adverse events associated with biliary ERCP; Incidence of adverse events and preventive measures for post-endoscopic retrogrde cholangiopancreatography pancreatitis. Dig Endosc 34:1198–1204. https://doi.org/10.1111/den.14225
Cotton PB, Eisen GM, Aabakken L, Baron TH, Hutter MM, Jacobson BC, Mergener K, Nemcek A, Petersen BT, Petrini JL, Pike IM, Rabeneck L, Romagnuolo J, Vargo JJ (2010) A lexicon for endoscopic adverse events: Report of an ASGE workshop. Gastrointest Endosc 71:446–454. https://doi.org/10.1016/j.gie.2009.10.027
Matsushita M, Takakuwa H, Shimeno N, Uchida K, Nishio A, Okazaki K (2009) Epinephrine sprayed on the papilla for prevention of post-ERCP pancreatitis. J Gastroenterol 44:71–75. https://doi.org/10.1007/s00535-008-2272-8
Isayama H, Nakai Y, Hamada T, Matsubara S, Kogure H, Koike K (2016) Understanding the mechanical forces of self-expandable metal stents in the biliary ducts. Curr Gastroenterol Rep 18:1–6. https://doi.org/10.1007/s11894-016-0538-5
Tamura T, Ogura T, Takenaka M, Tanioka K, Itonaga M, Yamao K, Kamata K, Hirono S, Okada K, Imanishi M, Higuchi K, Yamaue H, Kitano M (2020) Endoscopic sphincterotomy to prevent post-ERCP pancreatitis in patients with biliary neoplasms: A multicenter retrospective cohort study. Endosc Int Open 08:E513–E522. https://doi.org/10.1055/a-1107-2629
Elshimi E, Morad W, Elshaarawy O, Attia A (2020) Optimization of biliary drainage in inoperable distal malignant strictures. World J Gastrointest Endosc 12:285–296. https://doi.org/10.4253/wjge.v12.i9.285
Tamura T, Itonaga M, Ashida R, Yamashita Y, Hatamaru K, Kawaji Y, Emori T, Kitahata Y, Miyazawa M, Hirono S, Okada K, ichi, Kawai M, Shimokawa T, Yamaue H, Kitano M, (2021) Covered self-expandable metal stents versus plastic stents for preoperative biliary drainage in patient receiving neo-adjuvant chemotherapy for borderline resectable pancreatic cancer: Prospective randomized study. Dig Endosc 33:1170–1178. https://doi.org/10.1111/den.13926
Akshintala VS, Hutfless SM, Colantuoni E, Kim KJ, Khashab MA, Li T, Elmunzer BJ, Puhan MA, Sinha A, Kamal A, Lennon AM, Okolo PI, Palakurthy MK, Kalloo AN, Singh VK (2013) Systematic review with network meta-analysis: Pharmacological prophylaxis against post-ERCP pancreatitis. Aliment Pharmacol Ther 38:1325–1337. https://doi.org/10.1111/apt.12534
Xu LH, Qian JB, Gu LG, Qiu JW, Ge ZM, Lu F, Wang YM, Li YM, Lu HS (2011) Prevention of post-endoscopic retrograde cholangiopancreatography pancreatitis by epinephrine sprayed on the papilla. J Gastroenterol Hepatol 26:1139–1144. https://doi.org/10.1111/j.1440-1746.2011.06718.x
Sawas T, Arwani N, Al Halabi S, Vargo J (2017) Sphincterotomy with endoscopic biliary drainage for severe acute cholangitis: a meta-analysis. Endosc Int Open 05:E103–E109. https://doi.org/10.1055/s-0042-120412
Acknowledgements
We thank all patients for participating in this cohort. The collaborators in the Bilio-pancreatic Study Group of West Japan were as follows: Keiji Hanada [Onomichi General Hospital]; Akihito Okazaki [Hiroshima Atomic Bomb Survivor Hospital]; Ken Hirao [Hiroshima City Hiroshima Citizens’ Hospital]; Hideki Kamada [Kagawa University]; Chishio Noguchi [Shin Beppu Hospital]; Daisuke Goto [Tottori Red Cross Hospital]; Ichro Moriyama [Shimane University Hospital]; Yoshinori Kushiyama [Matsue Red Cross Hospital]; Hidefumi Nishikiori [Oita Sanai Medical Center]; Kazuhiro Kamada [University Hospital Kyoto Prefectural University of Medicine]; Teru Kumagi [Ehime University Hospital]; Katsuhide Tanaka [Kita-Harima Medical Center]; Nobuaki Azemoto [Shikoku Cancer Center], Chisato Ishida [Tazuke Kofukai Medical Research Institute].
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Ryoji Takada has received honoraria for manuscript writing from Medicos Hirata, and honoraria for presentations from Teijin health care, Novartis pharma, and Hisamitsu pharmaceutical co. inc outside the submitted work. Hirofumi Kawamoto has received consulting fees from Gadelius Medical, Kaneka, Piloax, and J-MIT, and honoraria for lectures from Gadelius Medical, Kaneka, and Cook outside the submitted work. Hiroko Nebiki, Koichi Fujita, Shujiro Yazumi, Mamoru Takenaka, Toru Maruo, Kazuya Matsumoto, Masanori Asada, Takaaki Eguchi, Tokuhiri Matsuoka, Satoki Yasumura, Hisakazu Matsumoto, Takashi Tamura, Saiko Marui, Kazunori Hasegawa, Akira Mitoro, Atsuhiro Masuda, Ryuki Minami, Takeshi Ogura, Noriyuki Hoki, Eiji Funatsu, Akira Kurita, Takumi Onoyama, Takeshi Tomoda, Toshiharu Ueki, Tomoaki Yamasaki, Yuhei Sakata, Toshihiro Katayama, and Takashi Kawamura have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nebiki, H., Fujita, K., Yazumi, S. et al. Does endoscopic sphincterotomy contribute to the prevention of post-endoscopic retrograde cholangiopancreatography pancreatitis after endoscopic biliary stenting for malignant biliary obstruction? A multicenter prospective cohort study. Surg Endosc 37, 3463–3470 (2023). https://doi.org/10.1007/s00464-022-09823-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09823-5