Abstract
Background
Laparoscopic liver surgery has undergone substantial advancements over the past few decades, and the key to this improvement has been an improved understanding of liver anatomy, radiologic imaging, and advancements in anesthesia and postoperative care. This study aimed to compare postoperative opioid consumption in patients receiving intrathecal morphine plus low-dose bupivacaine versus those receiving intravenous morphine.
Methods
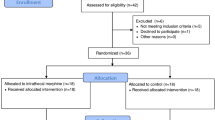
In this randomized controlled trial, 40 patients were enrolled and randomly assigned to two groups, of which one received 0.2 mg intrathecal morphine plus 0.25% Marcaine in a total volume of 4 mL and the other received intravenous morphine intraoperatively. Pain relief and patient satisfaction were evaluated using the visual analog scale. Intraoperative blood loss was measured at the end of the surgery while morphine consumption was measured by monitoring intravenous patient-controlled morphine at 12, 24, 36, and 48 h postoperatively. Treatment efficacy and complications were documented.
Results
Morphine consumption was significantly different in both groups at all time points, although the pain score did not show any difference. Shoulder pain, a common adverse effect of laparoscopic surgery, was significantly lower in the intrathecal group (25% vs. 75%). Blood loss and patient satisfaction were not different between the groups. However, the intrathecal group showed a significantly higher incidence of intraoperative hypotension.
Conclusion
Intrathecal morphine with bupivacaine can be used effectively for managing acute post-LLR pain.
Thai Clinical trial registry
TCTR20211015004.


Similar content being viewed by others
References
Reddy SK, Tsung A, Geller DA (2011) Laparoscopic liver resection. World J Surg 35:1478–1486
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS, Asbun H, OʼRourke N, Tanabe M, Koffron AJ, Tsung A, Soubrane O, Machado MA, Gayet B, Troisi RI, Pessaux P, Van Dam RM, Scatton O, Abu Hilal M, Belli G, Kwon CH, Edwin B, Choi GH, Aldrighetti LA, Cai X, Cleary S, Chen KH, Schön MR, Sugioka A, Tang CN, Herman P, Pekolj J, Chen XP, Dagher I, Jarnagin W, Yamamoto M, Strong R, Jagannath P, Lo CM, Clavien PA, Kokudo N, Barkun J, Strasberg SM, (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg. 261(4):619–29
Kehlet H (1997) Multimodal approach to control postoperative pathophysiology and rehabilitation. Br J Anaesth 78:606–617
Kehlet H, Wilmore DW (2002) Multimodal strategies to improve surgical outcome. Am J Surg 183:630–641
Savikko J, Vikatmaa L, Hiltunen AM, Mallat N, Tukiainen E, Salonen SM, Nordin A (2021) Enhanced recovery protocol in laparoscopic liver surgery. Surg Endosc 35:1058–1066
Sakowska M, Docherty E, Linscott D, Connor S (2009) A change in practice from epidural to intrathecal morphine analgesia for hepato-pancreato-biliary surgery. World J Surg 33:1802–1808
Melloul E, Hübner M, Scott M, Snowden C, Prentis J, Dejong CH, Garden OJ, Farges O, Kokudo N, Vauthey JN, Clavien PA, Demartines N (2016) guidelines for perioperative care for liver surgery: enhanced recovery after surgery (ERAS) society recommendations. World J Surg 40:2425–2440
Liu AY, Vanniyasingam T, Tidy A, Yao W, Shin D, Serrano PE, Nair S (2021) Postoperative pain after intrathecal analgesia in laparoscopic liver resection: a retrospective chart review. Minerva Anestesiol 87:856–863
Knaak C, Spies C, Schneider A, Jara M, Vorderwülbecke G, Kuhlmann AD, von Haefen C, Lachmann G, Schulte E (2020) Epidural anesthesia in liver surssgery-a propensity score-matched analysis. Pain Med 21:2650–2660
Ko JS, Choi SJ, Gwak MS, Kim GS, Ahn HJ, Kim JA, Hahm TS, Cho HS, Kim KM, Joh JW (2009) Intrathecal morphine combined with intravenous patient-controlled analgesia is an effective and safe method for immediate postoperative pain control in live liver donors. Liver Transpl 15:381–389
Nguyen M, Vandenbroucke F, Roy JD, Beaulieu D, Seal RF, Lapointe R, Dagenais M, Roy A, Massicotte L (2010) Evaluation of the addition of bupivacaine to intrathecal morphine and fentanyl for postoperative pain management in laparascopic liver resection. Reg Anesth Pain Med 35:261–266
Melloul E, Hübner M, Scott M, Snowden C, Prentis J, Dejong CHC, Garden OJ, Farges O, Kokudo N, Vauthey J-N, Clavien P-A (2016) Demartines N guidelines for perioperative care for liver surgery: enhanced recovery after surgery (ERAS) society recommendations. World J Surg. 40(10):2425–40
Beverly A, Kaye AD, Ljungqvist O, Urman RD (2017) Essential elements of multimodal analgesia in enhanced recovery after surgery (ERAS) guidelines. Anesthesiol Clin 35:e115–e143
Cook TM, Counsell D, Wildsmith JA, Project RCoATNA (2009) Major complications of central neuraxial block: report on the Third National Audit Project of the Royal College of Anaesthetists. Br J Anaesth 102:179–190
Fung AKY, Chong CCN, Lai PBS (2020) ERAS in minimally invasive hepatectomy. Ann Hepatobiliary Pancreat Surg 24:119–126
Yashpal K, Katz J, Coderre TJ (1996) Effects of preemptive or postinjury intrathecal local anesthesia on persistent nociceptive responses in rats. confounding influences of peripheral inflammation and the general anesthetic regimen. Anesthesiology 84:1119–1128
Zawar BP, Mehta Y, Juneja R, Arora D, Raizada A, Trehan N (2015) Nonanalgesic benefits of combined thoracic epidural analgesia with general anesthesia in high risk elderly off pump coronary artery bypass patients. Ann Card Anaesth 18:385–391
Fournier R, Van Gessel E, Macksay M, Gamulin Z (2000) Onset and offset of intrathecal morphine versus nalbuphine for postoperative pain relief after total hip replacement. Acta Anaesthesiol Scand 44:940–945
Funding
No funding was received in support of this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Kirada Apisutimaitri, Dr. Marvin Thepsoparn, Dr. Supichaya Chairat, Dr. Ontira Ruanma, and Dr. Wipusit Taesombat have no conflict or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Apisutimaitri, K., Thepsoparn, M., Chairat, S. et al. Comparison of intrathecal morphine and low-dose bupivacaine with intravenous morphine for postoperative analgesia in laparoscopic liver resection: a randomized controlled trial. Surg Endosc 37, 2035–2042 (2023). https://doi.org/10.1007/s00464-022-09700-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09700-1