Abstract
Background
Portal vein tumor thrombosis (PVTT) secondary to primary liver carcinoma (PLC) is commonly associated with poor prognosis and poses great challenge. This study was to evaluate the efficacy and safety of percutaneous endovascular radiofrequency ablation (RFA) in treatment of PVTT.
Methods
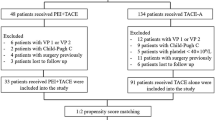
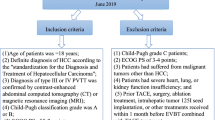
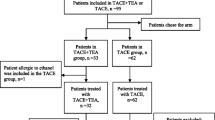
Consecutive patients who were performed endovascular RFA because of PVTT in single-institution in recent 8 years were retrospectively reviewed, compared with patients who underwent only sequential transcatheter arterial chemoembolization (TACE) during the contemporary period. Patency of portal vein, complications, and overall survival (OS) were investigated.
Results
One hundred and 20 patients who underwent endovascular RFA and 96 patients who underwent only sequential TACE were included. No severe complications happened in both groups. Except the higher rates of severe fever and moderate pain in the study group, no difference was found in the incidence of side effects and complications. The effective rate in the study group was (78.3%, 94/120) significantly higher than the comparison group (35.4%, 34/96). The median survival time and 1–3 years cumulative survival rates in the study group were 15.7 months and 42.5%, 21.7%, 2.5%, respectively, and 11.3 months, 21.9%, 9.4%, 0 correspondingly in the comparison group, without significant difference. Type of PVTT and Child–Pugh classification of liver function were independent risk factors, and OS was significantly improved by endovascular RFA and subsequent therapy.
Conclusion
Endovascular RFA is technically safe and feasible for unresectable PLC and PVTT to improve the prognosis and quality of life.



Similar content being viewed by others
References
Cerrito L, Annicchiarico BE, Iezzi R, Gasbarrini A, Pompili M, Ponziani FR (2019) Treatment of hepatocellular carcinoma in patients with portal vein tumor thrombosis: beyond the known frontiers. World J Gastroenterol 25:4360–4382
Liang L, Chen TH, Li C, Xing H, Han J, Wang MD et al (2018) A systematic review comparing outcomes of surgical resection and non-surgical treatments for patients with hepatocellular carcinoma and portal vein tumor thrombus. HPB (Oxford) 20:1119–1129
Yin J, Bo WT, Sun J, Xiang X, Lang JY, Zhong JH et al (2017) New evidence and perspectives on the management of hepatocellular carcinoma with portal vein tumor thrombus. J Clin Transl Hepatol 5:169–176
Cheng S, Chen M, Cai J, Sun J, Guo R, Bi X et al (2020) Chinese expert consensus on multidisciplinary diagnosis and treatment of hepatocellular carcinoma with portal vein tumor thrombus (2018 Edition). Liver Cancer. 9:28–40
Kim PH, Choi SH, Kim JH, Park SH (2019) Comparison of radioembolization and sorafenib for the treatment of hepatocellular carcinoma with portal vein tumor thrombosis: a systematic review and meta-analysis of safety and efficacy. Korean J Radiol 20:385–398
Silva JP, Berger NG, Tsai S, Christians KK, Clarke CN, Mogal H et al (2017) Transarterial chemoembolization in hepatocellular carcinoma with portal vein tumor thrombosis: a systematic review and meta-analysis. HPB (Oxford) 19:659–666
Chen ZW, Lin ZY, Chen YP, Chen J, Chen J (2018) Clinical efficacy of endovascular radiofrequency ablation in the treatment of portal vein tumor thrombus of primary hepatocellular carcinoma. J Cancer Res Ther 14:145–149
Colagrande S, Inghilesi AL, Aburas S, Taliani GG, Nardi C, Marra F (2016) Challenges of advanced hepatocellular carcinoma. World J Gastroenterol 22:7645–7659
Zhang X, Wang K, Wang M, Yang G, Ye X, Wu M et al (2017) Transarterial chemoembolization (TACE) combined with sorafenib versus TACE for hepatocellular carcinoma with portal vein tumor thrombus: a systematic review and meta-analysis. Oncotarget 8(17):29416–29427
Gao Y, Wang PX, Cheng JW, Sun YF, Hu B, Guo W et al (2019) Chemotherapeutic perfusion of portal vein after tumor thrombectomy and hepatectomy benefits patients with advanced hepatocellular carcinoma: a propensity score-matched survival analysis. Cancer Med 8:6933–6944
Wu TT, Li HC, Zheng F, Ao GK, Lin H, Li WM (2016) Percutaneous endovascular radiofrequency ablation for malignant portal obstruction: an initial clinical experience. Cardiovasc Interv Radiol 39:994–1000
Lawaetz M, Serup J, Lawaetz B, Bjoern L, Blemings A, Eklof B et al (2017) Comparison of endovenous ablation techniques, foam sclerotherapy and surgical stripping for great saphenous varicose veins. Extended 5-year follow-up of a RCT. J Vasc Surg Venous Lymphat Disord 36:281–288
Bilbao JI, Páramo M, Madrid JM, Benito A (2018) Hepatocellular carcinoma treatment: ablation and arterial embolization. Radiologia 60:156–166
Giorgio A, Gatti P, Montesarchio L, Santoro B, Dell’Olio A, Crucinio N et al (2019) Intrahepatic cholangiocarcinoma and thermal ablation: long-term results of an Italian retrospective multicenter study. J Clin Transl Hepatol 7:287–292
Lanza E, Muglia R, Bolengo I, Poretti D, D’Antuono F, Ceriani R et al (2020) Survival analysis of 230 patients with unresectable hepatocellular carcinoma treated with bland transarterial embolization. PLoS ONE 15:e0227711
Funding
The author have not disclosed any funding.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosure
Ya-Lin Kong, Jin-Jin Sun, Ying Xing, Cheng Wang, Yang Liu, Cheng-Li Liu, Xiao-Jun He, Ling-Hong Kong, Hong-Yi Zhang declare that there is no potential conflicts of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kong, YL., Sun, JJ., Zhang, HY. et al. Clinical evaluation of percutaneous endovascular radiofrequency ablation for portal vein tumor thrombus: experience in 120 patients. Surg Endosc 37, 1173–1180 (2023). https://doi.org/10.1007/s00464-022-09639-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09639-3