Abstract
Background
Current guidelines recommend cholecystectomy during the index admission for gallstone pancreatitis, and a growing body of evidence indicates that patients benefit from cholecystectomy within the first 48 h of admission. We examined the impact of hospital characteristics on adherence to these data-driven practices.
Methods
We queried the National Inpatient Sample for patients admitted for gallstone pancreatitis between October 2015 and December 2018. Patients who underwent same-admission cholecystectomy were identified by procedure codes. Cholecystectomies within the first two days were classified as early cholecystectomies. Multivariable logistic regression was used to determine the association between hospital characteristics and adherence to these practices.
Results
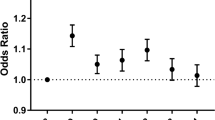
Of 163,390 admissions for gallstone pancreatitis, only 90,790 (55.6%) underwent cholecystectomy before discharge. Mean time from admission to cholecystectomy was 2.9 days; 27.0% of patients (44,005) underwent early cholecystectomy. Odds of same-admission cholecystectomy were highest in large hospitals (OR 1.21, 95% CI 1.13–1.28), urban teaching centers (OR 1.33, 95% CI 1.21–1.46), and the South (OR 1.70, 95% CI 1.57–1.83). Odds of early cholecystectomy did not vary with hospital size, urban–rural status, or teaching status but were highest in the West (OR 1.98, 95% CI 1.80–2.18).
Conclusion
Best-practice adherence for cholecystectomy in gallstone pancreatitis remains low despite an abundance of evidence and clinical practice guidelines. Active interventions are needed to improve delivery of surgical care for this patient population. Implementation efforts should focus on small hospitals, rural areas, and health systems in the Northeast region.
Graphical abstract

Similar content being viewed by others
References
Yadav D, Lowenfels AB (2006) Trends in the epidemiology of the first attack of acute pancreatitis: a systematic review. Pancreas 33(4):323–330
Forsmark CE, Baillie J, AGA Institute Clinical Practice and Economics Committee, AGA Institute Governing Board (2007) AGA institute technical review on acute pancreatitis. Gastroenterology 132(5):2022–2044
Johnson CD, Besselink MG, Carter R (2014) Acute pancreatitis. BMJ 349:g4859
Frei GJ, Frei VT, Thirlby RC, McClelland RN (1986) Biliary pancreatitis: clinical presentation and surgical management. Am J Surg 151(1):170–175
Uhl W, Müller CA, Krähenbühl L, Schmid SW, Schölzel S, Büchler MW (1999) Acute gallstone pancreatitis: timing of laparoscopic cholecystectomy in mild and severe disease. Surg Endosc 13(11):1070–1076
Moreau JA, Zinsmeister AR, Melton LJ, DiMagno EP (1988) Gallstone pancreatitis and the effect of cholecystectomy: a population-based cohort study. Mayo Clin Proc 63(5):466–473
Sandzén B, Haapamäki MM, Nilsson E, Stenlund HC, Oman M (2009) Cholecystectomy and sphincterotomy in patients with mild acute biliary pancreatitis in Sweden 1988–2003: a nationwide register study. BMC Gastroenterol 9:80
Bakker OJ, van Santvoort HC, Hagenaars JC et al (2011) Timing of cholecystectomy after mild biliary pancreatitis. Br J Surg 98(10):1446–1454
El-Dhuwaib Y, Deakin M, David GG, Durkin D, Corless DJ, Slavin JP (2012) Definitive management of gallstone pancreatitis in England. Ann R Coll Surg Engl 94(6):402–406
van Baal MC, Besselink MG, Bakker OJ et al (2012) Timing of cholecystectomy after mild biliary pancreatitis: a systematic review. Ann Surg 255(5):860–866
da Costa DW, Bouwense SA, Schepers NJ et al (2015) Same-admission versus interval cholecystectomy for mild gallstone pancreatitis (PONCHO): a multicentre randomised controlled trial. Lancet 386(10000):1261–1268
Leppäniemi A, Tolonen M, Tarasconi A et al (2019) 2019 WSES guidelines for the management of severe acute pancreatitis. World J Emerg Surg 14:27
Working Group IAP/APA Acute Pancreatitis Guidelines (2013) IAP/APA evidence-based guidelines for the management of acute pancreatitis. Pancreatology 13(4 Suppl 2):e1–e15
Crockett SD, Wani S, Gardner TB, Falck-Ytter Y, Barkun AN, American Gastroenterological Association Institute Clinical Guidelines Committee (2018) American Gastroenterological Association Institute guideline on initial management of acute pancreatitis. Gastroenterology 154(4):1096–1101
Tenner S, Baillie J, DeWitt J, Vege SS, American College of Gastroenterology (2013) American College of Gastroenterology guideline: management of acute pancreatitis. Am J Gastroenterol 108(9):1400–1415
Rosing DK, de Virgilio C, Yaghoubian A et al (2007) Early cholecystectomy for mild to moderate gallstone pancreatitis shortens hospital stay. J Am Coll Surg 205(6):762–766
Aboulian A, Chan T, Yaghoubian A et al (2010) Early cholecystectomy safely decreases hospital stay in patients with mild gallstone pancreatitis: a randomized prospective study. Ann Surg 251(4):615–619
Falor AE, de Virgilio C, Stabile BE et al (2012) Early laparoscopic cholecystectomy for mild gallstone pancreatitis: time for a paradigm shift. Arch Surg 147(11):1031–1035
Zhao X, Chen D-Z, Lang R et al (2013) Enhanced recovery in the management of mild gallstone pancreatitis: a prospective cohort study. Surg Today 43(6):643–647
Giuffrida P, Biagiola D, Cristiano A et al (2020) Laparoscopic cholecystectomy in acute mild gallstone pancreatitis: how early is safe? Updates Surg 72(1):129–135
Nguyen GC, Tuskey A, Jagannath SB (2008) Racial disparities in cholecystectomy rates during hospitalizations for acute gallstone pancreatitis: a national survey. Am J Gastroenterol 103(9):2301–2307
Nguyen GC, Boudreau H, Jagannath SB (2010) Hospital volume as a predictor for undergoing cholecystectomy after admission for acute biliary pancreatitis. Pancreas 39(1):e42–e47
Bilal M, Kline KT, Trieu JA et al (2019) Trends in same-admission cholecystectomy and endoscopic retrograde cholangiopancreatography for acute gallstone pancreatitis: a nationwide analysis across a decade. Pancreatology 19(4):524–530
Banks PA, Bollen TL, Dervenis C et al (2013) Classification of acute pancreatitis–2012: revision of the Atlanta classification and definitions by international consensus. Gut 62(1):102–111
Quan H, Sundararajan V, Halfon P et al (2005) Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care 43(11):1130–1139
Balas EA, Boren SA (2000) Managing clinical knowledge for health care improvement. Yearb Med Inform 1:65–70
Uhl W, Warshaw A, Imrie C et al (2002) IAP guidelines for the surgical management of acute pancreatitis. Pancreatology 2(6):565–573
Frossard J-L, Steer ML, Pastor CM (2008) Acute pancreatitis. Lancet 371(9607):143–152
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. James Etheridge, Manuel Castillo-Angeles, Robert Sinyard, Molly Jarman, and Joaquim Havens have no conflicts of interest or financial ties to declare.
Ethical approval
This study was conducted with ethical approval from the Mass General Brigham Institutional Review Board, #2015P001722.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Etheridge, J.C., Castillo-Angeles, M., Sinyard, R.D. et al. Impact of hospital characteristics on best-practice adherence for gallstone pancreatitis: a nationwide analysis. Surg Endosc 37, 127–133 (2023). https://doi.org/10.1007/s00464-022-09444-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09444-y