Abstract
Background and aims
Endoscopic ultrasonography-guided hepaticogastrostomy (EUS-HGS) is often performed using a single guidewire (SGW), but the efficacy of the double guidewire (DGW) technique during endoscopic ultrasonography-guided biliary drainage has been reported. We evaluated the efficacy of the DGW technique for EUS-HGS, focusing on the guidewire angle at the insertion site.
Methods
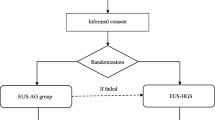
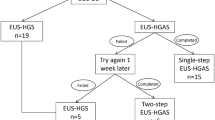
This retrospective cohort study included consecutive patients who underwent EUS-HGS between April 2012 and March 2021. We measured the guidewire angle at the insertion site using still fluoroscopic imaging. We compared the clinical outcomes of EUS-HGS with the DGW and SGW techniques. The factors associated with successful cannula insertion, need for additional fistula dilation and adverse event rate were assessed by a logistic regression multivariable analysis.
Results
The DGW group showed higher technical (p = 0.020) and clinical success rates (p = 0.016) than the SGW group, which showed more adverse events (p = 0.017) than the DGW group. Successful cannula insertion was associated with a guidewire angle > 137° and an uneven double-lumen cannula. The DGW technique made the guidewire angle obtuse at the insertion site (p < 0.0001). A guidewire angle ≤ 137° (OR, 35.6; 95% CI, 1.70–744; p = 0.0045) and intrahepatic bile duct diameter of the puncture site ≤ 3.0 mm (OR, 14.4; 95% CI, 1.37–152; p = 0.0056) were risk factors for needing additional fistula dilation in a multivariate analysis, and additional dilation was a significant predictive factor for adverse events (OR, 8.3; 95% CI, 0.9–77; p = 0.026).
Conclusions
The DGW technique can modify the guidewire angle at the insertion site and facilitate stent deployment with few adverse events.





Similar content being viewed by others
References
Fogel E, Sherman S, Devereaux B et al (2001) Therapeutic biliary endoscopy. Endoscopy 33:31–38
Freeman M, Guda N (2005) ERCP cannulation: a review of reported techniques. Gastrointest Endosc 61:112–125
Van Delden O, Lameris J (2008) Percutaneous drainage and stenting for palliation of malignant bile duct obstruction. Eur Radiol 18:448–456
Giovannini M, Moutardier V, Pesenti C et al (2001) Endoscopic ultrasound-guided bilioduodenal anastomosis: a new technique for biliary drainage. Endoscopy 33:898–900
Lee T, Choi J, Park Do H et al (2016) Similar efficacies of endoscopic ultrasound-guided transmural and percutaneous drainage for malignant distal biliary obstruction. Clin Gastroenterol Hepatol 14:1011–1019
Hedjoudje A, Sportes A, Grabar S et al (2019) Outcomes of endoscopic ultrasound-guided biliary drainage: a systematic review and meta-analysis. United European Gstroenterol J 7:E52-59
Miller CS, Barkun A, Martel M et al (2019) Endoscopic ultrasound-guided biliary drainage for distal malignant obstruction: a systematic review and meta-analysis of randomized trials. Endosc Int Open 7:E1563–E1573
Isayama H, Nakai Y, Itoi T et al (2019) Clinical practice guidelines for safe performance of endoscopic ultrasound/ultrasonography-guided biliary drainage: 2018. J Hepatobiliary Pancreat sci 26:249–269
Van Geenen EJM, Siersema PD (2018) Stent migration into the abdominal cavity after EUS-guided hepaticogastrostomy. Gastrointest Endosc 87:617–618
Prachayakul V, Aswakul P (2012) Successful endoscopic treatment of iatrogenic biloma as a complication of endosonography-guided hepaticogastrostomy: the first case report. J interv Gastroenterol 2:202–204
Nakai Y, Oyama H, Koike K et al (2021) Double guidewire technique using an uneven double lumen catheter for endoscopic ultrasound-guided interventions. Dig Dis Sci 66:1540–1547
Ishiwatari H, Satoh T, Sato J et al (2019) Double-guidewire technique facilitates endoscopic ultrasound- guided biliary drainage for hilar biliary obstruction. Endoscopy 11:E321–E322
Shiomi H, Masuda A, Kodama Y (2019) Novel approach for successful endoscopic ultrasound-guided hepaticogastrostomy using a double-guidewire technique. Dig Endosc 31:e50–e51
Cotton PB, Eisen GM, Aabakken L et al (2010) A lexicon for endoscopic adverse events: report of an ASGE workshop. Gastrointest Endosc 71:446–454
Hathom KE, Bazarbashi AN, Sack JS et al (2019) EUS-guided biliary drainage is equivalent to ERCP for primary treatment of malignant distal biliary obstruction: a systematic review and meta-analysis. Endosc Int Open 7:E1432–E1441
Wang K, Zhu J, Xing L et al (2016) Assessment of efficacy and safety of EUS-guided biliary drainage: a systematic review. Gastrointest Endosc 83:1218–1227
Kawakubo K, Isayama H, Kato H et al (2014) Multicenter retrospective study of endoscopic ultrasound-guided biliary drainage for malignant biliary obstruction in Japan. J Hepatobiliary Pancreat Sci 21:328–334
Oh D, Park DH, Song TJ et al (2017) Optimal biliary access point and learning curve for endoscopic ultrasound-guided hepaticogastrostomy with transmural stenting. Therap Adv Gastroenterol 10:42–53
Yamamoto Y, Ogura T, Nishioka N et al (2020) Risk factors for adverse events associated with bile leak during EUS-guided hepaticogastrostomy. Endosc Ultrasound 9:110–115
Ogura T, Nishioka N, Higuchi K et al (2021) Effect of echoendoscope angle on success of guidewire manipulation during endoscopic ultrasound- guided hepaticogastrostomy. Endoscopy 53:369–375
Ang TL, Teo EK, Fock KM et al (2008) EUS-guided drainage of infected pancreatic pseudocyst: use of a 10F Soehendra dilator to facilitate a double-wire technique for initial transgastric access (with videos). Gastrointest Endosc 68:192–194
Itoi T, Itokawa F, Tsuchiya T et al (2009) EUS-guided pancreatic pseudocyst drainage: simultaneous placement of stents and nasocystic catheter using double-guidewire technique. Dig Endosc 21:S53–S56
Vila JJ, Perez-Miranda M, Vazquez-Sequeiros E et al (2012) Initial experience with EUS-guided cholangiopancreatography for biliary and pancreatic duct drainage: a Spanish national survey. Gastrointest Endosc 76:1133–1141
Poincloux L, Rouquette O, Buc E et al (2015) Endoscopic ultrasound-guided biliary drainage after failed ERCP: cumulative experience of 101 procedures at a single center. Endoscopy 47:794–801
Manta R, Mutignani M, Galloro G et al (2018) Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a lumen-apposing metal stent: a systematic review of case series. Eur J Gastroenterol Hepatol 30:695–698
Chandrasekhara V, Barthet M, Deviere J et al (2020) Safety and efficacy of lumen-apposing metal stents versus plastic stents to treat walled-off pancreatic necrosis: systematic review and meta-analysis. Endosc Int Open 8:E1639–E1653
Acknowledgements
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Yuki Fujii, Hironari Kato, Hitomi Himei, Eijiro Ueta, Taiji Ogawa, Hiroyuki Terasawa, Tatsuhiro Yamazaki, Kazuyuki Matsumoto, Shigeru Horiguchi, Koichiro Tsutsumi, and Hiroyuki Okada have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fujii, Y., Kato, H., Himei, H. et al. Double guidewire technique stabilization procedure for endoscopic ultrasound-guided hepaticogastrostomy involving modifying the guidewire angle at the insertion site. Surg Endosc 36, 8981–8991 (2022). https://doi.org/10.1007/s00464-022-09350-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09350-3