Abstract
Background
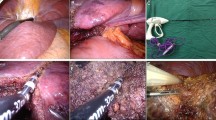
Liver parenchymal transection is the most critical step for laparoscopic liver resection (LLR). Ultrasonic scalpel (Harmonic) is a common used energy instrument in LLR; however, it is only recommended for superficial layer transection and the Cavitron Ultrasonic Surgical Aspirator (CUSA) is recommended for deep layer dissection. We herein introduce the “Harmonic mimic CUSA” technique for LLR.
Methods
We retrospectively reviewed the medical records of the patients who underwent LLR using CUSA or the “Harmonic mimic CUSA” for parenchymal transection between July 2018 and October 2020 at West China Hospital of Sichuan University. Observation indicators included general demographic information, operative time, intraoperative blood loss, blood transfusion volume, complication rate, hospital stay, and the costs. Perioperative data was compared between the two groups by propensity score matching analysis (PSM).
Results
A total of 298 patients, including 192 in Harmonic group and 106 in CUSA group, were enrolled in this study. After a 1:1 PSM, 99 patients using “Harmonic mimic CUSA” were matched with 99 patients via CUSA for parenchymal transection in LLRs. The Harmonic group had significantly less intraoperative blood loss (mean, 150 ml vs. 250 ml, P < 0.001), shorter operative time (mean 170 min vs. 250 min, P < 0.001) and less costs (mean 6723$ vs. 8307$, P < 0.001). The conversion to laparotomy, length of postoperative hospital stay, complications were comparable between the two groups. There perioperative mortality was nil.
Conclusion
The “Harmonic mimic CUSA” technique is safe, simple and feasible for LLR, which may be an alternative to CUSA for LLR.

Similar content being viewed by others
Data availability
On request.
Change history
09 September 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00464-022-09399-0
References
Schmidbauer S, Hallfeldt KK, Sitzmann G, Kantelhardt T, Trupka A (2002) Experience with ultrasound scissors and blades (ultracision) in open and laparoscopic liver resection. Ann Surg 235:27–30
Scatton O, Brustia R, Belli G, Pekolj J, Wakabayashi G, Gayet B (2015) What kind of energy devices should be used for laparoscopic liver resection? Recommendations from a systematic review. J Hepatobiliary Pancreat Sci 22:327–334
Poon R (2007) Current techniques of liver transection. HPB (Oxford) 9:166–173
Cai X (2018) Laparoscopic liver resection: the current status and the future. Hepatobiliary Surg Nutr 7:98
Chenyang J, Hongyu L, Ningyuan W, Junhua C, Yonggang W (2018) Laparoscopic liver resection: a review of current indications and surgical techniques. Hepatobiliary Surg Nutr 7:277
Otsuka Y, Kaneko H, Cleary SP, Buell JF, Cai X, Wakabayashi G (2015) What is the best technique in parenchymal transection in laparoscopic liver resection? Comprehensive review for the clinical question on the 2nd International Consensus Conference on Laparoscopic Liver Resection. J Hepatobiliary Pancreat Sci 22:363–370
Gorgen A, Goldaracena N, Zhang W, Rosales R, Ghanekar A, Lilly L, Cattral M, Greig P, McCluskey S, McGilvray I (2018) Surgical complications after right hepatectomy for live liver donation: largest single-center western world experience. Semin Liver Dis 38:134–144
Bodzin AS, Leiby BE, Ramirez CG, Frank AM, Doria C (2014) Liver resection using cavitron ultrasonic surgical aspirator (CUSA) versus harmonic scalpel: a retrospective cohort study. Int J Surg 12:500–503
Scatton O, Vibert E (2018) Chirurgie hépatique par laparoscopie. Arnette, Paris
Soubrane O, Cherqui D, Scatton O, Stenard F, Bernard D, Branchereau S, Martelli H, Gauthier F (2006) Laparoscopic left lateral sectionectomy in living donors: safety and reproducibility of the technique in a single center. Ann Surg 244:815
Choi G, Chung Y, Lee J, Gil E, Kim J, Kwon C, Joh J, Lee SJT (2018) Safety and risk factors of pure laparoscopic living donor right hepatectomy: comparison to open technique in propensity matched analysis. Transplantation 102:128–128
Liu F, Xu H, Li Q, Wei Y, Li H, Wang W, Wen T, Wu H, Yang J, Xu M (2019) Outcomes of pure laparoscopic Glissonian pedicle approach hepatectomy for hepatocellular carcinoma: a propensity score matching analysis. Surg Endosc 33:1155–1166
Liu F, Wei Y, Li H, Wang W, Wen T, Wu H, Yang J, Xu M, Li B (2018) LigaSure versus CUSA for parenchymal transection during laparoscopic hepatectomy in hepatocellular carcinoma patients with cirrhosis: a propensity score-matched analysis. Surg Endosc 32:2454–2465
Morise Z, Wakabayashi G (2017) First quarter century of laparoscopic liver resection. World J Gastroenterol 23:3581–3588
Yoh T, Cauchy F, Soubrane O (2019) Techniques for laparoscopic liver parenchymal transection. Hepatobiliary Surg Nutr 8:572–581
Wakabayashi G, Cherqui D, Geller D, Buell J, Kaneko H, Han H, Asbun H, O’Rourke N, Tanabe M, Lo C (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619
Honda G, Ome Y, Yoshida N, Kawamoto Y (2020) How to dissect the liver parenchyma: excavation with cavitron ultrasonic surgical aspirator. J Hepatobiliary Pancreat Sci 27:907–912
Ntourakis D, Memeo R, Soler L, Marescaux J, Mutter D, Pessaux PJ (2016) Augmented reality guidance for the resection of missing colorectal liver metastases: an initial experience. World J Surg 40:419–426
Msika S, Deroide G, Kianmanesh R, Iannelli A, Hay J-M, Fingerhut A, Flamant YJ (2001) Harmonic scalpel™ in laparoscopic colorectal surgery. Dis Colon Rectum 44:432–436
Nomi T, Hokuto D, Yoshikawa T, Kamitani N, Matsuo Y, Sho M (2021) Clamp-crush technique for laparoscopic liver resection. Ann Surg Oncol 28:866
Martins PN, Theruvath TP, Neuhaus P (2008) Rodent models of partial hepatectomies. Liver Int 28:3–11
Jersenius U, Fors D, Rubertsson S, Arvidsson D (2007) Laparoscopic parenchymal division of the liver in a porcine model: comparison of the efficacy and safety of three different techniques. Surg Endosc 21:315–320
Yamamoto J, Nagai M, Smith B, Tamaki S, Kubota T, Sasaki K, Ohmori T, Maeda K (2006) Hand-assisted laparoscopic splenectomy and devascularization of the upper stomach in the management of gastric varices. World J Surg 30:1520–1525
Gagner M, Rogula T, Selzer D (2004) Laparoscopic liver resection: benefits and controversies. Surg Clin 84:451–462
Romano F, Garancini M, Uggeri F, Degrate L, Nespoli L, Gianotti L, Nespoli A, Uggeri F (2012) Bleeding in hepatic surgery: sorting through methods to prevent it. HPB Surg 2012:12
Gotohda N, Yamanaka T, Saiura A, Uesaka K, Hashimoto M, Konishi M, Shimada K (2015) Impact of energy devices during liver parenchymal transection: a multicenter randomized controlled trial. World J Surg 39:1543–1549
Cherqui D, Husson E, Hammoud R, Malassagne B, Stéphan F, Bensaid S, Rotman N, Fagniez P-L (2000) Laparoscopic liver resections: a feasibility study in 30 patients. Ann Surg 232:753
Zhao X, Lei Z, Gao F, Yang J, Xie Q, Jiang K, Jie G (2021) Minimally invasive versus open living donors right hepatectomy: a systematic review and meta-analysis. Int J Surg (London, England) 95:106152
Erdogan D, Busch O, Van Delden O, Rauws E, Gouma D, Van Gulik T (2008) Incidence and management of bile leakage after partial liver resection. Dig Surg 25:60–66
Appere F, Piardi T, Memeo R, Lardiere-Deguelte S, Chetboun M, Sommacale D, Pessaux P, Kianmanesh R (2017) Comparative study with propensity score matching analysis of two different methods of transection during hemi-right hepatectomy: ultracision harmonic scalpel versus Cavitron ultrasonic surgical aspirator. Surg Innov 24:499–508
Lesurtel M, Selzner M, Petrowsky H, McCormack L, Clavien P-A (2005) How should transection of the liver be performed?: A prospective randomized study in 100 consecutive patients: comparing four different transection strategies. Ann Surg 242:814
Funding
This work was supported by grants from the National Natural Science Foundation of China (No. 81602910, No. 81302344, and No. 81802095) and the Sichuan Science and Technology Program (No. 2019YFS0370, No. 2019YFS0372, and No.2022YFS0090).
Author information
Authors and Affiliations
Contributions
YY: designed research/study, performed research/study, collected data, analyzed data, wrote the paper, edited the manuscript. YP and KC: collected data, analyzed data. BL and YGW: reviewed/edited the manuscript. FL: designed research/study, performed research/study, reviewed the manuscript, revised the manuscript.
Corresponding author
Ethics declarations
Disclosures
Yubo Yang, Yufu Peng, Kefei Chen, YongGang Wei, Bo Li, Fei Liu have no conflicts of interest or financial ties to disclose.
Ethical approval
This study was approved by the clinic trial ethics committee of West China hospital (NO.20211291).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 130706 kb)
Supplementary file2 (MP4 1296 kb)
Supplementary file3 (MP4 1239 kb)
Supplementary file4 (MP4 1428 kb)
Supplementary file5 (MP4 1756 kb)
Rights and permissions
About this article
Cite this article
Yang, Y., Peng, Y., Chen, K. et al. Laparoscopic liver resection with “ultrasonic scalpel mimic CUSA" technique. Surg Endosc 36, 8927–8934 (2022). https://doi.org/10.1007/s00464-022-09341-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09341-4