Abstract
Background
Minimally invasive esophagectomy (MIE) for esophageal cancer has been associated with decreased pain, less blood loss, and shorter hospital stay with comparable survival to open surgery. To date, there is minimal information regarding what factors are associated with access to MIE.
Methods
The National Cancer Database (NCDB) was used to compare rates of MIE (either robotic or laparoscopic) and open esophagectomy (OE) by demographic and clinical factors. Continuous variables were compared using a linear trend test, and categorical variables were compared using Mantel–Haenszel tests. Binomial regression was performed to examine significant factors after adjusting for confounding variables.
Results
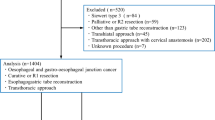
There were 18,366 patients included in the analysis. Of all esophagectomies performed in the US, 49% were performed by OE and 51% were performed by MIE. Patients who had undergone MIE were more likely to live in the Eastern US as compared with the Midwest [odds ratio (OR) 1.72; 95% confidence interval (CI) 1.58, 1.88] or the South (OR 1.31; 95% CI 1.19, 1.44). They were also more likely to be treated at an academic center (OR 1.64; 95% CI 1.53, 1.75) rather than a community hospital, and to be of White race as compared with Asian race (OR 1.46; 95% CI 1.10, 1.92). There was not a significant difference in the rates of MIE between White and Black patients (OR 1.12; 95% CI 0.96, 1.32). MIE was more likely with each passing year, and higher TNM stages of cancer were less likely to be treated with MIE (P < 0.001 for all).
Conclusion
While MIE is evolving, OE is still considered standard of care with robotic approaches representing a minority of MIE. While there are several factors associated with access to MIE, including race, facility type and geographic location, these factors should be further explored to help increase access to MIE.



Similar content being viewed by others
References
Barsouk A, Rawla P, Hadjinicolaou AV, Aluru JS, Barsouk A (2019) Targeted therapies and immunotherapies in the treatment of esophageal cancers. Med Sci 7(10):100. https://doi.org/10.3390/medsci7100100
Wyant T, Alteri R, Kalidas M, Ogoro C, Lubejko B (2009) Esophageal cancer risk factors. American Cancer Society. https://www.cancer.org/cancer/esophagus-cancer/causes-risks-prevention/risk-factors.html. Accessed 26 Feb 2021
Wyant T, Alteri R, Kalidas M, Ogoro C, Lubejko B (2021) Key statistics for esophageal cancer. American Cancer Society. https://www.cancer.org/cancer/esophagus-cancer/about/key-statistics.html. Accessed 26 Feb 2021
Chai J, Jamal MM (2012) Esophageal malignancy: a growing concern. World J Gastroenterol 18(45):6521–6526. https://doi.org/10.3748/wjg.v18.i45.6521
Malhotra GK, Yanala U, Ravipati A, Follet M, Vijayakumar M, Are CA (2017) Global trends in esophageal cancer. J Surg Oncol 115:564–579. https://doi.org/10.1002/jso.24592
Zhang H, Chen SH, Li YM (2004) Epidemiological investigation of esophageal carcinoma. World J Gastroenterol 10(12):1834–1835. https://doi.org/10.3748/wjg.v10.i12.1834
Esophageal cancer—cancer stat facts. https://seer.cancer.gov/statfacts/html/esoph.html. Accessed 26 Feb 2021
He H et al (2020) Trends in the incidence and survival of patients with esophageal cancer: a SEER database analysis. Thorac Cancer 11(5):1121–1128. https://doi.org/10.1111/1759-7714.13311
Kohler BA et al (2011) Annual report to the nation on the status of cancer, 1975–2007, featuring tumors of the brain and other nervous system. J Natl Cancer Inst 103(9):714–736. https://doi.org/10.1093/jnci/djr077
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics, GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries”. CA Cancer J Clin. https://doi.org/10.3322/caac.21492
Klevebro F, Ekman S, Nilsson M (2017) Current trends in multimodality treatment of esophageal and gastroesophageal junction cancer—review article. Surg Oncol 26(3):290–295. https://doi.org/10.1016/j.suronc.2017.06.002
Barret M, Prat F (2018) Diagnosis and treatment of superficial esophageal cancer. Ann Gastroenterol 31(3):256–265. https://doi.org/10.20524/aog.2018.0252
Lazzarino AI, Nagpal K, Bottle A, Faiz O, Moorthy K, Aylin P (2010) Open versus minimally invasive esophagectomy: trends of utilization and associated outcomes in England. Ann Surg 252(2):292–298. https://doi.org/10.1097/SLA.0b013e3181dd4e8c
Mallipeddi MK, Onaitis MW (2014) The contemporary role of minimally invasive esophagectomy in esophageal cancer topical collection on gastrointestinal cancers. Curr Oncol Rep. https://doi.org/10.1007/s11912-013-0374-9
Biere SS et al (2011) Traditional invasive vs. minimally invasive esophagectomy: a multi-center, randomized trial (TIME-trial). BMC Surg 11:2. https://doi.org/10.1186/1471-2482-11-2
Weksler B, Sullivan JL (2017) Survival after esophagectomy: a propensity-matched study of different surgical approaches. Ann Thorac Surg 104(4):1138–1146. https://doi.org/10.1016/j.athoracsur.2017.04.065
Lv L, Hu W, Ren Y, Wei X (2016) Minimally invasive esophagectomy versus open esophagectomy for esophageal cancer: a meta-analysis. OncoTargets Ther 9:6751–6762. https://doi.org/10.2147/OTT.S112105
Straatman J et al (2017) Minimally invasive versus open esophageal resection. Ann Surg 266(2):232–236. https://doi.org/10.1097/SLA.0000000000002171
Smedley BD, Stith AY, Nelson AR (2003), Assessing potential sources of racial and ethnic disparities in care: patient- and system-level factors. https://www.ncbi.nlm.nih.gov/books/NBK220359/. Accessed 26 Feb 2021
Dubecz A et al (2012) Temporal trends in long-term survival and cure rates in esophageal cancer: a SEER database analysis. J Thorac Oncol 7(2):443–447. https://doi.org/10.1097/JTO.0b013e3182397751
Sridhar P et al (2019) Esophageal cancer presentation, treatment, and outcomes vary with hospital safety-net burden. Ann Thorac Surg 107(5):1472–1479. https://doi.org/10.1016/j.athoracsur.2018.11.065
Baquet CR, Commiskey P, Mack K, Meltzer S, Mishra SI (2005) Esophageal cancer epidemiology in blacks and whites: racial and gender disparities in incidence, mortality, survival rates and histology. J Natl Med Assoc 97(11):1471–1478. www.seer.cancer.gov. Accessed 26 Feb 2021
Savitch SL et al (2020) Racial disparities in rates of surgery for esophageal cancer: a study from the National Cancer Database. J Gastrointest Surg. https://doi.org/10.1007/s11605-020-04653-z
Wasif N et al (2018) Racial and socioeconomic differences in the use of high-volume commission on cancer-accredited hospitals for cancer surgery in the United States. Ann Surg Oncol 25(5):1116–1125. https://doi.org/10.1245/s10434-018-6374-0
Marsh HW (1998) Pairwise deletion for missing data in structural equation models: nonpositive definite matrices, parameter estimates, goodness of fit, and adjusted sample sizes. Struct Equ Model 5(1):22–36. https://doi.org/10.1080/10705519809540087
Manigrasso M et al (2021) Robotic esophagectomy. A systematic review with meta-analysis of clinical outcomes. J Pers Med. https://doi.org/10.3390/JPM11070640
Espinoza-Mercado F et al (2019) Does the approach matter? Comparing survival in robotic, minimally invasive, and open esophagectomies. Ann Thorac Surg. https://doi.org/10.1016/j.athoracsur.2018.08.039
Larson E, Andrilla C, Kearny J, Garberson L, Patterson D (2021) The distribution of the general surgery workforce in rural and urban American in 2019 Policy Brief 1–9. https://familymedicine.uw.edu/rhrc/wp-content/uploads/sites/4/2021/03/RHRC_PBMAR2021_LARSON.pdf. Accessed 14 July 2021
Zhang X, Lin D, Pforsich H, Lin VW (2020) Physician workforce in the United States of America: forecasting nationwide shortages. Hum Resour Health. https://doi.org/10.1186/S12960-020-0448-3
Revels SL, Morris AM, Reddy RM, Akateh C, Wong SL (2013) Racial disparities in esophageal cancer outcomes. Ann Surg Oncol 20(4):1136. https://doi.org/10.1245/S10434-012-2807-3
Chen Z et al (2017) Incidence and survival differences in esophageal cancer among ethnic groups in the United States. Oncotarget 8(29):47037. https://doi.org/10.18632/ONCOTARGET.16694
Pickens A, Orringer MB (2003) Geographical distribution and racial disparity in esophageal cancer. Ann Thorac Surg 76(4):S1367–S1369
Kubo A, Corley DA (2004) Marked multi-ethnic variation of esophageal and gastric cardia carcinomas within the United States. Am J Gastroenterol 99(4):582–588. https://doi.org/10.1111/j.1572-0241.2004.04131.x
Brusselaers N, Mattsson F, Lindblad M, Lagergren J (2015) Association between education level and prognosis after esophageal cancer surgery: a Swedish population-based cohort study. PLoS ONE 10(3):e0121928. https://doi.org/10.1371/journal.pone.0121928
Schandl AR, Johar A, Mälberg K, Lagergren P (2018) Education level and health-related quality of life after oesophageal cancer surgery: a nationwide cohort study. BMJ Open 8(8):20702. https://doi.org/10.1136/bmjopen-2017-020702
Lagergren J et al (2016) Marital status, education, and income in relation to the risk of esophageal and gastric cancer by histological type and site. Cancer 122(2):207–212. https://doi.org/10.1002/cncr.29731
Acknowledgements
The authors would like to thank Kevin Kennedy for his statistical expertise in cross-checking analyses for accuracy.
NCDB Disclaimer
The CoC's NCDB and the hospitals participating in the CoC NCDB are the source of the de-identified data used herein; they have not verified and are not responsible for the statistical validity of the data analysis or the conclusions derived by the authors.
Funding
No funding was required for the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Benny Weksler, Elizabeth Blears, Hiran Fernando and James Shahoud have no conflicts of interest or financial ties to disclose. Dr. Benny Weksler is a lecturer for AstraZeneca, but his lecture material does not directly overlap with this study. This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Presented at SAGES 2021 Annual Meeting, Las Vegas, NV, 31 August–3 September.
Rights and permissions
About this article
Cite this article
Blears, E., Fernando, H.C., Shahoud, J. et al. Factors associated with access and approach to esophagectomy for cancer: a National Cancer Database study. Surg Endosc 36, 7016–7024 (2022). https://doi.org/10.1007/s00464-022-09032-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09032-0