Abstract
Background
The number of scientific articles published each year is increasing, resulting in greater competition to get work published. Spin is defined as specific reporting strategies used to distort the readers’ interpretation of results so that they are viewed more favorable. However, prevalence of spin in studies comparing robot-assisted groin hernia repair with traditional methods is unknown.
Objectives/aim
To determine the frequency and extent of spin in studies assessing robot-assisted groin hernia repair.
Methods
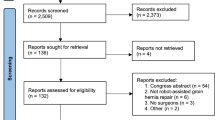
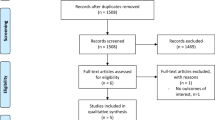
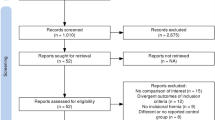
This systematic review was reported according to PRISMA guidelines, and a protocol was registered at PROSPERO before data extraction. Database search included PubMed, EMBASE, and Cochrane Central.
Results
Of 35 included studies, spin was present in 57%. Within these, 95% had spin present in the abstract and 80% in the conclusion of the article. There was no association between study size and spin (p > 0.05). However, presence of spin in studies positively minded towards robot-assisted hernia repair was higher (p < 0.001) compared with those against or being neutral in their view of the procedure. Furthermore, being funded by or receiving grants from Intuitive Surgical were associated with a higher prevalence of spin (p < 0.05) compared with those who were not.
Conclusion
Spin was found to be common in articles reporting on robot-assisted groin hernia repair, and presence of spin was higher in studies funded by or receiving grants from the robot company. This suggests that readers should be cautious when reading similar literature.

Similar content being viewed by others
Availability of data, code and other materials
All relevant data are available in the presented article.
References
HerniaSurge Group (2018) International guidelines for groin hernia management. Hernia 22:1–165
Kingsnorth A, LeBlanc K (2003) Hernias: inguinal and incisional. Lancet 362:1561–1571
Sheetz KH, Claflin J, Dimick JB (2020) Trends in the adoption of robotic surgery for common surgical procedures. JAMA Netw Open 3:e1918911
Andresen K, Rosenberg J (2021) Decreasing use of open procedures in elective inguinal hernia surgery. Laparosc Surg 5:17
Aiolfi A, Cavalli M, Micheletto G, Bruni PG, Lombardo F, Perali C et al (2019) Robotic inguinal hernia repair: is technology taking over? Systematic review and meta-analysis. Hernia 23:509–519
Aiolfi A, Cavalli M, Micheletto G, Lombardo F, Bonitta G, Morlacchi A et al (2019) Primary inguinal hernia: systematic review and bayesian network meta-analysis comparing open, laparoscopic transabdominal preperitoneal, totally extraperitoneal, and robotic preperitoneal repair. Hernia 23:473–484
Qabbani A, Aboumarzouk OM, ElBakry T, Al-Ansari A, Elakkad MS (2021) Robotic inguinal hernia repair: systematic review and meta-analysis. ANZ J Surg 91:2277–2287
Rosenberg J (2019) A critical appraisal about robotic-assisted surgery. Laparosc Surg 3:50
Gunnarsson U, Dahlstrand U, Strigård K (2021) Is robotic-assisted surgery a step in the right direction for routine inguinal hernia repair? Laparosc Surg. in press
Boutron I, Dutton S, Ravaud P, Altman DG (2010) Reporting and interpretation of randomized controlled trials with statistically nonsignificant results for primary outcomes. JAMA 303:2058–2064
Boutron I, Altman DG, Hopewell S, Vera-Badillo F, Tannock I, Ravaud P (2014) Impact of spin in the abstracts of articles reporting results of randomized controlled trials in the field of cancer: the SPIIN randomized controlled trial. J Clin Oncol 32:4120–4126
Patel SV, Van Koughnett JAM, Howe B, Wexner SD (2015) Spin is common in studies assessing robotic colorectal surgery: an assessment of reporting and interpretation of study results. Dis Colon Rectum 58:878–884
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71
Hansen DL, Fonnes S, Rosenberg J (2021) Spin in studies assessing robotic groin hernia repair: a systematic review (CRD42021244618). https://www.crd.york.ac.uk/prospero/display_record.php?RecordID=244618. Accessed 14 Nov 2021
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2021) Rayyan QCRI. https://rayyan.qcri.org/reviews. Accessed 14 Nov 2021
Greenhalgh T, Peacock R (2005) Effectiveness and efficiency of search methods in systematic reviews of complex evidence: audit of primary sources. BMJ 331:1064–1065
Chiu K, Grundy Q, Bero L (2017) ‘Spin’ in published biomedical literature: a methodological systematic review. PLoS Biol 15:e2002173
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, et al (2021) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Ottawa Hospital Research Institute. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 14 Nov 2021
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Aghayeva A, Benlice C, Bilgin IA, Bengur FB, Bas M, Kirbiyik E et al (2020) Laparoscopic totally extraperitoneal vs robotic transabdominal preperitoneal inguinal hernia repair: assessment of short- and long-term outcomes. Int J Med Robot 16:e2111
Gundogdu E, Guldogan CE, Ozmen MM (2020) Bilateral inguinal hernia repair: robotic TAPP versus laparoscopic TEP. Surg Laparosc Endosc Percutan Tech 31:439–443
Janjua H, Cousin-Peterson E, Barry TM, Kuo MC, Baker MS, Kuo PC (2019) The paradox of the robotic approach to inguinal hernia repair in the inpatient setting. Am J Surg 219:497–501
Janjua H, Cousin-Peterson E, Barry TM, Kuo MC, Baker MS, Kuo PC (2020) Robotic approach to outpatient inguinal hernia repair. J Am Coll Surg 231:61–72
Vossler JD, Pavlosky KK, Murayama SM, Moucharite MA, Murayama KM, Mikami DJ (2019) Predictors of robotic versus laparoscopic inguinal hernia repair. J Surg Res 241:247–253
Kadakia N, Malek K, Lee SK, Lee EJ, Burruss S, Srikureja D et al (2020) Impact of robotic surgery on residency training for herniorrhaphy and cholecystectomy. Am Surg 86:1318–1323
Khoraki J, Gomez PP, Mazzini GS, Pessoa BM, Browning MG, Aquilina GR et al (2020) Perioperative outcomes and cost of robotic-assisted versus laparoscopic inguinal hernia repair. Surg Endosc 34:3496–3507
Kosturakis AK, LaRusso KE, Carroll ND, Nicholl MB (2018) First 100 consecutive robotic inguinal hernia repairs at a veterans affairs hospital. J Robot Surg 12:699–704
Kolachalam R, Dickens E, D’Amico L, Richardson C, Rabaza J, Gamagami R et al (2018) Early outcomes of robotic-assisted inguinal hernia repair in obese patients: a multi-institutional retrospective study. Surg Endosc 32:229–235
Kudsi OY, McCarty JC, Paluvoi N, Mabardy AS (2017) Transition from laparoscopic totally extraperitoneal inguinal hernia repair to robotic transabdominal preperitoneal inguinal hernia repair: a retrospective review of a single surgeon’s experience. World J Surg 41:2251–2257
LeBlanc K, Dickens E, Gonzalez A, Gamagami R, Pierce R, Balentine C et al (2020) Prospective, multicenter, pairwise analysis of robotic-assisted inguinal hernia repair with open and laparoscopic inguinal hernia repair: early results from the Prospective Hernia Study. Hernia 24:1069–1081
Abdelmoaty WF, Dunst CM, Neighorn C, Swanstrom LL, Hammill CW (2019) Robotic-assisted versus laparoscopic unilateral inguinal hernia repair: a comprehensive cost analysis. Surg Endosc 33:3436–3443
Mehaffey JH, Michaels AD, Mullen MG, Yount KW, Meneveau MO, Smith PW et al (2017) Adoption of robotics in a general surgery residency program: at what cost? J Surg Res 213:269–273
Mustafa S, Handren E, Farmer D, Ontiveros E, Ogola GO, Leeds SG (2019) Robotic curriculum enhances minimally invasive general surgery residents’ education. J Surg Educ 76:548–553
Muysoms F, Vierstraete M, Nachtergaele F, Van Garsse S, Pletinckx P, Ramaswamy A (2021) Economic assessment of starting robot-assisted laparoscopic inguinal hernia repair in a single-centre retrospective comparative study: the EASTER study. BJS Open 5:zraa046
Muysoms F, Van Cleven S, Kyle-Leinhase I, Ballecer C, Ramaswamy A (2018) Robotic-assisted laparoscopic groin hernia repair: observational case-control study on the operative time during the learning curve. Surg Endosc 32:4850–4859
Dhanani NH, Olavarria OA, Millas S, Askenasy EP, Ko TC, Liang MK et al (2020) Is robotic surgery feasible at a safety net hospital? Surg Endosc 35:4452–4458
Prabhu AS, Carbonell A, Hope W, Warren J, Higgins R, Jacob B et al (2020) Robotic inguinal vs transabdominal laparoscopic inguinal hernia repair: the RIVAL randomized clinical trial. JAMA Surg 155:380–387
Higgins RM, Frelich MJ, Bosler ME, Gould JC (2016) Cost analysis of robotic versus laparoscopic general surgery procedures. Surg Endosc 31:185–192
Rose ED, Modlin DM, Ciampa ML, Mangieri CW, Faler BJ, Bandera BC (2019) Evaluation of operative waste in a military medical center: analysis of operating room cost and waste during surgical cases. Am Surg 85:717–720
Saito T, Fukami Y, Uchino T, Kurahashi S, Matsumura T, Osawa T et al (2020) Preliminary results of robotic inguinal hernia repair following its introduction in a single-center trial. Ann Gastroenterol Surg 4:441–447
Sheldon RR, Do WS, Weiss JB, Forte DM, Sohn VY (2019) Sage wisdom or anecdotal dictum? Equivalent opioid use after open, laparoscopic, and robotic inguinal hernia repair. Am J Surg 217:839–842
AlMarzooqi R, Tish S, Huang L-C, Prabhu A, Rosen M (2019) Review of inguinal hernia repair techniques within the Americas Hernia Society Quality Collaborative. Hernia 23:429–438
Tatarian T, Nie L, McPartland C, Brown AM, Yang J, Altieri MS, et al (2021) Comparative perioperative and 5-year outcomes of robotic and laparoscopic or open inguinal hernia repair: a study of 153,727 patients in the state of New York. Surg Endosc. In press
Waite KE, Herman MA, Doyle PJ (2016) Comparison of robotic versus laparoscopic transabdominal preperitoneal (TAPP) inguinal hernia repair. J Robot Surg 10:239–244
Zayan NE, Meara MP, Schwartz JS, Narula VK (2019) A direct comparison of robotic and laparoscopic hernia repair: patient-reported outcomes and cost analysis. Hernia 23:1115–1121
Truong A, Al-Aufey BS, Towfigh S (2019) Step-by-step guide to safe removal of pre-peritoneal inguinal mesh. Surg Endosc 33:2680–2685
Bittner Iv JG, Cesnik LW, Kirwan T, Wolf L, Guo D (2018) Patient perceptions of acute pain and activity disruption following inguinal hernia repair: a propensity-matched comparison of robotic-assisted, laparoscopic, and open approaches. J Robot Surg 12:625–632
Pokala B, Armijo PR, Flores L, Hennings D, Oleynikov D (2019) Minimally invasive inguinal hernia repair is superior to open: a national database review. Hernia 23:593–599
Charles EJ, Mehaffey JH, Tache-Leon CA, Hallowell PT, Sawyer RG, Yang Z (2018) Inguinal hernia repair: is there a benefit to using the robot? Surg Endosc 32:2131–2136
Kakiashvili E, Bez M, Abu Shakra I, Ganam S, Bickel A, Merei F et al (2021) Robotic inguinal hernia repair: is it a new era in the management of inguinal hernia? Asian J Surg 44:93–98
Gamagami R, Dickens E, Gonzalez A, D’Amico L, Richardson C, Rabaza J et al (2018) Open versus robotic-assisted transabdominal preperitoneal (R-TAPP) inguinal hernia repair: a multicenter matched analysis of clinical outcomes. Hernia 22:827–836
Tracy BM, Finnegan TM, Smith RN, Senkowski CK (2020) Random forest modeling using socioeconomic distress predicts hernia repair approach. Surg Endosc 35:3890–3895
Huerta S, Timmerman C, Argo M, Favela J, Pham T, Kukreja S et al (2019) Open, laparoscopic, and robotic inguinal hernia repair: outcomes and predictors of complications. J Surg Res 241:119–127
Als-Nielsen B, Chen W, Gluud C, Kjaergard LL (2003) Association of funding and conclusions in randomized drug trials: a reflection of treatment effect or adverse events? J Am Med Assoc 290:921–928
Emerson GB, Warme WJ, Wolf FM, Heckman JD, Brand RA, Leopold SS (2010) Testing for the presence of positive-outcome bias in peer review: a randomized controlled trial. Arch Intern Med 170:1934–1939
Publications Output: U.S. trends and international comparisons | NSF—National Science Foundation. https://ncses.nsf.gov/pubs/nsb20206/executive-summary. Accessed 14 Nov 2021
Barrow JM, Brannan GD, Khandhar PB (2021) Research ethics. StatPearls 2021
Resnik DB, Shamoo AE (2011) The Singapore statement on research integrity. Account Res 18:71
Funding
The study received no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Mr. Hansen, Dr. Fonnes and Prof. Rosenberg have no conflicts of interest or financial tires to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hansen, D.L., Fonnes, S. & Rosenberg, J. Spin is present in the majority of articles evaluating robot-assisted groin hernia repair: a systematic review. Surg Endosc 36, 2271–2278 (2022). https://doi.org/10.1007/s00464-021-08990-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08990-1