Abstract
Background
There is a paucity of evidence surrounding the issue of delays on the day of surgery with respect to both causes and consequences. We sought to determine whether patients whose operations started late were at increased risk of post-operative complications.
Methods
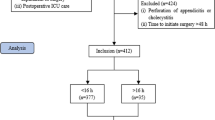
We conducted a retrospective cohort study of 1420 first-of-the-day common general surgical procedures, dividing these into “on-time start” (OTS) and “late-start” (LS) cases. Our primary outcomes were minor and major complication rate; our secondary objective was to identify factors predicting LS. Groups were compared using univariable and multivariable analysis.
Results
LS rate was 55.3%. On univariable analysis, LS had higher rates of major and minor complications (7.3% vs. 3.5%, p = 0.002; 3.8% vs. 1.6%, p = 0.011). On multivariable analysis, LS was not associated with increased odds of any complications. Minor complications were predicted by operative duration [OR = 1.005 (1.002–1.008)], female sex [OR = 1.78 (1.037–3.061)], and undergoing an ileostomy closure procedure [OR = 10.60 (2.791–40.246)], and were reduced in those undergoing surgery on Wednesdays [OR = 0.38 (0.166–0.876)]. Major complications were predicted by operative duration [OR = 1.007 (1.003–1.011)] and ASA class [OR = 6.73 (1.505–30.109)]. Multivariable analysis using LS as an outcome identified that anesthesia time [OR = 1.35 (1.031–1.403)], insulin-dependent diabetes [OR = 1.91 (1.128–3.246)], and dyspnea upon moderate exertion [OR = 2.52 (1.423–4.522)] were predictive of LS.
Conclusions
Most cases in our study started late. While this has significant efficiency and economic costs, it is not associated with adverse patient outcomes. This topic remains incompletely described. Further research is needed to improve efficiency and patient experience by investigating the causes of operative delays.


Similar content being viewed by others
References
Chen Y, Gabriel RA, Kodali BS, Urman RD (2016) Effect of anesthesia staffing ratio on first-case surgical start time. J Med Syst 40:115
van Veen-Berkx E, Elkhuizen SG, Kalkman CJ, Buhre WF, Kazemier G (2014) Successful interventions to reduce first-case tardiness in Dutch university medical centers: results of a nationwide operating room benchmark study. Am J Surg 207:949–959
Wright JG, Roche A, Khoury AE (2010) Improving on-time surgical starts in an operating room. Can J Surg 53:167–170
Mazzei WJ (1994) Operating room start times and turnover times in a university hospital. J Clin Anesth 6:405–408
Chu MW, Barr JS, Hill JB, Weichman KE, Karp NS, Levine JP (2015) Late-start days increase total operative time in microvascular breast reconstruction. J Reconstr Microsurg 31:401–406
Jallad K, Barber MD, Ridgeway B, Paraiso MF, Unger CA (2016) The effect of surgical start time in patients undergoing minimally invasive sacrocolpopexy. Int Urogynecol J 27:1535–1539
Funding
There are no funding or financial support sources to report for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Sami Chadi has received consulting and speaking honoraria from Stryker Endoscopy. Fayez Quereshy has received consulting and speaking honoraria from Minogue Medical and Medtronic. Keegan Guidolin and Kimberley Lam-Tin Cheung reported no financial interests or potential conflicts of interest.
Ethical approval
This study protocol was reviewed and approved by the University Health Network Institutional Research Ethics Board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Guidolin, K., Lam-Tin-Cheung, K., Chadi, S. et al. Starting late does not increase the risk of post-operative complications in patients undergoing common general surgical procedures. Surg Endosc 36, 3781–3788 (2022). https://doi.org/10.1007/s00464-021-08694-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08694-6