Abstract
Background
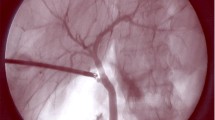
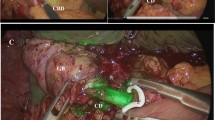
Laparoscopic cholecystectomy (LC) is the most common elective abdominal surgery in the USA, with over 750,000 performed annually. Fluorescent cholangiography (FC) using indocyanine green dye (ICG) permits identification of extrahepatic biliary structures to facilitate dissection without requiring cystic duct cannulation. Achieving the “critical view of safety” with assistance of ICG cholangiogram may support identification of anatomy, safely reduce conversion to open procedures, and decrease operative time. We assess the utility of FC with respect to anatomic visualization during LC and its effects on patient outcomes.
Methods
A retrospective review of a prospectively maintained database identified patients undergoing laparoscopic cholecystectomy at a single academic center from 2013 to 2019. Exclusion criteria were primary open and single incision cholecystectomy. Patient factors included age, sex, BMI, and Charlson Comorbidity Index. Outcomes included operative time, conversion to open procedure, length of stay (LOS), mortality rate, and 30-day complications. A multivariable logistic regression was performed to determine independent predictors for open conversion.
Results
A total of 1389 patients underwent laparoscopic cholecystectomy. 69.8% were female; mean age 48.6 years (range 15–94), average BMI 29.4 kg/m2 (13.3–55.6). 989 patients (71.2%) underwent LC without fluorescence and 400 (28.8%) underwent FC with ICG. 30-day mortality detected 2 cases in the non-ICG group and zero with ICG. ICG reduced operative time by 26.47 min per case (p < 0.0001). For patients with BMI ≥ 30 kg/m2, operative duration for ICG vs non-ICG groups was 75.57 vs 104.9 min respectively (p < 0.0001). ICG required conversion to open at a rate of 1.5%, while non-ICG converted at a rate of 8.5% (p < 0.0001). Conversion rate remained significant with multivariable analysis (OR 0.212, p = 0.001). A total of 19 cases were aborted (1.35%), 8 in the ICG group (1.96%) and 11 in the non-ICG group (1.10%), these cases were not included in LC totals. Average LOS was 0.69 vs 1.54 days in the ICG compared to non-ICG LCs (p < 0.0001), respectively. Injuries were more common in the non-ICG group, with 9 patients sustaining Strasberg class A injuries in the non-ICG group and 2 in the ICG group. 1 CBDI occurred in the non-ICG group. There was no significant difference in 30-day complication rates between groups.
Conclusion
ICG cholangiography is a non-invasive adjunct to laparoscopic cholecystectomy, leading to improved patient outcomes with respect to operative times, decreased conversion to open procedures, and shorter length of hospitalization. Fluorescence cholangiography improves visualization of biliary anatomy, thereby decreasing rate of CBDI, Strasberg A injuries, and mortality. These findings support ICG as standard of care during laparoscopic cholecystectomy.





Similar content being viewed by others
References
Flum DR, Dellinger EP, Cheadle A, Chan L, Koepsell T (2003) Intraoperative cholangiography and risk of common bile duct injury during cholecystectomy. J Am Med Assoc. https://doi.org/10.1001/jama.289.13.1639
Kohn JF, Trenk A, Kuchta K et al (2018) Characterization of common bile duct injury after laparoscopic cholecystectomy in a high-volume hospital system. Surg Endosc. https://doi.org/10.1007/s00464-017-5790-8
van de Graaf FW, Zaïmi I, Stassen LPS, Lange JF (2018) Safe laparoscopic cholecystectomy: a systematic review of bile duct injury prevention. Int J Surg. https://doi.org/10.1016/j.ijsu.2018.11.006
Tayeb M, Raza SA, Khan MR, Azami R (2005) Conversion from laparoscopic to open cholecystectomy: multivariate analysis of preoperative risk factors. J Postgrad Med 51(1):17–20
Zroback C, Chow G, Meneghetti A et al (2016) Fluorescent cholangiography in laparoscopic cholecystectomy: the initial Canadian experience. Am J Surg. https://doi.org/10.1016/j.amjsurg.2016.01.013
de Reuver PR, Sprangers MAG, Rauws EAJ et al (2008) Impact of bile duct injury after laparoscopic cholecystectomy on quality of life: a longitudinal study after multidisciplinary treatment. Endoscopy. https://doi.org/10.1055/s-2008-1077444
Lipman JM, Claridge JA, Haridas M et al (2007) Preoperative findings predict conversion from laparoscopic to open cholecystectomy. Surgery. https://doi.org/10.1016/j.surg.2007.07.010
Shah AA, Bhatti UF, Petrosyan M et al (2019) The heavy price of conversion from laparoscopic to open procedures for emergent cholecystectomies. Am J Surg. https://doi.org/10.1016/j.amjsurg.2018.12.038
Stefanidis D, Chintalapudi N, Anderson-Montoya B, Oommen B, Tobben D, Pimentel M (2017) How often do surgeons obtain the critical view of safety during laparoscopic cholecystectomy? Surg Endosc. https://doi.org/10.1007/s00464-016-4943-5
Aziz H, Pandit V, Joseph B, Jie T, Ong E (2015) Age and obesity are independent predictors of bile duct injuries in patients undergoing laparoscopic cholecystectomy. World J Surg. https://doi.org/10.1007/s00268-015-3010-z
Keus F, De Jong JAF, Gooszen HG, Van Laarhoven CJHM (2006) Laparoscopic versus small-incision cholecystectomy for patients with symptomatic cholecystolithiasis. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD006229
Keus F, De Jong JAF, Gooszen HG, Van Laarhoven CJHM (2006) Laparoscopic versus open cholecystectomy for patients with symptomatic cholecystolithiasis. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD006231
Strasberg SM, Hertl M, Soper NJ (1995) An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 180(1):101–125
Buddingh KT, Nieuwenhuijs VB, Van Buuren L, Hulscher JBF, De Jong JS, Van Dam GM (2011) Intraoperative assessment of biliary anatomy for prevention of bile duct injury: a review of current and future patient safety interventions. Surg Endosc. https://doi.org/10.1007/s00464-011-1639-8
Ishizawa T, Bandai Y, Ijichi M, Kaneko J, Hasegawa K, Kokudo N (2010) Fluorescent cholangiography illuminating the biliary tree during laparoscopic cholecystectomy. Br J Surg. https://doi.org/10.1002/bjs.7125
Dip FD, Asbun D, Rosales-Velderrain A et al (2014) Cost analysis and effectiveness comparing the routine use of intraoperative fluorescent cholangiography with fluoroscopic cholangiogram in patients undergoing laparoscopic cholecystectomy. Surg Endosc. https://doi.org/10.1007/s00464-013-3394-5
Bjerregaard J, Pandia MP, Jaffe RA (2013) Occurrence of severe hypotension after indocyanine green injection during the intraoperative period. A A Case Rep. https://doi.org/10.1097/acc.0b013e3182933c12
Chu W, Chennamsetty A, Toroussian R, Lau C (2017) Anaphylactic shock after intravenous administration of indocyanine green during robotic partial nephrectomy. Urol Case Rep. https://doi.org/10.1016/j.eucr.2017.02.006
Procter LD, Davenport DL, Bernard AC, Zwischenberger JB (2010) General surgical operative duration is associated with increased risk-adjusted infectious complication rates and length of hospital stay. J Am Coll Surg. https://doi.org/10.1016/j.jamcollsurg.2009.09.034
Buchs NC, Pugin F, Azagury DE et al (2013) Real-time near-infrared fluorescent cholangiography could shorten operative time during robotic single-site cholecystectomy. Surg Endosc. https://doi.org/10.1007/s00464-013-3005-5
Boni L, David G, Mangano A et al (2015) Clinical applications of indocyanine green (ICG) enhanced fluorescence in laparoscopic surgery. Surg Endosc. https://doi.org/10.1007/s00464-014-3895-x
Vlek SL, van Dam DA, Rubinstein SM et al (2017) Biliary tract visualization using near-infrared imaging with indocyanine green during laparoscopic cholecystectomy: results of a systematic review. Surg Endosc. https://doi.org/10.1007/s00464-016-5318-7
Esposito C, Corcione F, Settimi A et al (2019) Twenty-five year experience with laparoscopic cholecystectomy in the pediatric population—from 10 mm clips to indocyanine green fluorescence technology: long-term results and technical considerations. J Laparoendosc Adv Surg Tech. https://doi.org/10.1089/lap.2019.0254
Ballal M, David G, Willmott S, Corless DJ, Deakin M, Slavin JP (2009) Conversion after laparoscopic cholecystectomy in England. Surg Endosc. https://doi.org/10.1007/s00464-009-0338-1
Genc V, Sulaimanov M, Cipe G et al (2011) What necessitates the conversion to open cholecystectomy? A retrospective analysis of 5164 consecutive laparoscopic operations. Clinics. https://doi.org/10.1590/S1807-59322011000300009
Frank AP, De Souza SR, Palmer BF, Clegg DJ (2019) Determinants of body fat distribution in humans may provide insight about obesity-related health risks. J Lipid Res. https://doi.org/10.1194/jlr.R086975
Strasberg SM, Brunt LM (2017) The critical view of safety. Ann Surg. https://doi.org/10.1097/SLA.0000000000002054
Strasberg SM, Brunt LM (2010) Rationale and use of the critical view of safety in laparoscopic cholecystectomy. J Am Coll Surg. https://doi.org/10.1016/j.jamcollsurg.2010.02.053
Schols RM, Connell NJ, Stassen LPS (2015) Near-infrared fluorescence imaging for real-time intraoperative anatomical guidance in minimally invasive surgery: a systematic review of the literature. World J Surg. https://doi.org/10.1007/s00268-014-2911-6
Funding
Funding was provided via a grant from Stryker Corporation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
This study was conducted with a grant from Stryker Corporation. Dr. Santiago Horgan is a consultant for Stryker Corporation, Intuitive Surgical, Fortimedix Surgical, and Medtronic. Dr. Jacobsen receives a teaching honorarium from Gore Medical. Dr. Sandler is a consultant for Intuitive Surgical and Boston Scientific. Drs. Doucet, Broderick, Lee, Zhao, Blitzer, Patel, and Cheverie have no conflicts of interest or financial ties to disclose. Ms. Soltero has no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Ryan C. Broderick and Arielle M. Lee have shared co-first authorship.
Rights and permissions
About this article
Cite this article
Broderick, R.C., Lee, A.M., Cheverie, J.N. et al. Fluorescent cholangiography significantly improves patient outcomes for laparoscopic cholecystectomy. Surg Endosc 35, 5729–5739 (2021). https://doi.org/10.1007/s00464-020-08045-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-08045-x