Abstract
Background
Competency in endoscopy has traditionally been based on number of procedures performed. With movement towards milestone-based accreditation, new standards of establishing competency are required. The Thompson Endoscopic Skills Trainer (TEST) is a training device previously shown to differentiate between novice and expert endoscopists. This study aims to correlate TEST scores to other markers of performance in endoscopy.
Methods
Trainees of a gastroenterology fellowship program were guided through the TEST. Their scores and sub-scores were correlated to their endoscopic metrics of performance, including adenoma detection rate, cecal intubation rate, cecal intubation time, withdrawal time, fentanyl usage, midazolam usage, pain score, overall procedure time, and performance on the ASGE Assessment of Competency in Endoscopy Tool (ACE Tool).
Results
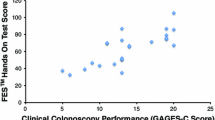
The Overall Score positively correlated with the ACE Tool Total Score (r = 0.707, p = 0.010) and sub-scores (Cognitive Skills Score: r = 0.624, p = 0.030; Motor Skills Score: r = 0.756, p = 0.004), and negatively correlated with cecal intubation time (r = − 0.591, p = 0.043). The Gross Motor Score positively correlated with cecal intubation rate (r = 0.593, p = 0.042), ACE Tool Total Score (r = 0.594, p = 0.042) and Motor Skills Score (r = 0.623, p = 0.031), and negatively correlated with cecal intubation time (r = − 0.695, p = 0.012). The Fine Motor Score positively correlated with the ACE Tool Polypectomy Score (r = 0.601, p = 0.039), and negatively correlated with procedure time (r = − 0.640, p = 0.025), cecal intubation time (r = − 0.645, p = 0.024), and withdrawal time (r = − 0.629, p = 0.028).
Conclusion
This study demonstrates that performance on the TEST correlate to endoscopic measures. Given these results, the TEST may be used in conjunction with existing assessment tools for demonstrating competency in endoscopy.




Similar content being viewed by others
References
Peery AF, Dellon ES, Lund J, Crockett SD, McGowan CE, Bulsiewicz WJ, Gangarosa LM, Thiny MT, Stizenberg K, Morgan DR, Ringel Y, Kim HP, Dibonaventura MD, Carroll CF, Allen JK, Cook SF, Sandler RS, Kappelman MD, Shaheen NJ (2012) Burden of gastrointestinal disease in the United States: 2012 update. Gastroenterology 143(1179–1187):e1171–1173
ASGE Training Committee (2004) Esophagogastroduodenoscopy (EGD) Core Curriculum.
Training Committee ASGE, Sedlack RE, Shami VM, Adler DG, Coyle WJ, DeGregorio B, Dua KS, DiMaio CJ, Lee LS, McHenry L Jr, Pais SA, Rajan E, Faulx AL (2012) Colonoscopy core curriculum. Gastrointest Endosc 76:482–490
Training Committee ASGE, Adler DG, Bakis G, Coyle WJ, DeGregorio B, Dua KS, Lee LS, McHenry L Jr, Pais SA, Rajan E, Sedlack RE, Shami VM, Faulx AL (2012) Principles of training in GI endoscopy. Gastrointest Endosc 75:231–235
Ward ST, Mohammed MA, Walt R, Valori R, Ismail T, Dunckley P (2014) An analysis of the learning curve to achieve competency at colonoscopy using the JETS database. Gut 63:1746–1754
Eckert LD, Short MW, Domagalski JE, Jaboori KA, Short PA (2009) Assessing colonoscopy training outcomes using quality indicators. J Grad Med Educ 1:89–92
Spier BJ, Benson M, Pfau PR, Nelligan G, Lucey MR, Gaumnitz EA (2010) Colonoscopy training in gastroenterology fellowships: determining competence. Gastrointest Endosc 71:319–324
Koch AD, Haringsma J, Schoon EJ, de Man RA, Kuipers EJ (2012) Competence measurement during colonoscopy training: the use of self-assessment of performance measures. Am J Gastroenterol 107:971–975
Sedlack RE, Coyle WJ, Group ACER (2016) Assessment of competency in endoscopy: establishing and validating generalizable competency benchmarks for colonoscopy. Gastrointest Endosc 83(516–523):e511
Nasca TJ, Philibert I, Brigham T, Flynn TC (2012) The next GME accreditation system–rationale and benefits. N Engl J Med 366:1051–1056
Patel SG, Keswani R, Elta G, Saini S, Menard-Katcher P, Del Valle J, Hosford L, Myers A, Ahnen D, Schoenfeld P, Wani S (2015) Status of competency-based medical education in endoscopy training: a Nationwide Survey of US ACGME-accredited gastroenterology training programs. Am J Gastroenterol 110:956–962
Training Committee ASGE, Sedlack RE, Coyle WJ, Obstein KL, Al-Haddad MA, Bakis G, Christie JA, Davila RE, DeGregorio B, DiMaio CJ, Enestvedt BK, Jorgensen J, Mullady DK, Rajan L (2014) ASGE's assessment of competency in endoscopy evaluation tools for colonoscopy and EGD. Gastrointest Endosc 79:1–7
Education ACfGM (2018) ACGME program requirements for graduate medical education in general surgery.
Gardner AK, Scott DJ, Pedowitz RA, Sweet RM, Feins RH, Deutsch ES, Sachdeva AK (2015) Best practices across surgical specialties relating to simulation-based training. Surgery 158:1395–1402
Stefanidis D, Sevdalis N, Paige J, Zevin B, Aggarwal R, Grantcharov T, Jones DB, Association for Surgical Education Simulation C (2015) Simulation in surgery: what's needed next? Ann Surg 261:846–853
Committee AT, Goodman AJ, Melson J, Aslanian HR, Bhutani MS, Krishnan K, Lichtenstein DR, Navaneethan U, Pannala R, Parsi MA, Schulman AR, Sethi A, Sullivan SA, Thosani N, Trikudanathan G, Trindade AJ, Watson RR, Maple JT (2019) Endoscopic simulators. Gastrointest Endosc 90:1–12
Cohen J, Thompson CC (2013) The next generation of endoscopic simulation. Am J Gastroenterol 108:1036–1039
Obstein KL, Patil VD, Jayender J, San-Jose-Estepar R, Spofford IS, Lengyel BI, Vosburgh KG, Thompson CC (2011) Evaluation of colonoscopy technical skill levels by use of an objective kinematic-based system. Gastrointest Endosc 73:315–321
Downing SM (2003) Validity: on meaningful interpretation of assessment data. Med Educ 37:830–837
Thompson CC, Jirapinyo P, Kumar N, Ou A, Camacho A, Lengyel B, Ryan MB (2014) Development and initial validation of an endoscopic part-task training box. Endoscopy 46:735–744
Jirapinyo P, Kumar N, Thompson CC (2015) Validation of an endoscopic part-task training box as a skill assessment tool. Gastrointest Endosc 81:967–973
Funding
No funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Amy Ou is named on the patent for the Thompson Endoscopic Skills Trainer, but receives no monetary compensation for its use or sale. Claire Shin, Adam J. Goodman, Michael A. Poles, and Violeta B. Popov have no conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ou, A., Shin, C.M., Goodman, A.J. et al. Endoscopic part-task training box scores correlate with endoscopic outcomes. Surg Endosc 35, 3592–3599 (2021). https://doi.org/10.1007/s00464-020-07830-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07830-y