Abstract
Background
Caudate lobectomy via laparoscopic surgery has rarely been described. This multicenter, propensity score-matched study was performed to assess the safety and efficacy of laparoscopic caudate lobectomy (LCL).
Methods
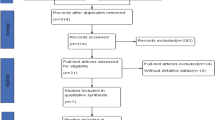
A multicenter retrospective study was performed including all patients who underwent LCL and open caudate lobectomy (OCL) in four institutions from January 2013 to December 2018. In total, 131 patients were included in this study and divided into LCL (n = 19) and OCL (n = 112) groups. LCLs were matched to OCLs (1:2) using a propensity score matching (PSM) based on nine preoperative variables, including patient demographics and tumor characteristics. The pathological results, perioperative and postoperative parameters, and short-term outcomes were compared between the two groups.
Results
After PSM, there were 18 and 36 patients in the LCL and OCL groups, respectively. Baseline characteristics were comparable after matching. LCL was associated with less blood (100 vs. 300 ml, respectively; P < 0.001) and a shorter postoperative stay (6.0 vs 8.0 days, respectively; P = 0.003). Most patients’ resection margins were > 10 mm in the LCL group (P = 0.021), and all patients with malignancy in both groups achieved R0 resection. In terms of early postoperative outcomes, the overall morbidity rate was identical in each group (11.1% vs. 11.1%, respectively; P = 1.000). No mortality occurred in either group.
Conclusions
Laparoscopy is a feasible choice for resection of tumors located in the caudate lobe with acceptable perioperative results.


Similar content being viewed by others
References
Reich H, McGlynn F, DeCaprio J, Budin R (1991) Laparoscopic excision of benign liver lesions. Obstet Gynecol 78:956–958
Cai X (2018) Laparoscopic liver resection: the current status and the future. Hepatobiliary Surg Nutr 7:98–104
Ciria R, Cherqui D, Geller DA, Briceno J, Wakabayashi G (2016) Comparative short-term benefits of laparoscopic liver resection: 9000 cases and climbing. Ann Surg 263:761–777
Jin B, Chen MT, Fei YT, Du SD, Mao YL (2018) Safety and efficacy for laparoscopic versus open hepatectomy: a meta-analysis. Surg Oncol 27:A26–a34
Kumon M (2017) Anatomical study of the caudate lobe with special reference to portal venous and biliary branches using corrosion liver casts and clinical application. Liver Cancer 6:161–170
Kosuge T, Yamamoto J, Takayama T, Shimada K, Yamasaki S, Makuuchi M, Hasegawa H (1994) An isolated, complete resection of the caudate lobe, including the paracaval portion, for hepatocellular carcinoma. Arch Surg 129:280–284
Lerut J, Gruwez JA, Blumgart LH (1990) Resection of the caudate lobe of the liver. Surg Gynecol Obstet 171:160–162
Dulucq JL, Wintringer P, Stabilini C, Mahajna A (2006) Isolated laparoscopic resection of the hepatic caudate lobe: surgical technique and a report of 2 cases. Surg Laparosc Endosc Percutan Tech 16:32–35
Araki K, Fuks D, Nomi T, Ogiso S, Lozano RR, Kuwano H, Gayet B (2016) Feasibility of laparoscopic liver resection for caudate lobe: technical strategy and comparative analysis with anteroinferior and posterosuperior segments. Surg Endosc 30:4300–4306
Oh D, Kwon CH, Na BG, Lee KW, Cho WT, Lee SH, Choi JY, Choi GS, Kim JM, Joh JW (2016) Surgical techniques for totally laparoscopic caudate lobectomy. J Laparoendosc Adv Surg Tech A 26:689–692
Ho KM, Han HS, Yoon YS, Cho JY, Choi YR, Jang JS, Kwon SU, Kim S, Choi JK (2017) Laparoscopic total caudate lobectomy for hepatocellular carcinoma. J Laparoendosc Adv Surg Tech A 27:1074–1078
Cai X, Li Z, Yu H, Liu K, Liang X, Wang Y, Liang Y (2014) Isolated laparoscopic resection of the hepatic caudate lobe. Chin Med J (Engl) 127:3194–3195
D'Agostino RB Jr (1998) Propensity score methods for bias reduction in the comparison of a treatment to a non-randomized control group. Stat Med 17:2265–2281
Yamamoto J, Kosuge T, Shimada K, Yamasaki S, Takayama T, Makuuchi M (1999) Anterior transhepatic approach for isolated resection of the caudate lobe of the liver. World J Surg 23:97–101
Bartlett D, Fong Y, Blumgart LH (1996) Complete resection of the caudate lobe of the liver: technique and results. Br J Surg 83:1076–1081
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Jacobs JP, Mavroudis C, Jacobs ML, Maruszewski B, Tchervenkov CI, Lacour-Gayet FG, Clarke DR, Yeh T Jr, Walters HL 3rd, Kurosawa H, Stellin G, Ebels T, Elliott MJ (2006) What is operative mortality? Defining death in a surgical registry database: a report of the STS Congenital Database Taskforce and the Joint EACTS-STS Congenital Database Committee. Ann Thorac Surg 81:1937–1941
Koffron AJ, Auffenberg G, Kung R, Abecassis M (2007) Evaluation of 300 minimally invasive liver resections at a single institution: less is more. Ann Surg 246:385–392 (discussion 392–384)
Kokkalera U, Ghellai A, Vandermeer TJ (2007) Laparoscopic hepatic caudate lobectomy. J Laparoendosc Adv Surg Tech A 17:36–38
Ishizawa T, Gumbs AA, Kokudo N, Gayet B (2012) Laparoscopic segmentectomy of the liver: from segment I to VIII. Ann Surg 256:959–964
Kyriakides C, Panagiotopoulos N, Jiao LR (2012) Isolated laparoscopic caudate lobe resection. Surg Laparosc Endosc Percutan Tech 22:e209
Chen KH, Jeng KS, Huang SH, Chu SH (2013) Laparoscopic caudate hepatectomy for cancer—an innovative approach to the no-man's land. J Gastrointest Surg 17:522–526
Gringeri E, Boetto R, Bassi D, D'Amico FE, Polacco M, Romano M, Barbieri S, Feltracco P, Spampinato M, Zanus G, Cillo U (2014) Totally laparoscopic caudate lobe resection: technical aspects and literature review. Surg Laparosc Endosc Percutan Tech 24:e233–236
Zarzavadjian Le Bian A, Borie F (2015) Caudate lobe resection: the laparoscopic approach (with video). J Visc Surg 152:135–136
Cai X, Zhao J, Wang Y, Yu H, Liang X, Jin R, Meng N, Chen J (2016) A left-sided, purely laparoscopic approach for anatomic caudate hepatectomy: a single-center experience. J Laparoendosc Adv Surg Tech A 26:103–108
Cheung TT (2016) Technical notes on pure laparoscopic isolated caudate lobectomy for patient with liver cancer. Transl Gastroenterol Hepatol 1:56
Salloum C, Lahat E, Lim C, Doussot A, Osseis M, Compagnon P, Azoulay D (2016) Laparoscopic isolated resection of caudate lobe (segment 1): a safe and versatile technique. J Am Coll Surg 222:e61–66
Chai S, Zhao J, Zhang Y, Xiang S, Zhang W (2018) Arantius ligament suspension: a novel technique for retraction of the left lateral lobe liver during laparoscopic isolated caudate lobectomy. J Laparoendosc Adv Surg Tech A 28:740–744
Jin B, Jiang Z, Hu S, Du G, Shi B, Kong D, Yang J (2018) Surgical technique and clinical analysis of twelve cases of isolated laparoscopic resection of the hepatic caudate lobe. Biomed Res Int 2018:5848309
Machado MA, Surjan R, Basseres T, Makdissi F (2018) Laparoscopic resection of caudate lobe. Technical strategies for a difficult liver segment—video article. Surg Oncol 27:674–675
Liu F, Wei Y, Li B (2019) Laparoscopic isolated total caudate lobectomy for hepatocellular carcinoma located in the paracaval portion of the cirrhotic liver. Ann Surg Oncol 26:2980
Siming Z, Jie Z, Hong L, Haibiao W (2019) Laparoscopic caudate lobe resection for the treatment of hepatolithiasis. J Minim Access Surg. https://doi.org/10.4103/jmas.jmas_194_18
Rowe AJ, Meneghetti AT, Schumacher PA, Buczkowski AK, Scudamore CH, Panton ON, Chung SW (2009) Perioperative analysis of laparoscopic versus open liver resection. Surg Endosc 23:1198–1203
Tsinberg M, Tellioglu G, Simpfendorfer CH, Walsh RM, Vogt D, Fung J, Berber E (2009) Comparison of laparoscopic versus open liver tumor resection: a case-controlled study. Surg Endosc 23:847–853
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection—2,804 patients. Ann Surg 250:831–841
Chaib E, Ribeiro MA Jr, Silva Fde S, Saad WA, Cecconello I (2008) Caudate lobectomy: tumor location, topographic classification, and technique using right- and left-sided approaches to the liver. Am J Surg 196:245–251
Sasada A, Ataka K, Tsuchiya K, Yamagishi H, Maeda H, Okada M (1998) Complete caudate lobectomy: its definition, indications, and surgical approaches. HPB Surg 11:87–93 (discussion 93–85)
Asahara T, Dohi K, Hino H, Nakahara H, Katayama K, Itamoto T, Ono E, Moriwaki K, Yuge O, Nakanishi T, Kitamoto M (1998) Isolated caudate lobectomy by anterior approach for hepatocellular carcinoma originating in the paracaval portion of the caudate lobe. J Hepatobiliary Pancreat Surg 5:416–421
Takayama T, Tanaka T, Higaki T, Katou K, Teshima Y, Makuuchi M (1994) High dorsal resection of the liver. J Am Coll Surg 179:72–75
Soubrane O, Schwarz L, Cauchy F, Perotto LO, Brustia R, Bernard D, Scatton O (2015) A conceptual technique for laparoscopic right hepatectomy based on facts and oncologic principles: the caudal approach. Ann Surg 261:1226–1231
Ogiso S, Nomi T, Araki K, Conrad C, Hatano E, Uemoto S, Fuks D, Gayet B (2015) Laparoscopy-specific surgical concepts for hepatectomy based on the laparoscopic caudal view: a key to reboot surgeons' minds. Ann Surg Oncol 22(Suppl 3):S327–S333
Kim J, Ahmad SA, Lowy AM, Buell JF, Pennington LJ, Soldano DA, James LE, Matthews JB, Hanto DW (2003) Increased biliary fistulas after liver resection with the harmonic scalpel. Am Surg 69:815–819
Aragon RJ, Solomon NL (2012) Techniques of hepatic resection. J Gastrointest Oncol 3:28–40
Polignano FM, Quyn AJ, de Figueiredo RS, Henderson NA, Kulli C, Tait IS (2008) Laparoscopic versus open liver segmentectomy: prospective, case-matched, intention-to-treat analysis of clinical outcomes and cost effectiveness. Surg Endosc 22:2564–2570
Jia C, Li H, Wen N, Chen J, Wei Y, Li B (2018) Laparoscopic liver resection: a review of current indications and surgical techniques. Hepatobiliary Surg Nutr 7:277–288
Kao CW, Wu SC, Lin KC, Chen CL, Huang CJ, Cheng KW, Jawan B, Wang CH (2012) Pain management of living liver donors with morphine with or without ketorolac. Transplant Proc 44:360–362
Vanounou T, Steel JL, Nguyen KT, Tsung A, Marsh JW, Geller DA, Gamblin TC (2010) Comparing the clinical and economic impact of laparoscopic versus open liver resection. Ann Surg Oncol 17:998–1009
Acknowledgements
The authors would like to thank Angela Morben, Ph.D, from Liwen Bianji, Edanz Editing China (www.liwenbianji.cn/ac), for editing the English text of a draft of this manuscript.
Funding
This research was supported by National Natural Science Foundation of China (Grant No. 81972698), CAMS Initiative for Innovative Medicine (Grant No. CAMS-2017-I2M-4-002) and Peking Union Medical College Graduate Student Innovation Fund (Grant No. 2019-1002-45).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Drs. Gang Xu, Junxiang Tong, Jiajun Ji, Hongguang Wang, Xiang’an Wu, Bao Jin, Haifeng Xu, Xin Lu, Xinting Sang, Yilei Mao, Shunda Du and Zhixiang Hong have no conflict of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Xu, G., Tong, J., Ji, J. et al. Laparoscopic caudate lobectomy: a multicenter, propensity score-matched report of safety, feasibility, and early outcomes. Surg Endosc 35, 1138–1147 (2021). https://doi.org/10.1007/s00464-020-07478-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07478-8