Abstract
Objectives
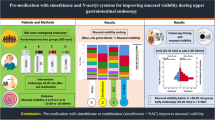
Early cancer detection is crucial in improving the patients’ quality of life and upper gastrointestinal endoscopy (EGD) plays a key role in this detection. Many clearing mechanisms may be applied to create good endoscopic visualizations for the upper gastrointestinal tract using mucolytic agents, antifoaming agents, proteolytic enzymes and neutralizers. The aim of this study is to compare the effects of simethicone, N-acetylcysteine (NAC), sodium bicarbonate and peppermint as pre-medications for visualization of esophagogastroduodenoscopy (EGD).
Methods
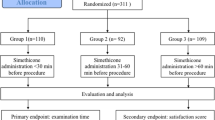
This study was a single center prospective randomized controlled trial. The patients were randomly allocated to one of four treatment groups. Group A: water; Group B: water with simethicone; Group C: water with simethicone plus NAC 600 mg; Group D: water with simethicone, NAC, sodium bicarbonate and peppermint.
Results
A total of 128 patients were enrolled and evaluated in this study. Total visibility score (TVS) of Groups A, B, C, and D were 13.4 ± 1.86, 10.5 ± 1.45, 7.15 ± 0.98 and 6.4 ± 1.43, respectively. Group D showed lower TVS than other groups. The procedural durations of Groups C and D were significantly shorter than Group A. The volume of solution for mucosal cleansing of Groups C and D was significantly lower than Groups A and B.
Conclusions
The application of simethicone plus NAC is safe, improves endoscopic visualization and requires a minimal amount of mucosal cleansing solution. The addition of sodium bicarbonate and peppermint further improved visualization for the upper and lower gastric body.
Thai Clinical Trials Registry (TCTR) with a reference number; TCTR20190501002.

Similar content being viewed by others
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6):394–424
Ferlay J, Colombet M, Soerjomataram I et al (2019) Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer 144(8):1941–1953
Hawkes N (2019) Cancer survival data emphasise importance of early diagnosis. BMJ 364:l408. https://doi.org/10.1136/bmj.l408
Cheung D, Menon S, Hoare J, Dhar A, Trudgill N (2016) Factors associated with upper gastrointestinal cancer occurrence after endoscopy that did not diagnose cancer. Dig Dis Sci 61(9):2674–2684
Jun JK, Choi KS, Lee HY et al (2017) Effectiveness of the Korean National Cancer Screening Program in reducing gastric cancer mortality. Gastroenterology 152(6):1319–2132
Busweiler LA, Wijnhoven BP, van Berge Henegouwen MI et al (2016) Early outcomes from the Dutch Upper Gastrointestinal Cancer Audit. Br J Surg 103(13):1855–1863
Veitch AM, Uedo N, Yao K, East JE (2015) Optimizing early upper gastrointestinal cancer detection at endoscopy. Nat Rev Gastroenterol Hepatol 12(11):660–667
Sumiyama K (2017) Past and current trends in endoscopic diagnosis for early stage gastric cancer in Japan. Gastric Cancer 20(Suppl 1):20–27
Chiu PWY, Uedo N, Singh R et al (2019) An Asian consensus on standards of diagnostic upper endoscopy for neoplasia. Gut 68(2):186–197
Ro TH, Mathew MA, Misra S (2015) Value of screening endoscopy in evaluation of esophageal, gastric and colon cancers. World J Gastroenterol 21(33):9693–9706
Yalamarthi S, Witherspoon P, McCole D, Auld CD (2004) Missed diagnoses in patients with upper gastrointestinal cancers. Endoscopy 36(10):874–879
Raftopoulos SC, Segarajasingam DS, Burke V, Ee HC, Yusoff IF (2010) A cohort study of missed and new cancers after esophagogastroduodenoscopy. Am J Gastroenterol 105(6):1292–1297
Telford JJ, Enns RA (2010) Endoscopic missed rates of upper gastrointestinal cancers: parallels with colonoscopy. Am J Gastroenterol 105(6):1298–1300
Menon S, Trudgill N (2014) How commonly is upper gastrointestinal cancer missed at endoscopy? A meta-analysis. Endosc Int Open 2(2):E46–E50
Pimenta-Melo AR, Monteiro-Soares M, Libânio D, Dinis-Ribeiro M (2016) Missing rate for gastric cancer during upper gastrointestinal endoscopy: a systematic review and meta-analysis. Eur J Gastroenterol Hepatol 28(9):1041–1049
Keeratichananont S, Sobhonslidsuk A, Kitiyakara T, Achalanan N, Soonthornpun S (2010) The role of liquid simethicone in enhancing endoscopic visibility prior to esophagogastroduodenoscopy (EGD): a prospective, randomized, double-blinded, placebo-controlled trial. J Med Assoc Thail 93(8):892–897
Wu L, Cao Y, Liao C, Huang J, Gao F (2011) Systematic review and meta-analysis of randomized controlled trials of Simethicone for gastrointestinal endoscopic visibility. Scand J Gastroenterol 46(2):227–235
Chen HW, Hsu HC, Hsieh TY, Yeh MK, Chang WK (2014) Pre-medication to improve esophagogastroduodenoscopic visibility: a meta-analysis and systemic review. Hepatogastroenterology 61(134):1642–1648
Monrroy H, Vargas JI, Glasinovic E et al (2018) Use of N-acetylcysteine plus simethicone to improve mucosal visibility during upper GI endoscopy: a double-blind, randomized controlled trial. Gastrointest Endosc 87(4):986–993
Elvas L, Areia M, Brito D, Alves S, Saraiva S, Cadime AT (2017) Premedication with simethicone and N-acetylcysteine in improving visibility during upper endoscopy: a double-blind randomized trial. Endoscopy 49(2):139–145
Neale JR, James S, Callaghan J, Patel P (2013) Premedication with N-acetylcysteine and simethicone improves mucosal visualization during gastroscopy: a randomized, controlled, endoscopist-blinded study. Eur J Gastroenterol Hepatol 25(7):778–783
Basford PJ, Brown J, Gadeke L et al (2016) A randomized controlled trial of pre-procedure simethicone and N-acetylcysteine to improve mucosal visibility during gastroscopy—NICEVIS. Endosc Int Open 4(11):E1197–E1202
Spinzi G, Andrealli A, Conforti FS (2018) Use of N-acetylcysteine plus simethicone to improve mucosal visibility during upper GI endoscopy. Gastrointest Endosc 88(3):575
Zhang LY, Li WY, Ji M et al (2018) Efficacy and safety of using premedication with simethicone/Pronase during upper gastrointestinal endoscopy examination with sedation: a single center, prospective, single blinded, randomized controlled trial. Dig Endosc 30(1):57–64
Kim GH, Cho YK, Cha JM, Lee SY, Chung IK (2015) Effect of pronase as mucolytic agent on imaging quality of magnifying endoscopy. World J Gastroenterol 21(8):2483–2489
Lee GJ, Park SJ, Kim SJ, Kim HH, Park MI, Moon W (2012) Effectiveness of premedication with pronase for visualization of the mucosa during endoscopy: a randomized, controlled trial. Clin Endosc 45(2):161–164
Liu X, Guan CT, Xue LY et al (2018) Effect of premedication on lesion detection rate and visualization of the mucosa during upper gastrointestinal endoscopy: a multicenter large sample randomized controlled double-blind study. Surg Endosc 32(8):3548–3556
Chang CC, Chen SH, Lin CP et al (2007) Premedication with pronase or N-acetylcysteine improves visibility during gastroendoscopy: an endoscopist-blinded, prospective, randomized study. World J Gastroenterol 13(3):444–447
Kuo CH, Sheu BS, Kao AW, Wu CH, Chuang CH (2002) A defoaming agent should be used with pronase premedication to improve visibility in upper gastrointestinal endoscopy. Endoscopy 34(7):531–534
Fujii T, Iishi H, Tatsuta M et al (1998) Effectiveness of premedication with pronase for improving visibility during gastroendoscopy: a randomized controlled trial. Gastrointest Endosc 47(5):382–387
Hiki N, Kurosaka H, Tatsutomi Y et al (2003) Peppermint oil reduces gastric spasm during upper endoscopy: a randomized, double-blind, double-dummy controlled trial. Gastrointest Endosc 57(4):475–482
Hikichi T, Irisawa A, Sato M et al (2011) Utility of peppermint oil for endoscopic diagnosis of gastric tumors. Fukushima J Med Sci 57(2):60–65
Imagawa A, Hata H, Nakatsu M et al (2012) Peppermint oil solution is useful as an antispasmodic drug for esophagogastroduodenoscopy, especially for elderly patients. Dig Dis Sci 57(9):2379–2384
The Paris endoscopic classification of superficial neoplastic lesions: esophagus, stomach, and colon: November 30 to December 1, 2002 (2003). Gastrointest Endosc 58(6 Suppl):S3–S43
Woo JG, Kim TO, Kim HJ et al (2013) Determination of the optimal time for premedication with pronase, dimethylpolysiloxane, and sodium bicarbonate for upper gastrointestinal endoscopy. J Clin Gastroenterol 47(5):389–392
Acknowledgements
The authors would like to thank Norman Mangnall for assistance in editing the English version of this manuscript and Dr. Saritphat Orrapin for scrutinizing methodology and for statistical consultation.
Funding
This research was supported by Faculty of Medicine, Thammasat University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Prasit Mahawongkajit and Dr. Amonpon Kanlerd have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mahawongkajit, P., Kanlerd, A. A prospective randomized controlled trial comparing simethicone, N-acetylcysteine, sodium bicarbonate and peppermint for visualization in upper gastrointestinal endoscopy. Surg Endosc 35, 303–308 (2021). https://doi.org/10.1007/s00464-020-07397-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07397-8