Abstract
Background
Robotic technology has become increasingly prevalent throughout modern surgical practice as surgical training programs are determining how to best include this robotic training in their curricula. In this study, we sought to measure changes in performance and workload metrics in the live operative setting following completion of a novel simulator-based robotic skills curriculum.
Methods
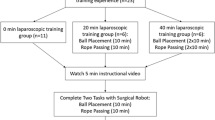
31 surgical residents naïve to robotic platforms were recruited. They first participated in a live robotic case and had a baseline assessment using RO-SCORE, a robotic modification of the O-SCORE tool, and self-assessed their workload using the NASA Task Load Index (NTLX). Subjects then completed the curriculum, created by an expert panel, on a da Vinci Skills Simulator to pre-set proficiency goals. Subjects were encouraged to train on their own time and could complete the curriculum in one or more sittings, in a 1-month time period. Subjects were then assessed after another live case. Data were analyzed using paired Student’s t test.
Results
Completion of the curriculum was associated with significant RO-SCORE improvements in operative performance across all domains including Camera Control (pre-curriculum mean: 1.9; post-curriculum mean: 4.8; p < 0.001), Needle Control (pre-curriculum mean: 1.7; post-curriculum mean: 4.4; p < 0.001), Tissue Handling (pre-curriculum mean: 2.0; post-curriculum mean: 4.4; p < 0.001). There were significant reductions in all NTLX workload domains including Physical Demand (pre-curriculum mean: 5.2; post-curriculum mean: 2.1; p < 0.001), and Frustration (pre-curriculum mean: 6.4; post-curriculum mean: 1.42; p < 0.001).
Conclusions
We describe a feasible robotic simulation curriculum that requires a reasonable amount of time and is self-directed. Significant improvements were seen across all performance metrics and subjective operator workload. Importantly, this is translated to the clinical environment. These types of curricula will be necessary for improving the skills and confidence of trainees and attending surgeons as robotic technology becomes more pervasive.



Similar content being viewed by others
References
Brody F, Richards NG (2014) Review of robotic versus conventional laparoscopic surgery. Surg Endosc 28:1413–1424
Amodeo A, Linares Quevedo A, Joseph JV, Belgrano E, Patel HRH (2009) Robotic laparoscopic surgery: cost and training. Minerva Urol Nefrol 61:121–128
Zihni A, Ge T, Ray S, Wang R, Liang Z, Cavallo JA, Awad MM (2016) Transfer and priming of surgical skills across minimally invasive surgical platforms. J Surg Res 206:48–52. https://doi.org/10.1016/j.jss.2016.06.026
Tanaka A, Graddy C, Simpson K, Perez M, Truong M, Smith R (2016) Robotic surgery simulation validity and usability comparative analysis. Surg Endosc 30:3720–3729. https://doi.org/10.1007/s00464-015-4667-y
Mills JT, Hougen HY, Bitner D, Krupski TL, Schenkman NS (2017) Does robotic surgical simulator performance correlate with surgical skill? J Surg Educ 74:1052–1056. https://doi.org/10.1016/j.jsurg.2017.05.011
Sullivan GM (2011) Deconstructing quality in education research. J Grad Med Educ 3:121–124. https://doi.org/10.4300/JGME-D-11-00083.1
Yardley S, Dornan T (2012) Kirkpatrick’s levels and education “evidence”. Med Educ 46:97–106
Guru KA, Shafiei SB, Khan A, Hussein AA, Sharif M, Esfahani ET (2015) Understanding cognitive performance during robot-assisted surgery. Urology 86:751–757. https://doi.org/10.1016/j.urology.2015.07.028
Ruiz-Rabelo JF, Navarro-Rodriguez E, Di-Stasi LL, Diaz-Jimenez N, Cabrera-Bermon J, Diaz-Iglesias C, Gomez-Alvarez M, Briceño-Delgado J (2015) Validation of the NASA-TLX Score in ongoing assessment of mental workload during a laparoscopic learning curve in bariatric surgery. Obes Surg 25:2451–2456. https://doi.org/10.1007/s11695-015-1922-1
Yurko YY, Scerbo MW, Prabhu AS, Acker CE, Stefanidis D (2010) Higher mental workload is associated with poorer laparoscopic performance as measured by the NASA-TLX tool. Simul Healthc 5:267–271. https://doi.org/10.1097/SIH.0b013e3181e3f329
Gofton WT, Dudek NL, Wood TJ, Balaa F, Hamstra SJ (2012) The Ottawa Surgical Competency Operating Room Evaluation (O-SCORE): a tool to assess surgical competence. Acad Med 87:1401–1407. https://doi.org/10.1097/ACM.0b013e3182677805
MacEwan MJ, Dudek NL, Wood TJ, Gofton WT (2016) Continued validation of the O-SCORE (Ottawa Surgical Competency Operating Room Evaluation): use in the simulated environment. Teach Learn Med 28:72–79. https://doi.org/10.1080/10401334.2015.1107483
Hart SG, Staveland LE (1988) Development of NASA-TLX (task load index): results of empirical and theoretical research. Adv Psychol 52:139–183. https://doi.org/10.1016/S0166-4115(08)62386-9
Stefanidis D, Wang F, Korndorffer JR, Dunne JB, Scott DJ (2010) Robotic assistance improves intracorporeal suturing performance and safety in the operating room while decreasing operator workload. Surg Endosc 24:377–382. https://doi.org/10.1007/s00464-009-0578-
Dulan G, Rege RV, Hogg DC, Gilberg-Fisher KM, Arain NA, Tesfay ST, Scott DJ (2012) Proficiency-based training for robotic surgery: construct validity, workload, and expert levels for nine inanimate exercises. Surg Endosc 26:1516–1521. https://doi.org/10.1007/s00464-011-2102-6
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Michael Awad: Intuitive research grant (on unrelated project); speaker’s bureau. William Gerull and Ahmed Zihni have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gerull, W., Zihni, A. & Awad, M. Operative performance outcomes of a simulator-based robotic surgical skills curriculum. Surg Endosc 34, 4543–4548 (2020). https://doi.org/10.1007/s00464-019-07243-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07243-6