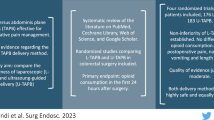
Abstract
Background
The transversus abdominis plane (TAP) block is an important non-narcotic adjunct for post-operative pain control in abdominal surgery. Surgeons can use laparoscopic guidance for TAP block placement (LTAP), however, direct comparisons to conventional ultrasound-guided TAP (UTAPs) have been lacking. The aim of this study is to determine if surgeon placed LTAPs were non-inferior to anesthesia placed UTAPs for post-operative pain control in laparoscopic colorectal surgery.
Methods
This was a prospective, randomized, patient and observer blinded parallel-arm non-inferiority trial conducted at a single tertiary academic center between 2016 and 2018 on adult patients undergoing laparoscopic colorectal surgery. Narcotic consumption and pain scores were compared for LTAP vs. UTAP for 48 h post-operatively.
Results
60 patients completed the trial (31 UTAP, 29 LTAP) of which 25 patients were female (15 UTAP, 10 LTAP) and the mean ages (SD) were 60.0 (13.6) and 61.5 (14.3) in the UTAP and LTAP groups, respectively. There was no significant difference in post-operative narcotic consumption between UTAP and LTAP at the time of PACU discharge (median [IQR] milligrams of morphine, 1.8 [0–4.5] UTAP vs. 0 [0–8.7] LTAP P = .32), 6 h post-operatively (5.4 [1.8–17.1] UTAP vs. 3.6 [0–12.6] LTAP P = .28), at 12 h post-operatively (9.0 [3.6–29.4] UTAP vs. 7.2 [0.9–22.5] LTAP P = .51), at 24 h post-operatively (9.0 [3.6–29.4] UTAP vs. 7.2 [0.9–22.5] LTAP P = .63), and 48 h post-operatively (39.9 [7.5–70.2] UTAP vs. 22.2 [7.5–63.8] LTAP P = .41). Patient-reported pain scores as well as pre-, intra-, and post-operative course were similar between groups. Non-inferiority criteria were met at all post-op time points up to and including 24 h but not at 48 h.
Conclusions
Surgeon-delivered LTAPs are safe, effective, and non-inferior to anesthesia-administered UTAPs in the immediate post-operative period.
Trial registry
The trial was registered at clinicaltrials.gov Identifier NCT03577912.




Similar content being viewed by others
Change history
18 March 2020
The following text should have been included in the Acknowledgments:
References
Spanjerberg W, Reurings J, Keus F, Cjhm VL (2011) Fast track surgery versus conventional recovery strategies for colorectal surgery. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD007635.pub2
Zhuang C-L, Ye X-Z, Zhang X-D et al (2013) Enhanced recovery after surgery programs versus traditional care for colorectal surgery. Dis Colon Rectum 56:667–678. https://doi.org/10.1097/DCR.0b013e3182812842
Lee L, Mata J, Ghitulescu GA et al (2015) Cost-effectiveness of enhanced recovery versus conventional perioperative management for colorectal surgery. Ann Surg 262:1026–1033. https://doi.org/10.1097/SLA.0000000000001019
Carmichael JC, Keller DS, Baldini G et al (2017) Clinical practice guidelines for enhanced recovery after colon and rectal surgery from the American Society of Colon and Rectal Surgeons and Society of American Gastrointestinal and Endoscopic Surgeons. Dis Colon Rectum 60:761–784. https://doi.org/10.1097/DCR.0000000000000883
Wick EC, Grant MC, Wu CL (2017) Postoperative multimodal analgesia pain management with nonopioid analgesics and techniques a review. JAMA Surg 152:691–697. https://doi.org/10.1001/jamasurg.2017.0898
Hain E, Maggiori L, Prost à la Denise J, Panis Y (2018) Transversus abdominis plane (TAP) block in laparoscopic colorectal surgery improves postoperative pain management: a meta-analysis. Color Dis 20:279–287. https://doi.org/10.1111/codi.14037
Johns N, O’Neill S, Ventham NT et al (2012) Clinical effectiveness of transversus abdominis plane (TAP) block in abdominal surgery: a systematic review and meta-analysis. Color Dis 14:635–642. https://doi.org/10.1111/j.1463-1318.2012.03104.x
Favuzza J, Brady K, Delaney CP (2013) Transversus abdominis plane blocks and enhanced recovery pathways: making the 23-h hospital stay a realistic goal after laparoscopic colorectal surgery. Surg Endosc Other Interv Tech 27:2481–2486. https://doi.org/10.1007/s00464-012-2761-y
Pirrera B, Alagna V, Lucchi A et al (2017) Transversus abdominis plane (TAP) block versus thoracic epidural analgesia (TEA) in laparoscopic colon surgery in the ERAS program. Surg Endosc Other Interv Tech. https://doi.org/10.1007/s00464-017-5686-7
Elkassabany N, Ahmed M, Malkowicz SB et al (2013) Comparison between the analgesic efficacy of transversus abdominis plane (TAP) block and placebo in open retropubic radical prostatectomy: a prospective, randomized, double-blinded study. J Clin Anesth 25:459–465. https://doi.org/10.1016/j.jclinane.2013.04.009
Jadon A, Jain P, Chakraborty S et al (2018) Role of ultrasound guided transversus abdominis plane block as a component of multimodal analgesic regimen for lower segment caesarean section: a randomized double blind clinical study. BMC Anesthesiol 18:1–7. https://doi.org/10.1186/s12871-018-0512-x
Gao T, Zhang JJ, Xi FC et al (2017) Evaluation of transversus abdominis plane (TAP) block in hernia surgery. Clin J Pain 33:369–375. https://doi.org/10.1097/AJP.0000000000000412
McDermott G, Korba E, Mata U et al (2012) Should we stop doing blind transversus abdominis plane blocks? Br J Anaesth 108:499–502. https://doi.org/10.1093/bja/aer422
Favuzza J, Delaney CP (2013) Laparoscopic-guided transversus abdominis plane block for colorectal surgery. Dis Colon Rectum 56:389–391. https://doi.org/10.1097/DCR.0b013e318280549b
Park SY, Park JS, Choi GS et al (2017) Comparison of analgesic efficacy of laparoscope-assisted and ultrasound-guided transversus abdominis plane block after laparoscopic colorectal operation: a randomized, single-blind, non-inferiority trial. J Am Coll Surg 225:403–410. https://doi.org/10.1016/j.jamcollsurg.2017.05.017
Fields AC, Gonzalez DO, Chin EH et al (2015) Laparoscopic-assisted transversus abdominis plane block for postoperative pain control in laparoscopic ventral hernia repair: a randomized controlled trial. J Am Coll Surg 221:462–469. https://doi.org/10.1016/j.jamcollsurg.2015.04.007
Elamin G, Waters PS, Hamid H et al (2015) Efficacy of a laparoscopically delivered transversus abdominis plane block technique during elective laparoscopic cholecystectomy: a prospective, double-blind randomized trial. J Am Coll Surg 221:335–344. https://doi.org/10.1016/j.jamcollsurg.2015.03.030
Zaghiyan KN, Mendelson BJ, Eng MR et al (2019) Randomized clinical trial comparing laparoscopic versus ultrasound-guided transversus abdominis plane block in minimally invasive colorectal surgery. Dis Colon Rectum 62:203–210. https://doi.org/10.1097/DCR.0000000000001292
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213. https://doi.org/10.1097/01.sla.0000133083.54934.ae
Schumi J, Wittes JT (2011) Through the looking glass: understanding non-inferiority. Trials 12:106. https://doi.org/10.1186/1745-6215-12-106
McDonnell JG, O’Donnell B, Curley G et al (2007) The analgesic efficacy of transversus abdominis plane block after abdominal surgery: a prospective randomized controlled trial. Anesth Analg 104:193–197. https://doi.org/10.1213/01.ane.0000250223.49963.0f
Siddiqui MRS, Sajid MS, Uncles DR et al (2011) A meta-analysis on the clinical effectiveness of transversus abdominis plane block. J Clin Anesth 23:7–14. https://doi.org/10.1016/j.jclinane.2010.05.008
Ma N, Duncan JK, Scarfe AJ et al (2017) Clinical safety and effectiveness of transversus abdominis plane (TAP) block in post-operative analgesia: a systematic review and meta-analysis. J Anesth 31:432–452. https://doi.org/10.1007/s00540-017-2323-5
Keller DS, Ermlich BO, Delaney CP (2014) Demonstrating the benefits of transversus abdominis plane blocks on patient outcomes in laparoscopic colorectal surgery: review of 200 consecutive cases. J Am Coll Surg 219:1143–1148. https://doi.org/10.1016/j.jamcollsurg.2014.08.011
Stokes AL, Adhikary SD, Quintili A et al (2017) Liposomal bupivacaine use in transversus abdominis plane blocks reduces pain and postoperative intravenous opioid requirement after colorectal surgery. Dis Colon Rectum 60:170–177. https://doi.org/10.1097/DCR.0000000000000747
Torgeson M, Kileny J, Pfeifer C et al (2018) Conventional epidural vs transversus abdominis plane block with liposomal bupivacaine: a randomized trial in colorectal surgery. J Am Coll Surg. https://doi.org/10.1016/j.jamcollsurg.2018.04.021
Barrington MJ, Ivanusic JJ, Rozen WM, Hebbard P (2009) Spread of injectate after ultrasound-guided subcostal transversus abdominis plane block: a cadaveric study. Anaesthesia 64:745–750. https://doi.org/10.1111/j.1365-2044.2009.05933.x
Acknowledgements
The authors thank Shaelah Huntington and Dr. Marc Shnider for their contributions. This work was conducted with support from Harvard Catalyst|The Harvard Clinical and Translational Science Center (National Center for Advancing Translational Sciences, National Institutes of Health Award UL1 TR001102) and financial contributions from Harvard University and its affiliated academic healthcare centers. The content is solely the responsibility of the authors and does not necessarily represent the official views of Harvard Catalyst, Harvard University and its affiliated academic healthcare centers, or the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Curran reports personal fees from KCI Inc, outside the scope of the submitted work. Dr. Wong, Dr. Poylin, and Dr. Cataldo have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wong, D.J., Curran, T., Poylin, V.Y. et al. Surgeon-delivered laparoscopic transversus abdominis plane blocks are non-inferior to anesthesia-delivered ultrasound-guided transversus abdominis plane blocks: a blinded, randomized non-inferiority trial. Surg Endosc 34, 3011–3019 (2020). https://doi.org/10.1007/s00464-019-07097-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07097-y