Abstract
Background
While multiple studies have evaluated endoscopic submucosal dissection (ESD) and transanal endoscopic microsurgery (TEM) to remove large rectal tumors, there remains a paucity of data to evaluate their comparative efficacy and safety. The primary aim of this study was to perform a structured systematic review and meta-analysis to compare efficacy and safety of ESD versus TEM for the treatment of rectal tumors.
Methods
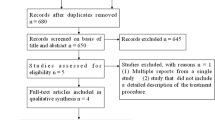
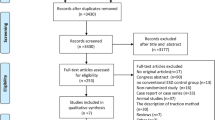
Individualized search strategies were developed from inception through November 2018 in accordance with PRISMA guidelines. Measured outcomes included pooled enbloc resection rates, margin-negative (R0) resection rates, procedure-associated adverse events, and rates of recurrence. This was a cumulative meta-analysis performed by calculating pooled proportions. Heterogeneity was assessed with Cochran Q test and I2 statistics, and publication bias by funnel plot using Egger and Begg tests.
Results
Three studies (n = 158 patients; 55.22% male) were included in this meta-analysis. Patients with ESD compared to TEM had similar age (P = 0.090), rectal tumor size (P = 0.108), and diagnosis rate of adenoma to cancer (P = 0.53). ESD lesions were more proximal as compared to TEM (8.41 ± 3.49 vs. 5.11 ± 1.43 cm from the anal verge; P < 0.001). Procedure time and hospital stay were shorter for ESD compared to TEM [(79.78 ± 24.45 vs. 116.61 ± 19.35 min; P < 0.001) and (3.99 ± 0.32 vs. 5.83 ± 0.94 days; P < 0.001), respectively]. No significant differences between enbloc resection rates [OR 0.98 (95% CI 0.22–4.33); P = 0.98; I2 = 0.00%] and R0 resection rates [OR 1.16 (95% CI 0.36–3.76); P = 0.80; I2 = 0.00%] were noted between ESD and TEM. ESD and TEM reported similar rates of adverse events [OR 1.15 (95% CI 0.47–2.77); P = 0.80; I2 = 0.00%] and rates of recurrence [OR 0.46 (95% CI 0.07–3.14); P = 0.43; I2 = 0.00%].
Conclusion
ESD and TEM possess similar rates of resection, adverse events, and recurrence for patients with large rectal tumors; however, ESD is associated with significantly shorter procedure times and duration of hospitalization. Future studies are needed to evaluate healthcare utilization for these two strategies.






Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A (2019) Cancer statistics, 2019. CA Cancer J Clin 69:7–34
Park SU, Min YW, Shin JU et al (2012) Endoscopic submucosal dissection or transanal endoscopic microsurgery for nonpolypoid rectal high grade dysplasia and submucosa-invading rectal cancer. Endoscopy 44:1031–1036
Park HW, Byeon JS, Park YS et al (2010) Endoscopic submucosal dissection for treatment of rectal carcinoid tumors. Gastrointest Endosc 72:143–149
Nam MJ, Sohn DK, Hong CW et al (2015) Cost comparison between endoscopic submucosal dissection and transanal endoscopic microsurgery for the treatment of rectal tumors. Ann Surg Treat Res 89:202–207
Repici A, Hassan C, De Paula Pessoa D et al (2012) Efficacy and safety of endoscopic submucosal dissection for colorectal neoplasia: a systematic review. Endoscopy 44:137–150
Guerrieri M, Baldarelli M, de Sanctis A, Campagnacci R, Rimini M, Lezoche E (2010) Treatment of rectal adenomas by transanal endoscopic microsurgery: 15 years’ experience. Surg Endosc 24:445–449
Kunitake H, Abbas MA (2012) Transanal endoscopic microsurgery for rectal tumors: a review. Perm J 16:45–50
Kawaguti FS, Nahas CS, Marques CF et al (2014) Endoscopic submucosal dissection versus transanal endoscopic microsurgery for the treatment of early rectal cancer. Surg Endosc 28:1173–1179
Jung Y, Lee J, Cho JY et al (2018) Comparison of efficacy and safety between endoscopic submucosal dissection and transanal endoscopic microsurgery for the treatment of rectal tumor. Saudi J Gastroenterol 24:115–121
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med 151:W65–W94
Sterne JA, Hernan MA, Reeves BC et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Wells G, Shea B et al (2000) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analysis. In: 3rd symposium on systematic reviews: beyond the basics; July 3–5; Oxford. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 18 Dec 2018
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Stuart A, Ord JK (1994) Kendall’s advanced theory of statistics, 6th edn. Edward Arnold, London
Suzuki H, Furukawa K, Kan H et al (2005) The role of transanal endoscopic microsurgery for rectal tumors. J Nippon Med Sch 72:278–284
Tanaka S, Toyonaga T, Morita Y et al (2016) Feasibility and safety of endoscopic submucosal dissection for lower rectal tumors with hemorrhoids. World J Gastroenterol 22:6268–6275
Arezzo A, Passera R, Saito Y et al (2014) Systematic review and meta-analysis of endoscopic submucosal dissection versus transanal endoscopic microsurgery for large noninvasive rectal lesions. Surg Endosc 28:427–438
Saito Y, Sakamoto T, Nakajima T, Matsuda T (2014) Colorectal ESD: current indications and latest technical advances. Gastrointest Endosc Clin N Am 24:245–255
Takeuchi Y, Uedo N, Ishihara R et al (2010) Efficacy of an endo-knife with a water-jet function (Flushknife) for endoscopic submucosal dissection of superficial colorectal neoplasms. Am J Gastroenterol 105:314–322
Toyoizumi H, Kaise M, Arakawa H et al (2009) Ultrathin endoscopy versus high-resolution endoscopy for diagnosing superficial gastric neoplasia. Gastrointest Endosc 70:240–245
Maslekar S, Pillinger SH, Sharma A, Taylor A, Monson JR (2007) Cost analysis of transanal endoscopic microsurgery for rectal tumours. Colorectal Dis 9:229–234
Higgins JP, Green S. Cochrane handbook for systematic reviews of interventions. Version 5.1.0. http://handbook-5-1.cochrane.org. Accessed 2 Dec 2018
Hon SS, Ng SS, Chiu PW et al (2011) Endoscopic submucosal dissection versus local excision for early rectal neoplasms: a comparative study. Surg Endosc 25:3923–3927
Hitzler MH, Heintz A (2015) Single centre study: results of transanal endoscopic microsurgery of rectal tumors since 2003 vs. results of endoscopic submucosal dissection reported in the literature. Zentralbl Chir 140:645–650
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Chris C. Thompson is a consultant for Boston Scientific, Olympus America, and Apollo Endosurgery. Hiroyuki Aihara is a consultant for Olympus America, Boston Scientific, and Fujifilm Medical Systems. Thomas R. McCarty, Ahmad Najdat Bazarbashi, and Kelly E. Hathorn have no conflicts to disclose.
Ethical approval
Institutional IRB approval and written consent was not required given the design of this systematic review and meta-analysis.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
McCarty, T.R., Bazarbashi, A.N., Hathorn, K.E. et al. Endoscopic submucosal dissection (ESD) versus transanal endoscopic microsurgery (TEM) for treatment of rectal tumors: a comparative systematic review and meta-analysis. Surg Endosc 34, 1688–1695 (2020). https://doi.org/10.1007/s00464-019-06945-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-06945-1