Abstract
Background
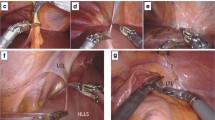
Retracting the lateral liver segment during laparoscopic distal gastrectomy is important for achieving an optimal surgical field. However, excessive force may injure the liver, causing temporary abnormalities of liver function tests after laparoscopic surgery. We developed a new liver retraction method and assessed its safety and utility.
Patients and methods
We retrospectively analyzed records in our surgical database of consecutive surgical patients who underwent laparoscopic distal gastrectomy for early gastric cancer. We divided the 229 patients into two groups based on the liver retraction method used, either flexible liver retraction with clipping and suturing (FLICS) or the Nathanson retractor (NR). One-to-one propensity score matching was performed to match patients, resulting in the records of 53 pairs of cases extracted from the database. Operative and postoperative outcomes were assessed, including following the values of serum liver enzymes, total bilirubin, and C-reactive protein until postoperative day 30.
Results
There were no significant differences in patient characteristics or preoperative data in the two groups. The retraction method was not changed intraoperatively for any patients. The operative time was significantly shorter in the FLICS group, but the amount of bleeding did not differ. Liver injury was not observed as a result of liver retraction during surgery. In both groups, serum liver enzymes temporarily increased after surgery but improved rapidly thereafter. The postoperative increases in aspartate transaminase, alanine transaminase, and C-reactive protein levels were significantly lower in the FLICS than in the NR group. No serious complications associated with liver retraction were observed in either group.
Conclusions
Our new liver retraction technique provided an optimal surgical field without inducing liver dysfunction. It is a simple, safe, and effective liver retraction technique.




Similar content being viewed by others
References
Kitano S, Iso Y, Moriyama M, Sugimachi K (1994) Laparoscopy-assisted Billroth I gastrectomy. Surg Laparosc Endosc 4:146–148
Huscher CG, Mingoli A, Sgarzini G, Sansonetti A, Di Paola M, Recher A, Ponzano C (2005) Laparoscopic versus open subtotal gastrectomy for distal gastric cancer: five-year results of a randomized prospective trial. Ann Surg 241:232–237
Katai H, Sasako M, Fukuda H, Nakamura K, Hiki N, Saka M, Yamaue H, Yoshikawa T, Kojima K (2010) Safety and feasibility of laparoscopy-assisted distal gastrectomy with suprapancreatic nodal dissection for clinical stage I gastric cancer: a multicenter phase II trial (JCOG 0703). Gastric Cancer 13:238–244
Noshiro H, Shimizu S, Nagai E, Ohuchida K, Tanaka M (2003) Laparoscopy-assisted distal gastrectomy for early gastric cancer: is it beneficial for patients of heavier weight? Ann Surg 238:680–685
Vinuela EF, Gonen M, Brennan MF, Coit DG, Strong VE (2012) Laparoscopic versus open distal gastrectomy for gastric cancer: a meta-analysis of randomized controlled trials and high-quality nonrandomized studies. Ann Surg 255:446–456
Katai H, Mizusawa J, Katayama H, Takagi M, Yoshikawa T, Fukagawa T, Terashima M, Misawa K, Teshima S, Koeda K, Nunobe S, Fukushima N, Yasuda T, Asao Y, Fujiwara Y, Sasako M (2017) Short-term surgical outcomes from a phase III study of laparoscopy-assisted versus open distal gastrectomy with nodal dissection for clinical stage IA/IB gastric cancer: Japan Clinical Oncology Group Study JCOG0912. Gastric Cancer 20:699–708
Hu Y, Huang C, Sun Y, Su X, Cao H, Hu J, Xue Y, Suo J, Tao K, He X, Wei H, Ying M, Hu W, Du X, Chen P, Liu H, Zheng C, Liu F, Yu J, Li Z, Zhao G, Chen X, Wang K, Li P, Xing J, Li G (2016) Morbidity and mortality of laparoscopic versus open D2 distal gastrectomy for advanced gastric cancer: a randomized controlled trial. J Clin Oncol 34:1350–1357
Inokuchi M, Nakagawa M, Tanioka T, Okuno K, Gokita K, Kojima K (2018) Long- and short-term outcomes of laparoscopic gastrectomy versus open gastrectomy in patients with clinically and pathological locally advanced gastric cancer: a propensity-score matching analysis. Surg Endosc 32:735–742
Paolucci V, Schaeff B, Gutt CN, Litynski GS (1997) Exposure of the operative field in laparoscopic surgery. Surg Endosc 11:856–863
Etoh T, Shiraishi N, Tajima M, Shiromizu A, Yasuda K, Inomata M, Kitano S (2007) Transient liver dysfunction after laparoscopic gastrectomy for gastric cancer patients. World J Surg 31:1115–1120
Morris-Stiff G, Jones R, Mitchell S, Barton K, Hassn A (2008) Retraction transaminitis: an inevitable but benign complication of laparoscopic fundoplication. World J Surg 32:2650–2654
Shinohara T, Kanaya S, Yoshimura F, Hiramatsu Y, Haruta S, Kawamura Y, Giacopuzzi S, Fujita T, Uyama I (2011) A protective technique for retraction of the liver during laparoscopic gastrectomy for gastric adenocarcinoma: using a Penrose drain. J Gastrointest Surg 15:1043–1048
Uyama I, Sakurai Y, Komori Y, Nakamura Y, Syoji M, Tonomura S, Yoshida I, Masui T, Inaba K, Ochiai M (2005) Laparoscopy-assisted uncut Roux-en-Y operation after distal gastrectomy for gastric cancer. Gastric Cancer 8:253–257
Uyama I, Sakurai Y, Komori Y, Nakamura Y, Syoji M, Tonomura S, Yoshida I, Masui T, Ochiai M (2005) Laparoscopic gastrectomy with preservation of the vagus nerve accompanied by lymph node dissection for early gastric carcinoma. J Am Coll Surg 200:140–145
Genser L, Torcivia A, Saget A, Vaillant JC, Siksik JM (2016) Minimal invasive internal liver retractor in conventional and trans-umbilical single-incision laparoscopic sleeve gastrectomy: video report. Obes Surg 26:704–705
Kinjo Y, Okabe H, Obama K, Tsunoda S, Tanaka E, Sakai Y (2011) Elevation of liver function tests after laparoscopic gastrectomy using a Nathanson liver retractor. World J Surg 35:2730–2738
Kitajima T, Shinohara H, Haruta S, Momose K, Ueno M, Udagawa H (2015) Prevention of transient liver damage after laparoscopic gastrectomy via modification of the liver retraction technique using the Nathanson liver retractor. Asian J Endosc Surg 8:413–418
Japanese Gastric Cancer A (2011) Japanese classification of gastric carcinoma: 3rd English edition. Gastric Cancer 14:101–112
Hamabe A, Omori T, Tanaka K, Nishida T (2012) Comparison of long-term results between laparoscopy-assisted gastrectomy and open gastrectomy with D2 lymph node dissection for advanced gastric cancer. Surg Endosc 26:1702–1709
Kanaya S, Kawamura Y, Kawada H, Iwasaki H, Gomi T, Satoh S, Uyama I (2011) The delta-shaped anastomosis in laparoscopic distal gastrectomy: analysis of the initial 100 consecutive procedures of intracorporeal gastroduodenostomy. Gastric Cancer 14:365–371
Kitagami H, Morimoto M, Nozawa M, Nakamura K, Tanimura S, Murakawa K, Murakami Y, Kikuchi K, Ushigome H, Sato L, Yamamoto M, Shimizu Y, Hayakawa T, Tanaka M, Hirano S (2014) Evaluation of the delta-shaped anastomosis in laparoscopic distal gastrectomy: midterm results of a comparison with Roux-en-Y anastomosis. Surg Endosc 28:2137–2144
Chen AP, Setser A, Anadkat MJ, Cotliar J, Olsen EA, Garden BC, Lacouture ME (2012) Grading dermatologic adverse events of cancer treatments: the common terminology criteria for adverse events version 4.0. J Am Acad Dermatol 67:1025–1039
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Tamhankar AP, Kelty CJ, Jacob G (2011) Retraction-related liver lobe necrosis after laparoscopic gastric surgery. J Soc Laparoendosc Surg 15:117–121
Harikrishnan J, Jackson P, Patel R, Najmaldin A (2014) Segmental liver atrophy: a complication of the nathanson retractor. JSM Clincal Case Rep 2:1012
Kawahira H, Mori M, Hayashi H, Natsume T, Akai T, Hanari N, Horibe D, Hayano K, Matsubara H (2013) A flexible-arm liver retractor that provides an optimal surgical field without postoperative liver dysfunction. Hepatogastroenterology 60:2016–2018
Nozaki T, Kato T, Komiya A, Fuse H (2014) Retraction-related acute liver failure after urological laparoscopic surgery. Curr Urol 7:199–203
Orr KE, Williams MP (2014) MDCT of retractor-related hepatic injury following laparoscopic surgery: appearances, incidence, and follow-up. Clin Radiol 69:606–610
Shibao K, Higure A, Yamaguchi K (2011) Disk suspension method: a novel and safe technique for the retraction of the liver during laparoscopic surgery (with video). Surg Endosc 25:2733–2737
Yoshikawa K, Shimada M, Higashijima J, Nakao T, Nishi M, Takasu C, Kashihara H, Eto S (2016) Combined liver mobilization and retraction: a novel technique to obtain the optimal surgical field during laparoscopic total gastrectomy. Asian J Endosc Surg 9:111–115
Tan M, Xu FF, Peng JS, Li DM, Chen LH, Lv BJ, Zhao ZX, Huang C, Zheng CX (2003) Changes in the level of serum liver enzymes after laparoscopic surgery. World J Gastroenterol 9:364–367
Nguyen NT, Braley S, Fleming NW, Lambourne L, Rivers R, Wolfe BM (2003) Comparison of postoperative hepatic function after laparoscopic versus open gastric bypass. Am J Surg 186:40–44
Yamazaki H, Oi H, Matsushita M, Inoue T, Tang JT, Inoue T (1995) C-reactive protein as an indicator of effect and of adverse reaction to transcatheter arterial embolization. Radiat Med 13:163–165
Nguyen NT, Longoria M, Gelfand DV, Sabio A, Wilson SE (2005) Staged laparoscopic Roux-en-Y: a novel two-stage bariatric operation as an alternative in the super-obese with massively enlarged liver. Obes Surg 15:1077–1081
Pasenau J, Mamazza J, Schlachta CM, Seshadri PA, Poulin EC (2000) Liver hematoma after laparoscopic nissen fundoplication: a case report and review of retraction injuries. Surg Laparosc Endosc Percutan Tech 10:178–181
Firoozmand E, Ritter M, Cohen R, Peters J (1996) Ventricular laceration and cardiac tamponade during laparoscopic Nissen fundoplication. Surg Laparosc Endosc 6:394–397
Funding
No funding was received for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Yuki Ushimaru, Takeshi Omori, Yoshiyuki Fujiwara, Yuji Shishido, Yoshitomo Yanagimoto, Keijirou Sugimura, Kazuyoshi Yamamoto, Jeong-Ho Moon, Hiroshi Miyata, Masayuki Ohue, and Masahiko Yano have no conflicts of interest or financial ties to disclose.
Ethics statement
All procedures in this study were in accordance with the ethical standards of the responsible committee on institutional human experimentation and with the Helsinki Declaration of 1964 and later versions.
Rights and permissions
About this article
Cite this article
Ushimaru, Y., Omori, T., Fujiwara, Y. et al. A novel liver retraction method in laparoscopic gastrectomy for gastric cancer. Surg Endosc 33, 1828–1836 (2019). https://doi.org/10.1007/s00464-018-6461-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6461-0