Abstract
Background
We hypothesized that the addition of a recruitment maneuver to protective ventilation (PVRM) would result in lower pulmonary and systemic inflammatory responses than traditional ventilation or protective ventilation (PV) alone in patients undergoing lung surgery.
Methods
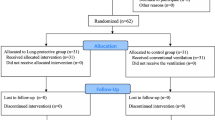
Sixty patients who underwent scheduled thoracoscopic lobectomy were randomly assigned to three groups: traditional ventilation, PV, or PVRM. Ventilations were performed using a tidal volume of 10 mL/kg for the traditional ventilation group and either 8 mL/kg (two-lung) or 6 mL/kg (one-lung, OLV) with a positive end-expiratory pressure of 5 cm H2O for the PV and PVRM groups. The RM was performed 10 min after the start of OLV. Fiberoptic bronchoalveolar lavage (BAL) was performed twice in dependent and non-dependent lungs: before the start and immediately after the end of OLV. Blood samples were collected at the same time points. The levels of cytokines, including TNF-α, IL-1β, IL-6, IL-8, and IL-10, were measured.
Results
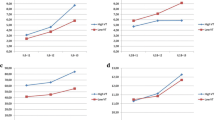
After OLV, the level of TNF-α in the BAL fluid of dependent lungs was significantly higher in the PV than in the PVRM group (P = 0.049), whereas IL-1β, IL-6, IL-8, and IL-10 levels were not significantly different among the groups. In non-dependent lung BAL fluid, no cytokines were significantly different among the groups. After OLV, IL-10 serum levels were significantly higher in the traditional ventilation than in the PVRM group (P = 0.027).
Conclusions
Lower inflammatory responses in the ventilated lung and serum were observed with PVRM than with traditional ventilation or PV alone. Larger multi-center clinical trials are warranted to confirm the effects of different ventilatory strategies on postoperative outcomes.

Similar content being viewed by others
References
Slutsky AS, Tremblay LN (1998) Multiple system organ failure. Is mechanical ventilation a contributing factor? Am J Respir Crit Care Med 157:1721–1725
Misthos P, Katsaragakis S, Milingos N, Kakaris S, Sepsas E, Athanassiadi K, Theodorou D, Skottis I (2005) Postresectional pulmonary oxidative stress in lung cancer patients. The role of one-lung ventilation. Eur J Cardiothorac Surg 27:379–382
Takenaka K, Ogawa E, Wada H, Hirata T (2006) Systemic inflammatory response syndrome and surgical stress in thoracic surgery. J Crit Care 21:48–53
Grichnik KP, D’Amico TA (2004) Acute lung injury and acute respiratory distress syndrome after pulmonary resection. Semin Cardiothorac Vasc Anesth 8:317–334
Brodsky JB, Fitzmaurice B (2001) Modern anesthetic techniques for thoracic operations. World J Surg 25:162–166
Licker M, de Perrot M, Spiliopoulos A, Robert J, Diaper J, Chevalley C, Tschopp JM (2003) Risk factors for acute lung injury after thoracic surgery for lung cancer. Anesth Analg 97:1558–1565
Slutsky AS, Ranieri VM (2013) Ventilator-induced lung injury. N Engl J Med 369:2126–2136
Schilling T, Kozian A, Huth C, Bühling F, Kretzschmar M, Welte T, Hachenberg T (2005) The pulmonary immune effects of mechanical ventilation in patients undergoing thoracic surgery. Anesth Analg 101:957–965
Muscedere JG, Mullen JB, Gan K, Slutsky AS (1994) Tidal ventilation at low airway pressures can augment lung injury. Am J Respir Crit Care Med 149:1327–1334
Wrigge H, Uhlig U, Zinserling J, Behrends-Callsen E, Ottersbach G, Fischer M, Uhlig S, Putensen C (2004) The effects of different ventilatory settings on pulmonary and systemic inflammatory responses during major surgery. Anesth Analg 98:775–781
Michelet P, D’Journo XB, Roch A, Doddoli C, Marin V, Papazian L, Decamps I, Bregeon F, Thomas P, Auffray JP (2006) Protective ventilation influences systemic inflammation after esophagectomy: a randomized controlled study. Anesthesiology 105:911–919
Levin MA, McCormick PJ, Lin HM, Hosseinian L, Fischer GW (2014) Low intraoperative tidal volume ventilation with minimal PEEP is associated with increased mortality. Br J Anaesth 113:97–108
Rothen HU, Sporre B, Engberg G, Wegenius G, Hedenstierna G (1993) Re-expansion of atelectasis during general anaesthesia: a computed tomography study. Br J Anaesth 71:788–795
Lachmann B (1992) Open up the lung and keep the lung open. Intensive Care Med 18:319–321
Unzueta C, Tusman G, Suarez-Sipmann F, Bohm S, Moral V (2012) Alveolar recruitment improves ventilation during thoracic surgery: a randomized controlled trial. Br J Anaesth 108:517–524
Meade MO, Cook DJ, Guyatt GH, Slutsky AS, Arabi YM, Cooper DJ, Davies AR, Hand LE, Zhou Q, Thabane L, Austin P, Lapinsky S, Baxter A, Russell J, Skrobik Y, Ronco JJ, Stewart TE, Lung Open Ventilation Study Investigators (2008) Ventilation strategy using low tidal volumes, recruitment maneuvers, and high positive end-expiratory pressure for acute lung injury and acute respiratory distress syndrome: a randomized controlled trial. JAMA 299:637–645
Wakabayashi K, Wilson MR, Tatham KC, O’Dea KP, Takata M (2014) Volutrauma, but not atelectrauma, induces systemic cytokine production by lung-marginated monocytes. Crit Care Med 42:e49–e57
Acute Respiratory Distress Syndrome Network, Brower RG, Matthay MA, Morris A, Schoenfeld D, Thompson BT, Wheeler A (2000) Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. The acute respiratory distress syndrome network. N Engl J Med 342:1301–1308
Schilling T, Kozian A, Kretzschmar M, Huth C, Welte T, Bühling F, Hedenstierna G, Hachenberg T (2007) Effects of propofol and desflurane anaesthesia on the alveolar inflammatory response to one-lung ventilation. Br J Anaesth 99:368–375
Schilling T, Kozian A, Senturk M, Huth C, Reinhold A, Hedenstierna G, Hachenberg T (2011) Effects of volatile and intravenous anesthesia on the alveolar and systemic inflammatory response in thoracic surgical patients. Anesthesiology 115:65–74
Kozian A, Schilling T, Schutze H, Senturk M, Hachenberg T, Hedenstierna G (2011) Ventilatory protective strategies during thoracic surgery: effects of alveolar recruitment maneuver and low-tidal volume ventilation on lung density distribution. Anesthesiology 114:1025–1035
Nagahiro I, Andou A, Aoe M, Sano Y, Date H, Shimizu N (2001) Pulmonary function, postoperative pain, and serum cytokine level after lobectomy: a comparison of VATS and conventional procedure. Ann Thorac Surg 72:362–365
Leite CF, Calixto MC, Toro IF, Antunes E, Mussi RK (2012) Characterization of pulmonary and systemic inflammatory responses produced by lung re-expansion after one-lung ventilation. J Cardiothorac Vasc Anesth 26:427–432
Reis Miranda D, Gommers D, Struijs A, Dekker R, Mekel J, Feelders R, Lachmann B, Bogers AJ (2005) Ventilation according to the open lung concept attenuates pulmonary inflammatory response in cardiac surgery. Eur J Cardiothorac Surg 28:889–895
de la Gala F, Pineiro P, Garutti I, Reyes A, Olmedilla L, Cruz P, Duque P, Casanova J, Rancan L, Benito P, Vara E (2015) Systemic and alveolar inflammatory response in the dependent and nondependent lung in patients undergoing lung resection surgery: a prospective observational study. Eur J Anaesthesiol 32:872–880
De Conno E, Steurer MP, Wittlinger M, Zalunardo MP, Weder W, Schneiter D, Schimmer RC, Klaghofer R, Neff TA, Schmid ER, Spahn DR, Z’graggen BR, Urner M, Beck-Schimmer B (2009) Anesthetic-induced improvement of the inflammatory response to one-lung ventilation. Anesthesiology 110:1316–1326
Lases EC, Duurkens VA, Gerritsen WB, Haas FJ (2000) Oxidative stress after lung resection therapy: a pilot study. Chest 117:999–1003
Ishizaka A, Watanabe M, Yamashita T, Ogawa Y, Koh H, Hasegawa N, Nakamura H, Asano K, Yamaguchi K, Kotani M, Kotani T, Morisaki H, Takeda J, Kobayashi K, Ogawa S (2001) New bronchoscopic microsample probe to measure the biochemical constituents in epithelial lining fluid of patients with acute respiratory distress syndrome. Crit Care Med 29:896–898
Acknowledgements
The authors are grateful to Ha Yan Kim (Biostatistics Collaboration Unit, Yonsei University College of Medicine, Seoul, Korea) for statistical consultation and data analysis. We would like to thank Editage (http://www.editage.co.kr) for English language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Hyun Joo Kim, Jeong-Hwa Seo, Kyoung-Un Park, Young Tae Kim, In Kyu Park, and Jae-Hyon Bahk have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Kim, H.J., Seo, JH., Park, KU. et al. Effect of combining a recruitment maneuver with protective ventilation on inflammatory responses in video-assisted thoracoscopic lobectomy: a randomized controlled trial. Surg Endosc 33, 1403–1411 (2019). https://doi.org/10.1007/s00464-018-6415-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6415-6