Abstract
Background
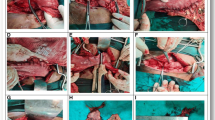
Billroth I reconstruction is a means of anastomosis that is widely performed after surgical resection for distal gastric cancer. Interest has grown in totally laparoscopic gastrectomy, and several methods for totally laparoscopic performance of Billroth I reconstruction have been reported. However, the methods are cumbersome, and postoperative complications such as twisting at the site of anastomosis and obstruction due to stenosis have arisen. We developed an augmented rectangle technique (ART) by which the anastomosis is created laparoscopically with the use of three automatic endoscopic linear staplers, and the resulting anastomotic opening is wide and less likely to become twisted or stenosed. The technical details of our ART-based Billroth I anastomosis are presented herein along with results of the procedure to date.
Methods
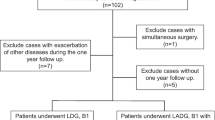
The technique was applied in 160 patients who underwent totally laparoscopic distal gastrectomy for gastric cancer between December 2013 and August 2017. Clinicopathological data, surgical data, and postoperative outcomes were analyzed.
Results
During surgery, there were no troubles associated with gastrointestinal reconstruction and there was no transition to laparotomy. There were no postoperative complications, including suture failure and stenosis, associated with the gastrointestinal reconstruction, and the average postoperative hospital stay was 12 days.
Conclusion
Totally laparoscopic ART-based Billroth I reconstruction is both feasible and safe. We expect this technique to contribute to the spread of safe totally laparoscopic surgery for gastric cancer.






Similar content being viewed by others
References
Kitano S, Iso Y, Moriyama M, Sugimachi K (1994) Laparoscopy-assisted Billroth I gastrectomy. Surg Laparosc Endosc 4:146–148
Fukunaga T, Hiki N, Tokunaga M, Nohara K, Akashi Y, Katayama H, Yoshiba H, Yamada K, Ohyama S, Yamaguchi T (2009) Left-sided approach for suprapancreatic lymph node dissection in laparoscopy-assisted distal gastrectomy without duodenal transection. Gastric Cancer 12:106–112
Shinohara T, Hanyu N, Kawano S, Tanaka Y, Murakami K, Watanabe A, Yanaga K (2014) Clinical significance of medial approach for suprapancreatic lymph node dissection during laparoscopic gastric cancer surgery. Surg Endosc 28:1678–1685
Kunisaki C, Makino H, Takagawa R, Sato K, Kawamata M, Kanazawa A, Yamamoto N, Nagano Y, Fujii S, Ono HA, Akiyama H, Shimada H (2009) Predictive factors for surgical complications of laparoscopy-assisted distal gastrectomy for gastric cancer. Surg Endosc 23:2085–2093
Tanaka C, Fujiwara M, Kanda M, Murotani K, Iwata N, Hayashi M, Kobayashi D, Yamada S, Nakayama G, Sugimoto H, Koike M, Fujii T, Kodera Y (2017) Stapling an extracorporeal Billroth-I anastomosis by the complete double stapling technique after laparoscopy-assisted distal gastrectomy. Asian J Endosc Surg 10:137–142
Kanaya S, Gomi T, Momoi H, Tamaki N, Isobe H, Katayama T, Wada Y, Ohtoshi M (2002) Delta-shaped anastomosis in totally laparoscopic Billroth I gastrectomy: new technique of intraabdominal gastroduodenostomy. J Am Coll Surg 195:284–287
Tanimura S, Higashino M, Fukunaga Y, Takemura M, Nishikawa T, Tanaka Y, Fujiwara Y, Osugi H (2008) Intracorporeal Billroth 1 reconstruction by triangulating stapling technique after laparoscopic distal gastrectomy for gastric cancer. Surg Laparosc Endosc Percutaneous Tech 18:54–58
Ikeda T, Kawano H, Hisamatsu Y, Ando K, Saeki H, Oki E, Ohga T, Kakeji Y, Tsujitani S, Kohnoe S, Maehara Y (2013) Progression from laparoscopic-assisted to totally laparoscopic distal gastrectomy: comparison of circular stapler (i-DST) and linear stapler (BBT) for intracorporeal anastomosis. Surg Endosc 27:325–332
Byun C, Cui LH, Son SY, Hur H, Cho YK, Han SU (2016) Linear-shaped gastroduodenostomy (LSGD): safe and feasible technique of intracorporeal Billroth I anastomosis. Surg Endosc 30:4505–4514
Japanese Gastric Cancer Association (2011) Japanese classification of gastric carcinoma. Gastric Cancer 14:101–112
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications. A new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Kim HG, Park JH, Jeong SH, Lee YJ, Ha WS, Choi SK, Hong SC, Jung EJ, Ju YT, Jeong CY, Park T (2013) Totally laparoscopic distal gastrectomy after learning curve completion: comparison with laparoscopy-assisted distal gastrectomy. J Gastric Cancer 13:26–33
Kim DG, Choi YY, An JY, Kwon IG, Cho I, Kim YM, Bae JM, Song MG, Noh SH (2013) Comparing the short-term outcomes of totally intracorporeal gastroduodenostomy with extracorporeal gastroduodenostomy after laparoscopic distal gastrectomy for gastric cancer: a single surgeon’s experience and a rapid systematic review with meta-analysis. Surg Endosc 27:3153–3161
Lin M, Zheng CH, Huang CM, Li P, Xie JW, Wang JB, Lin JX, Lu J, Chen QY, Cao LL, Tu RH (2016) Totally laparoscopic versus laparoscopy-assisted Billroth-I anastomosis for gastric cancer: a case-control and case-matched study. Surg Endosc 30:5245–5254
Jeong O, Jung MR, Park YK, Ryu SY (2015) Safety and feasibility during the initial learning process of intracorporeal Billroth I (delta-shaped) anastomosis for laparoscopic distal gastrectomy. Surg Endosc 29:1522–1529
Kosuga T, Hiki N, Nunobe S, Ohashi M, Kubota T, Kamiya S, Sano T, Yamaguchi T (2015) Does the single-stapling technique for circular-stapled esophagojejunostomy reduce anastomotic complications after laparoscopic total gastrectomy? Ann Surg Oncol 22:3606–3612
Acknowledgements
We acknowledge Duncan Mark Douglas, MD, from the Department of General Surgery, Johns Hopkins University, as the first to refer to our anastomosis technique as ART.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Tetsu Fukunaga, Yuji Ishibashi, Shinichi Oka, Satoshi Kanda, Yukinori Yube, Yoshinori Kohira, Yuta Matsuo, Osamu Mori, Shinya Mikami, Takeharu Enomoto, and Takehito Otsubo have no conflict of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Fukunaga, T., Ishibashi, Y., Oka, S. et al. Augmented rectangle technique for Billroth I anastomosis in totally laparoscopic distal gastrectomy for gastric cancer. Surg Endosc 32, 4011–4016 (2018). https://doi.org/10.1007/s00464-018-6266-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6266-1