Abstract
Background
The demonstration of competency in endoscopy is required prior to obtaining American Board of Surgery Certification. To demonstrate competency, the resident must pass a national high-stakes cognitive test and a technical skills exam on a virtual reality simulator. The purpose of this preliminary study was to design a proficiency-based endoscopy simulation curriculum to meet this competency requirement.
Methods
This is a mixed methods prospective cohort study at a single academic medical institution. Prior to taking the national exam, surgery residents were required to participate in a skills lab and demonstrate proficiency on 10 simulation tasks. Proficiency was based on time and percent of objects targeted/mucosa seen. Simulation practice time, number of task repetitions to proficiency, and prior endoscopic experience were recorded. Resident’s self-reported confidence scores in endoscopic skills prior to and following simulation lab training were obtained.
Results
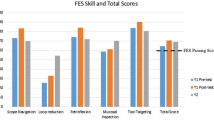
From January 1, 2016 through August 1, 2017, 20 surgical residents (8 PGY2, 8 PGY3, 4 PGY4) completed both a faculty-supervised endoscopy skills lab and independent learning with train-to-proficiency simulation tasks. Median overall simulator time per resident was 306 min (IQR: 247–405 min). Median overall time to proficiency in all tasks was 235 min (IQR: 208–283 min). The median time to proficiency decreased with increasing PGY status (r = 0.4, P = 0.05). There was no correlation between prior real-time endoscopic experience and time to proficiency. Reported confidence in endoscopic skills increased significantly from mean of 5.75 prior to 7.30 following the faculty-supervised endoscopy skills lab (P = 0.0002). All 20 residents passed the national exam.
Conclusions
In this preliminary study, a train-to-proficiency curriculum in endoscopy improved surgical resident’s confidence in their endoscopic skills and 100% of residents passed the FES technical skills test on their first attempt. Our findings also indicate that uniform proficiency was not achieved by real-time experience alone.

Similar content being viewed by others
References
http://surgicalcore.org/modules. Accessed 1 July 2016
http://www.fesprogram.org/. Accessed 1 July 2016
Vassiliou M et al (2014) Fundamentals of endoscopic surgery: creation and validation of the hands-on test. Surg Endosc 28:704–7114
Poulose B (2014) Fundamentals of endoscopic surgery cognitive examination: development and validity evidence. Surg Endosc 28:631–638
Gardner A, Scott D, Willlis R et al (2017) Is current surgery resident and GI fellow training adequate to pass FES? Surg Endosc 31:352–358
Van Sickle K et al (2011) A multicenter, simulation-based skills training collaborative using shared GI Mentor II systems: results from the Texas Association of Surgical Skills Laboratories (TASSL) flexible endoscopy curriculum. Surg Endosc 25:2980–2986
Heneghan SJ, Borley J, Dietz PA et al (2005) Comparison of urban and rural general surgeons: motivations for practice location, practice pattern, and education requirements. J Am Coll Surg 201:732–736
Stoller J, Joseph J, Parodi N, Gardner A (2015) Are there detrimental effects from proficiency-based training in fundamentals of laparoscopic surgery among novices? An exploration of goal theory. J Surg Ed 31:215–221
Willis R, Richa J, Oppeltz R, Nguyen P, Wagner K, Van Sicklle K, Dent D (2012) Comparing three pedagogical approaches to psychomotor skills acquisition. Am J Surg 203:8–13
Motola I, Devine LA, Chung HS, Sullivan JE, Issenberg SB (2013) Simulation in healthcare education; a best evidence practical guide. AMEE 82. Med Teach 35:1510–1530
McGaghie WC, Issenberg SB, Cohen MER, Barsuk JH, Wayne DB (2011) Does simulation-based medical education with deliberate practice yield better results than traditional clinical education? A meta-analytic comparative review of the evidence. Acad Med 86:706
Hashimoto D, Petrusa E, Phitayakorn R, Valle C, Casey B, Gee D (2017) A proficiency-based virtual reality endoscopy curriculum improves performance on the fundamentals of endoscopic surgery examination. Surg Endosc. https://doi.org/10.1007/s00464-017-5821-5
Mueller CL, Kaneva P, Fried GM, Feldman LS, Vassiliou MC (2014) Colonoscopy performance correlates with scores on the FES manual skills test. Surg Endosc 28:3081–3085
Kishiki T, Lapin B, Tanaka R, Francis T, Hughes K, Carbray J, Ujiki M (2016) Goal setting results in improvement in surgical skills: a randomized controlled trial. Surgery 160:1028–1037
Kaltenbach T, Leung C, Wu K, Yan K, Friedland S, Soetiko R (2011) Use of the colonoscopy training model with the colonoscopy 3D imaging probe improved trainee colonoscopy performance: a pilot study. Dig Dis Sci 56:1496–1502
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Susan Gearhart, Michael Marohn, Saowanee Ngamruengphong, Gina Adrales, Oluwafemi Owodunni, Kim Duncan, Emil Petrusa, and Pamela Lipsett have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Gearhart, S., Marohn, M., Ngamruengphong, S. et al. Development of a train-to-proficiency curriculum for the technical skills component of the fundamentals of endoscopic surgery exam. Surg Endosc 32, 3070–3075 (2018). https://doi.org/10.1007/s00464-017-6018-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-6018-7