Abstract
Background
Recent evidence indicates that a preoperative warm-up is a potentially useful tool in facilitating performance. But what factors drive such improvements and how should a warm-up be implemented?
Methods
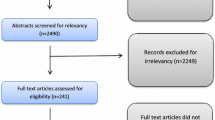
In order to address these issues, we adopted a two-pronged approach: (1) we conducted a systematic review of the literature to identify existing studies utilising preoperative simulation techniques; (2) we performed task analysis to identify the constituent parts of effective warm-ups. We identified five randomised control trials, four randomised cross-over trials and four case series. The majority of these studies reviewed surgical performance following preoperative simulation relative to performance without simulation.
Results
Four studies reported outcome measures in real patients and the remainder reported simulated outcome measures. All but one of the studies found that preoperative simulation improves operative outcomes—but this improvement was not found across all measured parameters. While the reviewed studies had a number of methodological issues, the global data indicate that preoperative simulation has substantial potential to improve surgical performance. Analysis of the task characteristics of successful interventions indicated that the majority of these studies employed warm-ups that focused on the visual motor elements of surgery. However, there was no theoretical or empirical basis to inform the design of the intervention in any of these studies.
Conclusions
There is an urgent need for a more rigorous approach to the development of “warm-up” routines if the potential value of preoperative simulation is to be understood and realised. We propose that such interventions need to be grounded in theory and empirical evidence on human motor performance.

Similar content being viewed by others
References
Catchpole K, Panesar SS, Russell J, Tang V, Hibbert P, Cleary K (2009) Surgical safety can be improved through better understanding of incidents reported to a national database. Nat Patient Safety Agency
White AD, Skelton M, Mushtaq F, Pike TW, Lodge JPA, Wilkie RM (2015) Inconsistent reporting of minimally invasive surgery errors. Ann R Coll Surg Engl. doi:10.1308/rcsann.2015.0038
Chalmers C, Joshi S, Bentley P, Boyle N (2010) The lost generation: impact of the 56-hour EWTD on current surgical training. Bull R Coll Surg Engl 92:102–106. doi:10.1308/147363510X491105
Independent Working Time Regulations Taskforce (2014) The implementation of the working time directive, and its impact on the NHS and health professionals
House of Commons Health Committee (2008) HC 25-I modernising medical careers third report of session 2007–08 Volume I Report, together with formal minutes
Healy N, Chang K, Conneely J, Malone C, Kerin M (2013) Impact of supervised training on the acquisition of simulated laparoscopic skills. Bull R Coll Surg Engl 95:1–6. doi:10.1308/003588413X13643054410340
Ahmed N, Devitt KS, Keshet I, Spicer J, Imrie K, Feldman L, Cools-Lartigue J, Kayssi A, Lipsman N, Elmi M, Kulkarni AV, Parshuram C, Mainprize T, Warren RJ, Fata P, Gorman MS, Feinberg S, Rutka J (2014) A systematic review of the effects of resident duty hour restrictions in surgery. Ann Surg 259:1041–1053. doi:10.1097/SLA.0000000000000595
The Royal College of Surgeons of England (2009) Patient safety. RCSE, London
House of Commons Health Committee (2009) Patient safety: sixth report of session 2009-09, vol 1
Sturm LP, Windsor JA, Cosman PH, Cregan P, Hewett PJ, Maddern GJ (2008) A systematic review of skills transfer after surgical simulation training. Ann Surg 248:166–179. doi:10.1097/SLA.0b013e318176bf24
Dawe SR, Pena GN, Windsor JA, Broeders JAJL, Cregan PC, Hewett PJ, Maddern GJ (2014) Systematic review of skills transfer after surgical simulation-based training. Br J Surg 101:1063–1076. doi:10.1002/bjs.9482
Abdalla G, Moran-Atkin E, Chen G, Schweitzer MA, Magnuson TH, Steele KE (2015) The effect of warm-up on surgical performance: a systematic review. Surg Endosc 29:1259–1269. doi:10.1007/s00464-014-3811-4
Moran-Atkin E, Abdalla G, Chen G, Magnuson TH, Lidor AO, Schweitzer MA, Steele KE (2015) Preoperative warm-up the key to improved resident technique: a randomized study. Surg Endosc Other Interv Tech 29:1057–1063. doi:10.1007/s00464-014-3778-1
van Swieten LM, van Bergen E, Williams JHG, Wilson AD, Plumb MS, Kent SW, Mon-Williams MA (2010) A test of motor (not executive) planning in developmental coordination disorder and autism. J Exp Psychol Hum Percept Perform 36:493–499. doi:10.1037/a0017177
Diedrichsen J, Kornysheva K (2015) Motor skill learning between selection and execution. Trends Cogn Sci. doi:10.1016/j.tics.2015.02.003
Calhoun VD, Eichele T, Adalı T, Allen EA (2012) Decomposing the brain: components and modes, networks and nodes. Trends Cogn Sci 16:255–256. doi:10.1016/j.tics.2012.03.008
Freedman DJ, Assad J (2011) A proposed common neural mechanism for categorization and perceptual decisions. Nat Neurosci 14:143–146. doi:10.1038/nn.2740
Cohen MX, Ranganath C (2005) Behavioral and neural predictors of upcoming decisions. Cogn Affect Behav Neurosci 5:117–126
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. Ann Intern Med 151(4):W65–W94
Higgins JPT, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JAC, Cochrane Bias Methods Group, Cochrane Statistical Methods Group (2011) The cochrane collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Mills EJ, Chan A-W, Wu P, Vail A, Guyatt GH, Altman DG, Mills E, Kelly S, Wu P, Guyatt G, Louis T, Lavori P, Bailar J, Polansky M, Elbourne D, Altman D, Higgins J, Curtin F, Worthington H, Vail A, Maclure M, Brown B, Cleophas T, de Vogel E, Cleophas T, Daya S, Khan K, Daya S, Collins J, Walter S, Chan A, Altman D, Robinson K, Dickersin K, Altman D, Schulz K, Moher D, Egger M, Davidoff F, Elbourne D, Gøtzsche P, Lang T, Jaynes ET, Schwartz J, Bugianesi K, Ebel D, De Smet M, Haesen R, Larson P, Powers J, Gooch W, Oddo L, Koutsoumbi P, Epanomeritakis E, Tsiaoussis J, Athanasakis H, Chrysos E, Zoras O, Vassilakis J, Xynos E, Turley E, McKeown A, Bonham M, Herrera D, Mayet L, Galindo M, Jung H, Kosoglou T, Salfi M, Lim J, Batra V, Cayen M, Affrime M, Lepore M, Pampanelli S, Fanelli C, Porcellati F, Di Vincenzo A, Cordoni C, Nakaishi H, Matsumoto H, Tominaga S, Hirayama M, Marathe P, Arnold M, Meeker J, Greene D, Barbhaiya R, Marx C, McIntosh E, Wilson W, McEvoy J, Holt S, Suder A, Dronfield C, Holt C, Beasley R, Fernhall B, Szymanksi L, Gorman P, Kamimori G, Kessler C, Schulz K, Chalmers I, Hayes R, Altman D, Moher D, Schulz K, Altman D, Devereaux P, Choi P, El-Dika S, Bhandari M, Montori V, Schünemann H, Wallenstein S, Fisher A, Senn S, Senn S, Liu G, Liang K (2009) Design, analysis, and presentation of crossover trials. Trials 10:27. doi:10.1186/1745-6215-10-27
Weston MK, Stephens JH, Schafer A, Hewett PJ (2012) Warm-up before laparoscopic surgery is not essential. ANZ J Surg. doi:10.1111/j.1445-2197.2012.06321.x
Chen CCG, Green IC, Colbert-Getz JM, Steele K, Chou B, Lawson SM, Andersen DK, Satin AJ (2013) Warm-up on a simulator improves residents’ performance in laparoscopic surgery: a randomized trial. Int Urogynecol J. doi:10.1007/s00192-013-2066-2
Plerhoples T, Zak Y, Hernandez-Boussard T, Lau J (2011) Another use of the mobile device: warm-up for laparoscopic surgery. J Surg Res 170:185–188. doi:10.1016/j.jss.2011.03.015
Lendvay TS, Brand TC, White L, Kowalewski T, Jonnadula S, Mercer LD, Khorsand D, Andros J, Hannaford B, Satava RM (2013) Virtual reality robotic surgery warm-up improves task performance in a dry laboratory environment: a prospective randomized controlled study. J Am Coll Surg 216:1181–1192. doi:10.1016/j.jamcollsurg.2013.02.012
Kroft J, Ordon M, Arthur R, Pittini R (2012) Does surgical “warming up” improve laparoscopic simulator performance? Simul Healthc 7:339–342. doi:10.1097/SIH.0b013e31826230d4
Willaert WIM, Aggarwal R, Daruwalla F, Van Herzeele I, Darzi AW, Vermassen FE, Cheshire NJ (2012) Simulated procedure rehearsal is more effective than a preoperative generic warm-up for endovascular procedures. Ann Surg 255:1184–1189. doi:10.1097/SLA.0b013e31824f9dbf
Lee JY, Mucksavage P, Kerbl DC, Osann KE, Winfield HN, Kahol K, McDougall EM (2012) Laparoscopic warm-up exercises improve performance of senior-level trainees during laparoscopic renal surgery. J Endourol 26:545–550. doi:10.1089/end.2011.0418
Calatayud D, Arora S, Aggarwal R, Kruglikova I, Schulze S, Funch-Jensen P, Grantcharov T (2010) Warm-up in a virtual reality environment improves performance in the operating room. Ann Surg 251:1181–1185. doi:10.1097/SLA.0b013e3181deb630
Moldovanu R, Târcoveanu E, Dimofte G, Lupaşcu C, Bradea C (2011) Preoperative warm-up using a virtual reality simulator. JSLS 15:533–538. doi:10.4293/108680811X13176785204409
Rosser JC, Gentile DA, Hanigan K, Danner OK (2012) The effect of video game “warm-up” on performance of laparoscopic surgery tasks. JSLS 16:3–9. doi:10.4293/108680812X13291597715664
Do AT, Cabbad MF, Kerr A, Serur E, Robertazzi RR, Stankovic MR (2006) A warm-up laparoscopic exercise improves the subsequent laparoscopic performance of Ob-Gyn residents: a low-cost laparoscopic trainer. JSLS 10:297–301
Kahol K, Satava RM, Ferrara J, Smith ML (2009) Effect of short-term pretrial practice on surgical proficiency in simulated environments: a randomized trial of the “preoperative warm-up” effect. J Am Coll Surg 208:255–268. doi:10.1016/j.jamcollsurg.2008.09.029
Arora S, Aggarwal R, Sirimanna P, Moran A, Grantcharov T, Kneebone R, Sevdalis N, Darzi A (2011) Mental practice enhances surgical technical skills: a randomized controlled study. Ann Surg 253:265–270. doi:10.1097/SLA.0b013e318207a789
Derossis AM, Fried GM, Abrahamowicz M, Sigman HH, Barkun JS, Meakins JL (1998) Development of a model for training and evaluation of laparoscopic skills. Am J Surg 175:482–487. doi:10.1016/S0002-9610(98)00080-4
Van Herzeele I, Aggarwal R, Malik I, Gaines P, Hamady M, Darzi A, Cheshire N, Vermassen F (2009) Validation of video-based skill assessment in carotid artery stenting. Eur J Vasc Endovasc Surg 38:1–9. doi:10.1016/j.ejvs.2009.03.008
Martin RCG, Scoggins CR, McMasters KM (2010) Laparoscopic hepatic lobectomy: advantages of a minimally invasive approach. J Am Coll Surg 210:627–634. doi:10.1016/j.jamcollsurg.2009.12.022
Kundhal PS, Grantcharov TP (2009) Psychomotor performance measured in a virtual environment correlates with technical skills in the operating room. Surg Endosc 23:645–649. doi:10.1007/s00464-008-0043-5
Vassiliou MC, Feldman LS, Andrew CG, Bergman S, Leffondré K, Stanbridge D, Fried GM (2005) A global assessment tool for evaluation of intraoperative laparoscopic skills. Am J Surg 190:107–113. doi:10.1016/j.amjsurg.2005.04.004
Blencowe NS, McNair AGK, Davis CR, Brookes ST, Blazeby JM (2012) Standards of outcome reporting in surgical oncology: a case study in esophageal cancer. Ann Surg Oncol 19:4012–4018. doi:10.1245/s10434-012-2497-x
Reznick RK (1993) Teaching and testing technical skills. Am J Surg 165:358–361. doi:10.1016/S0002-9610(05)80843-8
Kahneman D, Tversky A (1979) Prospect theory: an analysis of decision under risk. Econometrica 47:263
Allen RJ, Waterman AH (2014) How does enactment affect the ability to follow instructions in working memory? Mem Cognit. doi:10.3758/s13421-014-0481-3
Körding KP, Wolpert DM, Kording KP (2006) Bayesian decision theory in sensorimotor control. Trends Cogn Sci 10:319–326. doi:10.1016/j.tics.2006.05.003
Friston KJ, Daunizeau J, Kilner J, Kiebel SJ, Friston KJ, Daunizeau J, Kilner J, Kiebel SJ (2010) Action and behavior: a free-energy formulation. Biol Cybern. doi:10.1007/s00422-010-0364-z
Reyna VF, Estrada SM, DeMarinis JA, Myers RM, Stanisz JM, Mills BA (2011) Neurobiological and memory models of risky decision making in adolescents versus young adults. J Exp Psychol Learn Mem Cogn 37:1125–1142. doi:10.1037/a0023943
Wang X-J (2008) Decision making in recurrent neuronal circuits. Neuron 60:215–234. doi:10.1016/j.neuron.2008.09.034
Starcke K, Brand M (2012) Decision making under stress: a selective review. Neurosci Biobehav Rev 36:1228–1248. doi:10.1016/j.neubiorev.2012.02.003
Sanfey AG, Chang LJ (2008) Multiple systems in decision making. Ann N Y Acad Sci 1128:53–62. doi:10.1196/annals.1399.007
Rangel A, Camerer C, Montague PR (2008) A framework for studying the neurobiology of value-based decision making. Nat Rev Neurosci 9:545–556. doi:10.1038/nrn2357
Whistance RN, Forsythe RO, McNair AGK, Brookes ST, Avery KNL, Pullyblank AM, Sylvester PA, Jayne DG, Jones JE, Brown J, Coleman MG, Dutton SJ, Hackett R, Huxtable R, Kennedy RH, Morton D, Oliver A, Russell A, Thomas MG, Blazeby JM, Core Outcomes and iNformation SEts iN SUrgical Studies—ColoRectal Cancer Working Group (2013) A systematic review of outcome reporting in colorectal cancer surgery. Colorectal Dis 15:e548–e560. doi:10.1111/codi.12378
Macefield RC, Boulind CE, Blazeby JM (2014) Selecting and measuring optimal outcomes for randomised controlled trials in surgery. Langenbeck’s Arch Surg 399:263–272. doi:10.1007/s00423-013-1136-8
Gargon E, Gurung B, Medley N, Altman DG, Blazeby JM, Clarke M, Williamson PR, Chalmers I, Glasziou P, Hirsch B, Califf R, Cheng S, Tasneem A, Horton J, Kirkham J, Gargon E, Clarke M, Williamson P, Miyar J, Adams C, Dwan K, Altman D, Arnaiz J, Bloom J, Chan A-W, Williamson P, Altman D, Blazeby J, Clarke M, Devane D, Sinha I, Jones L, Smyth R, Williamson P, Moher D, Liberati A, Tetzlaff J, Altman D, Group P, Chan A, Tetzlaff J, Gotzsche P, Altman D, Mann H, Moher D, Schulz K, Simera I, Altman D, Kostanjsek N (2014) Choosing important health outcomes for comparative effectiveness research: a systematic review. PLoS ONE 9:e99111. doi:10.1371/journal.pone.0099111
Al-Saud LM, Mushtaq F, Allsop MJ, Culmer PC, Mirghani I, Yates E, Keeling A, Mon-Williams MA, Manogue M (2016) Feedback and motor skill acquisition using a haptic dental simulator. Eur J Dent Educ. doi:10.1111/eje.12214
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Mr. T. W. Pike, Mr. S. Pathak, Dr. F. Mushtaq, Dr. R. M. Wilkie, Professor M. Mon-Williams and Professor J. P. A. Lodge have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Pike, T.W., Pathak, S., Mushtaq, F. et al. A systematic examination of preoperative surgery warm-up routines. Surg Endosc 31, 2202–2214 (2017). https://doi.org/10.1007/s00464-016-5218-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5218-x