Abstract
Background
Laparoscopic endoscopic cooperative surgery (LECS) is a safe alternative to endoscopic submucosal dissection (ESD) for select gastric gastrointestinal stromal tumors (GISTs) that are <2 cm in size. To date, there have been no randomized studies comparing the feasibility of these two techniques. Therefore, we compared their feasibility and safety using the propensity score matching method in this study.
Methods
This was a single-center, retrospective, propensity score-matched study of patients who underwent resection of selected gastric GISTs between 2004 and 2014. All patients underwent curative resection for pathologically diagnosed small gastric GISTs. The primary aim was to determine intraoperative complications and postoperative courses. To overcome selection biases, we performed a 1:1 match using five covariates, including age, gender, body mass index, Charlson comorbidity index, and tumor location, to generate propensity scores.
Results
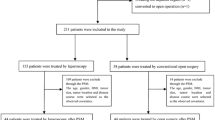
In total, 32 patients treated with LECS and 102 patients treated with ESD were balanced into 30 pairs. The rate of intraoperative complications was significantly lower in the LECS group than in the ESD group (P = 0.029). LECS patients had less intraoperative bleeding than did ESD patients (15.0 ml [range 9.5–50.0 ml] vs. 43.5 ml [range 22.3–56.0 ml], P = 0.004). The two groups had similar postoperative courses. There was no difference in the reoperation rate between the two groups (P = 0.112). The ESD group had a shorter operating time than did the LECS group (41.5 min vs. 96.5 min, P < 0.001). However, during a follow-up of 57.9 (±28.9) months, the recurrence rate did not differ significantly between the two groups (0.0 vs. 6.7 %, respectively; P = 0.256).
Conclusions
LECS for selected gastric GIST patients is feasible and is associated with a better intraoperative outcome and an equal postoperative course compared with the results of ESD.


Similar content being viewed by others
References
Corless CL, Fletcher JA, Heinrich MC (2004) Biology of gastrointestinal stromal tumors. J Clin Oncol 22:3813–3825
Connolly E, Gaffney E, Reynolds J (2003) Gastrointestinal stromal tumors. Br J Surg 90:1178–1186
Kindblom L, Remotti H, Aldenborg F, Meis-Kindblom J (1998) Gastrointestinal pacemaker cell tumors (GIPACT): gastrointestinal stromal tumors show phenotypic characteristic of the interstitial cells of cajal. Am J Pathol 152:1259–1269
Sircar K, Hewlett B, Huizinga J, Chorneyko K, Berezin I, Riddell R (1999) Interstitial cells of cajal as precursors of gastrointestinal stromal tumors. Am J Surg Pathol 23:979–987
DeMatteo RP, Lewis JJ, Leung D, Mudan SS, Woodruff JM, Brennan MF (2000) Two hundred gastrointestinal stromal tumors recurrence patterns and prognostic factors for survival. Ann Surg 231:51–58
Heinrich MC, Corless CL (2005) Gastric GI stromal tumors (GISTs): the role of surgery in the era of targeted therapy. J Surg Oncol 90: 195–207; discussion 207
Nowain ABH, Pais S (2005) Gastrointestinal stromal tumors: clinical profile, pathogenesis, treatment strategies and prognosis. J Gastroenterol Hepatol 20:818–824
Hirao M, Masuda K, Asanuma T (1988) Endoscopic resection of early gastric cancer and other tiumors with local injection of hypertonic saline-epinephrine. Gastrointest Endosc 34:264–269
Blay JY, Bonvalot S, Casali P, Choi H, Debiec-Richter M, Dei Tos AP, Emile JF, Gronchi A, Hogendoorn PC, Joensuu H, Le Cesne A, McClure J, Maurel J, Nupponen N, Ray-Coquard I, Reichardt P, Sciot R, Stroobants S, van Glabbeke M, van Oosterom A, Demetri GD (2005) GIST consensus meeting panelists,Consensus meeting for the management of gastrointestinal stromal tumors. Report of the GIST consensus conference of 20–21 March 2004, under the auspices of ESMO. Ann Oncol 16:566–578
Nishida T, Hirota S, Yanagisawa A, Sugino Y, Minami M, Yamamura Y, Otani Y, Shimada Y, Takahashi F, Kubota T, Guideline Subcommittee GIST (2008) Clinical practice guidelines for gastrointestinal stromal tumor (GIST) in Japan: english version. Int J Clin Oncol 13:416–430
Bedard EL, Mamazza J, Schlachta CM, Poulin EC (2006) Laparoscopic resection of gastrointestinal stromal tumors: not all tumors are created equal. Surg Endosc 20:500–503
Novitsky YW, Kercher KW, Sing RF, Heniford BT (2006) Long-term outcomes of laparoscopic resection of gastric gastrointestinal stromal tumors. Ann Surg 243: 738–745; discussion 745–737
De Vogelaere K, Van Loo I, Peters O, Hoorens A, Haentjens P, Delvaux G (2012) Laparoscopic resection of gastric gastrointestinal stromal tumors (GIST) is safe and effective, irrespective of tumor size. Surg Endosc 26:2339–2345
Kim KH, Kim MC, Jung GJ, Kim SJ, Jang JS, Kwon HC (2012) Long term survival results for gastric GIST: is laparoscopic surgery for large gastric GIST feasible? World J Surg Oncol 10:230
Honda M, Hiki N, Nunobe S, Ohashi M, Kiyokawa T, Sano T, Yamaguchi T (2014) Long-term and surgical outcomes of laparoscopic surgery for gastric gastrointestinal stromal tumors. Surg Endosc 28:2317–2322
Masoni L, Gentili I, Maglio R, Meucci M, D’Ambra G, Di Giulio E, Di Nardo G, Corleto VD (2014) Laparoscopic resection of large gastric GISTs: feasibility and long-term results. Surg Endosc 28:2905–2910
ESMO/European Sarcoma Network Working Group (2014) Gastrointestinal stromal tumours: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 25(Suppl 3):iii21–iii26
Demetri G, Von Mehren M, Antonescu C, Dematteo R, Ganjoo K, Maki R, Pisters P, Raut C, Riedel R, Schuetze S, Sundar H, Trent J, Wayne J (2010) NCCN task force reports: update on the management of patients with gastrointestinal stromal tumors. J Natl Compr Cancer Netw 8:S1
Lee ILLP, Tung SY, Shen CH, Wei KI, Wu CS (2006) Endoscopic submucosal dissection for the treatment of intraluminal gastric subepithelial tumors originating from the muscularis propria layer. Endoscopy 38:1024–1028
Hiki N, Yamamoto Y, Fukunaga T, Yamaguchi T, Nunobe S, Tokunaga M, Miki A, Ohyama S, Seto Y (2008) Laparoscopic and endoscopic cooperative surgery for gastrointestinal stromal tumor dissection. Surg Endosc 22:1729–1735
Wilhelm D, von Delius S, Burian M, Schneider A, Frimberger E, Meining A, Feussner H (2008) Simultaneous use of laparoscopy and endoscopy for minimally invasive resection of gastric subepithelial masses—analysis of 93 interventions. World J Surg 32:1021–1028
Wong DCT, Wong SKH, Leung ALH, Chung CCC, Li MK (2009) Combined endolaparoscopic intragastric excision for gastric neoplasms. J Laparoendosc Adv Surg Tech 19:765–770
Sakon M, Takata M, Seki H, Hayashi K, Munakata Y, Tateiwa N (2010) A novel combined laparoscopic-endoscopic cooperative approach for duodenal lesions. J Laparoendosc Adv Surg Tech A 20:555–558
Gayer CP, Edelman DA, Curtis B, Laker S, Webber J (2011) Combined endoscopic and laparoscopic approach to a gastroesophageal tumor. JSLS 15:228–231
Nunobe S, Hiki N, Gotoda T, Murao T, Haruma K, Matsumoto H, Hirai T, Tanimura S, Sano T, Yamaguchi T (2012) Successful application of laparoscopic and endoscopic cooperative surgery (LECS) for a lateral-spreading mucosal gastric cancer. Gastric Cancer 15:338–342
Vecchio R, Marchese S, Ferla F, Intagliata E, Spataro L (2013) Combined laparoscopic and endoscopic excision of a gastric gist. Surg Endosc 27:3501–3502
de Filippo FR, Perrotta N, Cappiello A, Esposito T, Loffredo D (2013) Combined endo-laparoscopic approach in a patient with a duodenal foreign body and bowel obstruction. Updates Surg 65:231–235
Austin PC (2011) An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivar Behav Res 46:399–424
Brookhart MA, Schneeweiss S, Rothman KJ, Glynn RJ, Avorn J, Sturmer T (2006) Variable selection for propensity score models. Am J Epidemiol 163:1149–1156
Rosenbaum P, Rubin D (1983) The central role of the propensity score in observational studies for causal effects. Biometrika 79:516–524
Rubin D, Thomas N (1996) Matching using estimated propensity score: relating theory to practice. Biometrics 52:249–264
Teoh AY, Chiu PW (2014) Collaboration between laparoscopic surgery and endoscopic resection: an evidence-based review. Dig Endosc 26(Suppl 1):12–19
Hoteya S, Haruta S, Shinohara H, Yamada A, Furuhata T, Yamashita S, Kikuchi D, Mitani T, Ogawa O, Matsui A, Iizuka T, Udagawa H, Kaise M (2014) Feasibility and safety of laparoscopic and endoscopic cooperative surgery for gastric submucosal tumors, including esophagogastric junction tumors. Dig Endosc 26:538–544
Qiu WQ, Zhuang J, Wang M, Liu H, Shen ZY, Xue HB, Shen L, Ge ZZ, Cao H (2013) Minimally invasive treatment of laparoscopic and endoscopic cooperative surgery for patients with gastric gastrointestinal stromal tumors. J Dig Dis 14:469–473
Chiu P (2006) Endoscopic submucosal dissection-bigger piece, better outcomes. Gastrointest Endosc 64:884–885
Yahagi N (2008) Is esophageal endoscopic submucosal dissection an extreme treatment modality, or can it be a standard treatment modality? Gastrointest Endosc 68:1073–1075
Chung I, Lee S, Kim S, Cho W (2009) Theurapeutic outcomes in 1000 cases of endoscopic submucosal dissection for early gastric neoplasms: Korean ESD study group multicenter study. Gastrointest Endosc 69:1228–1235
Neuhaus H, Costamagna G, Deviere J, Fockens P, Ponchon T, Rosch T (2006) Endoscopic submucosal dissection (ESD) of early gastric lesion using a new double-channel endoscope (The R-scope). Endoscopy 65:1016–1023
Coda S, Lee S-Y, Gotoda T (2007) Endoscopic mucosal resection and endoscopic submucosal dissection as treatment for early gastro intestinal cancers in western countries Gut. Liver 1:12–21
Deprez P, Aouattah T, Yeung C-P, Fiasse R, Horsmans Y, Piessevaux H (2007) Endoscopic resection of superficial gastric tumors (abstract). Gastrointest Endosc 65:164
Coda S, Trentino P, Antonellis F, Porowska B, Gossetti F, Ruberto F, Pugliese F, D’Amati G, Negro P, Gotoda T (2010) A western single-center experience with endoscopic submucosal dissection for early gastrointestinal cancers. Gastric Cancer 13:258–263
Asge Technology Committee, Maple JT, Abu Dayyeh BK, Chauhan SS, Hwang JH, Komanduri S, Manfredi M, Konda V, Murad FM, Siddiqui UD, Banerjee S (2015) Endoscopic submucosal dissection. Gastrointest Endosc 81:1311–1325
Pimentel-Nunes P, Dinis-Ribeiro M (2015) Endoscopic submucosal dissection in the treatment of gastrointestinal superficial lesions: follow the guidelines! GE Port J Gastroenterol 22:184–186
Rodrigues J, Carmo J, Carvalho L, Barreiro P, Chagas C (2015) Endoscopic submucosal dissection for gastrointestinal superficial lesions: initial experience in a single Portuguese center. GE Port J Gastroenterol 22:190–197
Cao Y, Liao C, Tan A, Gao Y, Mo Z, Gao F (2009) Meta-analysis of endoscopic submucosal dissection versus endoscopic mucosal resection for tumors of the gastrointestinal tract. Endoscopy 41:751–757
Bouillot J, Bresler L, Fagniez P (2003) Laparoscopic resection of benign submucosal stomach tumors. A report of 65 cases. Gastroenterol Clin Biol 27:272–276
Schubert D, Kuhn R, Nestler G (2005) Laparoscopic endoscopic rendezvous resection of upper gastrointestinal tumors. Dig Dis 23:106–112
Acknowledgments
This work was supported by the National High Technology Research and Development Program (863 Program) issued by the Ministry of Science and Technology of China, No. 2012AA011103; The Development Center for Medical Science and Technology, the Ministry of Health of China, No. W2011 WAI44; the Major Program of Science and Technology Program of Guangzhou, No. 201300000087; the Research Fund of Public Welfare in Health Industry, Health Ministry of China, No. 201402015; and the Key Clinical Specialty Discipline Construction Program.
Authors’ contributions
Study conception and design: A. I. Balde, Guoxin Li. Collection of the data: A. I. Balde, J. D. Redondo N. Statistical analysis: A. I. Balde, Hao Liu. Data interpretation: A. I. Balde. Drafting of the manuscript: A. I. Balde, Tao Chen, Yanfeng Hu. Critical revision: Guoxin Li, Li Zhen, Wei Gong, Jiang Yu.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Drs. A. I. Balde, Tao Chen, Yanfeng Hu, J. D. Redondo N., Hao Liu, Wei Gong, Jiang Yu, Li Zhen, and Guoxin Li have no conflicts of interest or financial ties to disclose.
Additional information
Balde A.I. and Tao Chen contributed equally to this work, including the design of the study and the preparation of the manuscript, and should be considered as co-first authors.
Rights and permissions
About this article
Cite this article
Balde, A.I., Chen, T., Hu, Y. et al. Safety analysis of laparoscopic endoscopic cooperative surgery versus endoscopic submucosal dissection for selected gastric gastrointestinal stromal tumors: a propensity score-matched study. Surg Endosc 31, 843–851 (2017). https://doi.org/10.1007/s00464-016-5042-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5042-3