Abstract
Background
Obstructive sleep apnea (OSA), present in 60–70 % of bariatric surgery patients, is a potentially life-threatening condition when not detected and managed appropriately. The best available method to identify the severity of OSA is polysomnography. However, routine polysomnography measurements have not been accepted as standard modality in bariatric surgery. We report our experience with routine polysomnography in a cohort of patients undergoing bariatric surgery to determine the true prevalence of OSA with respect to the different severity levels as determined by the apnea–hypopnea index (AHI).
Methods
AHI data were retrospectively collected from all patients who underwent bariatric surgery from 2012 onward, when the performance of preoperative polysomnography became mandatory. Mild, moderate and severe OSA were defined as an AHI ≥5, ≥15 and ≥30/h, respectively. Prevalence and number needed to screen (NNS) were calculated for all OSA severity levels.
Results
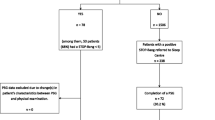
A total of 1358 patients were included. OSA was detected in 813 (59.9 %; NNS: 2) patients. Moreover, 405 (29.8 %; NNS: 4) patients were diagnosed with an AHI ≥15/h and 213 (15.7 %; NNS: 7) with severe OSA (AHI ≥30/h). Extreme AHI thresholds of ≥60 and ≥90/h were detected in 79 (5.8 %; NNS: 18) and 17 (1.3 %; NNS: 77) patients, respectively.
Conclusion
One-third of the bariatric surgery patients have an AHI ≥15/h and would benefit from continuous positive airway pressure therapy. In order to increase perioperative safety and avoid the preventable risk of perioperative complications, we recommend mandatory P(S)G prior to bariatric surgery.
Similar content being viewed by others
Abbreviations
- AHI:
-
Apnea–hypopnea index
- BMI:
-
Body mass index
- CPAP:
-
Continuous positive airway pressure
- CV:
-
Cardiovascular
- IFSO:
-
International Federation for the Surgery of Obesity and Metabolic Disorders
- LRYGB:
-
Laparoscopic Roux-en-Y gastric bypass
- LSG:
-
Laparoscopic sleeve gastrectomy
- NNS:
-
Number needed to screen
- OSA:
-
Obstructive sleep apnea
- PG:
-
Polygraphy
- PSG:
-
Polysomnography
References
Malhotra A, White DP (2002) Obstructive sleep apnoea. Lancet 360(9328):237–245
Colquitt JL, Picot J, Loveman E, Clegg AJ (2009) Surgery for obesity. Cochrane Database Syst Rev (2):CD003641
Ravesloot MJ, Van Maanen JP, Hilgevoord AA, Van Wagensveld BA, de Vries N (2012) Obstructive sleep apnea is underrecognized and underdiagnosed in patients undergoing bariatric surgery. Eur Arch Otorhinolaryngol 269(7):1865–1871
ASMBS Clinical Issues Committee (2012) Peri-operative management of obstructive sleep apnea. Surg Obes Relat Dis 8(3):e27–e32
Fonseca MI, Pereira T, Caseiro P (2015) Death and disability in patients with sleep apnea—a meta-analysis. Arg Bras Cardiol 104(1):58–66
Jennum P, Tonnesen P, Ibsen R, Kjellberg J (2015) All-cause mortality from obstructive sleep apnea in male and female patients with and without continuous positive airway pressure treatment: a registry study with 10 years of follow-up. Nat Sci Sleep 7:43–50
Kaw R, Chung F, Pasupuleti V, Mehta J, Gay PC, Hernandez AV (2012) Meta-analysis of the association between obstructive sleep apnoea and postoperative outcome. Br J Anaesth 109(6):897–906
Hai F, Porhomayon J, Vermont L, Frydrych L, Jaoude P, El-Solh AA (2014) Postoperative complications in patients with obstructive sleep apnea: a meta-analysis. J Clin Anesth 26(8):591–600
Abrishami A, Khajehdehi A, Chung F (2010) A systematic review of screening questionnaires for obstructive sleep apnea. Can J Anaesth 57(5):423–438
de Raaff CA, Coblijn UK, de Vries N, Heymans MW, van den Berg BTJ, van Tets WF, van Wagensveld BA (2015) Predictive factors for insufficient weight loss after bariatric surgery: Does obstructive sleep apnea influence weight loss? Obes Surg. doi:10.1007/s11695-015-1830-4
de Raaff CA, Coblijn UK, de Vries N, van Wagensveld BA (2016) Is fear for postoperative cardiopulmonary complications after bariatric surgery in patients with obstructive sleep apnea justified? A systematic review. Am J Surg 211(4):793–801
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Prof. Dr. N. de Vries is a member of the Medical Advisory Board of NightBalance and has shares in Nightbalance. Prof. Dr. H. J. Bonjer receives personal fees from Olympus and grants from Johnson & Johnson, Applied Medical and Medtronic. Drs. C. A. L. de Raaff, Ms. A. S. Pierik, Drs. U. K. Coblijn and Dr. B. A. van Wagensveld declare that they have no conflicts of interest of financial ties to disclose.
Rights and permissions
About this article
Cite this article
de Raaff, C.A.L., Pierik, A.S., Coblijn, U.K. et al. Value of routine polysomnography in bariatric surgery. Surg Endosc 31, 245–248 (2017). https://doi.org/10.1007/s00464-016-4963-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-4963-1