Abstract
Background
The use of self-gripping mesh during laparoscopic TEP inguinal hernia repairs may eliminate the need for any additional fixation, and thus reduce post-operative pain without the added concern for mesh migration. Long-term outcomes are not yet prospectively studied in a controlled fashion.
Methods
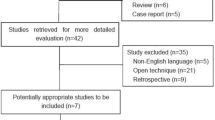
Under IRB approval, from January 2011–April 2013, 91 hernias were repaired laparoscopically with self-gripping mesh without additional fixation. Patients were followed for at least 1 year. Demographics and intraoperative data (defect location, size, and mesh deployment time) are recorded. VAS is used in the recovery room (RR) to score pain, and the Carolinas Comfort Scale ™ (CCS), a validated 0–5 pain/quality of life (QoL) score where a mean score of >1.0 means symptomatic pain, is employed at 2 weeks and at 1 year. Morbidities, narcotic usage, days to full activity and return to work, and CCS scores are reported.
Results
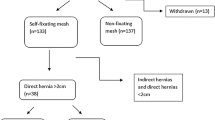
Sixty two patients, with 91 hernias repaired with self-gripping mesh, completed follow-up at a mean time period of 14.8 months. Seventeen hernias were direct defects (average size 3.0 cm). Mesh deployment time was 193.7 s. RR pain was 1.1/10 using a VAS. Total average oxycodone/acetaminophen (5 mg/325 mg) usage = 5.0 tablets, days to full activity was 1.6, and return to work was 4.2 days. Thirteen small asymptomatic seromas were palpated without any recurrences or groin tenderness, and all seromas resolved by the 6 month visit. Transient testis discomfort was reported in five patients. Urinary retention was 3.2 %. Mean CCS™ scores at the first visit for groin pain laying, bending, sitting, walking, and step-climbing were 0.2, 0.5, 0.4, 0.3, and 0.3, respectively. At the first post op visit, 4.8 % had symptomatic pain (CCS > 1). At 14.8 months, no patients reported symptomatic pain with CCS scores for all 62 patients averaging 0.02, (range 0–0.43). There are no recurrences thus far.
Conclusions
Self-gripping mesh can be safely used during laparoscopic TEP inguinal hernia repairs; our cohort had a rapid recovery, and at the 1-year follow-up visit, there were no recurrences and no patients reported any chronic pain as defined by a CCS™ > 1.




Similar content being viewed by others
References
Rotkow IM (2003) Demographic and socioeconomic aspects of hernia repair in the United States in 2003. Surg Clin N Am 83(5):1045–1051 v–vi
Simons MP (2009) European hernia society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13:343–403
Taylor C et al (2008) Laparoscopic inguinal hernia repair without mesh fixation, early results of a large randomised clinical trial. Surg Endosc 22(3):757–762
Belyansky I, Tsirline VB, Klima DA, Walters AL, Lincourt AE, Heniford TB (2011) Prospective, comparative study of postoperative quality of life in TEP, TAPP, and modified Lichtenstein repairs. Ann Surg 254(5):709–715
Kosai N, Sutton PA, Evans J, Varghese J (2011) Laparoscopic preperitoneal mesh repair using a novel self-adhesive mesh. J Minimal Access Surg 7(3):192–194
Kingsnorth A, Nienhuijs S, Schüle S, Appel P, Ziprin P, Eklund A, Smeds S (2010) Preliminary results of a comparative randomized study: benefit of self-gripping Parietex Progrip™ mesh. Hernia 14:0–001
Kingsnorth A (2012) Randomized controlled multicenter international clinical trial of self-gripping Parietex Progrip polyester mesh versus lightweight polypropylene mesh in open inguinal hernia repair: interim results at 3 months. Hernia 16(3):287–294
Chastan P (2009) Tension-free open hernia repair using an innovative self-gripping semi-resorbable mesh. Hernia 13(2):137–142
Heniford T, Walters AL, Lincourt AE, Novitsky YW, Hope WW, Kercher KW (2008) Comparison of generic versus specific quality-of-life scales for mesh hernia repairs. J Am Coll Surg 206(4):638–644
Lowham AS, Filipi CJ, Fitzgibbons RJ Jr, Stoppa R, Wantz GE, Felix EL, Crafton WB (1997) Mechanisms of hernia recurrence after preperitoneal mesh repair. Traditional and laparoscopic. Ann Surg 225(4):422
Ng WT, Auyeung K (2008) An inexpensive and effective technique for hernioplasty mesh anchorage. Surg Laparosc Endosc Percutaneous Tech 18(2):228–229
Melissa CS, Bun TA, Wing CK, Chung TY, Wai NE, Tat LH (2013) Randomized double-blinded prospective trial of fibrin sealant spray versus mechanical stapling in laparoscopic total extraperitoneal hernioplasty. Ann Surg 259(3):432–437
Hollinsky C et al (2009) Comparison of a new self-gripping mesh with other fixation methods for laparoscopic hernia repair in a rat model. JACS 208(6):1–1107
Kapischke M, Schulze H, Caliebe A (2010) Self-fixating mesh for the Lichtenstein procedure—a prestudy. Langenbecks Arch Surg 395(4):317–322
Fumagalli RU, Puccetti F, Elmore U, Massaron S, Rosati R (2013) Self-gripping mesh versus staple fixation in laparoscopic inguinal hernia repair: a prospective comparison. Surg Endosc 5:1798–1802
Birk D, Hess S, Garcia-Pardo C (2013) Low recurrence rate and low chronic pain associated with inguinal hernia repair by laparoscopic placement of Parietex ProGrip™ mesh: clinical outcomes of 220 hernias with mean follow-up at 23 months. Hernia 17(3):313–320
Khoury N (1998) A randomized prospective controlled trial of laparoscopic extraperitoneal hernia repair and mesh-plug hernioplasty: a study of 315 cases. J Laparosc Adv Surg Tech 8(6):367–372
Kumar Bansal V et al (2013) A prospective, randomized comparison of long-term outcomes: chronic groin pain and quality of life following totally extraperitoneal (TEP) and transabdominal preperitoneal (TAPP) laparoscopic inguinal hernia dfrepair. Surg Endosc 27:2373–2382
Disclosures
Dr. Brian Jacob provides consulting services for Covidien (New Haven, CT). Bresnahan Erin, Bates Andrew, Wu Andrew, Reiner Mark and Jacob Brian have financial interests to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bresnahan, E., Bates, A., Wu, A. et al. The use of self-gripping (Progrip™) mesh during laparoscopic total extraperitoneal (TEP) inguinal hernia repair: a prospective feasibility and long-term outcomes study. Surg Endosc 29, 2690–2696 (2015). https://doi.org/10.1007/s00464-014-3991-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3991-y