Abstract
Introduction
Many laparoscopic surgeons report musculoskeletal symptoms that are thought to be related to the ergonomic stress of performing laparoscopy. Robotic surgical systems may address many of these limitations. To date, however, there have been no studies exploring the quantitative ergonomics of robotic surgery. In this study, we sought to compare the activation of bilateral biceps, triceps, deltoid, and trapezius muscle groups during traditional laparoscopic surgery (TLS) and robot-assisted laparoscopic surgery (RALS) procedures, as quantified by surface electromyography (sEMG).
Methods
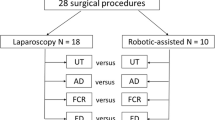
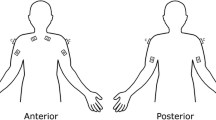
One surgeon with expertise in TLS and RALS performed 18 operative procedures (13 TLS, 5 RALS) while sEMG measurements were obtained from bilateral biceps, triceps, deltoid, and trapezius muscles. sEMG measurements were normalized to the maximum voluntary contraction of each muscle (%MVC). We compared mean %MVC values for each muscle group during TLS and RALS with unpaired t-tests and considered differences with a p value <0.05 to be statistically significant.
Results
Muscle activation was higher during TLS compared to RALS in bilateral biceps (L Biceps RALS:1.01 %MVC, L Biceps TLS:3.14, p = 0.01; R Biceps RALS:1.81 %MVC, R Biceps TLS:4.53, p = 0.0002). Muscle activation was higher during TLS compared to RALS in bilateral triceps (L Triceps RALS:1.73 %MVC, L Triceps TLS:3.58, p = 0.04; R Triceps RALS:1.59 %MVC, R Triceps TLS:5.11, p = 0.02). Muscle activation was higher during TLS compared to RALS in bilateral deltoids (L Deltoid RALS:1.50 %MVC, L Deltoid TLS:3.68, p = 0.03; R Deltoid RALS:1.19 %MVC, R Deltoid TLS:2.57, p = 0.01). Significant differences were not detected in the bilateral trapezius muscles (L Trapezius RALS:1.50 %MVC, L Trapezius TLS:3.68, p = 0.03; R Trapezius RALS:1.19 %MVC, R Trapezius TLS:2.57, p = 0.01).
Discussion
We have quantitatively examined the ergonomics of TLS and RALS and shown that in a single surgeon, TLS procedures are associated with significantly elevated biceps, triceps, and deltoid activation bilaterally when compared to RALS procedures.

Similar content being viewed by others
References
Bhogal RH, Athwal R, Durkin D, Deakin M, Cheruvu CN (2008) Comparison between open and laparoscopic repair of perforated peptic ulcer disease. World J Surg 32:2371–2374
Wilson CH, Sanni A, Rix DA, Soomro NA (2011) Laparoscopic versus open nephrectomy for live kidney donors. Cochrane Database Syst Rev 9(11):CD006124
Li MZ, Lian L, Xiao LB, Wu WH, He YL, Song XM (2012) Laparoscopic versus open adhesiolysis in patients with adhesive small bowel obstruction: a systematic review and meta-analysis. Am J Surg 204:779–786
Sari V, Nieboer TE, Vierhout ME, Stegeman DF, Kluivers KB (2010) The operation room as a hostile environment for surgeons: physical complaints during and after laparoscopy. Minim Invasive Ther Allied Technol 19:105–109
Park A, Lee G, Seagull FJ, Meenaghan N, Dexter D (2010) Patients benefit while surgeons suffer: an impending epidemic. J Am Coll Surg 210:306–313
Berguer R, Chen J, Smith WD (2003) A comparison of the physical effort required for laparoscopic and open surgical techniques. Arch Surg 138:967–970
Berguer R, Smith WD, Chung YH (2001) Performing laparoscopic surgery is significantly more stressful for the surgeon than open surgery. Surg Endosc 15:1204–1207
Lee G, Lee T, Dexter D, Godinez C, Meenaghan N, Catania R, Park A (2009) Ergonomic risk associated with assisting in minimally invasive surgery. Surg Endosc 23:182–188
Berguer R (1998) Surgical technology and the ergonomics of laparoscopic instruments. Surg Endosc 12:458–462
O’Sullivan OE, O’Reilly BA (2012) Robot-assisted surgery: impact on gynaecological and pelvic floor reconstructive surgery. Int Urogynecol J 23:1163–1173
Kumar P, Kommu SS, Challacombe BJ, Dasgup-Ta P (2010) Laparoendoscopic single-site surgery (LESS) prostatectomy–robotic and conventional approach. Minerva Urol Nefrol 62:425–430
Lunca S, Bouras G, Stanescu AC (2005) Gastrointestinal robot-assisted surgery. A current perspective. Rom J Gastroenterol 14:385–391
Wright AS, Gould JC, Melvin WS (2004) Computer-assisted robotic antireflux surgery. Minerva Gastroenterol Dietol 50:253–260
Frick AC, Falcone T (2009) Robotics in gynecologic surgery. Minerva Ginecol 61:187–199
Xia T, Baird C, Jallo G, Hayes K, Nakajima N, Hata N, Kazanzides P (2008) An integrated system for planning, navigation and robotic assistance for skull base surgery. Int J Med Robot 4:321–330
Anton D, Gerr F, Meyers A, Cook TM, Rosecrance JC, Reynolds J (2007) Effect of aviation snip design and task height on upper extremity muscular activity and wrist posture. J Occup Environ Hyg 4:99–113
Lee G, Lee T, Dexter D, Klein R, Park A (2007) Methodological infrastructure in surgical ergonomics: a review of tasks, models, and measurement systems. Surg Innov 14:153–167
Lee G, Sutton E, Clanton T, Park A (2010) Higher physical workload risks with NOTES versus laparoscopy: a quantitative ergonomic assessment. Surg Endosc 25:1585–1593
Berguer R, Smith W (2006) An ergonomic comparison of robotic and laparoscopic technique: the influence of surgeon experience and task complexity. J Surg Res 134:87–92
Zihni AM, Ohu I, Cavallo JA, Ousley J, Cho S, Awad MM (2014) FLS tasks can be used as an ergonomic discriminator between laparoscopic and robotic surgery. Surg Endosc. (Epub ahead of print)
Lee GI, Lee MR, Clanton T, Sutton E, Park AE, Marohn MR (2014) Comparative assessment of physical and cognitive ergonomics associated with robotic and traditional laparoscopic surgeries. Surg Endosc 28(2):456–465
Park A, Lee G, Seagull FJ, Meenaghan N, Dexter D (2010) Patients benefit while surgeons suffer: an impending epidemic. J Am Coll Surg 210:306–313
Acknowledgments
The authors thank Gyusung Lee, PhD of the Department of Surgery at Johns Hopkins University (Baltimore, MD) for his valuable advice. This study was supported by research grants from the Society of Gastrointestinal and Endoscopic Surgeons (SAGES) and Intuitive Surgical, Inc (Sunnyvale, CA).
Disclosures
This study was supported by a research grant from the Society of Gastrointestinal and Endoscopic Surgeons (SAGES). This study was supported by a research grant from Intuitive Surgical, Inc. (Sunnyvale, CA). Dr. Zihni received research grant funding for unrelated studies from the National Institutes of Health. Dr. Cavallo has received research grant funding for unrelated studies from the National Institutes of Health, the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES), and the American Hernia Society in collaboration with Davol® Incorporated; and has served as a one-time consultant for Guidepoint Global® Incorporated. Dr Cho has received research grant funding from the Society of Gastrointestinal and Endoscopic Surgeons (SAGES) and Intuitive, Surgical Inc. (Sunnyvale, CA). Dr Awad has received research grant funding from the Society of Gastrointestinal and Endoscopic Surgeons (SAGES) and Intuitive, Surgical Inc. (Sunnyvale, CA). Mr. Ohu has no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zihni, A.M., Ohu, I., Cavallo, J.A. et al. Ergonomic analysis of robot-assisted and traditional laparoscopic procedures. Surg Endosc 28, 3379–3384 (2014). https://doi.org/10.1007/s00464-014-3604-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3604-9