Abstract
Background
Laparoscopy is currently the gold standard for cholecystectomy. Recent literature suggests surgical trainees have limited exposure to open cholecystectomy, which may result in suboptimal performance in the event of conversion. Furthermore, most training and assessment models are designed for laparoscopic cholecystectomy, with limited opportunities for open simulator training. The present study’s purpose was to design an inexpensive model for open cholecystectomy and to validate a performance assessment tool.
Methods
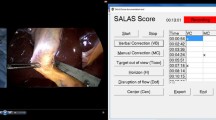
The simulator comprises a porcine liver and gallbladder in a mock human abdomen with silicon skin. The assessment tool utilizes inexpensive infrared (IR) cameras to provide tracking of participant hand motions. Eleven novice general surgery trainees (<20 cholecystectomies) and five expert surgeons (>100 cholecystectomies) completed an open cholecystectomy using the simulator. Procedures were recorded and assessed by a blinded evaluator using a global rating scale. Tracking data analysis was based on number of movements and total path length.
Results
Novices (t = 36.18 min) completed the procedure significantly slower than did experts (t = 19.53 min) (Mann–Whitney test U = 20, p < 0.05) and had significantly more hand movements (Mann–Whitney test U = 20, p < 0.05). Analysis of the total global rating scale scores showed a significant difference between novice (14/35) and expert (24/35) performance in all categories (Mann–Whitney test U = 58, p < 0.05).
Conclusion
The present model presents a realistic, low-cost tool for training and assessment of procedural skills in open cholecystectomy. The study demonstrated the validity of the IR tracking device as an objective assessment tool for open surgical skills training. Future training should incorporate this low-cost, highly effective training device into surgical curricula.







Similar content being viewed by others
References
Brennan TA, Leape LL, Laird NM et al (1991) Incidence of adverse events and negligence in hospitalized patients: results of the harvard medical practice study I. N Engl J Med 324:370–376
Leape LL (2009) Errors in medicine. Clin Chim Acta 404(1):2–5
Schijven MP, Jakimowicz JJ, Broeders IAMJ et al (2005) The Eindhoven laparoscopic cholecystectomy training course: improving operating room performance using virtual reality training: results from the first E.A.E.S. accredited virtual reality trainings curriculum. Surg Endosc 19(9):1220–1226
Fried GM, Feldman LS, Vassiliou MC et al (2004) Proving the value of simulation in laparoscopic surgery. Ann Surg 240(3):518–525 discussion 525–528
Keus F, de Jong JAF, Gooszen HG et al (2006) Laparoscopic versus open cholecystectomy for patients with symptomatic cholecystolithiasis. Cochrane Database Syst Rev (4):CD006231
Visser BC, Parks RW, Garden OJ (2008) Open cholecystectomy in the laparoendoscopic era. Am J Surg 195(1):108–114
Duffy AJ, Hogle NJ, McCarthy H et al (2005) Construct validity for the LAPSIM laparoscopic surgical simulator. Surg Endosc 19(3):401–405
García Galisteo E, Del Rosal Samaniego JM, Baena González V et al (2006) Laparoscopic surgery training in pelvitrainer and virtual simulators. Actas Urol Esp 30(5):451–456
Taffinder N, Sutton C, Fishwick RJ et al (1998) Validation of virtual reality to teach and assess psychomotor skills in laparoscopic surgery: results from randomised controlled studies using the MIST VR laparoscopic simulator. Stud Health Technol Inform 50:124–130
Martin JA, Regehr G, Reznick R et al (1997) Objective structured assessment of technical skill (OSATS) for surgical residents. Br J Surg 84(2):273–278
Aggarwal R, Grantcharov T, Moorthy K et al (2008) Toward feasible, valid, and reliable video-based assessments of technical surgical skills in the operating room. Ann Surg 247(2):372–379
Datta V, Mackay S, Mandalia M et al (2001) The use of electromagnetic motion tracking analysis to objectively measure open surgical skill in the laboratory-based model. J Am Coll Surg 193(5):479–485
Sonnadara RR, Rittenhouse N, Khan A et al (2012) A novel multimodal platform for assessing surgical technical skills. Am J Surg 203(1):32–36
King RC, Atallah L, Lo BPL, Yang G (2009) Development of a wireless sensor glove for surgical skills assessment. IEEE Trans Inf Technol Biomed 13(5):673–679
Dosis A, Aggarwal R, Bello F et al (2005) Synchronized video and motion analysis for the assessment of procedures in the operating theater. Arch Surg 140(3):293–299
Powers KA, Rehrig ST, Irias N et al (2008) Simulated laparoscopic operating room crisis: an approach to enhance the surgical team performance. Surg Endosc 22(4):885–900
Bouget J (2010). Camera calibration toolbox for Matlab. http://www.vision.caltech.edu/bouguetj/calib_doc/index.html#parameters. Accessed Aug 2010
Svoboda T, Martinec D, Pajdla T (2005) A convenient multi-camera self-calibration for virtual environments. PRESENCE Teleoper Virtual Environ 14(4):407–422
Peek B (2007) Managed library for Nintendo’s Wiimote. http://blogs.msdn.com/b/coding4fun/archive/2007/03/14/1879033.aspx. Accessed Aug 2010
Acknowledgments
The following people provided support related to the surgical environment: Lisa Satterthwaite, Marina Romanova, and Dezan Rego. Thomas Sun and Shunne Leung provided technical support towards the development of the IR system. Project supported by National Sciences and Engineering Research Council CGS M Scholarship and the Network for Excellence in Simulation for Clinical Teaching and Learning.
Disclosure
Ranil Sonnadara has, in the past, received a grant and travel reimbursement from the Network for Excellence in Simulation for Clinical Teaching and Learning. He is also employed at Mount Sinai Hospital consults on educational research on an ongoing basis for the University of Toronto. Teodor Grantcharov carries out ongoing consulting work for Covidien Canada and Ethicon Canada. Authors, Neil Rittenhouse, Bharat Sharma, and Alex Mihailidis have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rittenhouse, N., Sharma, B., Sonnadara, R. et al. Design and validation of an assessment tool for open surgical procedures. Surg Endosc 28, 918–924 (2014). https://doi.org/10.1007/s00464-013-3247-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-013-3247-2