Abstract
Background
Little evidence exists to guide educators in the best way to implement simulation within surgical skills curricula. This study investigated whether practicing a basic Fundamentals of Laparoscopic Surgery (FLS) simulator task [peg transfer (PT)] facilitates learning a more complex skill [intracorporeal suturing (ICS)] and compared the effect of PT training to mastery with training to the passing level on PT retention and on learning ICS.
Methods
For this study, 98 surgically naïve subjects were randomized to one of three PT training groups: control, standard training, and overtraining. All the participants then trained in ICS. The learning curves for ICS were analyzed by estimating the learning plateau and rate using nonlinear regression. Skill retention was assessed by retesting participants 1 month after training. The groups were compared using analysis of variance (ANOVA). Effectiveness of skill transfer was calculated using the transfer effectiveness ratio (TER). Data are presented as mean ± standard deviation (p < 0.05).
Results
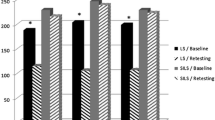
The study was completed by 77 participants (28 control, 26 standard, and 23 overtrained subjects). The ICS learning plateau rose with increasing PT training (452 ± 10 vs. 459 ± 10 vs. 467 ± 10; p < 0.01). Increased PT training was associated with a trend toward higher initial ICS scores (128 ± 107 vs. 127 ± 110 vs. 183 ± 106; p = 0.13) and faster learning rates (15 ± 4 vs. 14 ± 4 vs. 13 ± 4 trials; p = 0.10). At retention, there were no differences in PT scores (p = 0.5). The PT training took 20 ± 10 min for standard training and 39 ± 20 min for overtraining (p < 0.01). Overtrained participants saved 11 ± 5 min in ICS training compared with the control subjects (p = 0.04). However, TER was 0.165 for the overtraining group and 0.160 for the standard training group, suggesting that PT overtraining took longer than the time saved on ICS training.
Conclusion
For surgically naïve subjects, part-task training with PT alone was associated with slight improvements in the learning curve for ICS. However, overtraining with PT did not improve skill retention, and peg training alone was not an efficient strategy for learning ICS.

Similar content being viewed by others
References
Urbach DR, Horvath KD, Baxter NN, Jobe BA, Madan AK, Pryor AD, Khaitan L, Torquati A, Brower ST, Trus TL, Schwaitzberg S (2007) A research agenda for gastrointestinal and endoscopic surgery. Surg Endosc 21:11518–11525
Stefanidis D, Miles WS, Greene FL (2009) Factors influencing residency choice of general surgery applicants: how important is the availability of a skills curriculum? J Surg Educ 66:325–329
Fraser SA, Klassen DR, Feldman LS, Ghitulescu GA, Stanbridge D, Fried GM (2003) Evaluating laparoscopic skills: setting the pass/fail score for the MISTELS system. Surg Endosc 17:964–967
Fried GM (2008) FLS assessment of competency using simulated laparoscopic tasks. J Gastrointest Surg 12:210–212
ABS The American Board of Surgery (2008) ABS to require ACLS, ATLS, and FLS for general surgery certification. http://home.absurgery.org/default.jsp?news_newreqs. Retrieved 27 Oct 2009
Sroka G, Feldman LS, Vassiliou MC, Kaneva PA, Fayez R, Fried GM (2010) Fundamentals of laparoscopic surgery simulator training to proficiency improves laparoscopic performance in the operating room: a randomized controlled trial. Am J Surg 199:115–120
Strum LP, Windsor JA, Cosman PH, Cregan P, Hewett PJ, Maddern GJ (2008) A systematic review of skills transfer after surgical simulation training. Ann Surg 248:166–179
Lehto MR, Buck J (2008) Introduction to human factors and ergonomics for engineers. Taylor & Francis Group, New York
Proctor RW, Vu KPL (2006) Laboratory studies of training, skill acquisition, and retention of performance. In: Ericsson KA, Charness N, Feltovich PJ, Hoffman JR (eds) The Cambridge handbook of expertise and expert performance. Cambridge University Press, New York, pp 265–286
Fried GM, Feldman LS, Vassiliou MC, Fraser SA, Stanbridge D, Ghitulescu G, Andrew CG (2004) Proving the value of simulation in laparoscopic surgery. Ann Surg 240:518–525 discussion 525–518
Feldman LS, Cao J, Andalib A, Fraser S, Fried GM (2009) A method to characterize the learning curve for performance of a fundamental laparoscopic simulator task: defining “learning plateau” and “learning rate”. Surgery 46:381–386
Kolozsvari NO, Andalib A, Kaneva P, Cao J, Vassiliou MC, Fried GM, Feldman LS (2011) Sex is not everything: the role of gender in early performance of a fundamental laparoscopic skill. Surg Endosc 25:1037–1042
Ericsson KA, Krampe RT, Tesch-Romer C (1993) The role of deliberate practice in the acquision of expert performance. Psychol Rev 100:363–406
Gallagher AG, Ritter EM, Champion H, Higgins G, Fried MP, Moses G, Smith CD, Satava RM (2005) Virtual reality simulation for the operating room: proficiency-based training as a paradigm shift in surgical skills training. Ann Surg 241:364–372
Bell RH Jr (2009) Why Johnny cannot operate. Surgery 146:533–542
Scott DJ, Ritter EM, Tesfay ST, Pimentel EA, Nagji A, Fried GM (2008) Certification pass rate of 100% for fundamentals of laparoscopic surgery skills after proficiency-based training. Surg Endosc 22:1887–1893
Society of American Gastrointestinal and Endoscopic Surgeons (2003–2008) Fundamentals of laparoscopic surgery: technical skills proficiency-based training curriculum. http://www.flsprogram.org/wp-content/uploads/2010/08/Technical-Skills-Proficiency-Bases-Training-Curriculum.pdf. Retrieved 6 Feb 2011
Ebbinghaus H (1964) Memory: a contribution to experimental psychology. Dover Publications, New York
Lathan CE, Tracey MR, Sebrechts MM, Clawson DM, Higgins GA (2002) Using virtual environments as training simulators: measuring transfer. In: Stanney KM (ed) Handbook of virtual environments: design implementation and applications. Lawrence Erlbaum Associates, Mahwah, NJ, p 403
Hamdorf JM, Hall JC (2000) Acquiring surgical skills. Br J Surg 87:28–37
Kneebone RL, Scott W, Darzi A, Horrocks M (2004) Simulation and clinical practice: strengthening the relationship. Med Educ 38:1095–1102
Seymour NE, Gallagher AG, Roman SA, O’Brien MK, Bansal VK, Andersen DK, Satava RM (2002) Virtual reality training improves operating room performance. Ann Surg 236:458–464
Arthur WJ, Bennett WJ, Stanush PL, McNelly TL (1998) Factors that influence skill decay and retention: a quantitative review and analysis. Hum Perform 11:57–101
http://www.flsprogram.org. Retrieved 28 March 2009 accessed
Ritter EM, Scott DJ (2007) Design of a proficiency-based skills training curriculum for the fundamentals of laparoscopic surgery. Surg Innov 14:107–112
Grantcharov TP, Funch-Jensen P (2009) Can everyone achieve proficiency with the laparoscopic technique? Learning curve patterns in technical skills acquisition. Am J Surg 197:447–449
Heathcote A, Brown S, Mewhort DJK (2000) The power law repealed: the case for an exponential law of practice. Psychonom Bull Rev 7:185–207
Roscoe SN, Williges BH (1980) Measurement of transfer or training. Chap 16. In: Roscoe SN (ed) Aviation psychology. Iowa State University Press, Ames
Williges BH, Roscoe SN, Williges RC (1973) Synthetic flight training revisited. J Hum Factors Ergon Soc 15:543–560
Stefanidis D, Acker C, Heniford BT (2008) Proficiency-based laparoscopic simulator training leads to improved operating room skill that is resistant to decay. Surg Innov 15:69–73
Stefanidis D, Korndorffer JR Jr, Markley S, Sierra R, Heniford BT, Scott DJ (2007) Closing the gap in operative performance between novices and experts: does harder mean better for laparoscopic simulator training? J Am Coll Surg 205:307–313
Stefanidis D, Hope WW, Korndorffer JR Jr, Markley S, Scott DJ (2010) Initial laparoscopic basic skills training shortens the learning curve of laparoscopic suturing and is cost effective. J Am Coll Surg 210:436–440
Schaverien MV (2010) Development of expertise in surgical training. J Surg Educ 67:37–43
Dubrowski A, Backstein D, Abughaduma R, Leidl D, Carnahan H (2005) The influence of practice schedules in the learning of a complex bone-plating surgical task. Am J Surg 190:359–363
Norman G, Eva K, Brooks L, Hamstra SJ (2006) Expertise in medicine and surgery. In: Ericsson KA, Charness N, Feltovich PJ, Hoffman RR (eds) The Cambridge handbook of expertise and expert performance. Cambridge University Press, New York, pp 339–354
Ericsson KA (2004) Deliberate practice and the acquisition and maintenance of expert performance in medicine and related domains. Acad Med 10(Suppl):70–81
Stefanidis D (2010) Optimal acquisition and assessment of proficiency on simulators in surgery. Surg Clin North Am 90:475–489
Walters C, Acker C, Heniford BT, Greene FL, Stefanidis D (2008) Performance goals on simulators boost resident motivation and skills lab attendance. J Am Coll Surg 207:S88
Torkington J, Smith SG, Rees B, Darzi A (2001) The role of the basic surgical skills course in the acquisition and retention of laparoscopic skill. Surg Endosc 15:1071–1075
Dubrowski A, Park J, Moulton C-a, Larmer J, MacRae H (2007) A comparison of single- and multiple-stage approaches to teaching laparoscopic suturing. Am J Surg 193:269–273
Stefanidis D, Korndorffer JJR, Markley S, Sierra R, Scott DJ (2006) Proficiency maintenance: impact of ongoing simulator training on laparoscopic skill retention. J Am Coll Surg 202:599–603
Acknowledgments
This research project was supported by a Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) research grant. The Steinberg-Bernstein Centre for Minimally Invasive Surgery and Innovation receives an unrestricted educational grant from Covidien. We thank SAGES for awarding us a research grant for this project. We also thank the students who participated in this study.
Disclosures
Nicoleta O. Kolozsvari receives salary support from the McGill Surgeon Scientist program. Nicoleta O. Kolozsvari, Pepa Kaneva, Chantalle Brace, Genevieve Chartrand, Marilou Vaillancourt, Jiguo Cao, Daniel Banaszek, Sebastian Demyttenaere, Melina C. Vassiliou, Gerald M. Fried, and Liane S. Feldman have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kolozsvari, N.O., Kaneva, P., Brace, C. et al. Mastery versus the standard proficiency target for basic laparoscopic skill training: effect on skill transfer and retention. Surg Endosc 25, 2063–2070 (2011). https://doi.org/10.1007/s00464-011-1743-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-011-1743-9