Abstract
Background
The aim of this prospective study was the evaluation of the laparoscopic treatment of common bile duct stones (CBDS) and its indications.
Methods
Five hundred five patients who underwent laparoscopic treatment of CBDS from October 1990 to September 2006 were included in the prospective study. The mean age of the patients was 63 years (range = 19–93).Four hundred fifteen patients were classified ASA I and ASA II and 90 were ASA III and ASA IV. CBDS were suspected or diagnosed preoperatively in 373 patients (73.8%) and diagnosed at intraoperative cholangiography (IOC) in 132 patients (26.2%). A transcystic duct extraction (TCDE) was attempted in 254 patients (50.4%) and a primary choledochotomy in 251 patients (49.6%). Biliary drainage after choledochotomy was used in 148 cases (48.8%).
Results
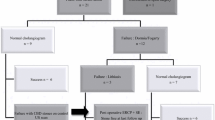
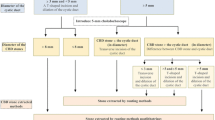
TCDE was successful in 191 cases (75.2%).The 63 failures were managed by laparoscopic choledochotomy in 53 cases and by endoscopic sphincterotomy (ES) in 10 cases. A choledochotomy was thus performed in 304 patients and successful in 295 cases (97%). The nine failures were managed by six conversions to laparotomy (2%) and three postoperative ES. The overall success rate was 96.2%. The morbidity rate was 7.9% with 4.8% of local complications and 3.1% of general complications. The mortality rate was 1%. There were 14 residual stones (2.8%) that were managed by a second laparoscopy in two cases and by ES in 12 cases with four failures managed by laparotomy in one case and laparoscopy in three cases.
Conclusion
Laparoscopic management of CBDS was effective in more than 96% of cases and particularly safe in ASA I and ASA II patients. It has the advantage over ES followed by laparoscopic cholecystectomy (LS) to be a one-stage procedure.
Similar content being viewed by others
References
Berthou JC, Drouard F, Charbonneau Ph, Moussalier K (1998) Evaluation of laparoscopic management of common bile duct stones in 220 patients. Surg Endosc 12: 16–22
Hammarstrom LE, Holmin T, Stridbeck H, Ihse I (1995) Long-term follow-up of a prospective randomized study of endoscopic versus surgical treatment of bile duct calculi in patients with gallbladder in situ. Br J Surg 82:1516–1521
Cotton PB (1993) Endoscopic retrograde pancreatography and laparoscopic cholecystectomy. Am J Surg 165:474–478
National Institutes of Health (2002) NIH state of the science on endoscopic retrograde cholangiopancreatography (ERCP) for diagnosis and therapy. NIH Consens Sci Statements 19:1–26
Waage A, Strömberg C, Leijonmarck CE, Arvidsson D (2003) Long-term results from laparoscopic common bile duct exploration. Surg Endosc 17:1181–1185
Prat F, Pelletier G, Etienne JP (1992) Diagnostic et traîtement de la lithiase de la voie biliaire principale. Gastroenterol Clin Biol 16:865–868
Neoptolemos JP, Carr-Locke DL, Fossard DP (1987) Prospective randomised study of preoperative endoscopic sphincterotomy versus surgery alone for common bile duct stones. BMJ 294:470–474
Sauerbruch T, Feussner H, Frimberger E, Hasegawa H, Ihse I, Riemann JF (1994) Treatment of common bile duct stones – A consensus report. Hepatogastroenterology 41:513–515
Huttl TP, Hrdina CH, Geiger TK, Meyer G, Schildberg FW, Kramling HJ (2002) Management of common bile duct stones. Results of a nationwide survey with analysis of 8433 common bile duct explorations in Germany. Zentrabl Chir 127:282–288
Lilly MC, Arregui ME (2001) A balanced approach to choledocholithiasis. Surg Endosc 15:467–472
Paganini AM, Lezoche E (1998) Follow-up of 161 unselected consecutive patients treated laparoscopically for common bile duct stones. Surg Endosc 12:23–29
Millat B, Deleuze A, de Saxce de Seguin C, Fingerhut A (1997) Routine intraoperative cholangiography is feasible and efficient during laparoscopic cholecystectomy. Hepatogastroenterology 144:22–27
Rhodes M, Sussman L, Cohen L, Lewis MP (1998) Randomized trial of laparoscopic exploration of common bile duct versus postoperative endoscopic retrograde cholangiography of common bile duct stones. Lancet 351:159–161
Cuschieri A, Lezoche E, Morino M, Croce E, Lacy A, Toouli J, Faggioni A, Ribeiro VM, Jakimowicz J, Visa J, Hanna GB (1999) EAES multicenter prospective randomized trial comparing two-stage vs single-stage management of patients with gallstone disease and ductal calculi. Surg Endosc 13:952–957
Sgourakis G, Karaliotas K (2002) Laparoscopic common bile duct exploration and cholecystectomy versus endoscopic stone extraction and laparoscopic cholecystectomy for choledocholithiasis. A prospective randomized study. Minerva Chir 57:467–474
Thompson MH, Tranter SE (2002) All-comers policy for laparoscopic exploration of the common bile duct. Br J Surg 89:1608–1612
Ebner S, Rechner J, Beller S, Erhart K, Riegler FM, Szinicz G (2004) Laparoscopic management of common bile duct stones. Surg Endosc 18:762–776
Berci G, Morgenstern L (1994) Laparoscopic management of common bile duct stones. A multi-institutional SAGES study. Surg Endosc 8:1168–1175
Petelin JB (2003) Laparoscopic common bile duct exploration. Lesson learnt from >12 years experience. Surg Endosc 17:1705–1715
Paganini AM, Feliciotti F, Guerrieri M, Tamburini A, Campagnacci R, Lezoche E (2002) Laparoscopic cholecystectomy and common bile duct exploration are safe for older patients. Surg Endosc 16:1302–1308
Assouline Y, Liguory C, Ink O, Fristch J, Choury AD, Lefebvre JF (1993) Resultats actuels de la sphinctérotomie endoscopique pour lithiase de la voie biliaire principale. Gastroenterol Clin Biol 17:51–55
Lenriot JP, Le Neel JC, Hay JM, Jaeck D, Millat B, Fagniez PL (1993) Cholangio-pancreatographie retrograde et sphincterotomie endoscopique pour lithiase biliaire. Gastroenterol Clin Biol 17:244–250
Coppola R, Riccioni ME, Ciletti S, Cosentino L, Coco C, Magistrelli P, Picciocchi A (1997) Analysis of complications of endoscopic sphincterotomy for biliary stones in a consecutive series of 546 patients. Surg Endosc 11:129–132
Tranter SE, Thompson MH (2002) Comparison of endoscopic sphincterotomy and laparoscopic exploration of the common bile duct. Br J Surg 89:1495–1504
Martin IJ, Bailey IS, Rhodes M, O’Rourke N, Nathanson N, Fielding G (1998) Towards T-tube free laparoscopic bile duct exploration: a methodologic evolution during 300 consecutive procedures. Ann Surg 228:29–34
Williams JAR, Treacy PJ, Sidey P, Worthley CS, Townsend NCW, Russell EA (1994) Primary duct closure versus T-tube drainage following exploration of the common bile duct. Aust N Z J Surg 64:823–826
Decker G, Borie F, Millat B, Berthou JC, Deleuze A, Drouard F, Guillon F, Rodier JG, Fingerhut A (2003) One hundred laparoscopic choledochotomies with primary closure of the common bile duct. Surg Endosc 17:12–18
Gigot JF, Navez B, Etienne J, Cambier E, Jadoul P, Guiot P, Kestens PJ (1997) A stratified intraoperative surgical strategy is mandatory during laparoscopic common bile duct exploration for common bile duct stones. Surg Endosc 11:722–728
Moreaux J (1995) Traditional surgical management of common bile duct stones: a prospective study during a 20 year experience. Am J Surg 169:220–226
Riciardi R, Islam S, Canete JJ, Arcand L, Stoker ME (2003) Effectiveness long-term results of laparoscopic common bile duct exploration. Surg Endosc 17:19–22
Waage A, Stromberg C, Leijonmarck CE, Ardvisson D (2003) Long-term results from laparoscopic common bile duct exploration. Surg Endosc 17:1181–1185
Tanaka M, Takahata S, Konomi H, Matsunaga H, Yokohata K, Takeda T, Utsunomiya N, Ikeda S (1998) Long term consequences of endoscopic sphincterotomy for bile duct stones. Gastrointest Endosc 48:465–469
Philips EH, Rosenthal RJ, Carroll BJ, Fallas MJ (1994) Laparoscopic trans-cystic duct common-bile-duct exploration. Surg Endosc 8:1389–1394
Tokamura H, Umezawa A, Cao H, Sakamoto N, Imaoka Y, Ouchi A, Yamamoto K (2002) Laparoscopic management of common bile duct stones: transcystic approach and choledochotomy. J Hepatobil Pancreat Surg 9:206–212
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Berthou, J.C., Dron, B., Charbonneau, P. et al. Evaluation of laparoscopic treatment of common bile duct stones in a prospective series of 505 patients: indications and results. Surg Endosc 21, 1970–1974 (2007). https://doi.org/10.1007/s00464-007-9387-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-007-9387-5