Abstract
Background
We aimed to determine if a poor response to proton pump inhibitors (PPIs) can predict a poor outcome following laparoscopic antireflux surgery (LARS) in our surgically treated population.
Methods
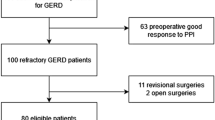
A total of 324 patients undergoing LARS were included in this study. Following standardized assessment, patients recorded the efficacy of their medication on visual analogue scales. Pre- and postoperative symptom scores were recorded, with outcomes measured by modified Visick scores.
Results
There were 233 good responders (>50% relief) and 91 poor responders (<49% relief). Both groups demonstrated a significant decline in postoperative symptom scores. Ninety-four percent of good responders had an excellent or good outcome, compared to 87% of poor responders. Twenty-seven patients reported a fair or poor outcome, despite improved postoperative symptom scores. Fifteen of these patients reported continuing heartburn; five had positive pH tests.
Conclusion
Our results do not support the assumption that a poor response to PPIs equates to a poor outcome after LARS.




Similar content being viewed by others
References
Anvari M, Allen C (2003) Surgical outcome in gastro-esophageal reflux disease patients with inadequate response to proton pump inhibitors. Surg Endosc 17: 1029–1035
Bammer T, Hinder RA, Klaus A, Klingler PJ (2001) Five- to eight-year outcome of the first laparoscopic Nissen fundoplications. J Gastrointest Surg 5:42–48
Bate CM, Griffin SM, Keeling PW, Axon ATR, Dronfield MW (1996) Reflux symptom relief in patients without unequivocal oesophagitis. Aliment Pharmacol Ther 10: 547–555
Beck IT, Champion MC, Lemire S, Thomson ABR (1997) The second Canadian consensus conference on the treatment of patients with gastroesophageal reflux disease. Can J Gastroenterol 11 (Suppl B): 7B–20B
Booth MI, Jones L, Stratford J, Dehn TCB (2002) Results of laparoscopic Nissen fundoplication at 2–8 years after surgery. Br J Surg 89: 476–481
Booth MI, Stratford J, Thompson E, Dehn TCB (2001) Laparoscopic anti-reflux surgery in the treatment of the acid-sensitive oesophagus. Br J Surg 88: 577–582
Campos GMR, Peters JH, DeMeester TR, Öberg S, Crookes PF, Tan S, DeMeester SR, Hagen JA, Bremner CG (1999) Multivariate analysis of factors predicting outcome after laparoscopic Nissen fundoplication. J Gastrointest Surg 3: 292–300
Carlsson R, Dent J, Watts J, et al. (1998) Gastro-esophageal reflux disease in primary care—an international study of different treatment strategies with omeprazole. Eur J Gastroenterol Hepatol 10:119–124
Champion G, Richter JE, Vaezi MF, Singh S, Alexander R (1994) Duodenogastroesophageal reflux: relationship to pH and importance in Barrett’s esophagus. Gastroenterology 107: 747–754
Farrell TM, Richardson WS, Trus TL, Smith CD, Hunter JG (2001) Response of atypical symptoms of gastro-oesophageal reflux to antireflux surgery. Br J Surg 88:1649–1652
Juul-Hansen P, Rydning A, Jacobsen CD, Hansen T (2001) High-dose proton-pump inhibitors as a diagnostic test of gastro-oesophageal reflux disease in endoscopic-negative patients. Scand J Gastroenterol 36: 806–810
Khajanchee YS, O’Rourke RW, Lockhart B, Patterson EJ, Hansen PD, Swanstrom LL (2002) Postoperative symptoms and failure after antireflux surgery. Arch Surg 137: 1008–1013
Lafullarde T, Watson DI, Jamieson GG, Myers JC, Game PA, Devitt PG (2001) Laparoscopic Nissen fundoplication: five-year results and beyond. Arch Surg 136:180–184
Lind T, Havelund T, Carlsson R, et al. (1997) Heartburn without oesophagitis: efficacy of omeprazole therapy and features determining therapeutic response. Scand J Gastroenterol 32: 974–979
Lundell L, Backman L, Ekstrom P, et al. (1991) Prevention of relapse of reflux esophagitis after endoscopic healing: the efficacy and safety of omeprazole compared to ranitidine. Scand J Gastroenterol 26: 248–256
Richardson WS, Trus TL, Hunter JG (1996) Laparoscopic antireflux surgery. Surg Clin North Am 76:437–450
Talley NJ (2004) Review article: gastro-oesophageal reflux disease—how wide is its span? Aliment Pharmacol Ther20 (suppl5): 27–37
Tutuian R, Castell DO (2003) Use of multichannel intraluminal impedance to document proximal esophageal and pharyngeal nonacidic reflux episodes. Am J Med 115: 119S–123S
VelaMF, Camacho-Lobato L, Srinivasan R, Tutuian R, Katz PO, Castell DO (2001) Simultaneous intraesophageal impedance and pH measurement of acid and non-acid gastroesophageal reflux: effect of omeprazole. Gastroenterology 120: 1599–1606
Watson RGP, Tham TCK, Johnston BT, McDougall NI (1997) Double blind cross-over placebo controlled study of omeprazole in the treatment of patients with reflux symptoms and physiological levels of acid reflux—the “sensitive oesophagus”. Gut 40: 587–590
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wilkerson, P., Stratford, J., Jones, L. et al. A poor response to proton pump inhibition is not a contraindication for laparoscopic antireflux surgery for gastro esophageal reflux disease. Surg Endosc 19, 1272–1277 (2005). https://doi.org/10.1007/s00464-004-2238-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-004-2238-8