Abstract
Background
Advantages of laparoscopic surgery have, among other factors, been attributed to a shorter length of abdominal incision and the use of CO2 versus air. An analysis of these factors taking pressure-induced alterations into account is lacking. The objective of the study was to determine the impact of laparoscopy and laparotomy with exposure to CO2 and room air under a similar pressure on local, systemic, and distant organ immune responses.
Methods
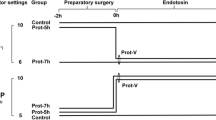
Twenty piglets were randomized into four groups: CO2 laparoscopy, air laparoscopy, CO2 laparotomy, and air laparotomy. Laparotomy was performed in a sterile balloon pressurized similar to laparoscopy. Peritoneal interleukin-1, interleukin-6, tumor necrosis factor-α, and counts of polymorphnuclear cells (PMNs), and macrophages (MFs) were determined in abdominal lavage fluids at 0, 2, and 48 h. Macrophages were assessed for reactive oxygen species (ROS) production. Systemic responses were gauged by white blood cell count (WBC) and cytokines. Alveolar lavage was performed at 48 h to determine cytokine levels, cell counts, and MF ROS production. Blood, lavage fluids, and mesenteric lymph nodes were tested for bacterial translocation.
Results
Regarding the peritoneal response, laparotomy versus laparoscopy when performed with CO2 significantly increased PMN and decreased the percentage of macrophages (%MF) up to 48 h. There was a significant increase in interleukin-6, and there was a fourfold increase in MF ROS production. Similar differences between the procedures were found with exposure to air. The use of air versus CO2 in laparoscopy, but not in laparotomy, resulted in an increase of peritoneal PMN and a decrease of the %MF up to 48 h. Air increased the local interleukin-6 release in both procedures and increased MF ROS production fourfold. Regarding the systemic response, laparotomy produced a significant increase in WBC, which was significantly more pronounced with exposure to air. No alteration of other systemic cytokines was seen. Regarding the pulmonary response, the number of MFs and MF ROS production were significantly increased after air versus CO2 laparoscopy. There were no such differences between the laparotomy groups. Regarding bacterial translocation, no bacteria were cultured from peritoneal fluids, lymphnodes, or blood.
Conclusions
Inflammatory responses were reduced by a laparoscopic approach and by exposure to CO2 versus air. Peritoneal responses were affected to a larger degree than systemic parameters. Laparotomy overruled the effects of CO2 on chemotaxis and distant organ injury but not on peritoneal cytokine release.
Similar content being viewed by others
References
Allendorf JDF, Bessler RL, Whelan RL, Trokel M, Laird DA, Terry MB, Treat MR (1997) Postoperative immune function varies inversely with the degree of surgical trauma in a murine model. Surg Endosc 11: 427–430
Bertoni G, Kuhnert P, Peterhans E, Pauli U (1993) Improved bioassay for the detection of porcine tumour necrosis factor using a homologous cell line: PK(15) J Immunol Methods 160: 267–271
Bloechle C, Emmermann A, Treu H, Achilles E, Mack D, Zornig C, Broelsch CE (1995) Effect of pneumoperitoneum on the extent and severity of peritonitis induced by gastric ulcer perforation in the rat. Surg Endosc 9: 898–901
Bloechle C, Kluth D, Holstein AF, Emmermann A, Strate T, Zornig Izbicki JR (1999) A pneumoperitoneum perpetuates severe damage to the ultrastructural integrity of parietal peritoneum in gastric perforation-induced peritonitis in rats Surg Endosc 13: 683–688
Brune IB, Wilke W, Hensler T, Holzmann B, Siewert JR (1999) Downregulation of T helper type I immune response and altered pre-inflammatory and anti-inflammatory T cell cytokine balance following conventional but not laparoscopic surgery. Am J Surg 177: 55–60
Chekan EG, Nataraj C, Clary EM, Hayward TZ, Brody FJ, Stamat JC, Fina MC, Eubanks WS, Westcott CJ (1999) Intraperitoneal immunity and pneumoperitoneum. Surg Endosc 13: 1135–1138
Collet D, Vitale GC, Reynolds M, Klar E, Cheadle WG (1995) Peritoneal host defense is less impaired by laparoscopy than by open operation. Surg Endosc 9: 1059–1064
Cruickshank AM, Fraser WD, Burns HJG, van Damme J, Shenkin A (1999) Response of serum interleukin-6 in patients undergoing elective surgery of varying severity. Clin Sci 79: 161–165
Eleftheriadis E, Kotzampassi K, Papanotas K, Heliadis N, Sarris K (1996) Gut ischemia, oxidative stress, and bacterial translocation in elevated abdominal pressure in rats. World J Surg 20: 11–16
Emmendörfer A, Hecht M, Lohmann-Matthes M, Roessler J (1990) A fast and easy method to determine the production of reactive oxygen intermediates by human and murine phagocytes using dihydrorhodamine 123. J Immunol Methods 131: 269–275
Garden DL, Granger DN (2000) Pathophysiology of ischaemia-reperfusion injury. J Pathol 190: 255–266
Glaser F, Sannwald GA, Buhr HJ, Kuntz C, Mayer H, Klee F, Herfarth C (1995) General stress response to conventional and laparoscopic cholecystectomy. Ann Surg 221: 372–380
Hell M (1988) Functional discrimination between IL6 and IL1 Eur J Immunol 18: 1535–1540
Hudson L, Hay FC (1980) Practical Immunology, 2nd ed. Blackwell Scientific, Oxford, pp 29–31
Iwanaka T, Arkovitz MS, Arya G, Ziegler MM (1977) Evaluation of operative stress and peritoneal macrophage function in minimally invasive operations. J Am Coll Surg 184: 357–363
Kirsch AJ, Hensle TW, Chang DT, Kayton ML, DeCarli AJ, Olsson CA, Sawczuk IS (1994) Renal effects of CO2 insufflation: oliguria and acute renal dysfunction in a rat pneumoperitoneum model. Urology 43: 453–459
Kloosterman T, von Blomberg ME, Borgstein P, Cuesta MA, Scheper RJ, Mijer S (1995) Unimpaired immune functions after laparoscopic cholecystectomy. Surgery 115: 424–428
Kopernik G, Avinoach E, Grossman Y, Levy R, Yulzari R, Rogachev B, Douvdevani A (1998) The effect of a high partial pressure of carbon dioxide environment on metabolism and immune functions of human peritoneal cells — relevance to carbon dioxide pneumoperitoneum. Am J Obstet Gynecol 179: 1505–1510
Lee SW, Southall JC, Gleason NR, Huang EH, Bessler M, Whelan RL (2000) Lymphocyte proliferation in mice after a full laparotomy is the same whether performed in a sealed carbon dioxide chamber or in room air. Surg Endosc 14: 233–238
Little D, Regan M, Keana RM, Bouchier-Hayes D (1993) Perioperative immune modulation. Surgery 114: 87–91
Ortega AE, Peters JH, Incarbone R, Estrada L, Ehsan A, Kwan Y, Spencer CJ, Moore-Jeffries E, Kuchta K, Nocoloff JT (1996) A prospective randomized comparison of the metabolic and stress hormonal responses of laparoscopic and open cholecystectomy. J Am Coll Surg 183: 249–256
Papadimitriou E, Lelkes PI (1993) Measurement of cell numbers in microtiter culture plates using the fluorescent dye Hoechst 33258. J Immunol Method 162: 41–45
Redmond HP, Watson RWG, Houghton T, Condron C, Watson RGK, Bouchier-Hayes D (1994) Immune function in patients undergoing open vs laparoscopic cholecystectomy. Arch Surg 129: 1240–1246
Rosenkranz AR, Schmaldienst S, Stuhlmeier KM, Chen W, Knapp W, Zlabinger GJ (1992) A microplate assay for the detection of oxidative products using 2′, 7′-dichlorofluorescin-diacetate. J Immunol Method 156: 39–45
Schoevers EJ, van Leengoed LAMG, Verheyden JHM, Niewold TA (1999) Effects of enrofloxacin on porcine phagocytic function. Antimicrob Agents Chemother 43: 2138–2143
Volz J, Köster S, Spacek Z, Paweletz N (1999) Characteristic alterations of the peritoneum after carbon dioxide pneumoperitoneum. Surg Endosc 13: 611–614
Vural B, Canturk NZ, Esen N, Solakoglu S, Canturk Z, Kirkali G, Sokmensuer C (1999) The role of neutrophils in the formation of peritoneal adhesions. Hum Reprod 14: 49–54
Walker CBJ, Duff MSc, Bruce DM, Steven MBChB, Heys SD, Gough DB, Binnie NR, Eremin O (1999) Minimal modulation of lymphocyte and natural killer cell subsets following minimal access surgery. Am J Surg 177: 48–54
Watson RWG, Redmond HP, McCarthy J, Burke PE (1995) Exposure of the peritoneal cavity to air regulates early inflammatory responses to surgery in a murine model. Br J Surg 82: 1060–1065
West MA, Hackman DJ, Baker J, Rodriguez JL, Bellingham J, Rotstein OD (1997) Mechanism of decreased in vitro murine macrophage cytokine release after exposure to carbon dioxide. Ann Surg 226: 179–190
Yoshida T, Kobayashi E, Suminaga Y, Yamauchi H, Kai T, Toyama N, Kiyozaki H, Fujimura A (1997) Hormone-cytokine response. Surg Endosc 11: 907–910
Author information
Authors and Affiliations
Additional information
Online publication: 8 February 2002
Rights and permissions
About this article
Cite this article
Ure, B.M., Niewold, T.A., Bax, N.M.A. et al. Peritoneal, systemic, and distant organ inflammatory responses are reduced by a laparoscopic approach and carbon dioxide vs air. Surg Endosc 16, 836–842 (2002). https://doi.org/10.1007/s00464-001-9093-7
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00464-001-9093-7