Abstract
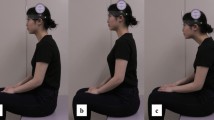
Thoracolumbar kyphosis in sitting posture is associated with forward head posture and may adversely affect swallowing function. However, few studies have investigated the effect of spinal alignment in the sitting posture on the swallowing function of older adults. This cross-sectional study aimed to investigate whether spinal alignment in the sitting posture influences the swallowing function of older adult women. Overall, 18 older adult women (mean age, 69.78 ± 3.66 years) without dysphagia were enrolled. Participants were positioned in two sitting postures, namely, comfortable sitting (CS) and thoracic upright sitting (TUS). In each sitting posture, the kyphosis index (using a flexicurve), sagittal angles (head, cervical, shoulder, and pelvic angles; using a digital camera), and cervical range of motion (ROM) were evaluated. Swallowing speed (100-mL water swallowing test), maximum tongue pressure (MTP), and oral diadochokinesis (ODK) were also evaluated. Compared with TUS, CS showed a greater kyphosis index, anterior head translation, and posterior pelvic tilt. CS had greater flexion (p < 0.001) and less extension (p < 0.001) of cervical ROM than TUS. Swallowing speed was significantly decreased in CS compared with TUS (p = 0.008). MTP and ODK were not significantly different between CS and TUS. Thus, changes in sitting posture with spinal alignment may affect swallowing speed. Consequently, adjustments to reduce sitting postural kyphosis in older adult women may improve swallowing speed.


Similar content being viewed by others
Data Availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
References
Milidonis MK, Kraus SL, Segal RL, Widmer CG. Genioglossi muscle activity in response to changes in anterior/neutral head posture. Am J Orthod Dentofacial Orthop. 1993;103:39–44. https://doi.org/10.1016/0889-5406(93)70102-T.
Paris-Alemany A, Proy-Acosta A, Adraos-Juárez D, Suso-Martí L, La Touche R, Chamorro-Sánchez J. Influence of the craniocervical posture on tongue strength and endurance. Dysphagia. 2021;36:293–302. https://doi.org/10.1007/s00455-020-10136-9.
Leigh JH, Oh BM, Seo HG, Lee GJ, Min Y, Kim K, Lee JC, Han TR. Influence of the chin-down and chin-tuck maneuver on the swallowing kinematics of healthy adults. Dysphagia. 2015;30:89–98. https://doi.org/10.1007/s00455-014-9580-3.
Matsubara K, Kumai Y, Kamenosono Y, Samejima Y, Yumoto E. Effect of three different chin-down maneuvers on swallowing pressure in healthy young adults. Laryngoscope. 2016;126:437–41. https://doi.org/10.1002/lary.25552.
Holland T, Babyar S, Carroll B, Hunt S, Sheeleigh Albright K, Wnukowski M. A preliminary study of the influence of sagittal plane neck alignment on mylohyoid activity during oropharyngeal swallowing: a surface electromyographic analysis. Cranio. 2020;38:43–9. https://doi.org/10.1080/08869634.2018.1480149.
Yoshikawa M, Nagakawa K, Tanaka R, Yamawaki K, Mori T, Hiraoka A, Higa C, Nishikawa Y, Yoshida M, Tsuga K. Improper sitting posture while eating adversely affects maximum tongue pressure. J Dent Sci. 2021;16:467–73. https://doi.org/10.1016/j.jds.2020.08.012.
Moon IY, Yi CH, Park IW, Yong JH. Effects of sitting posture and bolus volume on activation of swallowing-related muscles. J Oral Rehabil. 2020;47:577–83. https://doi.org/10.1111/joor.12934.
Nakamura K, Nagami S, Kurozumi C, Harayama S, Nakamura M, Ikeno M, Yano J, Yokoyama T, Kanai S, Fukunaga S. Effect of spinal sagittal alignment in sitting posture on swallowing function in healthy adult women: a cross-sectional study. Dysphagia. 2023;38:379–88. https://doi.org/10.1007/s00455-022-10476-8.
Lau KT, Cheung KY, Chan KB, Chan MH, Lo KY, Chiu TT. Relationships between sagittal postures of thoracic and cervical spine, presence of neck pain, neck pain severity and disability. Man Ther. 2010;15:457–62. https://doi.org/10.1016/j.math.2010.03.009.
Quek J, Pua YH, Clark RA, Bryant AL. Effects of thoracic kyphosis and forward head posture on cervical range of motion in older adults. Man Ther. 2013;18:65–71. https://doi.org/10.1016/j.math.2012.07.005.
Kado DM, Lui LY, Ensrud KE, Fink HA, Karlamangla AS, Cummings SR, Cummings SR, Study of Osteoporotic Fractures. Hyperkyphosis predicts mortality independent of vertebral osteoporosis in older women. Ann Intern Med. 2009;19:681–7.
Okura M, Ogita M, Yamamoto M, Nakai T, Numata T, Arai H. Self-assessed kyphosis and chewing disorders predict disability and mortality in community-dwelling older adults. J Am Med Dir Assoc. 2017;18:550.e1-550.e6. https://doi.org/10.1016/j.jamda.2017.02.012.
Harrison RA, Siminoski K, Vethanayagam D, Majumdar SR. Osteoporosis-related kyphosis and impairments in pulmonary function: a systematic review. J Bone Miner Res. 2007;22:447–57. https://doi.org/10.1359/jbmr.061202.
Takahashi T, Ishida K, Hirose D, Nagano Y, Okumiya K, Nishinaga M, Matsubayashi K, Doi Y, Tani T, Yamamoto H. Trunk deformity is associated with a reduction in outdoor activities of daily living and life satisfaction in community-dwelling older people. Osteoporos Int. 2005;16:273–9. https://doi.org/10.1007/s00198-004-1669-3.
Martin AR, Sornay-Rendu E, Chandler JM, Duboeuf F, Girman CJ, Delmas PD. The impact of osteoporosis on quality-of-life: the OFELY cohort. Bone. 2002;31:32–6. https://doi.org/10.1016/s8756-3282(02)00787-1.
Wakabayashi H, Kayashita J. Translation, reliability, and validity of the Japanese version of the 10-item eating assessment tool (EAT-10) for the screening of dysphagia. J Jpn Soc Parenter Enter Nutr. 2014;29:871–6.
Chen LK, Woo J, Assantachai P, Auyeung TW, Chou MY, Iijima K, Jang HC, Kang L, Kim M, Kim S, Kojima T, Kuzuya M, Lee JSW, Lee SY, Lee WJ, Lee Y, Liang CK, Lim JY, Lim WS, Peng LN, Sugimoto K, Tanaka T, Won CW, Yamada M, Zhang T, Akishita M, Arai H. Asian working group for sarcopenia: 2019 consensus update on sarcopenia diagnosis and treatment. J Am Med Dir Assoc. 2020;21:300-307.e2. https://doi.org/10.1016/j.jamda.2019.12.012.
Satake S, Arai H. The, rev. Japanese version of the Cardiovascular Health Study criteria (revised J-CHS criteria). Geriatr Gerontol Int. 2020;20:992–3.
Arai H, Satake S. English translation of the Kihon checklist. Geriatr Gerontol Int. 2015;15:518–9. https://doi.org/10.1111/ggi.12397.
Bouillanne O, Morineau G, Dupont C, Coulombel I, Vincent JP, Nicolis I, Benazeth S, Cynober L, Aussel C. Geriatric nutritional risk index: a new index for evaluating at-risk elderly medical patients. Am J Clin Nutr. 2005;82:777–83. https://doi.org/10.1093/ajcn/82.4.777.
Andersson P, Hallberg IR, Renvert S. Inter-rater reliability of an oral assessment guide for elderly patients residing in a rehabilitation ward. Spec Care Dentist. 2002;22:181–6. https://doi.org/10.1111/j.1754-4505.2002.tb00268.x.
Tsoi KK, Chan JY, Hirai HW, Wong SY, Kwok TC. Cognitive tests to detect dementia: a systematic review and meta-analysis. JAMA Intern Med. 2015;175:1450–8. https://doi.org/10.1001/jamainternmed.2015.2152.
Yonemoto K, Ishigami S, Kondo T. Joint range of motion display and measurement method. J Rehabil Med. 1995;32:207–17.
Soen S, Fukunaga M, Sugimoto T, Sone T, Fujiwara S, Endo N, Gorai I, Shiraki M, Hagino H, Hosoi T, Ohta H, Yoneda T, Tomomitsu T, Japanese Society for Bone and Mineral Research, Japan Osteoporosis Society Joint Review Committee for the Revision of the Diagnostic Criteria for Primary Osteoporosis. Diagnostic criteria for primary osteoporosis: year 2012 revision. J Bone Miner Metab. 2013;31:247–57. https://doi.org/10.1007/s00774-013-0447-8.
Audette I, Dumas JP, Côté JN, De Serres SJ. Validity and between-day reliability of the cervical range of motion (CROM) device. J Orthop Sports Phys Ther. 2010;40:318–23. https://doi.org/10.2519/jospt.2010.3180.
Milne JS, Lauder IJ. Age effects in kyphosis and lordosis in adults. Ann Hum Biol. 1974;1:327–37. https://doi.org/10.1080/03014467400000351.
Raine S, Twomey LT. Head and shoulder posture variations in 160 asymptomatic women and men. Arch Phys Med Rehabil. 1997;78:1215–23. https://doi.org/10.1016/s0003-9993(97)90335-x.
Preece SJ, Willan P, Nester CJ, Graham-Smith P, Herrington L, Bowker P. Variation in pelvic morphology may prevent the identification of anterior pelvic tilt. J Man Manip Ther. 2008;16:113–7. https://doi.org/10.1179/106698108790818459.
Wu MC, Chang YC, Wang TG, Lin LC. Evaluating swallowing dysfunction using a 100-ml water swallowing test. Dysphagia. 2004;19:43–7. https://doi.org/10.1007/s00455-003-0030-x.
Oguchi K, Saitoh E, Mizuno M, Baba M, Okui M, Suzuki M. The repetitive saliva swallowing test (RSST) as a screening test of functional dysphagia (1) normal values of RSST. Jpn J Rehabil Med. 2000;37:375–82.
Crary MA, Mann GD, Groher ME. Initial psychometric assessment of a functional oral intake scale for dysphagia in stroke patients. Arch Phys Med Rehabil. 2005;86:1516–20. https://doi.org/10.1016/j.apmr.2004.11.049.
Utanohara Y, Hayashi R, Yoshikawa M, Yoshida M, Tsuga K, Akagawa Y. Standard values of maximum tongue pressure taken using newly developed disposable tongue pressure measurement device. Dysphagia. 2008;23:286–90. https://doi.org/10.1007/s00455-007-9142-z.
Maeda K, Akagi J. Decreased tongue pressure is associated with sarcopenia and sarcopenic dysphagia in the elderly. Dysphagia. 2015;30:80–7. https://doi.org/10.1007/s00455-014-9577-y.
Watanabe Y, Hirano H, Arai H, Morishita S, Ohara Y, Edahiro A, Murakami M, Shimada H, Kikutani T, Suzuki T. Relationship between frailty and oral function in community-dwelling elderly adults. J Am Geriatr Soc. 2017;65:66–76. https://doi.org/10.1111/jgs.14355.
Tanaka T, Takahashi K, Hirano H, Kikutani T, Watanabe Y, Ohara Y, Furuya H, Tetsuo T, Akishita M, Iijima K. Oral frailty as a risk factor for physical frailty and mortality in community-dwelling elderly. J Gerontol A Biol Sci Med Sci. 2018;73:1661–7. https://doi.org/10.1093/gerona/glx225.
Yamaguchi S, Ishida M, Hidaka K, Gomi S, Takayama S, Sato K, Yoshioka Y, Wakayama N, Sekine K, Matsune S, Otsuka T, Okubo K. Relationship between swallowing function and breathing/phonation. Auris Nasus Larynx. 2018;45:533–9. https://doi.org/10.1016/j.anl.2017.08.009.
Kanda Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant. 2013;48:452–8. https://doi.org/10.1038/bmt.2012.244.
Cohen J. Statistical power analysis for the behavioral sciences. Hillsdale: Lawrence Erlbaum Associates Inc.; 1988.
Hughes TA, Wiles CM. Clinical measurement of swallowing in health and in neurogenic dysphagia. QJM. 1996;89:109–16. https://doi.org/10.1093/qjmed/89.2.109.
Suzuki M, Koyama S, Kimura Y, Ishiyama D, Ohji S, Otobe Y, Nishio N, Kunieda Y, Ichikawa T, Ito D, Ogawa H, Yamada M. Relationship between tongue muscle quality and swallowing speed in community-dwelling older women. Aging Clin Exp Res. 2020;32:2073–9. https://doi.org/10.1007/s40520-019-01388-z.
Nathadwarawala KM, Nicklin J, Wiles CM. A timed test of swallowing capacity for neurological patients. J Neurol Neurosurg Psychiatry. 1992;55:822–5. https://doi.org/10.1136/jnnp.55.9.822.
Patterson JM, McColl E, Carding PN, Kelly C, Wilson JA. Swallowing performance in patients with head and neck cancer: a simple clinical test. Oral Oncol. 2009;45:904–7. https://doi.org/10.1016/j.oraloncology.2009.03.012.
Suzuki M, Kimura Y, Otobe Y, Kikuchi T, Masuda H, Taguchi R, Tanaka S, Narita Y, Shino S, Kusumi H, Yamada M. Relationship between sarcopenia and swallowing capacity in community-dwelling older women. Gerontology. 2020;66:549–52. https://doi.org/10.1159/000511359.
Chen YC, Chen PY, Wang YC, Wang TG, Han DS. Decreased swallowing function in the sarcopenic elderly without clinical dysphagia: a cross-sectional study. BMC Geriatr. 2020;20:419. https://doi.org/10.1186/s12877-020-01832-0.
Tamai T, Hara K, Nakagawa K, Namiki C, Yamaguchi K, Yoshimi K, Yanagida R, Hasegawa S, Nakane A, Okumura T, Ishii M, Tohara H. Strength and morphology of a suprahyoid muscle and their relationship to forward head posture in healthy older adults. Geriatr Gerontol Int. 2022;22:779–84. https://doi.org/10.1111/ggi.14457.
Tashiro M, Honda Y, Ohkubo M, Sugiyama T, Ishida R. Influence of cervical, thoracic and lumbar spines, and shoulder girdle range of motion on swallowing function of dependent older adults. Geriatr Gerontol Int. 2017;17:2565–72. https://doi.org/10.1111/ggi.13097.
Okada S, Saitoh E, Palmer JB, Matsuo K, Yokoyama M, Shigeta R, Baba M. What is the chin-down posture? A questionnaire survey of speech language pathologists in Japan and the United States. Dysphagia. 2007;22:204–9. https://doi.org/10.1007/s00455-006-9073-0.
Bartynski WS, Heller MT, Grahovac SZ, Rothfus WE, Kurs-Lasky M. Severe thoracic kyphosis in the older patient in the absence of vertebral fracture: association of extreme curve with age. AJNR Am J Neuroradiol. 2005;26:2077–85.
Acknowledgements
I would like to thank Nanami Mizukami and Suzuka Komatsu for their contribution to data collection. This work was conducted with the support of Kawasaki Medical School. This study was supported by grants from the KAWASAKI Foundation for Medical Science and Medical Welfare.
Funding
This study was supported by grants from the KAWASAKI Foundation for Medical Science and Medical Welfare.
Author information
Authors and Affiliations
Contributions
KN contributed to the protocol design, data collection and analysis, and writing of the manuscript. SN contributed to the protocol design, data collection and analysis, and writing of the manuscript and supervised the study. SF contributed to the protocol design, data collection and analysis, and writing of the manuscript. AS performed the data collection and reviewed the manuscript. YK and NO contributed to the review of the manuscript. SK contributed to the protocol design, data collection and analysis, and writing of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no conflicts of interest.
Ethical Approval
All study protocols were approved by the Ethics Committee of the Kawasaki Medical School in Okayama, Japan (Approval No. 5794-00), and all participants provided written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nakamura, K., Nagami, S., Fukunaga, S. et al. Influence of Spinal Sagittal Alignment in Sitting Posture on the Swallowing Speed of Older Adult Women: A Cross-Sectional Study. Dysphagia (2024). https://doi.org/10.1007/s00455-023-10657-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00455-023-10657-z