Abstract
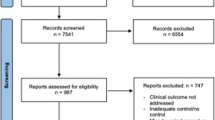
Dysphagia management is a core component of quality stroke care. Speech–Language Pathologists (SLPs) play a key role in the management of post-stroke dysphagia. We sought to elicit perceptions, attitudes, and practice patterns regarding post-stroke dysphagia management among SLPs in the United States. We conducted a survey among SLPs registered with the American Speech–Language–Hearing Association who indicated that they care for acute stroke patients. A total of 336 participants completed the survey. Over half of the participants (58.6%) indicated that they obtain objective swallow testing in ≥ 60% of their post-stroke dysphagia patients. Almost 1 in 5 SLPs indicated that they are often unable to perform objective dysphagia testing due to limited resources (18.8% indicated resource limitations; 78.9% indicated no resources limitations; 2.4% were unsure). SLPs in hospitals without stroke center certification had higher odds of indicating limited resources compared to SLPs in certified stroke centers (OR 2.08, 95% CI 1.11–3.87). Over 75% indicated that percutaneous endoscopic gastrostomy (PEG) tubes after stroke are placed too early. SLPs who obtain objective swallow testing in ≥ 60% of patients had higher odds of indicating that PEG tubes are placed too early (OR 1.70, 95% CI 1.13–2.56). While 19.4% indicated that the optimal timing for PEG after stroke is < 7 days after admission, 25.0% indicated that the optimal timing is > 12 days. Almost 35% indicated that health care system pressures influence their recommendations, and 47.6% indicated that ≥ 25% of PEGs could be avoided if patients were given up to 7 more days for swallowing recovery.


Similar content being viewed by others
References
Martino R, Foley N, Bhogal S, Diamant N, Speechley M, Teasell R. Dysphagia after stroke: incidence, diagnosis, and pulmonary complications. Stroke. 2005;36:2756–63.
Falsetti P, Acciai C, Palilla R, Bosi M, Carpinteri F, Zingarelli A, Pedace C, Lenzi L. Oropharyngeal dysphagia after stroke: incidence, diagnosis, and clinical predictors in patients admitted to a neurorehabilitation unit. J Stroke Cerebrovasc Dis. 2009;18:329–35.
Joundi RA, Martino R, Saposnik G, Giannakeas V, Fang J, Kapral MK. Predictors and outcomes of dysphagia screening after acute ischemic stroke. Stroke. 2017;48:900–6.
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL. Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the american heart association/american stroke association. Stroke. 2019;50:e344–418.
Bateman C, Leslie P, Drinnan MJ. Adult dysphagia assessment in the UK and Ireland: are SLTs assessing the same factors? Dysphagia. 2007;22:174–86.
Martino R, Pron G, Diamant NE. Oropharyngeal dysphagia: surveying practice patterns of the speech-language pathologist. Dysphagia. 2004;19:165–76.
McAllister S, Kruger S, Doeltgen S, Tyler-Boltrek E. Implications of variability in clinical bedside swallowing assessment practices by speech language pathologists. Dysphagia. 2016;31:650–62.
Pettigrew CM, O’Toole C. Dysphagia evaluation practices of speech and language therapists in Ireland: clinical assessment and instrumental examination decision-making. Dysphagia. 2007;22:235–44.
Vogels B, Cartwright J, Cocks N. The bedside assessment practices of speech-language pathologists in adult dysphagia. Int J Speech Lang Pathol. 2015;17:390–400.
Vose AK, Kesneck S, Sunday K, Plowman E, Humbert I. A survey of clinician decision making when identifying swallowing impairments and determining treatment. J Speech Lang Hear Res. 2018;61:2735–56.
Dennis MS, Lewis SC, Warlow C, Collaboration FT. Effect of timing and method of enteral tube feeding for dysphagic stroke patients (FOOD): a multicentre randomised controlled trial. Lancet. 2005;365:764–72.
Dennis MS, Lewis SC, Warlow C, Collaboration FT. Routine oral nutritional supplementation for stroke patients in hospital (FOOD): a multicentre randomised controlled trial. Lancet. 2005;365:755–63.
Joundi RA, Saposnik G, Martino R, Fang J, Porter J, Kapral MK. Outcomes among patients with direct enteral vs nasogastric tube placement after acute stroke. Neurology. 2018;90:e544–52.
Wilmskoetter J, Simpson AN, Logan SL, Simpson KN, Bonilha HS. Impact of gastrostomy feeding tube placement on the 1-year trajectory of care in patients after stroke. Nutr Clin Pract. 2018;33:553–66.
Wilmskoetter J, Simpson KN, Bonilha HS. Hospital readmissions of stroke patients with percutaneous endoscopic gastrostomy feeding tubes. J Stroke Cerebrovasc Dis. 2016;25:2535–42.
Burgos R, Breton I, Cereda E, Desport JC, Dziewas R, Genton L, Gomes F, Jesus P, Leischker A, Muscaritoli M, Poulia KA, Preiser JC, Van der Marck M, Wirth R, Singer P, Bischoff SC. ESPEN guideline clinical nutrition in neurology. Clin Nutr. 2018;37:354–96.
Wirth R, Smoliner C, Jager M, Warnecke T, Leischker AH, Dziewas R. Committee* DS: guideline clinical nutrition in patients with stroke. Exp Transl Stroke Med. 2013;5:14.
George BP, Kelly AG, Albert GP, Hwang DY, Holloway RG. Timing of percutaneous endoscopic gastrostomy for acute ischemic stroke: an observational study from the us nationwide inpatient sample. Stroke. 2017;48:420–7.
Wilmskoetter J, Simpson AN, Simpson KN, Bonilha HS. Practice patterns of percutaneous endoscopic gastrostomy tube placement in acute stroke: are the guidelines achievable? J Stroke Cerebrovasc Dis. 2016;25:2694–700.
Faigle R, Cooper LA, Gottesman RF. Race differences in gastrostomy tube placement after stroke in majority-white, minority-serving, and racially integrated US hospitals. Dysphagia. 2018;33:636–44.
Hwang DY, George BP, Kelly AG, Schneider EB, Sheth KN, Holloway RG. Variability in gastrostomy tube placement for intracerebral hemorrhage patients at US hospitals. J Stroke Cerebrovasc Dis. 2018;27:978–87.
Dziewas R, Allescher HD, Aroyo I, Bartolome G, Beilenhoff U, Bohlender J, Breitbach-Snowdon H, Fheodoroff K, Glahn J, Heppner HJ, Hormann K, Ledl C, Lucking C, Pokieser P, Schefold JC, Schroter-Morasch H, Schweikert K, Sparing R, Trapl-Grundschober M, Wallesch C, Warnecke T, Werner CJ, Wessling J, Wirth R, Pflug C. Diagnosis and treatment of neurogenic dysphagia - S1 guideline of the German Society of Neurology. Neurol Res Pract. 2021;3:23.
Dziewas R, Michou E, Trapl-Grundschober M, Lal A, Arsava EM, Bath PM, Clave P, Glahn J, Hamdy S, Pownall S, Schindler A, Walshe M, Wirth R, Wright D, Verin E. European stroke organisation and european society for swallowing disorders guideline for the diagnosis and treatment of post-stroke dysphagia. Eur Stroke J. 2021. https://doi.org/10.1177/23969873211039721.
Gomes CA Jr, Andriolo RB, Bennett C, Lustosa SA, Matos D, Waisberg DR, Waisberg J. Percutaneous endoscopic gastrostomy versus nasogastric tube feeding for adults with swallowing disturbances. Cochrane Database Syst Rev. 2015. https://doi.org/10.1002/14651858.CD008096.pub4.
Galovic M, Stauber AJ, Leisi N, Krammer W, Brugger F, Vehoff J, Balcerak P, Muller A, Muller M, Rosenfeld J, Polymeris A, Thilemann S, De Marchis GM, Niemann T, Leifke M, Lyrer P, Saladin P, Kahles T, Nedeltchev K, Sarikaya H, Jung S, Fischer U, Manno C, Cereda CW, Sander JW, Tettenborn B, Weder BJ, Stoeckli SJ, Arnold M, Kagi G. Development and validation of a prognostic model of swallowing recovery and enteral tube feeding after ischemic stroke. JAMA Neurol. 2019;76:561–70.
Burgermaster M, Slattery E, Islam N, Ippolito PR, Seres DS. Regional comparison of enteral nutrition-related admission policies in skilled nursing facilities. Nutr Clin Pract. 2016;31:342–8.
Funding
Dr. Faigle is supported by a National Institute of Neurological Disorders and Stroke career development award (K23NS101124).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, B.J., Suolang, D., Frost, N. et al. Practice Patterns and Attitudes Among Speech–Language Pathologists Treating Stroke Patients with Dysphagia: A Nationwide Survey. Dysphagia 37, 1715–1722 (2022). https://doi.org/10.1007/s00455-022-10432-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-022-10432-6