Abstract
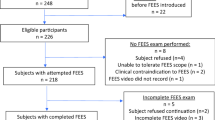
Quantitative measures of swallowing function were extracted from modified barium swallowing studies (MBS) to characterize swallowing pathophysiology in patients with unilateral vocal fold immobility (UVFI). All individuals with UVFI completing a MBS during the prior 5 years were included. Demographic information, penetration-aspiration score, timing of aspiration and quantitative measures from the MBS were extracted from electronic medical records and compared across 1, 3, and 20 cc liquid bolus swallows. UVFI patient measures were compared to normal age-matched controls to identify swallowing pathophysiology associated with aspiration. The incidence of aspiration by UVFI etiology groups (i.e., central nervous system, idiopathic, iatrogenic, skull base tumor, or peripheral tumor) was also compared. Of the 61 patients who met inclusion criteria, aspiration was observed in 23%. Maximum pharyngeal constriction was abnormal in 79% of aspirators compared to 34% of non-aspirators (p = .003). Delay in airway closure was the most common swallowing abnormality identified in the study population (62%) but was not associated with aspiration. Among the 14 individuals who aspirated, the iatrogenic and skull base tumor etiology groups comprised the majority (i.e., 36% each). However, the incidence of aspiration for the iatrogenic group was 19% compared to 50% of the skull base tumor group. Aspiration in patients with UVFI was associated with abnormally reduced pharyngeal constriction. Delayed airway closure was common in both aspirators and non-aspirators.

Similar content being viewed by others
References
Tsai MS, et al. Unilateral vocal fold paralysis and risk of pneumonia: a nationwide population-based cohort study. Otolaryngol Head Neck Surg. 2018;158(5):896–903.
Damrose EJ. Percutaneous injection laryngoplasty in the management of acute vocal fold paralysis. Laryngoscope. 2010;120(8):1582–90.
Zuniga SA, Ebersole B, Jamal N. Utility of eating assessment tool-10 in predicting aspiration in patients with unilateral vocal fold paralysis. Otolaryngol Head Neck Surg. 2018;159(1):92–6.
Zhou D, Jafri M, Husain I. Identifying the prevalence of dysphagia among patients diagnosed with unilateral vocal fold immobility. Otolaryngol Head Neck Surg. 2019;160(6):955–64.
Gould FD, et al. The physiologic impact of unilateral recurrent laryngeal nerve (RLN) lesion on infant oropharyngeal and esophageal performance. Dysphagia. 2015;30(6):714–22.
Schiedermayer B, et al. Prevalence, incidence, and characteristics of dysphagia in those with unilateral vocal fold paralysis. Laryngoscope. 2019. https://doi.org/10.1002/lary.28401.
Ellerston JK, et al. Quantitative measures of swallowing deficits in patients with parkinson’s disease. Ann Otol Rhinol Laryngol. 2016;125(5):385–92.
Kendall KA, et al. Objective measures of swallowing function applied to the dysphagia population: a one year experience. Dysphagia. 2016;31(4):538–46.
Kendall KA. Evaluation of airway protection: quantitative timing measures versus penetration/aspiration score. Laryngoscope. 2017;127(10):2314–8.
Rosenbek JC, et al. A penetration-aspiration scale. Dysphagia. 1996;11(2):93–8.
Kendall KA, et al. Timing of events in normal swallowing: a videofluoroscopic study. Dysphagia. 2000;15(2):74–83.
Matson JL, Fodstad JC, Boisjoli JA. Cutoff scores, norms and patterns of feeding problems for the Screening Tool of fEeding Problems (STEP) for adults with intellectual disabilities. Res Dev Disabil. 2008;29(4):363–72.
Nayak VK, et al. Patterns of swallowing failure following medialization in unilateral vocal fold immobility. Laryngoscope. 2002;112(10):1840–4.
Ha JF. Unilateral vocal fold palsy & dysphagia: a review. Auris Nasus Larynx. 2020. https://doi.org/10.1016/j.anl.2020.03.001.
Mu L, Sanders I. Neuromuscular specializations within human pharyngeal constrictor muscles. Ann Otol Rhinol Laryngol. 2007;116(8):604–17.
Domer AS, Leonard R, Belafsky PC. Pharyngeal weakness and upper esophageal sphincter opening in patients with unilateral vocal fold immobility. Laryngoscope. 2014;124(10):2371–4.
Cates DJ, et al. Effect of vocal fold medialization on dysphagia in patients with unilateral vocal fold immobility. Otolaryngol Head Neck Surg. 2016;155(3):454–7.
Anis MM, Memon Z. Injection medialization laryngoplasty improves dysphagia in patients with unilateral vocal fold immobility. World J Otorhinolaryngol Head Neck Surg. 2018;4(2):126–9.
Tibbetts KM, et al. Etiology and long-term functional swallow outcomes in pediatric unilateral vocal fold immobility. Int J Pediatr Otorhinolaryngol. 2016;88:179–83.
Kammer RE, et al. High-resolution manometry and swallow outcomes after vocal fold injection medialization for unilateral vocal fold paralysis/paresis. Head Neck. 2019;41(7):2389–97.
DeLozier KR, et al. Impact of recurrent laryngeal nerve lesion on oropharyngeal muscle activity and sensorimotor integration in an infant pig model. J Appl Physiol. 2018;125(1):159–66.
Funding
This investigation was supported by the University of Utah Study Design and Biostatistics Center, with funding in part from the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health, through Grant UL1TR002538 (formerly 5UL1TR001067-05, 8UL1TR000105 and UL1RR025764). Partial support was also provided by the National Institutes on Deafness and Other Communication Disorders through Grant R01DC011311. All authors have approved the manuscript and have agreed to its contents. All authors certify that they have no financial disclosures related to this work. All authors certify that they have no conflict of interest to report in relation to this work.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Stevens, M., Schiedermayer, B., Kendall, K.A. et al. Physiology of Dysphagia in Those with Unilateral Vocal Fold Immobility. Dysphagia 37, 356–364 (2022). https://doi.org/10.1007/s00455-021-10286-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-021-10286-4