Abstract
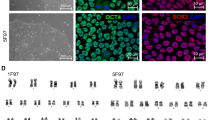
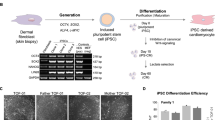
Cardiovascular diseases, atherosclerosis, and strokes are the most common causes of death in patients with Hutchinson-Gilford progeria syndrome (HGPS). The LMNA variant c.1824C > T accounts for ~ 90% of HGPS cases. The detailed molecular mechanisms of Lamin A in the heart remain elusive due to the lack of appropriate in vitro models. We hypothesize that HGPS patient’s induced pluripotent stem cell (iPSC)-derived cardiomyocytes (iCMCs) will provide a model platform to study the cardio-pathologic mechanisms associated with HGPS. To elucidate the effects of progerin in cardiomyocytes, we first obtained skin fibroblasts (SFs) from a de-identified HGPS patient (hPGP1, proband) and both parents from the Progeria Research Foundation. Through Sanger sequencing and restriction fragment length polymorphism, with the enzyme EciI, targeting Lamin A, we characterized hPGP1-SFs as heterozygous mutants for the LMNA variant c.1824 C > T. Additionally, we performed LMNA exon 11 bisulfite sequencing to analyze the methylation status of the progeria cells. Furthermore, we reprogrammed the three SFs into iPSCs and differentiated them into iCMCs, which gained a beating on day 7. Through particle image velocimetry analysis, we found that hPGP1-iCMCs had an irregular contractile function and decreased cardiac-specific gene and protein expressions by qRT-PCR and Western blot. Our progeria-patient-derived iCMCs were found to be functionally and structurally defective when compared to normal iCMCs. This in vitro model will help in elucidating the role of Lamin A in cardiac diseases and the cardio-pathologic mechanisms associated with progeria. It provides a new platform for researchers to study novel treatment approaches for progeria-associated cardiac diseases.







Similar content being viewed by others
Data availability
The datasets used or analyzed in this study and the reprogrammed cells are available from the corresponding author on reasonable request.
References
Benzoni P, Campostrini G, Landi S, Bertini V, Marchina E, Iascone M, Ahlberg G, Olesen MS, Crescini E, Mora C, Bisleri G, Muneretto C, Ronca R, Presta M, Poliani PL, Piovani G, Verardi R, Di Pasquale E, Consiglio A, Dell’Era P (2019) Human iPSC modelling of a familial form of atrial fibrillation reveals a gain of function of If and ICaL in patient-derived cardiomyocytes. Cardiovasc Res 116(6):1147–1160. https://doi.org/10.1093/cvr/cvz217
Bishop WR, Doll R, Kirschmeier P (2011) 15 - Farnesyl Transferase inhibitors: from targeted cancer therapeutic to a potential treatment for progeria. In: Tamanoi F, Hrycyna CA, Bergo MO (eds) The Enzymes, vol 29. Academic Press, pp 275–303
Bolderson E, Burgess JT, Li J, Gandhi NS, Boucher D, Croft LV, Beard S, Plowman JJ, Suraweera A, Adams MN, Naqi A, Zhang SD, Sinclair DA, O’Byrne KJ, Richard DJ (2019) Barrier-to-autointegration factor 1 (Banf1) regulates poly [ADP-ribose] polymerase 1 (PARP1) activity following oxidative DNA damage. Nat Commun 10(1):5501. https://doi.org/10.1038/s41467-019-13167-5
Bonne G, Barletta MRD, Varnous S, Bécane H-M, Hammouda E-H, Merlini L, Muntoni F, Greenberg CR, Gary F, Urtizberea J-A (1999) Mutations in the gene encoding lamin A/C cause autosomal dominant Emery-Dreifuss muscular dystrophy. Nat Genet 21(3):285–288
Brodsky GL, Muntoni F, Miocic S, Sinagra G, Sewry C, Mestroni L (2000) Lamin A/C gene mutation associated with dilated cardiomyopathy with variable skeletal muscle involvement. Circulation 101(5):473–476
Burgess JT, Cheong CM, Suraweera A, Sobanski T, Beard S, Dave K, Rose M, Boucher D, Croft LV, Adams MN, O’Byrne K, Richard DJ, Bolderson E (2021) Barrier-to-autointegration-factor (Banf1) modulates DNA double-strand break repair pathway choice via regulation of DNA-dependent kinase (DNA-PK) activity. Nucleic Acids Res 49(6):3294–3307. https://doi.org/10.1093/nar/gkab110
Cattin M-E, Muchir A, Bonne G (2013) ‘State-of-the-heart’ of cardiac laminopathies. Curr Opin Cardiol 28(3):297–304. https://doi.org/10.1097/HCO.0b013e32835f0c79
Chen CY, Chi YH, Mutalif RA, Starost MF, Myers TG, Anderson SA, Stewart CL, Jeang KT (2012) Accumulation of the inner nuclear envelope protein Sun1 is pathogenic in progeric and dystrophic laminopathies. Cell 149(3):565–577. https://doi.org/10.1016/j.cell.2012.01.059
Chen ZJ, Wang WP, Chen YC, Wang JY, Lin WH, Tai LA, Liou GG, Yang CS, Chi YH (2014) Dysregulated interactions between lamin A and SUN1 induce abnormalities in the nuclear envelope and endoplasmic reticulum in progeric laminopathies. J Cell Sci 127(Pt 8):1792–1804. https://doi.org/10.1242/jcs.139683
Cheng CJ, Wu YC, Shu JA, Ling TY, Kuo HC, Wu JY, Chang EE, Chang SC, Huang YH (2007) Aberrant expression and distribution of the OCT-4 transcription factor in seminomas. J Biomed Sci 14(6):797–807. https://doi.org/10.1007/s11373-007-9198-7
Czirok A, Isai DG, Kosa E, Rajasingh S, Kinsey W, Neufeld Z, Rajasingh J (2017) Optical-flow based non-invasive analysis of cardiomyocyte contractility. Sci Rep 7(1):1–11
Dharmaraj T, Guan Y, Liu J, Badens C, Gaborit B, Wilson KL (2019) Rare BANF1 alleles and relatively frequent EMD alleles including ‘healthy lipid’ emerin p.D149H in the ExAC cohort. Front Cell Dev Biol 7:48. https://doi.org/10.3389/fcell.2019.00048
Dhillon S (2021) Lonafarnib: first approval. Drugs 81(2):283–289
Eriksson M, Brown WT, Gordon LB, Glynn MW, Singer J, Scott L, Erdos MR, Robbins CM, Moses TY, Berglund P (2003) Recurrent de novo point mutations in lamin A cause Hutchinson-Gilford progeria syndrome. Nature 423(6937):293–298
Fatkin D, MacRae C, Sasaki T, Wolff MR, Porcu M, Frenneaux M, Atherton J, Vidaillet HJ Jr, Spudich S, De Girolami U (1999) Missense mutations in the rod domain of the lamin A/C gene as causes of dilated cardiomyopathy and conduction-system disease. N Engl J Med 341(23):1715–1724
Gilford H (1904) Progeria: a form of senilism. Practitioner 73:188–217
Gonzalez JM, Pla D, Perez-Sala D, Andres V (2011) A-type lamins and Hutchinson-Gilford progeria syndrome: pathogenesis and therapy
Gordon LB (2010) The premature aging syndrome Hutchinson-Gilford progeria: insights into normal aging. In Brocklehurst's Textbook of Geriatric Medicine and Gerontology. Elsevier, pp 66–72
Gordon LB, Rothman FG, López-Otín C, Misteli T (2014) Progeria: a paradigm for translational medicine. Cell 156(3):400–407
Gordon LB, Shappell H, Massaro J, D’Agostino RB, Brazier J, Campbell SE, Kleinman ME, Kieran MW (2018) Association of lonafarnib treatment vs no treatment with mortality rate in patients with Hutchinson-Gilford progeria syndrome. JAMA 319(16):1687–1695
Gurusamy N, Rajasingh S, Sigamani V, Rajasingh R, Isai DG, Czirok A, Bittel D, Rajasingh J (2021) Noonan syndrome patient-specific induced cardiomyocyte model carrying SOS1 gene variant c.1654A>G. Exp Cell Res 400(1):112508. https://doi.org/10.1016/j.yexcr.2021.112508
Haque F, Lloyd DJ, Smallwood DT, Dent CL, Shanahan CM, Fry AM, Trembath RC, Shackleton S (2006) SUN1 interacts with nuclear lamin A and cytoplasmic nesprins to provide a physical connection between the nuclear lamina and the cytoskeleton. Mol Cell Biol 26(10):3738–3751. https://doi.org/10.1128/mcb.26.10.3738-3751.2006
Haque F, Mazzeo D, Patel JT, Smallwood DT, Ellis JA, Shanahan CM, Shackleton S (2010) Mammalian SUN protein interaction networks at the inner nuclear membrane and their role in laminopathy disease processes. J Biol Chem 285(5):3487–3498. https://doi.org/10.1074/jbc.M109.071910
Hasselberg NE, Haland TF, Saberniak J, Brekke PH, Berge KE, Leren TP, Edvardsen T, Haugaa KH (2017) Lamin A/C cardiomyopathy: young onset, high penetrance, and frequent need for heart transplantation. Eur Heart J 39(10):853–860. https://doi.org/10.1093/eurheartj/ehx596
Hennekam RC (2006) Hutchinson-Gilford progeria syndrome: review of the phenotype. Am J Med Genet A 140(23):2603–2624. https://doi.org/10.1002/ajmg.a.31346
Hutchinson J (1886a) Congenital absence of hair and mammary glands with atrophic condition of the skin and its appendages, in a boy whose mother had been almost wholly bald from alopecia areata from the age of six. Med Chir Trans 69:473–477. https://doi.org/10.1177/095952878606900127
Hutchinson J (1886b) Congenital absence of hair and mammary glands with atrophic condition of the skin and its appendages, in a boy whose mother had been almost wholly bald from alopecia areata from the age of six. Med Chir Trans 69:473
Kychygina A, Dall’Osto, M., Allen, J. A., Cadoret, J.-C., Piras, V., Pickett, H. A., & Crabbe, L. (2021) Progerin impairs 3D genome organization and induces fragile telomeres by limiting the dNTP pools. Sci Rep 11(1):1–20
Loo TH, Ye X, Chai RJ, Ito M, Bonne G, Ferguson-Smith AC, Stewart CL (2019) The mammalian LINC complex component SUN1 regulates muscle regeneration by modulating drosha activity. Elife 8. https://doi.org/10.7554/eLife.49485
Mattioli E, Columbaro M, Capanni C, Maraldi NM, Cenni V, Scotlandi K, Marino MT, Merlini L, Squarzoni S, Lattanzi G (2011) Prelamin A-mediated recruitment of SUN1 to the nuclear envelope directs nuclear positioning in human muscle. Cell Death Differ 18(8):1305–1315. https://doi.org/10.1038/cdd.2010.183
Meta M, Yang SH, Bergo MO, Fong LG, Young SG (2006) Protein farnesyltransferase inhibitors and progeria. Trends Mol Med 12(10):480–487. https://doi.org/10.1016/j.molmed.2006.08.006
Muchir A, Bonne G, van der Kooi AJ, van Meegen M, Baas F, Bolhuis PA, de Visser M, Schwartz K (2000) Identification of mutations in the gene encoding lamins A/C in autosomal dominant limb girdle muscular dystrophy with atrioventricular conduction disturbances (LGMD1B). Hum Mol Genet 9(9):1453–1459
Muchir A, Pavlidis P, Decostre V, Herron AJ, Arimura T, Bonne G, Worman HJ (2007) Activation of MAPK pathways links LMNA mutations to cardiomyopathy in Emery-Dreifuss muscular dystrophy. J Clin Investig 117(5):1282–1293
Östlund C, Chang W, Gundersen GG, Worman HJ (2019) Pathogenic mutations in genes encoding nuclear envelope proteins and defective nucleocytoplasmic connections. Exp Biol Med (maywood) 244(15):1333–1344. https://doi.org/10.1177/1535370219862243
Paquet N, Box JK, Ashton NW, Suraweera A, Croft LV, Urquhart AJ, Bolderson E, Zhang SD, O’Byrne KJ, Richard DJ (2014) Néstor-Guillermo progeria syndrome: a biochemical insight into barrier-to-autointegration factor 1, alanine 12 threonine mutation. BMC Mol Biol 15:27. https://doi.org/10.1186/s12867-014-0027-z
Perepelina K, Zaytseva A, Khudiakov A, Neganova I, Vasichkina E, Malashicheva A, Kostareva A (2022) LMNA mutation leads to cardiac sodium channel dysfunction in the Emery-Dreifuss muscular dystrophy patient. Front Cardiovasc Med 9:932956. https://doi.org/10.3389/fcvm.2022.932956
Pollex R, Hegele RA (2004) Hutchinson-Gilford progeria syndrome. Clin Genet 66(5):375–381
Prakash A, Gordon LB, Kleinman ME, Gurary EB, Massaro J, D’Agostino R, Kieran MW, Gerhard-Herman M, Smoot L (2018) Cardiac abnormalities in patients with Hutchinson-Gilford progeria syndrome. JAMA Cardiol 3(4):326–334
Puente XS, Quesada V, Osorio FG, Cabanillas R, Cadiñanos J, Fraile JM, Ordóñez GR, Puente DA, Gutiérrez-Fernández A, Fanjul-Fernández M, Lévy N, Freije JM, López-Otín C (2011) Exome sequencing and functional analysis identifies BANF1 mutation as the cause of a hereditary progeroid syndrome. Am J Hum Genet 88(5):650–656. https://doi.org/10.1016/j.ajhg.2011.04.010
Rajasingh S, Thangavel J, Czirok A, Samanta S, Roby KF, Dawn B, Rajasingh J (2015) Generation of functional cardiomyocytes from efficiently generated human iPSCs and a novel method of measuring contractility. PLoS ONE 10(8)
Sánchez-López A, Espinós-Estévez C, González-Gómez C, Gonzalo P, Andrés-Manzano MJ, Fanjul V, Riquelme-Borja R, Hamczyk MR, Macías Á, Del Campo L (2021) Cardiovascular progerin suppression and lamin A restoration rescue Hutchinson-Gilford progeria syndrome. Circulation 144(22):1777–1794
Ullrich NJ, Gordon LB (2015) Hutchinson-Gilford progeria syndrome. Handb Clin Neurol 132:249–264
Zangrossi S, Marabese M, Broggini M, Giordano R, D’Erasmo M, Montelatici E, Intini D, Neri A, Pesce M, Rebulla P, Lazzari L (2007) Oct-4 expression in adult human differentiated cells challenges its role as a pure stem cell marker. Stem Cells 25(7):1675–1680. https://doi.org/10.1634/stemcells.2006-0611
Funding
This work was supported in part by the American Heart Association–Transformational Project Award 20TPA35490215 to JR, National Institute of Health R01 grant HL141345 to JR, and the American Heart Association postdoctoral award 952237 to SP.
Author information
Authors and Affiliations
Contributions
Conceptualization, J.R., SP.; methodology, S.R., V.S., S.P., A.C.; validation and formal analysis, SP., S.R, V.S.; writing—original draft preparation, V.S., S.P.; writing—review and editing, J.R., S.P., S.R.; supervision, J.R.; project administration, S.R., J.R; funding acquisition, J.R. All authors have read and agreed to the current version of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Conflict of interest
The authors declare no conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Perales, S., Sigamani, V., Rajasingh, S. et al. Hutchinson-Gilford progeria patient-derived cardiomyocyte model of carrying LMNA gene variant c.1824 C > T. Cell Tissue Res 394, 189–207 (2023). https://doi.org/10.1007/s00441-023-03813-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-023-03813-2