Abstract
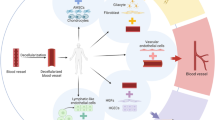
Non-destructive imaging strategies to monitor long-term cultures is essential for vascular engineering. The goal of this study is to investigate whether optical coherence tomography (OCT) can be a suitable approach to monitor the long-term remodeling process of biodegradable polymeric scaffold-based tissue-engineered vascular grafts (TEVG) after pulsatile stimulation and to observe polymeric scaffold degradation during bioreactor cultivation. In the present study, a perfusion system driven by a ventricular assist device was provided for a three-dimensional culture system as a pulsatile force. We characterized the structural features of wall thickness and polyglycolic acid degradation based on optical signal attenuation using catheter-based OCT. Scanning electron microscopy confirmed morphological changes. Also, polymer degradation and the detection of different types of collagen was visualized after 4 weeks of culture by means of polarized microscopy. Findings on OCT imaging correlated with those on histological examination and revealed the effects of pulsatile stimulation on the development of engineered vessels. This finding demonstrated that real-time imaging with OCT may be a promising tool for monitoring the growth and remodeling characterization of TEVG and provide a basis to promote the ideal and long-term culture of vascular tissue engineering.









Similar content being viewed by others
Abbreviations
- bFGF:
-
Basic fibroblast growth factor
- ECM:
-
Extracellular matrix
- ePTFE:
-
Expanded polytetrafluoroethylene
- HE:
-
Hematoxylin and eosin
- NLOM:
-
Nonlinear optical microscopy
- OCT:
-
Optical coherence tomography
- PDGF:
-
Platelet-derived growth factor
- PGA:
-
Polyglycolic acid
- SEM:
-
Scanning electron microscopy
- TEVG:
-
Tissue-engineered vascular grafts
- VSMCs:
-
Vascular smooth muscle cells
References
Appel AA, Anastasio MA, Larson JC, Brey EM (2013) Imaging challenges in biomaterials and tissue engineering. Biomaterials 34:6615–6630
Ballyns JJ, Bonassar LJ (2009) Image-guided tissue engineering. J Cell Mol Med 13:1428–1436
Bonnema GT, Cardinal KO, McNally JB, Williams SK, Barton JK (2007) Assessment of blood vessel mimics with optical coherence tomography. J Biomed Opt 12:24018
Chan-Park MB, Shen JY, Cao Y, Xiong Y, Liu Y, Rayatpisheh S, Kang GC, Greisler HP (2009) Biomimetic control of vascular smooth muscle cell morphology and phenotype for functional tissue-engineered small-diameter blood vessels. J Biomed Mater Res A 88:1104–1121
Chapman GB, Durante W, Hellums JD, Schafer AI (2000 2000-03-01) Physiological cyclic stretch causes cell cycle arrest in cultured vascular smooth muscle cells. Am J Physiol Heart Circ Physiol 278(3):H748–H754
Chen LC, Lloyd WR, Kuo S, Kim HM, Marcelo CL, Feinberg SE, Mycek MA (2014) The potential of label-free nonlinear optical molecular microscopy to non-invasively characterize the viability of engineered human tissue constructs. Biomaterials 35:6667–6676
Chen WW, Liao WJ, Wu YH, Li DF, Zhou JH, Yang JQ, Lin ZY (2015) Application of optical coherence tomography in tissue engineered blood vessel culture based on Luo-ye pump. Chin J Thorac Cardiovasc Surg 31(11):687–690
Couet F, Meghezi S, Mantovani D (2012) Fetal development, mechanobiology and optimal control processes can improve vascular tissue regeneration in bioreactors: an integrative review. Med Eng Phys 34:269–278
Gu K, Chang Y, Gao B, Wan F, Loisance D, Zeng Y (2014) Development of ventricular assist devices in China: present status, opportunities and challenges. Eur J Cardiothorac Surg 46:179–185
Gui L, Zhao L, Spencer RW, Burghouwt A, Taylor MS, Shalaby SW, Niklason LE (2011) Development of novel biodegradable polymer scaffolds for vascular tissue engineering. Tissue Eng Part A 17:1191–1200
Gurjarpadhye AA, Whited BM, Sampson A, Niu G, Sharma KS, Vogt WC, Wang G, Xu Y, Soker S, Rylander MN, Rylander CG (2013) Imaging and characterization of bioengineered blood vessels within a bioreactor using free-space and catheter-based OCT. Lasers Surg Med 45:391–400
Haga JH, Li YS, Chien S (2007) Molecular basis of the effects of mechanical stretch on vascular smooth muscle cells. J Biomech 40:947–960
Huang AH, Niklason LE (2011) Engineering biological-based vascular grafts using a pulsatile bioreactor. J Vis Exp 52: 2646
Huang AH, Niklason LE (2014) Engineering of arteries in vitro. Cell Mol Life Sci 71:2103–2118
Junqueira LC, Cossermelli W, Brentani R (1978) Differential staining of collagens type I, II and III by Sirius red and polarization microscopy. Arch Histol Jpn 41:267–274
Lehoux S, Tedgui A (2003) Cellular mechanics and gene expression in blood vessels. J Biomech 36:631–643
Lutolf MP, Hubbell JA (2005) Synthetic biomaterials as instructive extracellular microenvironments for morphogenesis in tissue engineering. Nat Biotechnol 23:47–55
Martinho JA, Freitas AZ, Raele MP, Santin SP, Soares FA, Herson MR, Mathor MB (2015) Dependence of optical attenuation coefficient and mechanical tension of irradiated human cartilage measured by optical coherence tomography. Cell Tissue Bank 16:47–53
Mills I, Cohen CR, Kamal K, Li G, Shin T, Du W, Sumpio BE (1997) Strain activation of bovine aortic smooth muscle cell proliferation and alignment: study of strain dependency and the role of protein kinase a and C signaling pathways. J Cell Physiol 170:228-234
Naito Y, Williams-Fritze M, Duncan DR, Church SN, Hibino N, Madri JA, Humphrey JD, Shinoka T, Breuer CK (2012) Characterization of the natural history of extracellular matrix production in tissue-engineered vascular grafts during neovessel formation. Cell Tissue Organ 195:60–72
Naito Y, Lee YU, Yi T, Church SN, Solomon D, Humphrey JD, Shin'Oka T, Breuer CK (2014) Beyond burst pressure: initial evaluation of the natural history of the biaxial mechanical properties of tissue-engineered vascular grafts in the venous circulation using a murine model. Tissue Eng Part A 20:346–355
Niklason LE, Yeh AT, Calle EA, Bai Y, Valentin A, Humphrey JD (2010) Enabling tools for engineering collagenous tissues integrating bioreactors, intravital imaging, and biomechanical modeling. Proc Natl Acad Sci U S A 107:3335–3339
Novosel EC, Kleinhans C, Kluger PJ (2011) Vascularization is the key challenge in tissue engineering. Adv Drug Deliv Rev 63:300–311
Poirier-Quinot M, Frasca G, Wilhelm C, Luciani N, Ginefri JC, Darrasse L, Letourneur D, Le Visage C, Gazeau F (2010) High-resolution 1.5-Tesla magnetic resonance imaging for tissue-engineered constructs: a noninvasive tool to assess three-dimensional scaffold architecture and cell seeding. Tissue Eng Part C 16:185–200
Prati F, Regar E, Mintz GS, Arbustini E, Di Mario C, Jang IK, Akasaka T, Costa M, Guagliumi G, Grube E, Ozaki Y, Pinto F, Serruys PW (2010) Expert review document on methodology, terminology, and clinical applications of optical coherence tomography: physical principles, methodology of image acquisition, and clinical application for assessment of coronary arteries and atherosclerosis. Eur Heart J 31:401–415
Rice WL, Firdous S, Gupta S, Hunter M, Foo CW, Wang Y, Kim HJ, Kaplan DL, Georgakoudi I (2008) Non-invasive characterization of structure and morphology of silk fibroin biomaterials using non-linear microscopy. Biomaterials 29:2015–2024
Smart N, Dube KN, Riley PR (2009) Coronary vessel development and insight towards neovascular therapy. Int J Exp Pathol 90:262–283
Smith LE, Smallwood R, Macneil S (2010) A comparison of imaging methodologies for 3D tissue engineering. Microsc Res Tech 73:1123–1133
Solan A, Dahl SL, Niklason LE (2009) Effects of mechanical stretch on collagen and cross-linking in engineered blood vessels. Cell Transplant 18:915–921
Stegemann JP, Hong H, Nerem RM (2005) Mechanical, biochemical, and extracellular matrix effects on vascular smooth muscle cell phenotype. J Appl Physiol (1985) 98:2321–2327
Vielreicher M, Schurmann S, Detsch R, Schmidt MA, Buttgereit A, Boccaccini A, Friedrich O (2013) Taking a deep look: modern microscopy technologies to optimize the design and functionality of biocompatible scaffolds for tissue engineering in regenerative medicine. J R Soc Interface 10:20130263
Yang Y, Dubois A, Qin XP, Li J, El HA, Wang RK (2006) Investigation of optical coherence tomography as an imaging modality in tissue engineering. Phys Med Biol 51:1649–1659
Zheng K, Rupnick MA, Liu B, Brezinski ME (2009) Three dimensional OCT in the engineering of tissue constructs: a potentially powerful tool for assessing optimal scaffold structure. Open Tissue Eng Regen Med J 2:8–13
Acknowledgement
This research was supported by the Science and Technology Planning Project of the Guangdong Province of China (2013B010404034,2016B070701007).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, W., Yang, J., Liao, W. et al. In vitro remodeling and structural characterization of degradable polymer scaffold-based tissue-engineered vascular grafts using optical coherence tomography. Cell Tissue Res 370, 417–426 (2017). https://doi.org/10.1007/s00441-017-2683-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-017-2683-z