Abstract
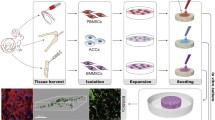
Uncultured bone marrow mononuclear cells (BMMC) were recently used to successfully repair damaged cartilage. However, the effect of BMMCs on the proliferation and differentiation of chondrocytes that are critical to cartilage repair is unclear. Here, we investigate the influence of BMMCs on chondrocyte dedifferentiation in pellet culture. We isolated and mixed BMMCs and chondrocytes in a 1:1 (BMMC/C) ratio and cultured in pellets (1.6 × 106 cells per pellet) for 2, 4, or 8 weeks. Chondrocyte differentiation was evaluated using macrography, histological examination, immunohistochemistry and gene expression analysis. While a transparent and smooth surface was observed in both BMMC/C and chondrocyte cultures over time, the former was smaller in size after 2 and 4 weeks of culture. Interestingly, after 8 weeks, BMMC/C cultures became significantly larger than chondrocyte cultures (P = 0.003). The distribution of a cartilage-specific extracellular matrix (ECM), that includes components like glycosaminoglycan (GAG) and type II collagen, was gradually reduced in chondrocyte cultures. On the other hand, while we found no obvious differences in the ECM in BMMC/C cultures between 2 and 4 weeks in vitro, after 8 weeks the concentration of ECM components decreased significantly. Further, we detected an upregulation of cartilage-specific genes in BMMC/C cultures, when compared with chondrocytes. Altogether, we demonstrate that co-culture with BMMCs delays the dedifferentiation of chondrocytes in pellet cultures in vitro. This suggests that uncultured BMMC, which can be quickly and safely obtained, could serve as a potential alternative cell source for engineering of cartilage tissue.







Similar content being viewed by others
References
Ahmed N, Gan L, Nagy A, Zheng J, Wang C, Kandel RA (2009) Cartilage tissue formation using redifferentiated passaged chondrocytes in vitro. Tissue Eng Part A 15:665–673
Balakumaran A, Robey PG, Fedarko N, Landgren O (2010) Bone marrow microenvironment in myelomagenesis: its potential role in early diagnosis. Expert Rev Mol Diagn 10:465–480
Beane OS, Darling EM (2012) Isolation, characterization, and differentiation of stem cells for cartilage regeneration. Ann Biomed Eng 40:2079–2097
Bekkers JE, Creemers LB, Tsuchida AI, van Rijen MH, Custers RJ, Dhert WJ, Saris DB (2013) One-stage focal cartilage defect treatment with bone marrow mononuclear cells and chondrocytes leads to better macroscopic cartilage regeneration compared to microfracture in goats. Osteoarthritis Cartilage 21:950–956
Benthien JP, Behrens P (2011) The treatment of chondral and osteochondral defects of the knee with autologous matrix-induced chondrogenesis (AMIC): method description and recent developments. Knee Surg Sports Traumatol Arthrosc 19:1316–1319
Benya PD, Padilla SR, Nimni ME (1978) Independent regulation of collagen types by chondrocytes during the loss of differentiated function in culture. Cell 15:1313–1321
Beris AE, Lykissas MG, Kostas-Agnantis I, Manoudis GN (2012) Treatment of full-thickness chondral defects of the knee with autologous chondrocyte implantation: a functional evaluation with long-term follow-up. Am J Sports Med 40:562–567
Brittberg M (2008) Autologous chondrocyte implantation–technique and long-term follow-up. Injury 39(Suppl 1):S40–S49
Carr AJ, Robertsson O, Graves S, Price AJ, Arden NK, Judge A, Beard DJ (2012) Knee replacement. Lancet 379:1331–1340
Chamberlain G, Fox J, Ashton B, Middleton J (2007) Concise review: mesenchymal stem cells: their phenotype, differentiation capacity, immunological features, and potential for homing. Stem Cells 25:2739–2749
Chang F, Ishii T, Yanai T, Mishima H, Akaogi H, Ogawa T, Ochiai N (2008) Repair of large full-thickness articular cartilage defects by transplantation of autologous uncultured bone-marrow-derived mononuclear cells. J Orthop Res 26:18–26
Danišovič L, Varga I, Polák S (2012) Growth factors and chondrogenic differentiation of mesenchymal stem cells. Tissue Cell 44:69–73
Dessau W, Vertel BM, von der Mark H, von der Mark K (1981) Extracellular matrix formation by chondrocytes in monolayer culture. J Cell Biol 90:78–83
Diaz-Romero J, Gaillard JP, Grogan SP, Nesic D, Trub T, Mainil-Varlet P (2005) Immunophenotypic analysis of human articular chondrocytes: changes in surface markers associated with cell expansion in monolayer culture. J Cell Physiol 202:731–742
Gan L, Kandel RA (2007) In vitro cartilage tissue formation by co-culture of primary and passaged chondrocytes. Tissue Eng 13:831–842
Hangody L, Füles P (2003) Autologous osteochondral mosaicplasty for the treatment of full-thickness defects of weight-bearing joints: ten years of experimental and clinical experience. J Bone Joint Surg Am 85-A(Suppl 2):25–32
Inui A, Iwakura T, Reddi AH (2012) Human stem cells and articular cartilage regeneration. Cells 1:994–1009
Jakob M, Démarteau O, Schäfer D, Hintermann B, Dick W, Heberer M, Martin I (2001) Specific growth factors during the expansion and redifferentiation of adult human articular chondrocytes enhance chondrogenesis and cartilaginous tissue formation in vitro. J Cell Biochem 81:368–377
Koga H, Engebretsen L, Brinchmann JE, Muneta T, Sekiya I (2009) Mesenchymal stem cell-based therapy for cartilage repair: a review. Knee Surg Sports Traumatol Arthrosc 17:1289–1297
Lin Z, Fitzgerald JB, Xu J, Willers C, Wood D, Grodzinsky AJ, Zheng MH (2008) Gene expression profiles of human chondrocytes during passaged monolayer cultivation. J Orthop Res 26:1230–1237
Matsumoto T, Okabe T, Ikawa T, Iida T, Yasuda H, Nakamura H, Wakitani S (2010) Articular cartilage repair with autologous bone marrow mesenchymal cells. J Cell Physiol 225:291–295
McNickle AG, L’Heureux DR, Yanke AB, Cole BJ (2009) Outcomes of autologous chondrocyte implantation in a diverse patient population. Am J Sports Med 37:1344–1350
Micheli LJ, Browne JE, Erggelet C, Fu F, Mandelbaum B, Moseley JB, Zurakowski D (2001) Autologous chondrocyte implantation of the knee: multicenter experience and minimum 3-year follow-up. Clin J Sport Med 11:223–228
Minas T (1998) Chondrocyte implantation in the repair of chondral lesions of the knee: economics and quality of life. Am J Orthop 27:739–744
Mithoefer K, Williams RJ 3rd, Warren RF, Potter HG, Spock CR, Jones EC, Wickiewicz TL, Marx RG (2005) The microfracture technique for the treatment of articular cartilage lesions in the knee. A prospective cohort study. J Bone Joint Surg Am 87:1911–1920
Nuernberger S, Cyran N, Albrecht C, Redl H, Vecsei V, Marlovits S (2011) The influence of scaffold architecture on chondrocyte distribution and behavior in matrix-associated chondrocyte transplantation grafts. Biomaterials 32:1032–1040
Peterson L, Minas T, Brittberg M, Nilsson A, Sjögren-Jansson E, Lindahl A (2000) Two- to 9-year outcome after autologous chondrocyte transplantation of the knee. Clin Orthop Relat Res 374:212–234
Peterson L, Vasiliadis HS, Brittberg M, Lindahl A (2010) Autologous chondrocyte implantation: a long-term follow-up. Am J Sports Med 38:1117–1124
Schindler OS (2011) Current concepts of articular cartilage repair. Acta Orthop Belg 77:709–726
Schulze-Tanzil G, de Souza P, Villegas Castrejon H, John T, Merker HJ, Scheid A, Shakibaei M (2002) Redifferentiation of dedifferentiated human chondrocytes in high-density cultures. Cell Tissue Res 308:371–379
Sohn DH, Lottman LM, Lum LY, Kim SG, Pedowitz RA, Coutts RD, Sah RL (2002) Effect of gravity on localization of chondrocytes implanted in cartilage defects. Clin Orthop Relat Res 394:254–262
Steadman JR, Rodkey WG, Briggs KK (2003) Microfracture chondroplasty: indications, techniques, and outcomes. Sports Med Arthrosc 11:236–244
von der Mark K, Gauss V, von der Mark H, Müller P (1977) Relationship between cell shape and type of collagen synthesised as chondrocytes lose their cartilage phenotype in culture. Nature 267:531–532
Wang W, Li B, Yang J, Xin L, Li Y, Yin H, Qi Y, Jiang Y, Ouyang H, Gao C (2010) The restoration of full-thickness cartilage defects with BMSCs and TGF-beta 1 loaded PLGA/fibrin gel constructs. Biomaterials 31:8964–8973
Wei B, Jin C, Xu Y, Du X, Yan C, Tang C, Ansari M, Wang L (2014) Chondrogenic differentiation of marrow clots after microfracture with BMSC-derived ECM scaffold in vitro. Tissue Eng Part A 20:2646–2655
Wise JK, Alford AI, Goldstein SA, Stegemann JP (2014) Comparison of uncultured marrow mononuclear cells and culture-expanded mesenchymal stem cells in 3D collagen-chitosan microbeads for orthopedic tissue engineering. Tissue Eng Part A 20:210–224
Wu L, Leijten JC, Georgi N, Post JN, van Blitterswijk CA, Karperien M (2011) Trophic effects of mesenchymal stem cells increase chondrocyte proliferation and matrix formation. Tissue Eng Part A 17:1425–1436
Wu L, Prins HJ, Helder MN, van Blitterswijk CA, Karperien M (2012) Trophic effects of mesenchymal stem cells in chondrocyte co-cultures are independent of culture conditions and cell sources. Tissue Eng Part A 18:1542–1551
Zhang Y, Wang F, Chen J, Ning Z, Yang L (2012) Bone marrow-derived mesenchymal stem cells versus bone marrow nucleated cells in the treatment of chondral defects. Int Orthop 36:1079–1086
Zhang Q, Lu H, Kawazoe N, Chen G (2014) Pore size effect of collagen scaffolds on cartilage regeneration. Acta Biomater 10:2005–2013
Acknowledgments
This work was supported by the National Natural Science Foundation of China (No. 81171745), the Science and Technology Planning Project of Xuzhou City, China (No. KC14SH010) and the Orthopedic Clinical Medical Center of Nanjing City, China.
Conflict of interest
All authors declare no conflict of interest regarding the design and outcomes of this study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Xiao Ouyang and Bo Wei contributed equally to this work.
Rights and permissions
About this article
Cite this article
Ouyang, X., Wei, B., Mao, F. et al. Uncultured bone marrow mononuclear cells delay the dedifferentiation of unexpanded chondrocytes in pellet culture. Cell Tissue Res 361, 811–821 (2015). https://doi.org/10.1007/s00441-015-2156-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-015-2156-1