Abstract
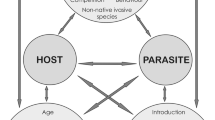
We performed a systematic review of the literature published since 1900 about leishmaniasis a neglected vector-borne disease, focused on environmental and social risk factors for visceral (VL) and cutaneous leishmaniasis (CL) to better understand their impact on the incidence of disease. The search terms were “leishmaniasis” AND “risk factors” using Google Scholar, PudMed, and Scielo. We reviewed 177 articles, 95 studies for VL, 75 for CL, and 7 on both forms. We identified 14 categories of risk factors which were divided into three groups: socioeconomic (7), environmental (5), and climate (2) variables. Socioeconomic factors were also associated with disease incidence in vulnerable human populations of arid and tropical developing regions. Environmental and climate factors showed significant associations with the incidence of VL and CL in all the studies that considered them. Proximity to natural vegetation remnants increased disease risk in both the New and Old World while the climate conditions favorable for disease transmission differed among regions. We propose a common conceptual framework for both clinical forms that highlights networks of interaction among risk factors. In both clinical forms, the interplay of these factors played a major role in disease incidence. Although there are similarities in environmental and socioeconomic conditions that mediate the transmission cycle of tropical, arid, and Mediterranean regions, the behavior of vector and reservoirs in each region is different. Special attention should be given to the possibility of vector adaptation to urban environments in developing countries where populations with low socioeconomic status are particularly vulnerable to the disease.





Similar content being viewed by others
References
Abaker AS, Mohammed AA, Elawad AE (2017) Socioeconomic and behavioral risk factors for infection of visceral leishmaniasis Gedaref State - Sudan. Glob J Med Public Health 6:1–7
Abdulla QB, Shabila NP, Al-Hadithi TS (2018) An outbreak of cutaneous leishmaniasis in erbil governorate of Iraqi Kurdistan region in 2015. J Infect Dev Ctries 12:600–607. https://doi.org/10.3855/JIDC.10306
Abdullah AYM, Dewan A, Shogib MRI et al (2017) Environmental factors associated with the distribution of visceral leishmaniasis in endemic areas of Bangladesh: modeling the ecological niche. Trop Med Health 45:13. https://doi.org/10.1186/s41182-017-0054-9
Adegboye OA, Adegboye M (2017) Spatially correlated time series and ecological niche analysis of cutaneous leishmaniasis in Afghanistan. Int J Environ Res Public Health 14:1–14. https://doi.org/10.3390/ijerph14030309
Adegboye MA, Olumoh J, Saffary T et al (2019) Effects of time-lagged meteorological variables on attributable risk of leishmaniasis in central region of Afghanistan. Sci Total Environ 685:533–541. https://doi.org/10.1016/j.scitotenv.2019.05.401
Adhikari SR, Supakankunti S, Khan MM (2010a) Kala azar in Nepal: Estimating the effects of socioeconomic factors on disease incidence. Kathmandu Univ Med J 8(1):73–79
Adhikari SR, Supakankunti S, Khan MM (2010b) Incidence of kala-azar in Nepal: estimating the effects of individual and household characteristics. Trans R Soc Trop Med Hyg 104:720–725. https://doi.org/10.1016/j.trstmh.2010.08.013
Akhoundi M, Kuhls K, Cannet A et al (2016) A historical overview of the classification, evolution, and dispersion of Leishmania parasites and sandflies. PLoS Negl Trop Dis 10:1–40. https://doi.org/10.1371/journal.pntd.0004349
Alcais A, Abel L, David C et al (1997) Risk factors for onset of cutaneous and mucocutaneous leishmaniasis in Bolivia. Am J Trop Med Hyg 57:79–84
Alebie G, Worku A, Yohannes S et al (2019) Epidemiology of visceral leishmaniasis in Shebelle Zone of Somali Region, eastern Ethiopia. Parasit Vectors 12:1–10. https://doi.org/10.1186/s13071-019-3452-5
Alemayehu B, Alemayehu M (2017) Leishmaniasis: a review on parasite, vector and reservoir host. Health Sci J 11:1–6. https://doi.org/10.21767/1791-809X.1000519
Ali-Akbarpour M, Mohammadbeigi A, Tabatabaee SHR, Hatam G (2012) Spatial analysis of eco-environmental risk factors of cutaneous leishmaniasis in Southern Iran. J Cutan Aesthet Surg 5:30. https://doi.org/10.4103/0974-2077.94338
Almeida AS, Werneck GL (2014) Prediction of high-risk areas for visceral leishmaniasis using socioeconomic indicators and remote sensing data. Int J Health Geogr 13:7. https://doi.org/10.1186/1476-072X-13-13
Alvar J, Yactayo S, Bern C (2006) Leishmaniasis and poverty. Trends Parasitol 22:552–557. https://doi.org/10.1016/j.pt.2006.09.004
Alvar J, Vélez ID, Bern C et al (2012) Leishmaniasis worldwide and global estimates of its incidence. PLoS One 7:1–12. https://doi.org/10.1371/journal.pone.0035671
Alves EB, Costa CHN, de Carvalho FAA et al (2016) Risk profiles for Leishmania infantum infection in Brazil. Am J Trop Med Hyg 94:1276–1281. https://doi.org/10.4269/ajtmh.15-0513
Al-Warid HS, Al-Saqur IM, Kadhem AJ et al (2019) Spatial and demographic aspects of kala-azar (Visceral leishmaniasis) in iraq during 2011-2013. Trop Biomed 36:22–34
Amro A, Al-Dwibe H, Gashout A et al (2017) Spatiotemporal and molecular epidemiology of cutaneous leishmaniasis in Libya. PLoS Negl Trop Dis 11:e0005873. https://doi.org/10.1371/journal.pntd.0005873
Andrade-Narvaez FJ, Canto Lara SB, Van Wynsberghe NR et al (2003) Seasonal transmission of Leishmania (Leishmania) mexicana in the State of Campeche, Yucatan Peninsula, Mexico. Mem Inst Oswaldo Cruz 98:995–998. https://doi.org/10.1590/S0074-02762003000800002
Antonialli SAC, Torres TG, Filho ACP, Tolezano JE (2007) Spatial analysis of American visceral leishmaniasis in Mato Grosso do Sul State, Central Brazil. J Inf Secur 54:509–514. https://doi.org/10.1016/j.jinf.2006.08.004
Aparicio C, Bitencourt MD (2004) Modelagem espacial de zonas de risco da leishmaniose tegumentar americana. Rev Saude Publica 38:511–516. https://doi.org/10.1590/S0034-89102004000400005
Argaw D, Mulugeta A, Herrero M et al (2013) Risk factors for visceral Leishmaniasis among residents and migrants in Kafta-Humera, Ethiopia. PLoS Negl Trop Dis 7:9. https://doi.org/10.1371/journal.pntd.0002543
Armijos RX, Weigel MM, Izurieta R et al (1997) The epidemiology of cutaneous leishmaniasis in subtropical Ecuador. Tropical Med Int Health 2:140–152. https://doi.org/10.1046/j.1365-3156.1997.d01-236.x
Arroub H, Alaoui A, Lemrani M, Habbari K (2012) Cutaneous Leishmaniasis in Foum Jamâa (Azilal, Morocco): micro-environmental and socio-economical risk factors. J Agric Soc Sci 8:1813–2235
Artun O, Kavur H (2017) Geographical information systems in determination of spatial factors in cutaneous leishmaniasis cases distribution, in Adana, Turkey. Sci Pap E-l Reclam Earth Obs Surv Environ Eng 6:141–146
Artun O, Kavur H (2018) Prediction of cutaneous Leishmaniasis epidemiology in mersin using ecological niche modeling. Turkiye parazitolojii Derg 42:191–195. https://doi.org/10.5152/tpd.2018.5924
Ashford RW (1996) Leishmaniasis reservoirs and their significance in control. Clin Dermatol 14:523–532. https://doi.org/10.1016/0738-081X(96)00041-7
Ashford RW, Bray MA, Hutchinson MP, Bray RS (1973) The Epidemiology of cutaneous leishmaniasis in Ethiopia. Trans R Soc Trop Med Hyg 67:568–601
Assefa A (2018) Leishmaniasis in Ethiopia: a systematic review and meta-analysis of prevalence in animals and humans. Heliyon 4:e00723. https://doi.org/10.1016/j.heliyon.2018.e00723
Azene W, Sissay M, Kebede A, Gashaw F (2017) Visceral leishmaniasis and associated risk factors in Libo Kemkem, Bura Egzi Abhier Ab Kebele, Northwestern Ethiopia. EC Microbiol 7:162–172
Azimi F, Shirian S, Jangjoo S et al (2017) Impact of climate variability on the occurrence of cutaneous leishmaniasis in Khuzestan Province, southwestern Iran. Geospat Health 12:15–22. https://doi.org/10.4081/gh.2017.478
Badaró R (1988) Progress of research in visceral leishmaniasis in the endemic area of Jacobina—Bahia 1934-1989. Rev Soc Bras Med Trop 21:159–164
Bamorovat M, Sharifi I, Aflatoonian MR et al (2018) Risk factors for anthroponotic cutaneous leishmaniasis in unresponsive and responsive patients in a major focus, southeast of Iran. PLoS One 13:e0192236. https://doi.org/10.1371/journal.pone.0192236
Barnett P, Singh SP, Bern C et al (2005) Virgin soil: the spread of visceral leishmaniasis into Uttar Pradesh, India. Am J Trop Med Hyg 73:720–725
Bashaye S, Nombela N, Argaw D et al (2009) Risk factors for visceral leishmaniasis in a new epidemic site in Amhara region, Ethiopia. Am J Trop Med Hyg 81:34–39
Bates PA, Depaquit J, Galati EAB et al (2015) Recent advances in phlebotomine sand fly research related to leishmaniasis control. Parasit Vectors 8:1–8. https://doi.org/10.1186/s13071-015-0712-x
Bavia ME, Carneiro DDMT, Gurgel Hda C et al (2005) Remote sensing and geographic information systems and risk of American visceral leishmaniasis in Bahia, Brazil. Parasitologia 47:165–169
Beier JC, El Sawaf BM, Merdan AI et al (1986) Sand flies (Diptera : Psychodidae) associated with visceral leishmaniasis in El Agamy, Alexandria Governorate, Egypt. I. Population ecology. J Med Entomol 23:600–608
Bellali H, Chemak F, Nouiri I et al (2017) Zoonotic cutaneous leishmaniasis prevalence among farmers in Central Tunisia, 2014. J Agromed 22:244–250. https://doi.org/10.1080/1059924X.2017.1318725
Belo VS, Werneck GL, Barbosa DS et al (2013) Factors associated with visceral leishmaniasis in the Americas: a systematic review and meta-analysis. PLoS Negl Trop Dis 7:12. https://doi.org/10.1371/journal.pntd.0002182
Ben-Ahmed K, Aoun K, Jeddi F et al (2009) Visceral leishmaniasis in Tunisia: spatial distribution and association with climatic factors. Am J Trop Med Hyg 81:40–45
Bern C, Joshi AB, Jha SN et al (2000) Factors associated with visceral leishmaniasis in Nepal: bed-net use is strongly protective. Am J Trop Med Hyg 63:184–188
Bern C, Hightower AW, Chowdhury R et al (2005) Risk factors for kala-azar in Bangladesh. Emerg Infect Dis 11:655–662. https://doi.org/10.3201/eid1105.040718
Bern C, Courtenay O, Alvar J (2010) Of cattle, sand flies and men: a systematic review of risk factor analyses for South Asian visceral leishmaniasis and implications for elimination. PLoS Negl Trop Dis 4:1–10. https://doi.org/10.1371/journal.pntd.0000599
Bhowmick AR, Khanum H (2017) Prevalence of visceral leishmaniasis, risk factors and associated disorders: knowledge of inhabitants and professionals in Fulbaria, Mymensingh. Bangladesh J Zool 45:73–83. https://doi.org/10.3329/bjz.v45i1.34197
Bhunia GS, Kesari S, Jeyaram A et al (2010a) Influence of topography on the endemicity of Kala-azar: a study based on remote sensing and geographical information system. Geospat Health 4:155–165. https://doi.org/10.4081/gh.2010.197
Bhunia GS, Kumar V, Kumar AJ et al (2010b) The use of remote sensing in the identification of the eco-environmental factors associated with the risk of human visceral leishmaniasis (kala-azar) on the Gangetic plain, in north-eastern India. Ann Trop Med Parasitol 104:35–53. https://doi.org/10.1179/136485910X12607012373678
Bhunia GS, Kesari S, Chatterjee N et al (2011) Incidence of visceral leishmaniasis in the Vaishali district of Bihar, India: spatial patterns and role of inland water bodies. Geospat Health 5:205–215. https://doi.org/10.4081/gh.2011.173
Bhunia GS, Chatterjee N, Kumar V et al (2012) Delimitation of kala-azar risk areas in the district of Vaishali in Bihar (India) using a geo-environmental approach. Mem Inst Oswaldo Cruz 107:609–620. https://doi.org/10.1590/S0074-02762012000500007
Boelaert M, Meheus F, Sanchez A et al (2009) The poorest of the poor: a poverty appraisal of households affected by visceral leishmaniasis in Bihar, India. Tropical Med Int Health 14:639–644. https://doi.org/10.1111/j.1365-3156.2009.02279.x
Borges BKA, Silva JA, JPA H et al (2009) Presença de animais associada ao risco de transmissão da leishmaniose visceral em humanos em Belo Horizonte, Minas Gerais. Arq Bras Med Vet e Zootec 61:1035–1043. https://doi.org/10.1590/S0102-09352009000500004
Bsrat A, Berhe N, Balkew M et al (2015) Epidemiological study of cutaneous leishmaniasis in Saesie Tsaeda-emba district, eastern Tigray, Northern Ethiopia. Parasit Vectors 8:1–9. https://doi.org/10.1186/s13071-015-0758-9
Bsrat A, Berhe M, Gadissa E et al (2018) Serological investigation of visceral Leishmania infection in human and its associated risk factors in Welkait District, Western Tigray, Ethiopia. Parasite Epidemiol Control 3:13–20. https://doi.org/10.1016/j.parepi.2017.10.004
Bulstra CA, Le Rutte EA, Malaviya P et al (2018) Visceral leishmaniasis: spatiotemporal heterogeneity and drivers underlying the hotspots in Muzaffarpur, Bihar, India. PLoS Negl Trop Dis 12:1–21. https://doi.org/10.1371/journal.pntd.0006888
Campbell-Lendrum DH, Pinto MC, Brandão-Filho SP et al (1999) Experimental comparison of anthropophily between geographically dispersed populations of Lutzomyia whitmani (Diptera: Psychodidae). Med Vet Entomol 13:299–309. https://doi.org/10.1046/j.1365-2915.1999.00174.x
Cardenas R, Sandoval CM, Rodriguez-Morales AJ, Franco-Paredes C (2006) Impact of climate variability in the occurrence of leishmaniasis in Northeastern Colombia. Am J Trop Med Hyg 75:273–277
Cardim MFM, Rodas LAC, Dibo MR et al (2013) Introduction and expansion of human American visceral leishmaniasis in the state of Sao Paulo, Brazil, 1999-2011. Rev Saude Publica 47:1–9. https://doi.org/10.1590/S0034-8910.2013047004454
Cardim MFM, Guirado MM, Dibo MR, Neto FC (2016) Visceral leishmaniasis in the state of Sao Paulo, Brazil: spatial and space-time analysis. Rev Saude Publica 50:1–11. https://doi.org/10.1590/S1518-8787.2016050005965
Cardoso RM, de Araújo NNSL, Romero GAS et al (2015) Expanding the knowledge about Leishmania species in wild mammals and dogs in the Brazilian savannah. Parasit Vectors 8:1–8. https://doi.org/10.1186/s13071-015-0780-y
Carrada Figueroa Gdel C, Leal Ascencio VJ, Jiménez Sastré A, López Álvarez J (2014) Transmission of cutaneous leishmaniasis associated with cacao (Theobroma cacao) plantations in Tabasco. Gac Med Mex 150:499–508
Cerbino Neto J, Werneck GL, Costa CHN (2009) Factors associated with the incidence of urban visceral leishmaniasis: an ecological study in Teresina, Piauí State, Brazil. Cad Saude Publica 25:1543–1551. https://doi.org/10.1590/S0102-311X2009000700012
Chalghaf B, Chlif S, Mayala B et al (2016) Ecological niche modeling for the prediction of the geographic distribution of cutaneous leishmaniasis in Tunisia. Am J Trop Med Hyg 94:844–851. https://doi.org/10.4269/ajtmh.15-0345
Chaniotis BN (1983) Improved trapping of phlebotomine sand flies (Diptera: Psychodidae) in light traps supplemented with dry ice in a neotropical rain forest. J Med Entomol 20:222–223
Chaves LF, Pascual M (2006) Climate cycles and forecasts of cutaneous leishmaniasis, a nonstationary vector-borne disease. PLoS Med 3:1320–1328. https://doi.org/10.1371/journal.pmed.0030295
Chavy A, Ferreira Dales Nava A, Luz SLB et al (2019) Ecological niche modelling for predicting the risk of cutaneous leishmaniasis in the Neotropical moist forest biome. PLoS Negl Trop Dis 13:e0007629. https://doi.org/10.1371/journal.pntd.0007629
Costa CH, Werneck GL, Rodrigues L Jr et al (2005) Household structure and urban services: neglected targets in the control of visceral leishmaniasis. 99:229–236. https://doi.org/10.1179/136485905X28018
da Paixão Sevá A, Mao L, Galvis-Ovallos F et al (2017) Risk analysis and prediction of visceral leishmaniasis dispersion in São Paulo State, Brazil. PLoS Negl Trop Dis 11:1–17. https://doi.org/10.1371/journal.pntd.0005353
da Silva LMR, Cunha PR (2007) A urbanização da leishmaniose tegumentar americana no município de Campinas – São Paulo (SP) e região: Magnitude Campinas – Sao Paulo (SP) and region: problems and challenges. An Bras Dermatol 82:515–519. https://doi.org/10.1590/S0365-05962007000600003
Dantas-Torres F, Brandão-Filho SP (2006) Visceral leishmaniasis in Brazil: revisiting paradigms of epidemiology and control. Rev Inst Med Trop Sao Paulo 48:151–156. https://doi.org/10.1590/S0036-46652006000300007
Dantas-Torres F, Solano-Gallego L, Baneth G et al (2012) Canine leishmaniosis in the Old and New Worlds: unveiled similarities and differences. Trends Parasitol 28:531–538. https://doi.org/10.1016/j.pt.2012.08.007
Davies CR, Llanos-Cuentas EA, Campos P et al (1997) Cutaneous leishmaniasis in the peruvian Andes: risk factors identified from a village cohort study. Am J Trop Med Hyg 56:85–95
Dawit G, Girma Z, Simenew K (2013) A review on biology, epidemiology and public health significance of leishmaniasis. J Bacteriol Parasitol 4:7. https://doi.org/10.4172/2155-9597.1000166
de Almeida AS, Medronho Rde A, Werneck GL (2011) Identification of risk areas for visceral leishmaniasis in Teresina, Piaui State, Brazil. Am J Trop Med Hyg 84:681–687. https://doi.org/10.4269/ajtmh.2011.10-0325
de Almeida AS, Werneck GL, da Costa Resendes AP (2014) Classificação orientada a objeto de imagens de sensoriamento remoto em estudos epidemiológicos sobre leishmaniose visceral em área urbana. Cad Saude Publica 30:1639–1653. https://doi.org/10.1590/0102-311X00059414
de Araújo PF, de Alencar Ximenes RA (2009) Sociodemographic and environmental risk factors for American cutaneous leishmaniasis (ACL) in the State of Alagoas, Brazil. Am J Trop Med Hyg 81:195–201
de Araújo VEM, Pinheiro LC, de Mattos Almeida MC et al (2013) Relative risk of visceral leishmaniasis in Brazil: a spatial analysis in urban area. PLoS Negl Trop Dis 7:9. https://doi.org/10.1371/journal.pntd.0002540
De Araujo AR, Portela NC, Feitosa APS et al (2016) Risk factors associated with american cutaneous leishmaniasis in an endemic area of Brazil. Rev Inst Med Trop Sao Paulo 58:2–7. https://doi.org/10.1590/S1678-9946201658086
de Freitas Rocha AT, de Espindola GM, Soares MRA et al (2018) Visceral leishmaniasis and vulnerability conditions in an endemic urban area of Northeastern Brazil. Trans R Soc Trop Med Hyg 112:317–325. https://doi.org/10.1093/trstmh/try058
de Oliveira EF, Silva EA, Fernandes CE et al (2012) Biotic factors and occurrence of Lutzomyia longipalpis in endemic area of visceral leishmaniasis, Mato Grosso do Sul, Brazil. Mem Inst Oswaldo Cruz 107:396–401. https://doi.org/10.1590/S0074-02762012000300015
de Oliveira IP, da Fonseca AH, Silveira AK et al (2016) Spatial analysis of areas likely to harbor American cutaneous leishmaniasis in Seropédica, Rio de Janeiro State, Brazil. Semin Ciências Agrárias 37:193–202. https://doi.org/10.5433/1679-0359.2016v37n1p193
de Santana Martins M (2015) The use of geographic information systems and cological niche modeling to map transmission risk for visceral leishmaniasis in Bahia. Louisiana State University, Brazil
de Souza RAF, Andreoli RV, Kayano MT, Carvalho AL (2015) American cutaneous leishmaniasis cases in the metropolitan region of manaus, Brazil: association with climate variables over time. Geospat Health 10:40–47. https://doi.org/10.4081/gh.2015.314
Desjeux P (2001) The increase in risk factors for leishmaniasis worldwide. Trans R Soc Trop Med Hyg 95:239–243. https://doi.org/10.1016/S0035-9203(01)90223-8
Desjeux P (2004) Leishmaniasis: Current situation and new perspectives. Comp Immunol Microbiol Infect Dis 27:305–318. https://doi.org/10.1016/j.cimid.2004.03.004
Dias ES, França-Silva JC, Costa J et al (2007) Flebotomíneos (Diptera : Psychodidae) de um foco de leishmaniose tegumentar no Estado de Minas Gerais Sandflies (Diptera : Psychodidae) in an outbreak of cutaneous leishmaniasis in the State of Minas Gerais. Rev Soc Bras Med Trop 40:49–52
dos Reis LL, da Silva Balieiro AA, Fonseca FR, Gonçalves MJF (2019) Leishmaniose visceral e sua relação com fatores climáticos e ambientais no Estado do Tocantins, Brasil, 2007 a 2014. Cad Saude Publica 35:e00047018. https://doi.org/10.1590/0102-311x00047018
dos Santos Afonso MM, de Miranda Chaves SA, de Avelar Figueiredo Mafra Magalhães M, et al (2017) Ecoepidemiology of American visceral Leishmaniasis in Tocantins State, Brazil: factors associated with the occurrence and spreading of the vector lutzomyia (Lutzomyia) longipalpis (Lutz & Neiva, 1912) (Diptera: Psychodidae: Phlebotominae). In: The Epidemiology and Ecology of Leishmaniasis. InTech, p 91
Dujardin J-C (2006) Risk factors in the spread of leishmaniases: towards integrated monitoring? Trends Parasitol 22:4–6. https://doi.org/10.1016/j.pt.2005.11.004
Dulacha D, Mwatha S, Lomurukai P et al (2019) Epidemiological characteristics and factors associated with Visceral Leishmaniasis in Marsabit County, Northern Kenya. J Interv Epidemiol Public Heal 2:1–25
Eid D, Guzman-Rivero M, Rojas E et al (2018) Correction to: risk factors for cutaneous leishmaniasis in the rainforest of Bolivia: a cross-sectional study. Trop Med Health:46
El Alem MMM, Hakkour M, Hmamouch A et al (2018) Risk factors and prediction analysis of cutaneous leishmaniasis due to Leishmania tropica in Southwestern Morocco. Infect Genet Evol 61:84–91. https://doi.org/10.1016/j.meegid.2018.03.017
Elnaiem DEA, Mukhawi AM, Hassan MM et al (2003a) Factors affecting variations in exposure to infections by Leishmania donovani in eastern Sudan. East Mediterr Health J 9:827–836
Elnaiem DEA, Schorscher J, Bendall A et al (2003b) Risk mapping of visceral leishmaniasis: The role of local variation in rainfall and altitude on the presence and incidence of kala-azar in eastern Sudan. Am J Trop Med Hyg 68:10–17
Espejo JT, Le Pont F, Mouchet J et al (1989) Epidemiologie de la leishmaniose tegumentaire en Bolivie. 1. Description des zones d’etude et frequence de la maladie. Ann Soc Belg Med Trop (1920) 69:297–306
Fakhar M, Karamian M, Ghatee MA et al (2017) Distribution pattern of anthroponotic cutaneous leishmaniasis caused by Leishmania tropica in Western Afghanistan during 2013-2014. Acta Trop 176:22–28. https://doi.org/10.1016/j.actatropica.2017.07.028
Faris R, Massoud A, El Said S et al (1988) The epidemiology of human visceral leishmaniasis in El Agamy (Alexandria Governorate), Egypt: serosurvey and case/control study. Ann Trop Med Parasitol 82:445–452. https://doi.org/10.1080/00034983.1988.11812274
Faucher B, Gaudart J, Faraut F et al (2012) Heterogeneity of environments associated with transmission of visceral leishmaniasis in South-eastern France and implication for control strategies. PLoS Negl Trop Dis 6:1–9. https://doi.org/10.1371/journal.pntd.0001765
Feliciangeli MD, Delgado O, Suarez B, Bravo A (2006) Leishmania and sand flies: Proximity to woodland as a risk factor for infection in a rural focus of visceral leishmaniasis in west central Venezuela. Tropical Med Int Health 11:1785–1791. https://doi.org/10.1111/j.1365-3156.2006.01747.x
Ferro C, López M, Fuya P et al (2015) Spatial distribution of sand fly vectors and eco-epidemiology of cutaneous leishmaniasis transmission in Colombia. PLoS One 10:1–16. https://doi.org/10.1371/journal.pone.0139391
Forattini OP, Rabello EX, Serra OP et al (1976) Observações sobre a transmissão da leishmaniose tegumentar no estado de São Paulo. Brasil Rev Saude Publica:31–43
Galgamuwa LS, Dharmaratne SD, Iddawela D (2018) Leishmaniasis in Sri Lanka: spatial distribution and seasonal variations from 2009 to 2016. Parasit Vectors 11:60. https://doi.org/10.1186/s13071-018-2647-5
Gao X, Cao Z (2019) Meteorological conditions, elevation and land cover as predictors for the distribution analysis of visceral leishmaniasis in Sinkiang province, Mainland China. Sci Total Environ 646:1111–1116. https://doi.org/10.1016/j.scitotenv.2018.07.391
Gebremichael Tedla D, Bariagabr FH, Abreha HH (2018) Incidence and trends of Leishmaniasis and its risk factors in humera, Western Tigray. J Parasitol Res. https://doi.org/10.1155/2018/8463097
Ghatee MA, Haghdoost AA, Kooreshnia F et al (2018) Role of environmental, climatic risk factors and livestock animals on the occurrence of cutaneous leishmaniasis in newly emerging focus in Iran. J Infect Public Health 11:425–433. https://doi.org/10.1016/j.jiph.2017.12.004
Giannakopoulos A, Tsokana CN, Pervanidou D et al (2016) Environmental parameters as risk factors for human and canine Leishmania infection in Thessaly, Central Greece. Parasitology 143:1179–1186. https://doi.org/10.1017/S0031182016000378
Gijón-Robles P, Abattouy N, Merino-Espinosa G et al (2018) Risk factors for the expansion of cutaneous leishmaniasis by Leishmania tropica: possible implications for control programmes. Transbound Emerg Dis 65:1615–1626. https://doi.org/10.1111/tbed.12914
Gil JF, Nasser JR, Cajal SP et al (2010) Urban transmission of american cutaneous leishmaniasis in Argentina: spatial analysis study. Am J Trop Med Hyg 82:433–440. https://doi.org/10.4269/ajtmh.2010.09-0113
Godana AA, Mwalili SM, Orwa GO (2019) Dynamic spatiotemporal modeling of the infected rate of visceral leishmaniasis in human in an endemic area of Amhara regional state, Ethiopia. PLoS One 14:e0212934. https://doi.org/10.1371/journal.pone.0212934
Golpayegani AA, Moslem AR, Akhavan AA et al (2018) Modeling of environmental factors affecting the prevalence of zoonotic and anthroponotic cutaneous, and zoonotic visceral leishmaniasis in foci of Iran: a remote sensing and GIS based study. J Arthropod Borne Dis 12:41–66
Gomez-Barroso D, Herrador Z, San Martin JV et al (2015) Spatial distribution and cluster analysis of a leishmaniasis outbreak in the South-western Madrid region, Spain, September 2009 to April 2013. Euro Surveill 20:1–10. https://doi.org/10.2807/1560-7917.ES2015.20.7.21037
Grimaldi GJ, Tesh RB (1993) Leishmaniases of the New World: current concepts and implications for future research. Clin Microbiol Rev 6:230–250. https://doi.org/10.1128/CMR.6.3.230.Updated
Guerra JADO, Guerra MDGVB, Vasconcelos ZS et al (2019) Socioenvironmental aspects of the Purus Region - Brazilian Amazon: why relate them to the occurrence of American Tegumentary Leishmaniasis? PLoS One 14:e0211785. https://doi.org/10.1371/journal.pone.0211785
Gutierrez JD, Martínez-Vega R, Ramoni-Perazzi J et al (2017) Environmental and socio-economic determinants associated with the occurrence of cutaneous leishmaniasis in the northeast of Colombia. Trans R Soc Trop Med Hyg 111:564–571. https://doi.org/10.1093/trstmh/try011
Hasker E, Singh SP, Malaviya P et al (2012) Visceral leishmaniasis in rural Bihar, India. Emerg Infect Dis 18:1662–1664. https://doi.org/10.3201/eid1810.111083
Haydon DT, Cleaveland S, Taylor LH, Laurenson MK (2002) Identifying reservoirs of infection: a conceptual and practical challenge. Emerg Infect Dis 8:1468–1473. https://doi.org/10.3201/eid0812.010317
Hernández AM, Gutierrez JD, Xiao Y et al (2019) Spatial epidemiology of cutaneous leishmaniasis in Colombia: socioeconomic and demographic factors associated with a growing epidemic. Trans R Soc Trop Med Hyg 113:560–568. https://doi.org/10.1093/trstmh/trz043
Holakouie-Naieni K, Mostafavi E, Boloorani AD et al (2017) Spatial modeling of cutaneous leishmaniasis in Iran from 1983 to 2013. Acta Trop 166:67–73. https://doi.org/10.1016/j.actatropica.2016.11.004
Iddawela D, Vithana SMP, Atapattu D, Wijekoon L (2018) Clinical and epidemiological characteristics of cutaneous leishmaniasis in Sri Lanka. BMC Infect Dis 18:108. https://doi.org/10.1186/s12879-018-2999-7
Iliopoulou P, Tsatsaris A, Katsios I et al (2018) Risk mapping of visceral leishmaniasis: a spatial regression model for Attica Region, Greece. Trop Med Infect Dis 3:83. https://doi.org/10.3390/tropicalmed3030083
Jones TC, Johnson WD, Barretto AC et al (1987) Epidemiology of American cutaneous leishmaniasis due to Leishmania braziliensis brasiliensis. J Infect Dis 156:73–83
Karagiannis-Voules DA, Scholte RGC, Guimarães LH et al (2013) Bayesian geostatistical modeling of leishmaniasis incidence in Brazil. PLoS Negl Trop Dis 7:13. https://doi.org/10.1371/journal.pntd.0002213
Kariyawasam KKGDUL, Edirisuriya CS, Senerath U et al (2015) Characterisation of cutaneous leishmaniasis in Matara district, southern Sri Lanka: evidence for case clustering. Pathog Glob Health 109:1–8. https://doi.org/10.1179/2047773215Y.0000000032
Kassem HA, Siri J, Kamal HA, Wilson ML (2012) Environmental factors underlying spatial patterns of sand flies (Diptera: Psychodidae) associated with leishmaniasis in southern Sinai, Egypt. Acta Trop 123:8–15. https://doi.org/10.1016/j.actatropica.2012.02.067
Khanal B, Picado A, Bhattarai NR et al (2010) Spatial analysis of Leishmania donovani exposure in humans and domestic animals in a recent kala azar focus in Nepal. Parasitology 137:1597–1603. https://doi.org/10.1017/S0031182010000521
Kirstein OD, Skrip L, Abassi I et al (2018) A fine scale eco-epidemiological study on endemic visceral leishmaniasis in north ethiopian villages. Acta Trop 183:64–77. https://doi.org/10.1016/j.actatropica.2018.04.005
Kolaczinski JH, Reithinger R, Worku DT et al (2008) Risk factors of visceral leishmaniasis in East Africa: a case-control study in Pokot territory of Kenya and Uganda. Int J Epidemiol 37:344–352. https://doi.org/10.1093/ije/dym275
Kumar N, Singh TB, Meena LP (2017) Socio-economic and behavioural risk factors of visceral leishmaniasis in the East Champaran district of Bihar. Int J Community Med Public Health 4:1577. https://doi.org/10.18203/2394-6040.ijcmph20171767
Lainson R, Rangel BF (2005) Lutzomyia longipalpis and the eco-epidemiology of American visceral leishmaniasis, with particular reference to Brazil—a review. Mem Inst Oswaldo Cruz 100:811–827
Lemma W, Tekie H, Yared S et al (2015) Sero-prevalence of Leishmania donovani infection in labour migrants and entomological risk factors in extra-domestic habitats of Kafta-Humera lowlands - kala-azar endemic areas in the northwest Ethiopia. BMC Infect Dis 15:1–8. https://doi.org/10.1186/s12879-015-0830-2
Li Y, Zheng C (2019) Associations between meteorological factors and visceral leishmaniasis outbreaks in Jiashi County, Xinjiang Uygur Autonomous Region, China, 2005–2015. Int J Environ Res Public Health 16:1775. https://doi.org/10.3390/ijerph16101775
Lima ID, Lima ALM, Mendes-Aguiar CO et al (2018) Changing demographics of visceral leishmaniasis in northeast Brazil: lessons for the future. PLoS Negl Trop Dis 12:e0006164. https://doi.org/10.1371/journal.pntd.0006164
Loiseau R, Nabet C, Simon S et al (2019) American cutaneous leishmaniasis in French Guiana: an epidemiological update and study of environmental risk factors. Int J Dermatol ijd.14625. https://doi.org/10.1111/ijd.14625
López K, Tartaglino LC, Steinhorst II et al (2016) Factores de riesgo, representaciones y prácticas asociadas con la leishmaniasis visceral humana en un foco urbanoemergente en Posadas, Argentina. Biomédica 36:51–63
Lopez J, Freire C, Moncayo T et al (2018) Prevalence and factors associated with cutaneous leishmaniasis in Tena-Napo, Ecuador 2012-2013. Síndrome Cardiometabólico y enfermedades crónica Degener 8:5–9
Lotukoi JA (2017) Exposure Factors Associated with Visceral Leishmaniasis (kala-azar) in Loima Sub-County of Turkana County, Kenya. Am J Lab Med 2:144. https://doi.org/10.11648/j.ajlm.20170206.16
Machado-Coelho GLL, Assunção R, Mayrink W, Caiaffa WT (1999) American cutaneous leishmaniasis in Southeast Brazil: space-time clustering. Int J Epidemiol 28:982–989. https://doi.org/10.1093/ije/28.5.982
Madalosso G, Fortaleza CM, Ribeiro AF et al (2012) American visceral leishmaniasis: factors associated with lethality in the state of São Paulo, Brazil. J Trop Med 2012:1–8. https://doi.org/10.1155/2012/281572
Maia CS, Pimentel DS, Santana MA et al (2013) The perception of the risk factors associated with American visceral leishmaniasis in Petrolina, Pernambuco, Brazil. Rev Med Vet (Bogota) 7:19–25
Maia Z, Viana V, Muniz E et al (2016) Risk factors associated with human visceral leishmaniasis in an urban area of Bahia, Brazil. Vector-Borne Zoonotic Dis 16:368–376. https://doi.org/10.1089/vbz.2015.1880
Mandal P, Wagle RR, Thakur AK et al (2019) “Risk Factors for Visceral Leishmaniasis in Selected High Endemic Areas of Morang District, Nepal”: a case control Study. bioRxiv:530741. https://doi.org/10.1101/530741
Melchior LAK, Brilhante AF, Chiaravalloti-Neto F (2017) Spatial and temporal distribution of American cutaneous leishmaniasis in Acre state, Brazil. Infect Dis Poverty 6:99. https://doi.org/10.1186/s40249-017-0311-5
Melo HA, Rossoni DF, Teodoro U (2018) Effect of vegetation on cutaneous leishmaniasis in Paraná. Brazil Mem Inst Oswaldo Cruz 113. https://doi.org/10.1590/0074-02760170505
Menezes JA, Luz TCB, de Sousa FF et al (2016) Fatores de risco peridomiciliares e conhecimento sobre leishmaniose visceral da população de Formiga, Minas Gerais. Rev Bras Epidemiol 19:362–374. https://doi.org/10.1590/1980-5497201600020013
Miranda C, Marques CCA, Massa JL (1998) Sensoriamento remoto orbital como recurso para análise da ocorrência da leishmaniose tegumentar americana em localidade urbana da região Sudeste do Brasil. Rev Saude Publica 32:455–463
Mokhtari M, Miri M, Nikoonahad A et al (2016) Cutaneous leishmaniasis prevalence and morbidity based on environmental factors in Ilam, Iran: Spatial analysis and land use regression models. Acta Trop 163:90–97. https://doi.org/10.1016/j.actatropica.2016.08.002
Monteiro WM, Neitzke-Abreu HC, Ferreira MEM et al (2009) Population mobility and production of American tegumentary leishmaniasis in the State of Paraná , southern Brazil. Rev Soc Bras Med Trop 42:509–514
Montoya J, Jaramillo C, Palma G et al (1990) Report of an epidemic outbreak of tegumentary leishmaniasis in a coffee-growing area of Colombia. Mem Inst Oswaldo Cruz 85:119–121
Moo Llanes DA (2016) Nicho ecológico actual y futuro de la leishmaniasis en la región Neotropical. Rev Biol Trop 64:1237–1245
Moradiasl E, Rassi Y, Hanafi-Bojd AA et al (2018) The relationship between climatic factors and the prevalence of visceral leishmaniasis in North West of Iran. Int. J Pediatr 6:7169–7178. https://doi.org/10.22038/ijp.2018.26837.2314
Moradi-Asl E, Hanafi-Bojd AA, Rassi Y et al (2017) Situational analysis of visceral leishmaniasis in the most important endemic area of the disease in Iran. J Arthropod Borne Dis 11:482–496
Moreno EC, Melo MN, Genaro O et al (2005) Risk factors for Leishmania chagasi infection in an urban area of Minas Gerais State. Rev Soc Bras Med Trop 38:456–463. https://doi.org/10.1590/S0037-86822005000600002
Moškovskij ŠD, Duhanina NN (1971) Epidemiology of the leishmaniases: general considerations. Bull World Health Organ 44:529–534
Mott KE, Desjeux P, Moncayo A et al (1990) Parasitic diseases and urban development. Bull World Health Organ 68:691–698
Myers SS, Gaffikin L, Golden CD et al (2013) Human health impacts of ecosystem alteration. Proc Natl Acad Sci U S A 110:18753–18760. https://doi.org/10.1073/pnas.1218656110
Nackers F, Mueller YK, Salih N et al (2015) Determinants of Visceral Leishmaniasis: a case-control study in Gedaref State, Sudan. PLoS Negl Trop Dis 9:1–16. https://doi.org/10.1371/journal.pntd.0004187
Nasser JT, Donalisio MR, Vasconcelos CH (2009) Distribuição espacial dos casos de leishmaniose tegumentar americana no município de Campinas , Estado de São Paulo , no período de 1992 a 2003 Spatial distribution of American tegumentary leishmaniasis cases in Campinas , State of São Paulo , between 199. Rev Soc Bras Med Trop 42:309–314
Navin TR, Sierra M, Custodio R et al (1985) Epidemiologic study of visceral leishmaniasis in Honduras, 1975-1983. Am J Trop Med Hyg 34:1069–1075
Nazari M, Nazari S, Hanafi-Bojd AA et al (2017) Situation analysis of cutaneous leishmaniasis in an endemic area, south of Iran. Asian Pac J Trop Med 10:92–97. https://doi.org/10.1016/j.apjtm.2016.12.001
Negera E, Gadisa E, Yamuah L et al (2008) Outbreak of cutaneous leishmaniasis in Silti woreda, Ethiopia: risk factor assessment and causative agent identification. Trans R Soc Trop Med Hyg 102:883–890. https://doi.org/10.1016/j.trstmh.2008.03.021
Nikonahad A, Khorshidi A, Ghaffari HR et al (2017) A time series analysis of environmental and metrological factors impact on cutaneous leishmaniasis incidence in an endemic area of Dehloran, Iran. Environ Sci Pollut Res 24:14117–14123. https://doi.org/10.1007/s11356-017-8962-0
Nilforoushzadeh MA, Hosseini SM, Heidari A et al (2014) Domestic and peridomestic risk factors associated with transmission of cutaneous leishmaniasis in three hypo endemic, endemic, and hyper endemic areas: a randomized epidemiological study. J Res Med Sci 19:928–932
Ocampo CB, Ferro MC, Cadena H et al (2012) Environmental factors associated with American cutaneous leishmaniasis in a new Andean focus in Colombia. Tropical Med Int Health 17:1309–1317. https://doi.org/10.1111/j.1365-3156.2012.03065.x
Oliveira CDL, Diez-Roux A, César CC, Proietti FA (2006) A case-control study of microenvironmental risk factors for urban visceral leishmaniasis in a large city in Brazil, 1999-2000. Pan Am J Public Health 20:369–376. https://doi.org/10.1590/S1020-49892006001100002
Oliveira AM, López RVM, Dibo MR et al (2018) Dispersion of Lutzomyia longipalpis and expansion of visceral leishmaniasis in São Paulo State, Brazil: identification of associated factors through survival analysis. Parasit Vectors 11:503. https://doi.org/10.1186/s13071-018-3084-1
Pace D (2014) Leishmaniasis. J Inf Secur 20:1–9. https://doi.org/10.1016/j.jinf.2014.07.016
Patz JA, Daszak P, Tabor GM et al (2004) Unhealthy landscapes: policy recommendations on land use change and infectious disease emergence. Environ Health Perspect 112:1092–1098. https://doi.org/10.1289/ehp.6877
Pérez-Flórez M, Ocampo CB, Valderrama-Ardila C, Alexander N (2016) Spatial modeling of cutaneous leishmaniasis in the Andean region of Colombia. Mem Inst Oswaldo Cruz 111:433–442. https://doi.org/10.1590/0074-02760160074
Perilla-González Y, Gómez-Suta D, Delgado-Osorio N et al (2014) Study of the scientific production on leishmaniasis in Latin America. Recent Pat Antiinfect Drug Discov 9:216–222
Perry D, Dixon K, Garlapati R et al (2013) Visceral leishmaniasis prevalence and associated risk factors in the Saran District of Bihar, India, from 2009 to July of 2011. Am J Trop Med Hyg 88:778–784. https://doi.org/10.4269/ajtmh.12-0442
Pigott DM, Bhatt S, Golding N et al (2014a) Global distribution maps of the leishmaniases. Elife:1–21. https://doi.org/10.7554/eLife.02851
Pigott DM, Golding N, Messina JP et al (2014b) Global database of leishmaniasis occurrence locations, 1960-2012. Sci Data 1:1–7. https://doi.org/10.1038/sdata.2014.36
Ponte CB, Souza NC, Cavalcante MN et al (2011) Risk factors for Leishmania chagasi infection in an endemic area in Raposa, State of Maranhão, Brazil. Rev Soc Bras Med Trop 44:712–721. https://doi.org/10.1590/S0037-86822011005000059
Prestes-Carneiro LE, Daniel LAF, Almeida LC et al (2019) Spatiotemporal analysis and environmental risk factors of visceral leishmaniasis in an urban setting in São Paulo State, Brazil. Parasit Vectors 12:251. https://doi.org/10.1186/s13071-019-3496-6
Prudhomme J, Rahola N, Toty C et al (2015) Ecology and spatiotemporal dynamics of sandflies in the Mediterranean Languedoc region (Roquedur area, Gard, France). Parasit Vectors 8:1–14. https://doi.org/10.1186/s13071-015-1250-2
Quintana MG, Fernández MS, Salomón OD (2012) Distribution and abundance of phlebotominae, vectors of leishmaniasis, in Argentina: Spatial and temporal analysis at different scales. J Trop Med 2012:1–16. https://doi.org/10.1155/2012/652803
Rajabi M, Mansourian A, Pilsejo P, Bazmani A (2014) Environmental modelling of visceral leishmaniasis by susceptibility-mapping using neural networks: a case study in north-western Iran. Geospat Health 9:179–191. https://doi.org/10.4081/gh.2014.15
Rajabi M, Pilesjö P, Bazmani A, Mansourian A (2016a) Identification of visceral leishmaniasis-susceptible areas using spatial modelling in Southern Caucasus. Zoonoses Public Health:1–18. https://doi.org/10.1111/zph.12325
Rajabi M, Pilesjö P, Shirzadi MR et al (2016b) A spatially explicit agent-based modeling approach for the spread of cutaneous leishmaniasis disease in central Iran, Isfahan. Environ Model Softw 82:330–346. https://doi.org/10.1016/j.envsoft.2016.04.006
Ramezankhani R, Hosseini A, Sajjadi N et al (2017a) Environmental risk factors for the incidence of cutaneous leishmaniasis in an endemic area of. A GIS-based approach. Spat Spatiotemporal Epidemiol, Iran. https://doi.org/10.1016/j.sste.2017.03.003
Ramezankhani R, Sajjadi N, Esmaeilzadeh RN et al (2017b) Spatial analysis of cutaneous leishmaniasis in an endemic area of Iran based on environmental factors. Geospat Health 12:282–293. https://doi.org/10.4081/gh.2017.578
Ramezankhani R, Sajjadi N, Nezakati esmaeilzadeh R et al (2018) Climate and environmental factors affecting the incidence of cutaneous leishmaniasis in Isfahan, Iran. Environ Sci Pollut Res 25:11516–11526. https://doi.org/10.1007/s11356-018-1340-8
Ranasinghe S, Wickremasinghe R, Munasinghe A et al (2013) Cross-sectional study to assess risk factors for leishmaniasis in an endemic region in Sri Lanka. Am J Trop Med Hyg 89:742–749. https://doi.org/10.4269/ajtmh.12-0640
Ranjan A, Sur D, Singh VP et al (2005) Risk factors for Indian kala-azar. Am J Trop Med Hyg 73:74–78
Ready PD (2013) Biology of phlebotomine sand flies as vectors of disease agents. Annu Rev Entomol 58:227–250. https://doi.org/10.1146/annurev-ento-120811-153557
Reithinger R, Mohsen M, Leslie T (2010) Risk factors for anthroponotic cutaneous leishmaniasis at the household level in Kabul, Afghanistan. PLoS Negl Trop Dis 4:1–8. https://doi.org/10.1371/journal.pntd.0000639
Reyes A, Arrivillaga J (2009) Fauna Mammalia asociada a los focos de leishmaniasis neotropical: Situación en Venezuela. Boletín Malariol y Salud Ambient 49:35–52
Rijal S, Uranw S, Chappuis F et al (2010) Epidemiology of Leishmania donovani infection in high-transmission foci in Nepal. Tropical Med Int Health 15:21–28. https://doi.org/10.1111/j.1365-3156.2010.02518.x
Rodrigues MGA, Sousa JDB, Dias ÁLB et al (2019) The role of deforestation on American cutaneous leishmaniasis incidence: spatial-temporal distribution, environmental and socioeconomic factors associated in the Brazilian Amazon. Tropical Med Int Health 24:348–355. https://doi.org/10.1111/tmi.13196
Rodríguez-Morales AJ, Pascual-González Y, Benítez JA et al (2010) Asociación entre la incidencia de leishmaniosis cutánea y el índice de desarrollo humano y sus componentes en cuatro estados endémicos de Venezuela. Rev Peru Med Exp Salud Publica 27:22–30
Roque ALR, Jansen AM (2014) Wild and synanthropic reservoirs of Leishmania species in the Americas. Int J Parasitol Parasites Wildl 3:251–262. https://doi.org/10.1016/j.ijppaw.2014.08.004
Ruh E, Bostanci A, Kunter V et al (2017) Leishmaniasis in northern Cyprus: human cases and their association with risk factors. J Vector Borne Dis 54:358–365. https://doi.org/10.4103/0972-9062.225842
Rutledge LC, Gupta RK (2002) Moth flies and sand flies (Psychodidae ). In: Medical and Veterinary Entomology. Elsevier Science, pp 147–161
Ryan JR, Mbui J, Rashid JR et al (2006) Spatial clustering and epidemiological aspects of visceral leishmaniasis in two endemic villages, Baringo District, Kenya. Am J Trop Med Hyg 74:308–317
Salomón OD, Wilson ML, Munstermann LE, Travi BL (2004) Spatial and temporal patterns of phlebotomine sand flies (Diptera: Psychodidae) in a cutaneous leishmaniasis focus in Northern Argentina. J Med Entomol 41:33–39. https://doi.org/10.1603/0022-2585-41.1.33
Salomón OD, Feliciangeli MD, Quintana MG et al (2015) Lutzomyia longipalpis urbanisation and control. Mem Inst Oswaldo Cruz 110:831–846. https://doi.org/10.1590/0074-02760150207
Schenkel K, Rijal S, Koirala S et al (2006) Visceral leishmaniasis in southeastern Nepal: a cross-sectional survey on Leishmania donovani infection and its risk factors. Tropical Med Int Health 11:1792–1799. https://doi.org/10.1111/j.1365-3156.2006.01735.x
Seid A, Gadisa E, Tsegaw T et al (2014) Risk map for cutaneous leishmaniasis in Ethiopia based on environmental factors as revealed by geographical information systems and statistics. Geospat Health 8:377–387. https://doi.org/10.4081/gh.2014.27
Shah H (2005) Prevalence of visceral leishmaniasis associated with the behaviors of the people in rural areas. J Nepal Med Assoc 44:116–120
Sharma U, Singh S (2008) Insect vectors of Leishmania: distribution , physiology and their control. J Vector Borne Dis 45:255–272
Shaw J (2007) The leishmaniases—survival and expansion in a changing world. A mini-review. Mem Inst Oswaldo Cruz 102:541–546. https://doi.org/10.1590/S0074-02762007000500001
Shiravand B, Tafti AAD, Hanafi-Bojd AA et al (2018) Modeling spatial risk of zoonotic cutaneous leishmaniasis in Central Iran. Acta Trop 185:327–335. https://doi.org/10.1016/j.actatropica.2018.06.015
Singh NS, Singh PD (2019) A review on major risk factors and current status of visceral leishmaniasis in north India. Am J Entomol 3:6. https://doi.org/10.11648/j.aje.20190301.12
Singh SP, Hasker E, Picado A et al (2010) Risk factors for visceral leishmaniasis in India: further evidence on the role of domestic animals. Tropical Med Int Health 15:29–35. https://doi.org/10.1111/j.1365-3156.2010.02515.x
Sosa-Estani S, Segura EL, Gomez A et al (2001) Leishmaniose cutânea no Norte da Argentina: fatores de risco identificados num estudo caso-coorte em três municípios de Salta. Rev Soc Bras Med Trop 34:511–517
Southgate BA (1964) Studies in the epidemiology of East African leishmaniasis. 2. The human distribution and its determinants. Trans R Soc Trop Med Hyg 58:377–390
Souza VAF, Cortez LR, Dias RA et al (2012) Space-time cluster analysis of American visceral leishmaniasis in Bauru, São Paulo State, Brazil. Cad Saude Publica 28:1949–1964. https://doi.org/10.1590/S0102-311X2012001000013
Steffens I (2010) Vector-borne diseases Special edition. Eur J Infect:1–124
Talmoudi K, Bellali H, Ben-Alaya N et al (2017) Modeling zoonotic cutaneous leishmaniasis incidence in central Tunisia from 2009-2015: Forecasting models using climate variables as predictors. PLoS Negl Trop Dis 11:1–18. https://doi.org/10.1371/journal.pntd.0005844
Temponi AOD, de Brito MG, Ferraz ML et al (2018) Ocorrência de casos de leishmaniose tegumentar americana: uma análise multivariada dos circuitos espaciais de produção, Minas Gerais, Brasil, 2007 a 2011. Cad Saude Publica 34:1–15. https://doi.org/10.1590/0102-311x00165716
Thompson RA, Wellington de Oliveira Lima J, Maguire JH et al (2002) Climatic and demographic determinants of American visceral leishmaniasis in northeastern Brazil using remote sensing technology for environmental categorization of rain and region influences on leishmamiasis. Am J Trop 67:648–655
Toledo CRS, Almeida AS, Chaves SAM et al (2017) Vulnerability to the transmission of human visceral leishmaniasis in a Brazilian urban area. Rev Saude Publica 51:49. https://doi.org/10.1590/S1518-8787.2017051006532
Tsegaw T, Gadisa E, Seid A et al (2013) Identification of environmental parameters and risk mapping of visceral leishmaniasis in Ethiopia by using geographical information systems and a statistical approach. Geospat Health 7:299–308. https://doi.org/10.4081/gh.2013.88
Ullah K, Khan NH, Sepúlveda N et al (2016) Assessing incidence patterns and risk factors for cutaneous leishmaniasis in Peshawar Region, Khyber Pakhtunkhwa, Pakistan. J Parasitol 102:501–506. https://doi.org/10.1645/15-919
Uranw S, Hasker E, Roy L et al (2013) An outbreak investigation of visceral leishmaniasis among residents of Dharan town, Eastern Nepal, evidence for urban transmission of Leishmania donovani. BMC Infect Dis 13:9. https://doi.org/10.1186/1471-2334-13-21
Valderrama-Ardila C, Alexander N, Ferro C et al (2010) Environmental risk factors for the incidence of American cutaneous leishmaniasis in a sub-andean zone of Colombia (Chaparral, Tolima). Am J Trop Med Hyg 82:243–250. https://doi.org/10.4269/ajtmh.2010.09-0218
Viana GM, Nascimento Mdo D, Rabelo ÉM et al (2011) Relationship between rainfall and temperature: observations on the cases of visceral leishmaniasis in São Luis Island, State of Maranhão, Brazil. Rev Soc Bras Med Trop 44:722–724. https://doi.org/10.1590/S0037-86822011000600013
Votýpka J, Kasap OE, Volf P et al (2012) Risk factors for cutaneous leishmaniasis in Cukurova region, Turkey. Trans R Soc Trop Med Hyg 106:186–190. https://doi.org/10.1016/j.trstmh.2011.12.004
Wade TG, Riitters KH, Wickham JD, Jones KB (2003) Distribution and causes of global forest fragmentation. Ecol Soc 7
Weerakoon HS, Ranawaka RR, Warnasekara J, Bandara P (2018) Analysis of gap in the correct diagnosis of leishmaniasis at primary care level, socio demographic and environmental risk factors of leishmaniasis transmission in Anuradhapura. In: Anuradhapura Med J
Weigle K, Santrich C, Martinez F et al (1993) Epidemiology of cutaneous leishmaniasis in Colombia: environmental and behavioral risk factors for infection, clinical manifestations, and pathogenicity. J Infect Dis 168:709–714
Werneck GL, Costa CHN, Walker AM et al (2002) The urban spread of visceral leishmaniasis: clues from spatial analysis. Epidemiology 13:364–367. https://doi.org/10.1097/00001648-200205000-00020
Werneck GL, Costa CHN, Walker AM et al (2007) Multilevel modelling of the incidence of visceral leishmaniasis in Teresina, Brazil. Epidemiol Infect 135:195–201. https://doi.org/10.1017/S0950268806006881
Wood CL, Lafferty KD, DeLeo G et al (2014) Does biodiversity protect humans against infectious disease? Ecology 95:817–832. https://doi.org/10.1890/13-1041.1
World Health Organization (2010) Control of the leishmaniases. World Health Organ Tech Rep Ser:1–202. https://doi.org/10.1038/nrmicro1766
World Health Organization (2017) Global leishmaniasis update, 2006–2015: a turning point in leishmaniasis surveillance. World Heal Organ Geneva 92:557–572. https://doi.org/10.1186/1750-9378-2-15.Voir
World Health Organization (2018) Global Health Observatory (GHO) data| Leishmaniasis. In: WHO. https://www.who.int/gho/neglected_diseases/leishmaniasis/en/. Accessed 2 Mar 2019
Yadon ZE, Rodrigues LC, Davies CR, Quigley MA (2003) Indoor and peridomestic transmission of American cutaneous leishmaniasis in northwestern Argentina: a retrospective case-control study. Am J Trop Med Hyg 68:519–526. https://doi.org/10.4269/ajtmh.2003.68.519
Yared S, Deribe K, Gebreselassie A et al (2014) Risk factors of visceral leishmaniasis: a case control study in north-western Ethiopia. Parasit Vectors 7:1–11. https://doi.org/10.1186/s13071-014-0470-1
Zheng C, Fu J, Li Z et al (2018) Spatiotemporal variation and hot spot detection of visceral leishmaniasis disease in Kashi Prefecture, China. Int J Environ Res Public Health 15:2784. https://doi.org/10.3390/ijerph15122784
Zorrilla V, Agüero M, Cáceres A et al (2005) Factores de riesgo que determinan la transmisión de la leishmaniasis en el valle Llaucano , Chota-Cajamarca. Info 42:33–42
Acknowledgments
The authors would like to thank Dr. José Dilermando Andrade Filho (Fiocruz) for their valuable comments about leishmaniasis that contributed to the development of this review. We also thank Prof. Ligia Vizeu Barrozo (FLCH-USP), Dr. Paula Ribeiro Prist, Dr. Anaiá da Paixão Sevá and Dr. Elizabeth Nichols for insights that greatly improved the manuscript.
Funding
Nerida H. Valero PhD study was funded by the Brazilian Federal Agency for Support and Evaluation of Graduate Education – CAPES Process: PDSE - 88881.134367/2016-01.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Section Editor: Sarah Hendrickx
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 139 kb)
Rights and permissions
About this article
Cite this article
Valero, N.N.H., Uriarte, M. Environmental and socioeconomic risk factors associated with visceral and cutaneous leishmaniasis: a systematic review. Parasitol Res 119, 365–384 (2020). https://doi.org/10.1007/s00436-019-06575-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-019-06575-5