Abstract
Purpose
The objective of this investigation was to explore the diagnostic capability of Prostate Specific Antigen Mass Ratio (PSAMR) combined with Prostate Imaging Reporting and Data System (PI-RADS) scoring for clinically significant prostate cancer (CSPC), develop and validate a Nomogram prediction model for the probability of prostate cancer occurrence in patients who have not undergone prostate biopsy.
Methods
Initially, we retrospectively collected clinical and pathological data of patients who underwent trans-perineal prostate puncture at Yijishan Hospital of Wanan Medical College from July 2021 to January 2023. Through logistic univariate and multivariate regression analysis, independent risk factors for CSPC were determined. Receiver Operating Characteristic (ROC) curves were generated to compare the ability of different factors for diagnosis of CSPC. Then, we split the dataset into a training set and validation set, compared their heterogeneity, and developed a Nomogram prediction model based on the training set. Finally, we validated the Nomogram prediction model in terms of discrimination, calibration, and clinical usefulness.
Results
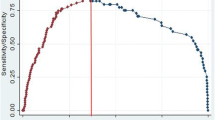
Logistic multivariate regression analysis illustrated that age [64–69 (OR = 2.736, P = 0.029); 69–75 (OR = 4.728, P = 0.001); > 75 (OR = 11.344, P < 0.001)], PSAMR [0.44–0.73 (OR = 4.144, P = 0.028); 0.73–1.64(OR = 13.022, P < 0.001); > 1.64(OR = 50.541, P < 0.001)], and PI-RADS score [4 points (OR = 7.780, P < 0.001); 5 points (OR = 24.533, P < 0.001)] were independent risk factors for CSPC. The Area Under the Curve (AUC) of the ROC curves of PSA, PSAMR, PI-RADS score, and PSAMR combined with PI-RADS score were respectively 0.797, 0.874, 0.889, and 0.928. The performance of PSAMR and PI-RADS score for diagnosis of CSPC was superior to PSA, but inferior to PSAMR combined with PI-RADS. Age, PSAMR, and PI-RADS were included in the Nomogram prediction model. The AUCs of the training set ROC curve and the validation set ROC curve were 0.943 (95% CI 0.917–0.970) and 0.878 (95% CI 0.816–0.940), respectively, in the discrimination validation. The calibration curve showed good consistency, and the decision analysis curve suggested the model had good clinical efficacy.
Conclusions
We found that PSAMR combined with PI-RADS scoring had a strong diagnostic capability for CSPC, and provided a Nomogram prediction model to predict the probability of prostate cancer occurrence combined with clinical data.





Similar content being viewed by others
Availability of data and materials
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
References
Ahmed HU, El-Shater Bosaily A, Brown LC, Gabe R, Kaplan R, Parmar MK et al (2017) Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet (Lond Engl) 389(10071):815–822. https://doi.org/10.1016/s0140-6736(16)32401-1
Baco E, Rud E, Vlatkovic L (2016) Reply to Yi Zhou, Weigang Yan, and Hanzhong Li’s letter to the editor re: Eduard Baco, Erik Rud, Lars Magne Eri a randomized controlled trial to assess and compare the outcomes of two-core prostate biopsy guided by fused magnetic resonance and transrectal ultrasound images and traditional 12-core systematic biopsy. Eur Urol 2016;69:149–156. Eur Urol 70(2):e55. https://doi.org/10.1016/j.eururo.2016.01.031
Balachandran VP, Gonen M, Smith JJ, DeMatteo RP (2015) Nomograms in oncology: more than meets the eye. Lancet Oncol 16(4):e173–e180. https://doi.org/10.1016/s1470-2045(14)71116-7
Bandini M, Fossati N, Briganti A (2019) Nomograms in urologic oncology, advantages and disadvantages. Curr Opin Urol 29(1):42–51. https://doi.org/10.1097/mou.0000000000000541
Bañez LL, Hamilton RJ, Partin AW, Vollmer RT, Sun L, Rodriguez C et al (2007) Obesity-related plasma hemodilution and PSA concentration among men with prostate cancer. JAMA 298(19):2275–2280. https://doi.org/10.1001/jama.298.19.2275
Choi HC, Park JH, Cho BL, Son KY, Kwon HT (2010) Prostate specific antigen mass ratio potential as a prostate cancer screening tool. J Urol 184(2):488–493. https://doi.org/10.1016/j.juro.2010.03.138
Christie DRH, Sharpley CF (2019) How accurately can prostate gland imaging measure the prostate gland volume? Results of a systematic review. Prostate Cancer 2019:6932572. https://doi.org/10.1155/2019/6932572
Epstein JI, Amin MB, Reuter VE, Humphrey PA (2017) Contemporary Gleason grading of prostatic carcinoma: an update with discussion on practical issues to implement the 2014 international society of urological pathology (ISUP) consensus conference on Gleason grading of prostatic carcinoma. Am J Surg Pathol 41(4):e1–e7. https://doi.org/10.1097/PAS.0000000000000820
Ferro M, de Cobelli O, Vartolomei MD, Lucarelli G, Crocetto F, Barone B et al (2021) Prostate cancer radiogenomics—from imaging to molecular characterization. Int J Mol Sci 22(18):9971. https://doi.org/10.3390/ijms22189971
Hong SKOJ, Byun SS, Hwang SI, Choo MS, Lee SE (2012) Value of prostate-specific antigen (PSA) mass ratio in the detection of prostate cancer in men with PSA levels of ≤10 ng/mL. BJU Int 110(2 Pt 2):E81–E85. https://doi.org/10.1111/j.1464-410X.2011.10764.x
Jiang Z, Yan L, Deng S, Gu J, Qin L, Mao F et al (2023) Development and interpretation of a clinicopathological-based model for the identification of microsatellite instability in colorectal cancer. Dis Markers 2023:5178750. https://doi.org/10.1155/2023/5178750
Kasivisvanathan V, Stabile A, Neves JB, Giganti F, Valerio M, Shanmugabavan Y et al (2019) Magnetic resonance imaging-targeted biopsy versus systematic biopsy in the detection of prostate cancer: a systematic review and meta-analysis. Eur Urol 76(3):284–303. https://doi.org/10.1016/j.eururo.2019.04.043
Korevaar TIM, Derakhshan A, Taylor PN, Meima M, Chen L, Bliddal S et al (2019) Association of thyroid function test abnormalities and thyroid autoimmunity with preterm birth: a systematic review and meta-analysis. JAMA 322(7):632–641. https://doi.org/10.1001/jama.2019.10931
Lee WK, Lee S, Hong SK, Lee SE, Choi WS, Byun SS (2014) Clinical utility of prostate-specific antigen mass ratio for prediction of prostate cancer detection on a repeated prostate biopsy. Int Braz J Urol Off J Braz Soc Urol 40(4):484–492. https://doi.org/10.1590/s1677-5538.Ibju.2014.04.06
Lin Z, Peng R, Li Z, Wang Y, Lu C, Shen Y et al (2015) 17-ABAG, a novel geldanamycin derivative, inhibits LNCaP-cell proliferation through heat shock protein 90 inhibition. Int J Mol Med 36(2):424–432. https://doi.org/10.3892/ijmm.2015.2239
Matuszczak M, Schalken JA, Salagierski M (2021) Prostate cancer liquid biopsy biomarkers’ clinical utility in diagnosis and prognosis. Cancers 13(13):3373. https://doi.org/10.3390/cancers13133373
Panebianco V, Barchetti F, Sciarra A, Ciardi A, Indino EL, Papalia R et al (2015) Multiparametric magnetic resonance imaging vs. standard care in men being evaluated for prostate cancer: a randomized study. Urol Oncol 33(1):17.e1-e7. https://doi.org/10.1016/j.urolonc.2014.09.013
Park H, Kim JY, Lee BM, Chang SK, Ko SY, Kim SJ et al (2011) A comparison of preplan MRI and preplan CT-based prostate volume with intraoperative ultrasound-based prostate volume in real-time permanent brachytherapy. Radiat Oncol J 29(3):199–205. https://doi.org/10.3857/roj.2011.29.3.199
Rodriguez JF, Eggener SE (2018) Prostate cancer and the evolving role of biomarkers in screening and diagnosis. Radiol Clin North Am 56(2):187–196. https://doi.org/10.1016/j.rcl.2017.10.002
Shen W, Song Z, Zhong X, Huang M, Shen D, Gao P et al (2022) Sangerbox: a comprehensive, interaction-friendly clinical bioinformatics analysis platform. iMeta 1(3):e36. https://doi.org/10.1002/imt2.36
Siddiqui MM, Rais-Bahrami S, Turkbey B, George AK, Rothwax J, Shakir N et al (2015) Comparison of MR/ultrasound fusion-guided biopsy with ultrasound-guided biopsy for the diagnosis of prostate cancer. JAMA 313(4):390–397. https://doi.org/10.1001/jama.2014.17942
Siegel RL, Miller KD, Jemal A (2020) Cancer statistics, 2020. CA Cancer J Clin 70(1):7–30. https://doi.org/10.3322/caac.21590
Tang Z, Liu WR, Zhou PY, Ding ZB, Jiang XF, Wang H et al (2019) Prognostic value and predication model of microvascular invasion in patients with intrahepatic cholangiocarcinoma. J Cancer 10(22):5575–5584. https://doi.org/10.7150/jca.32199
Turkbey B, Rosenkrantz AB, Haider MA, Padhani AR, Villeirs G, Macura KJ et al (2019) Prostate imaging reporting and data system version 2.1: 2019 update of prostate imaging reporting and data system version 2. Eur Urol 76(3):340–351. https://doi.org/10.1016/j.eururo.2019.02.033
Viana PCC, Horvat N, do Santos VRJ, Lima TC, Romão DDS, Cerri LMO et al (2019) Is possible to rule out clinically significant prostate cancer using PI-RADS v2 for the assessment of prostate MRI? Int Braz J Urol Off J Braz Soc Urol 45(4):724–731. https://doi.org/10.1590/s1677-5538.Ibju.2018.0382
Wang X, Lu J, Song Z, Zhou Y, Liu T, Zhang D (2022) From past to future: bibliometric analysis of global research productivity on nomogram (2000–2021). Front Public Health 10:997713. https://doi.org/10.3389/fpubh.2022.997713
Watanabe H (2015) Relapse of prostate cancer from the viewpoint of total gland volume kinetics theory. Asian J Androl 17(6):904–907. https://doi.org/10.4103/1008-682x.153543. (discussion 7)
Wei C, Pan P, Chen T, Zhang Y, Dai G, Tu J et al (2021) A nomogram based on PI-RADS v2.1 and clinical indicators for predicting clinically significant prostate cancer in the transition zone. Transl Androl Urol. 10(6):2435–2446. https://doi.org/10.21037/tau-21-49
Wilkinson S, Harmon SA, Terrigino NT, Karzai F, Pinto PA, Madan RA et al (2020) A case report of multiple primary prostate tumors with differential drug sensitivity. Nat Commun 11(1):837. https://doi.org/10.1038/s41467-020-14657-7
Xu B, Li G, Kong C, Chen M, Hu B, Jiang Q et al (2021) A multicenter retrospective study on evaluation of predicative factors for positive biopsy of prostate cancer in real-world setting. Curr Med Res Opin 37(9):1617–1625. https://doi.org/10.1080/03007995.2021.1949270
Yousaf T, Dervenoulas G, Politis M (2018) Advances in MRI methodology. Int Rev Neurobiol 141:31–76. https://doi.org/10.1016/bs.irn.2018.08.008
Funding
This work was supported by 2022 Provincial Key Clinical Specialty Construction Funds for Urology (KZSJZ010).
Author information
Authors and Affiliations
Contributions
DL and LZ conceived the study, performed the literature search and bioinformatics analysis, and prepared the figures; SH, XW, YX and YJ helped with data collection, analysis, and interpretation. DL, YG and QH wrote and revised the manuscript. The author(s) read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest in terms of the research, authorship, and/or publication of this article.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, D., Zhang, L., Xu, Y. et al. Exploration of the diagnostic capacity of PSAMR combined with PI-RADS scoring for clinically significant prostate cancer and establishment and validation of the Nomogram prediction model. J Cancer Res Clin Oncol 149, 11309–11317 (2023). https://doi.org/10.1007/s00432-023-05008-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-05008-2