Abstract
Purpose
As one of the most effective analgesics, opioids are essential for patients with cancer-related pain, even in the context of the opioid abuse crisis. The current meta-analysis aimed to identify whether concomitant exposure to opioids can affect the efficacy of ICIs and lead to a worse prognosis.
Methods
PubMed, Embase, and the Cochrane Library were searched based on the PRISMA checklist, through April 2022, for the following terms: ("opioids" OR "concomitant medication") AND ("Neoplasm" OR "Carcinoma" OR "Cancer" OR "Tumor") AND ("Immunotherapy" OR "Immune Checkpoint Inhibitor" OR "PD-L1 Inhibitor" OR "PD-1 Inhibitor" OR "CTLA-4 Inhibitor"). The outcomes considered were overall survival (OS) and progression-free survival (PFS) calculated using the random-effects or fixed-effects model.
Results
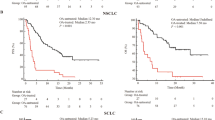
After screening 531 studies, a total of 7 articles involving 2690 patients were eligible for quantitative analysis. The use of opioids was negatively correlated with OS (HR 1.75, 95%CI 1.32–2.31, P < 0.001; I2 = 81%, P < 0.001) and significantly reduced the PFS (HR 1.61, 95%CI 1.41–1.83, P < 0.001; I2 = 0%, P = 0.63) of patients treated with ICIs. Similar results were obtained in each subgroup analysis. While NSAIDs could lead to poor OS (HR 1.25, 95% CI 1.03–1.51, P = 0.02; I2 = 0%, P = 0.60) but not PFS (HR 1.11, 95% CI = 0.89–1.39, P = 0.36) for ICIs patients. And sensitivity analyses confirmed the reliability of the results.
Conclusion
Opioids significantly reduced OS and PFS in patients receiving ICI therapy. Thus, the use of different types of opioids should be considered with caution, and it is necessary to actively develop alternative treatments.



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Angrish MD, Agha A, Pezo RC (2021) Association of antibiotics and other drugs with clinical outcomes in metastatic melanoma patients treated with immunotherapy. J Skin Cancer 2021:9120162. https://doi.org/10.1155/2021/9120162
Avery N, McNeilage AG, Stanaway F, Ashton-James CE, Blyth FM, Martin R, Gholamrezaei A, Glare P (2022) Efficacy of interventions to reduce long term opioid treatment for chronic non-cancer pain: systematic review and meta-analysis. BMJ 377:e066375. https://doi.org/10.1136/bmj-2021-066375
van den Beuken-van Everdingen MH, Hochstenbach LM, Joosten EA, Tjan-Heijnen VC, Janssen DJ (2016) Update on prevalence of pain in patients with cancer: systematic review and meta-analysis. J Pain Symptom Manage 51:1070-1090.e1079. https://doi.org/10.1016/j.jpainsymman.2015.12.340
Bironzo P, Pignataro D, Audisio M, Tagliamento M, Novello S (2019) P2.04–15 Association between opioids and outcome of 1st line immunotherapy in advanced nsclc patients: a retrospective evaluation. J Thoracic Oncol 14(10):S713
Botticelli A, Cirillo A, Pomati G, Cerbelli B, Scagnoli S, Roberto M, Gelibter A, Mammone G, Calandrella ML, Cerbelli E, Di Pietro FR, De Galitiis F, Lanzetta G, Cortesi E, Mezi S, Marchetti P (2021) The role of opioids in cancer response to immunotherapy. J Transl Med 19:119. https://doi.org/10.1186/s12967-021-02784-8
Che T, Roth BL (2021) Structural insights accelerate the discovery of opioid alternatives. Annu Rev Biochem 90:739–761. https://doi.org/10.1146/annurev-biochem-061620-044044
Cortellini A, Tucci M, Adamo V, Stucci LS, Russo A, Tanda ET, Spagnolo F, Rastelli F, Bisonni R, Santini D, Russano M, Anesi C, Giusti R, Filetti M, Marchetti P, Botticelli A, Gelibter A, Occhipinti MA, Marconcini R, Vitale MG, Nicolardi L, Chiari R, Bareggi C, Nigro O, Tuzi A, De Tursi M, Petragnani N, Pala L, Bracarda S, Macrini S, Inno A, Zoratto F, Veltri E, Di Cocco B, Mallardo D, Vitale MG, Pinato DJ, Porzio G, Ficorella C, Ascierto PA (2020) Integrated analysis of concomitant medications and oncological outcomes from PD-1/PD-L1 checkpoint inhibitors in clinical practice. J Immunother Cancer. https://doi.org/10.1136/jitc-2020-001361
Derosa L, Routy B, Thomas AM, Iebba V, Zalcman G, Friard S, Mazieres J, Audigier-Valette C, Moro-Sibilot D, Goldwasser F, Silva CAC, Terrisse S, Bonvalet M, Scherpereel A, Pegliasco H, Richard C, Ghiringhelli F, Elkrief A, Desilets A, Blanc-Durand F, Cumbo F, Blanco A, Boidot R, Chevrier S, Daillère R, Kroemer G, Alla L, Pons N, Le Chatelier E, Galleron N, Roume H, Dubuisson A, Bouchard N, Messaoudene M, Drubay D, Deutsch E, Barlesi F, Planchard D, Segata N, Martinez S, Zitvogel L, Soria JC, Besse B (2022) Intestinal Akkermansia muciniphila predicts clinical response to PD-1 blockade in patients with advanced non-small-cell lung cancer. Nat Med 28:315–324. https://doi.org/10.1038/s41591-021-01655-5
Gandhi S, Pandey M, Ammannagari N, Wang C, Bucsek MJ, Hamad L, Repasky E, Ernstoff MS (2020) Impact of concomitant medication use and immune-related adverse events on response to immune checkpoint inhibitors. Immunotherapy 12:141–149. https://doi.org/10.2217/imt-2019-0064
Gaucher L, Adda L, Séjourné A, Joachim C, Guillaume C, Poulet C, Liabeuf S, Gras-Champel V, Masmoudi K, Houessinon A, Bennis Y, Batteux B (2021) Associations between dysbiosis-inducing drugs, overall survival and tumor response in patients treated with immune checkpoint inhibitors. Ther Adv Med Oncol 13:17588359211000592. https://doi.org/10.1177/17588359211000591
Grivas P, Monk BJ, Petrylak D, Reck M, Foley G, Guenther S, Hennessy D, Makris C, Moehler M (2019) Immune checkpoint inhibitors as switch or continuation maintenance therapy in solid tumors: rationale and current state. Target Oncol 14:505–525. https://doi.org/10.1007/s11523-019-00665-1
WHO Guidelines Approved by the Guidelines Review Committee (2018). In: WHO Guidelines for the Pharmacological and Radiotherapeutic Management of Cancer Pain in Adults and Adolescents. World Health Organization © World Health Organization 2018., Geneva,
He Y, Guo X, May BH, Zhang AL, Liu Y, Lu C, Mao JJ, Xue CC, Zhang H (2020) Clinical evidence for association of acupuncture and acupressure with improved cancer pain: a systematic review and meta-analysis. JAMA Oncol 6:271–278. https://doi.org/10.1001/jamaoncol.2019.5233
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring Inconsistency in Meta-Analyses. BMJ 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Hoos A (2016) Development of immuno-oncology drugs - from CTLA4 to PD1 to the next generations. Nat Rev Drug Discov 15:235–247. https://doi.org/10.1038/nrd.2015.35
Hopkins AM, Badaoui S, Kichenadasse G, Karapetis CS, McKinnon RA, Rowland A, Sorich MJ (2022) Efficacy of Atezolizumab in patients with advanced NSCLC receiving concomitant antibiotic or proton pump inhibitor treatment: pooled analysis of five randomized control trials. J Thorac Oncol 17:758–767. https://doi.org/10.1016/j.jtho.2022.02.003
Huang R, Jiang L, Cao Y, Liu H, Ping M, Li W, Xu Y, Ning J, Chen Y, Wang X (2019) Comparative efficacy of therapeutics for chronic cancer pain: a bayesian network meta-analysis. J Clin Oncol 37:1742–1752. https://doi.org/10.1200/jco.18.01567
Iglesias-Santamaría A (2020) Impact of antibiotic use and other concomitant medications on the efficacy of immune checkpoint inhibitors in patients with advanced cancer. Clin Transl Oncol 22:1481–1490. https://doi.org/10.1007/s12094-019-02282-w
Knaul FM, Farmer PE, Krakauer EL, De Lima L, Bhadelia A, Jiang Kwete X, Arreola-Ornelas H, Gómez-Dantés O, Rodriguez NM, Alleyne GAO, Connor SR, Hunter DJ, Lohman D, Radbruch L, Madrigal DRS, M, Atun R, Foley KM, Frenk J, Jamison DT, Rajagopal MR, (2018) Alleviating the access abyss in palliative care and pain relief-an imperative of universal health coverage: the lancet commission report. Lancet 391:1391–1454. https://doi.org/10.1016/s0140-6736(17)32513-8
Kostine M, Mauric E, Tison A, Barnetche T, Barre A, Nikolski M, Rouxel L, Dutriaux C, Dousset L, Prey S, Beylot-Barry M, Seneschal J, Veillon R, Vergnenegre C, Daste A, Domblides C, Sionneau B, Gross-Goupil M, Ravaud A, Forcade E, Schaeverbeke T (2021) Baseline co-medications may alter the anti-tumoural effect of checkpoint inhibitors as well as the risk of immune-related adverse events. Eur J Cancer 157:474–484. https://doi.org/10.1016/j.ejca.2021.08.036
Lu H, Zhang H, Weng ML, Zhang J, Jiang N, Cata JP, Ma D, Chen WK, Miao CH (2021) Morphine promotes tumorigenesis and cetuximab resistance via EGFR signaling activation in human colorectal cancer. J Cell Physiol 236:4445–4454. https://doi.org/10.1002/jcp.30161
Macintyre PE, Quinlan J, Levy N, Lobo DN (2022) Current issues in the use of opioids for the management of postoperative pain: a review. JAMA Surg 157:158–166. https://doi.org/10.1001/jamasurg.2021.6210
Maher DP, Walia D, Heller NM (2020) Morphine decreases the function of primary human natural killer cells by both TLR4 and opioid receptor signaling. Brain Behav Immun 83:298–302. https://doi.org/10.1016/j.bbi.2019.10.011
Mao M, Qian Y, Sun J (2016) Morphine suppresses t helper lymphocyte differentiation to th1 type through pi3k/akt pathway. Inflammation 39:813–821. https://doi.org/10.1007/s10753-016-0310-x
Miura K, Sano Y, Niho S, Kawasumi K, Mochizuki N, Yoh K, Matsumoto S, Zenke Y, Ikeda T, Nosaki K, Kirita K, Udagawa H, Goto K, Kawasaki T, Hanada K (2021) Impact of concomitant medication on clinical outcomes in patients with advanced non-small cell lung cancer treated with immune checkpoint inhibitors: a retrospective study. Thorac Cancer 12:1983–1994. https://doi.org/10.1111/1759-7714.14001
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097. https://doi.org/10.1371/journal.pmed.1000097
Pinato DJ, Howlett S, Ottaviani D, Urus H, Patel A, Mineo T, Brock C, Power D, Hatcher O, Falconer A, Ingle M, Brown A, Gujral D, Partridge S, Sarwar N, Gonzalez M, Bendle M, Lewanski C, Newsom-Davis T, Allara E, Bower M (2019) Association of prior antibiotic treatment with survival and response to immune checkpoint inhibitor therapy in patients with cancer. JAMA Oncol 5:1774–1778. https://doi.org/10.1001/jamaoncol.2019.2785
Ribas A, Wolchok JD (2018) Cancer immunotherapy using checkpoint blockade. Science 359:1350–1355. https://doi.org/10.1126/science.aar4060
Scarborough BM, Smith CB (2018) Optimal pain management for patients with cancer in the modern era. CA Cancer J Clin 68:182–196. https://doi.org/10.3322/caac.21453
Svaton M, Zemanova M, Zemanova P, Kultan J, Fischer O, Skrickova J, Jakubikova L, Cernovska M, Hrnciarik M, Jirousek M, Krejci J, Krejci D, Bilek O, Blazek J, Hurdalkova K, Barinova M, Melichar B (2020) Impact of concomitant medication administered at the time of initiation of nivolumab therapy on outcome in non-small cell lung cancer. Anticancer Res. https://doi.org/10.21873/anticanres.14182
Taniguchi Y, Tamiya A, Isa S, Nakahama K, Atagi S (2019) P101–77 impact of oral drugs on the prognosis of non-small-cell lung cancer patients treated with Nivolumab. J Thoracic Oncol 14(10):S390
Taniguchi Y, Tamiya A, Matsuda Y, Adachi Y, Enomoto T, Azuma K, Kouno S, Tokoro A, Atagi S (2020) Opioids impair Nivolumab outcomes: a retrospective propensity score analysis in non-small-cell lung cancer. BMJ Support Palliat Care. https://doi.org/10.1136/bmjspcare-2020-002480
Tierney JF, Stewart LA, Ghersi D, Burdett S, Sydes MR (2007) Practical methods for incorporating summary time-to-event data into meta-analysis. Trials 8:16. https://doi.org/10.1186/1745-6215-8-16
Vercellino L, Cottereau A-S, Casasnovas O, Tilly H, Feugier P, Chartier L, Fruchart C, Roulin L, Oberic L, Pica GM, Ribrag V, Abraham J, Simon M, Gonzalez H, Bouabdallah R, Fitoussi O, Sebban C, López-Guillermo A, Sanhes L, Morschhauser F, Trotman J, Corront B, Choufi B, Snauwaert S, Godmer P, Briere J, Salles G, Gaulard P, Meignan M, Thieblemont C (2020) High total metabolic tumor volume at baseline predicts survival independent of response to therapy. Blood 135:1396–1405. https://doi.org/10.1182/blood.2019003526
Wells GA, Shea BJ, O'Connell D, Peterson J, Tugwell P (2000) The Newcastle–Ottawa Scale (NOS) for Assessing the Quality of Non-Randomized Studies in Meta-Analysis.
Xiong A, Wang J, Zhou C (2021) Immunotherapy in the first-line treatment of NSCLC: current status and future directions in china. Front Oncol 11:757993. https://doi.org/10.3389/fonc.2021.757993
Zajączkowska R, Leppert W, Mika J, Kocot-Kępska M, Woroń J, Wrzosek A, Wordliczek J (2018) Perioperative immunosuppression and risk of cancer progression: the impact of opioids on pain management. Pain Res Manag. https://doi.org/10.1155/2018/9293704
Funding
This work was supported by Liaoning Revitalization Talents Program (Grant No XLYC1905004), and Shenyang High-level Innovation Talents Plan (Grant No RC190403) for Kai Li, and Liaoning Provincial Natural Science Foundation (Grant No 2020-MS-157) for Liu Xiaofang, .
Author information
Authors and Affiliations
Contributions
Concept and design: L, G, Z. Acquisition, analysis, or interpretation of data: J, G, L. Drafting of the manuscript: J, G, Z, W. Critical revision of the manuscript for important intellectual content: L, Zhu. Statistical analysis: J, G, Z. Administrative, technical, or material support: L, L. Supervision: L, Z. All authors had full access to the data and take responsibility for the integrity of the data and accuracy of the analysis. K is the guarantor.
Corresponding author
Ethics declarations
Conflict of interest
NonE.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ju, M., Gao, Z., Liu, X. et al. The negative impact of opioids on cancer patients treated with immune checkpoint inhibitors: a systematic review and meta-analysis. J Cancer Res Clin Oncol 149, 2699–2708 (2023). https://doi.org/10.1007/s00432-022-04513-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04513-0