Abstract
Purpose
Prostate cancer (PCa) lacks specific markers capable of distinguishing aggressive tumors from those with indolent behavior. Therefore, the aim of this study was to evaluate the immunostaining of candidate proteins (PTEN, AKT, TRPM8, and NKX3.1) through the immunohistochemistry technique (IHC) on patients with metastatic and non-metastatic PCa.
Methods
Tissues from 60 patients were divided into three groups categorized according to prognostic parameters: better prognosis (n = 20), worse prognosis (n = 23), and metastatic (n = 17). Immunostaining was analyzed by a pathologist and staining classifications were considered according to signal intensity: (0) no staining, (+) weak, and (++ and +++) intermediate to strong.
Results
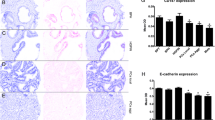
AKT protein was associated (p = 0.012) and correlated (p = 0.014; Tau = − 0.288) with the prognostic groups. The immunostaining for TRPM8 (p = 0.010) and NKX3.1 (p = 0.003) proteins differed between malignant tumor and non-tumoral adjacent tissue as well as for proteins in cellular locations (nucleus and cytoplasm). TRPM8 was independently associated with the ISUP grade ≥ 4 (p = 0.024; OR = 8.373; 95% CI = 1.319–53.164). The NKX3.1 showed positive and predominantly strong immunostaining in all patients in both tumoral and non-tumoral adjacent tissues. All metastatic samples had positive immunostaining, with strong intensity for NKX3.1 (p = 0.021; Tau = − 0.302). In the non-metastatic group, this strong protein staining was not observed in any patients.
Conclusion
This study confirmed that NKX3.1 is highly specific for prostate tissue and indicated that NKX3.1, AKT, and TRPM8 may be candidate markers for prostate cancer prognosis.


Similar content being viewed by others
Data availability
All data generated or analyzed during the current study are included in this published article.
Abbreviations
- WHO:
-
World Health Organization
- PCa:
-
Prostate cancer
- PSA:
-
Prostate-specific antigen
- IHC:
-
Immunohistochemistry
- PI3K:
-
Phosphatidylinositol-3-kinase
- AKT:
-
Serine/threonine kinase
- mTOR:
-
Mammalian target of the rapamycin complex
- TRPM8:
-
Transient receptor potential for melastatin 8
- NKX3.1:
-
NK3 homeobox 1
- HCL:
-
Londrina Cancer Hospital
- RP:
-
Radical prostatectomy
- TUR:
-
Transurethral resection
- NCCN:
-
National Comprehensive Cancer Network
- TNM:
-
Tumor/Node/Metastasis
- AJCC:
-
American Joint Committee on Cancer
- PBS:
-
Phosphate-buffered saline
- ISUP:
-
International Society of Urological Pathology
References
Abate-Shen C, Shen MM, Gelmann E (2008) Integrating differentiation and cancer: the NKx3.1 homeobox gene in prostate organogenesis and carcinogenesis. Differentiation 76:717–727. https://doi.org/10.1111/j.1432-0436.2008.00292.x
Abouhashem NS, Salah S (2020) Differential expression of NKX3.1 and HOXB13 in bone metastases originating from prostatic carcinoma among the Egyptian males. Pathol Res Pract 216:153221–153227. https://doi.org/10.1016/j.prp.2020.153221
Asuthkar S, Demirkhanyan L, Mueting SR, Cohen A, Zakharian E (2017) High-throughput proteome analysis reveals target TRPM8 degradation in prostate cancer. Oncotarget 8:12877–12891. https://doi.org/10.18632/oncotarget.14178
Asuthkar S, Demirkhanyan L, Sun X, Elustondo PA, Krishnan V, Baskaran P, Velpula KK, Thyagarajan B, Pavlov EV, Zakharian E (2015a) The TRPM8 protein is a testosterone receptor: II. Functional evidence for na ionotropic effect of testosterone on TRPM8. J Biol Chem 290:2670–2688. https://doi.org/10.1074/jbc.M114.610873
Asuthkar S, Elustondo PA, Demirkhanyan L, Sun X, Baskaran P, Velpula KK, Thyagarajan B, Pavlov EV, Zakharian E (2015b) The TRPM8 protein is a testosterone receptor: I. Biochemical evidence for direct TRPM8-testosterone interactions. J Biol Chem 290:2659–2669. https://doi.org/10.1074/jbc.M114.610824
Asuthkar S, Velpula KK, Elustondo PA, Demirkhanyan L, Zakharian E (2015c) TRPM8 channel as a novel molecular target in androgen-regulated prostate cancer cells. Oncotarget 6:17221–17236. https://doi.org/10.18632/oncotarget.3948
Bowen C, Stuart A, Ju JH, Tuan J, Blonder J, Conrads TP, Veenstra TD, Gelmann EP (2007) NKX3.1 homeodomain protein binds to topoisomerase I and enhances its activity. Mol Biol Pathol Genet 67:455–464. https://doi.org/10.1158/0008-5472.CAN-06-1591
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Glocal cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: A Cancer J Clin 68:394–424. https://doi.org/10.3322/caac.21492
Cambruzzi E, Zettler CG, Pegas KL, Teixeira SL (2010) Relação entre escore de Gleason e fatores prognósticos no adenocarcinoma acinar de próstata. Jornal Brasileiro De Patologia e Medicina Laboratorial 46:61–68. https://doi.org/10.1590/S1676-24442010000100011
Carrano AV, Natarajan AT (1988) Considerations for population monitoring using cytogenetic techniques. Mutat Res/genet Toxicol 204:379–406. https://doi.org/10.1016/0165-1218(88)90036-5
Compérat E (2019) New markers in prostate cancer: immunohistochemical. Arch Esp Urol 72:126–134
Culp MB, Soerjomataram I, Efstathiou JA, Bray F, Jemal A (2020) Recent global patterns in prostate cancer incidence and mortality rates. Eur Urol 77:38–52. https://doi.org/10.1016/j.eururo.2019.08.005
Epstein JI, Egevad L, Amin MB, Delahunt B, Srigley JR, Humphrey PA, Committee G (2016) The 2014 International Society of Urological Pathology (ISUP) consensus conference on Gleason grading of prostatic carcinoma: definition of grading patterns and proposal for a new grading system. Int Soc Urol Pathol 40:244–252. https://doi.org/10.1097/PAS.0000000000000530
European Association of Urology (2022) EAU – EANM – ESTRO – ESUR – ISUP – SIOG Guidelines on Prostate Cancer. Prostate Cancer. https://uroweb.org/guidelines/prostate-cancer/chapter/classification-and-staging-systems
Giannico GA, Arnold SA, Gellert LL, Hameed O (2017) New and emerging diagnostic and prognostic immunohistochemical biomarkers in prostate pathology. Adv Anat Pathol 24:35–44. https://doi.org/10.1097/PAP.0000000000000136
Global Cancer Observatory (2020) Câncer Today. International Agency for Research on Cancer. https://gco.iarc.fr/today/online-analysis-multi-bars?v=2020&mode=cancer&mode_population=countries&population=900&populations=900&key=total&sex=0&cancer=39&type=0&statistic=5&prevalence=0&population_group=0&ages_group%5B%5D=0&ages_group%5B%5D=17&nb_items=10&group_cancer=1&include_nmsc=1&include_nmsc_other=1&type_multiple=%257B%2522inc%2522%253Atrue%252C%2522mort%2522%253Afalse%252C%2522prev%2522%253Afalse%257D&orientation=horizontal&type_sort=0&type_nb_items=%257B%2522top%2522%253Atrue%252C%2522bottom%2522%253Afalse%257D. Accessed 7 Jan 2021
Goncalves MD, Hopkins BD, Cantley LC (2018) Phosphatidylinositol 3-Kinase, growth disorders, and cancer. N Engl J Med 379:2052–2062. https://doi.org/10.1056/NEJMra1704560
Griffin J, Chen Y, Catto JW, El-Khamisy S (2022) Gene of the month: NKX3.1. J Clin Pathol 75:361–364. https://doi.org/10.1136/jclinpath-2021-208073
Guembarovski AL, Guembarovski RL, Hirata BKB, Vitiello GAF, Suzuki KM, Enokida MT, Watanabe MAE, Reiche EMV (2018) CXCL12 chemokine and CXCR4 receptor: association with susceptibility and prognostic markers in triple negative breast cancer. Mol Biol Rep 45:741–750. https://doi.org/10.1007/s11033-018-4215-7
Gurel B, Ali TZ, Montgomery EA, Begum S, Hicks J, Goggins M, Eberhart CG, Clark DP, Bieberich CJ, Epsteins JI, De Marzo AM (2010) NKX3.1 as a marker of prostatic origin in metastatic tumors. Am J Surg Pathol 34:1097–1105. https://doi.org/10.1097/PAS.0b013e3181e6cbf3
Hamid AA, Gray KP, Huang Y, Bowden M, Pomerantz M, Loda M, Sweeney CJ (2019) Loss of PTEN expression detected by fluorescence immunohistochemistry predicts lethal prostate cancer in men treated with prostatectomy. Eur Urol Oncol 2:475–482. https://doi.org/10.1016/j.euo.2018.09.003
He WW, Sciavolino PJ, Wing J, Augustus M, Hudson P, Meissner PS, Curtis RT, Shell BK, Bostwick DG, Tindall DJ, Gelmann EP, Abate-Shen C (1997) A novel human prostate-specific, androgen-regulated homeobox gene (NKX3.1) that maps to 8p21, a region frequently deleted in prostate cancer. Genomics 43:69–77. https://doi.org/10.1006/geno.1997.4715
Huang H, Guma SR, Melamed J, Zhou M, Lee P, Deng FM (2018) NKX3.1 and PSMA are sensitive diagnostic markers for prostatic carcinoma in bone metastasis after decalcification of specimens. Am J Clin Exp Urol 6:182–188
Instituto Nacional de Câncer José Alencar Gomes da Silva (2019) Estimativa 2020: Incidência de Câncer no Brasil. INCA, Rio de Janeiro
Jamaspishvili T, Berman DM, Ross AE, Scher HI, De Marzo AM, Squire JÁ, Lotan TL (2018) Clinical implications of PTEN loss in prostate cancer. Nat Rev Urol 15:222–234. https://doi.org/10.1038/nrurol.2018.9
Junior FNF, Vasilceac FA, Gabriotti LFB, Spessoto LCF (2016) Câncer de próstata – atualidades. Artmed Panamericana, Porto Alegre
Koundouros N, Poulogiannis G (2018) Phophoinositide 3-Kinase/AKT signaling and redox metabolism in cancer. Front Oncol 8:160–169. https://doi.org/10.3389/fonc.2018.00160
Kristiansen G (2018) Markers of clinical utility in the differential diagnosis and prognosis of prostate cancer. Mod Pathol 31:143–155. https://doi.org/10.1038/modpathol.2017.168
Kristiansen I, Stephan C, Jung K, Dietel M, Rieger A, Tolkach Y, Kristiansen G (2017) Sensitivity of HOXB13 as a diagnostic immunohistochemical marker of prostatic origin in prostate cancer metastases: comparison to PSA, prostein, androgen receptor, ERG, NKX3.1, PSAP, and PSMA. Int J Mol Sci 18:1151–1160. https://doi.org/10.3390/ijms18061151
Kurose K, Zhou XP, Araki T, Cannistra SA, Maher ER, Eng C (2001) Frequent loss of PTEN expression is linked to elevated phosphorylated Akt levels, but not associated with p27 and cyclin D1 expression, in primary epithelial Ovarian Carcinomas. Am J Pathol 158:2097–2106. https://doi.org/10.1016/S0002-9440(10)64681-0
Löbler R, Pereira DV, Cóser VM, Neto NBF, Batuira GAC (2012) Avaliação do escore de Gleason como fator prognóstico em pacientes com cancer de próstata em hormonioterapia. Revista Brasileira De Oncologia Clínica 8:21–23
Lomas DJ, Ahmed HU (2020) All change in the prostate cancer diagnostic pathway. Nat Rev Clin Oncol 17:372–381. https://doi.org/10.1038/s41571-020-0332-z
Lotan TL, Gurel B, Sutcliffe S, Esopi D, Liu W, Xu J, Hicks JL, Park BH, Humphreys E, Partin AW, Han M, Netto GJ, Isaacs WB, De Marzo AM (2011) PTEN protein loss by immunostaining: analytic validation and prognostic indicator for a high risk surgical cohort of prostate cancer patients. Clin Cancer Res 17:6563–6573. https://doi.org/10.1158/1078-0432.CCR-11-1244
Lotan TL, Heumann A, Rico SD, Hicks J, Lecksell K, Koop C, Sauter G, Schlomm T, Simon R (2017) PTEN loss detection in prostate cancer: comparison of PTEN immunohistochemistry and PTEN FISH in a large retrospective prostatectomy cohort. Oncotarget 8:65566–65576. https://doi.org/10.18632/oncotarget.19217
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®) (2019) Prostate Cancer. NCCN
Orakpoghenor O, Avazi DO, Markus TP, Olaolu OS (2018) A short review of immunochemistry. Immunogenet Open Access 3:2–7
Porcaro AB, Tafuri A, Sebben M, Novella G, Processali T, Pirozzi M, Amigoni N, Rizzetto R, Shakir A, Panunzio A, De Michele M, Brunelli M, Cerruto MA, Migliorini F, Siracusano S, Artibani W (2019) Prostate volume index is able to differentiate between prostatic chronic inflammation and prostate cancer in patients with normal digital rectal examination and prostate-specific antigen values <10 ng/mL: results of 564 biopsy naïve cases. Urol Int 103:415–422. https://doi.org/10.1159/000502659
Puc J, Kozbial P, Li W, Tan Y, Liu Z, Suter T, Ohgi KA, Zhang J, Aggarwal AK, Rosenfeld MG (2015) Ligand-dependent enhancer activation regulated by topoisomerase-I activity. Cell 160:367–380. https://doi.org/10.1016/j.cell.2014.12.023
Robinson D, Allen EMV, Wu YM et al (2015) Integrative clinical genomics of advanced prostate cancer. Cell 161:1215–1228. https://doi.org/10.1016/j.cell.2015.05.001
Sociedade Brasileira de Urologia (2018) Nota oficial SBU e SBPC/ML – Rastreio de Câncer de Próstata. https://portaldaurologia.org.br/medicos/noticias/nota-oficial-sbu-e-sbpc-ml-rastreio-de-cancer-de-prostata/. Accessed 07 Jan 2021
Sreenivasulu K, Nandeesha H, Dorairajan LN, Ganesh RN (2018) Over expression of PI3K-AKT reduces apoptosis and increases prostate size in benign prostatic hyperplasia. Aging Male. https://doi.org/10.1080/13685538.2018.1519014
STRING CONSORTIUM 2020 (2021) Interation between PTEN and TRPM8. https://www.string-db.org/cgi/network?taskId=bLKI2jQjRS0r&sessionId=bjI64PH3Fa3s. Accessed 28 Jul 2021
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: Cancer J Clin 71:209–249. https://doi.org/10.3322/caac.21660
Taylor BS, Schultz N, Hieronymus H, Gopalan A, Xiao Y, Carver BS, Arora AK, Kaushik P, Cerami E, Reva B, Antipin Y, Mitsiades N, Landers T, Dolgalev I, Major JE, Wilson M, Socci ND, Lash AE, Heguy A, Eastham JA, Scher HI, Reuter VE, Scardino PT, Sander C, Sawyers CL, Gerald WL (2010) Integrative genomic profiling od human prostate cancer. Cancer Cell 18:11–22. https://doi.org/10.1016/j.ccr.2010.05.026
THE HUMAN PROTEIN ATLAS (2021a) PTEN. https://www.proteinatlas.org/ENSG00000171862-PTEN. Accessed 28 Jul 2021a
THE HUMAN PROTEIN ATLAS (2021b) AKT. https://www.proteinatlas.org/ENSG00000142208-AKT1. Accessed 28 Jul 2021b
THE HUMAN PROTEIN ATLAS (2021c) NKX3.1. https://www.proteinatlas.org/ENSG00000167034-NKX3-1. Accessed 28 Jul 2021c
Tsaveler L, Shapero MH, Morkowski S, Laus R (2001) Trp-p8, a novel prostate-specific gene, is up-regulated in prostate cancer and other malignancies and shares high homology with transiente receptor potencial calcium channel proteins. Can Res 61:3760–3769
Tse LA, Ho WM, Wang F, He YH, Ng CF (2018) Environmental risk factors of prostate cancer: a case-control study. Hong Kong Med J 24:S30-33
Vaidyanathan V, Karunasinghe N, Jabed A, Pallati R, Kao CHJ, Wang A, Marlow G, Ferguson LR (2016) Prostate cancer: is it a battle lost to age? Geriatrics 1:27–42. https://doi.org/10.3390/geriatrics1040027
Vendrami CL, McCarthy RJ, Chatterjee A, Casalino D, Schaeffer EM, Catalona WJ, Miller FH (2019) The utility of prostate specific antigen density, prostate health index, and prostate health index density in predicting positive prostate biopsy outcome is dependent on the prostate biopsy methods. Urology 129:153–159. https://doi.org/10.1016/j.urology.2019.03.018
Wozniak DJ, Kajdacsy-Balla A, Macias V, Ball-Kell S, Zenner ML, Bie W, Tyner AL (2017) PTEN is a protein phosphatase that targets active PTK6 and inhibits PTK6 oncogenic signaling in prostate cancer. Nat Commun 8:1–13. https://doi.org/10.1038/s41467-017-01574-5
Yee NS (2015) Roles of TRPM8 ion channels in cancer: proliferation, survival and invasion. Cancers 7:2134–2146. https://doi.org/10.3390/cancers7040882
Yu S, Xu Z, Zou C, Wu D, Wang Y, Yao X, Ng CF, Chan FL (2014) Ion channel TRPM8 promotes hypoxic growth of prostate cancer cells via an O2-independent and RACK1-mediated mechanism of HIF-1α stabilization. J Pathol 234:514–525. https://doi.org/10.1002/path.4413
Acknowledgements
All the authors would like to thank the Hospital do Câncer de Londrina and Angela Navarro Gordan for providing the samples for this study.
Funding
This study was supported by Fundação Araucária de Apoio ao Desenvolvimento Científico e Tecnológico do Paraná (Grant 185/2014), PPSUS (Grant 051/2021) and Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES—Finance Code 001). Pereira, E.R. received scholarship of CAPES and Cólus, I.M.S. received investigator fellowship awards from CNPq (Proc.308231/2017-1).
Author information
Authors and Affiliations
Contributions
ÉRP participated in the study design and acquisition of data, experimental procedures, performed the statistical analysis and interpretation, and drafted the manuscript. ALF and LCLP participated in the collection of samples and medical records, and also participated in the study design and immunohistochemical reactions. CAM participated in the study design and experimental procedures. AFMLG participated in the histopathological assays for the selection of tumor tissues and adjacent non-tumor tissues and performed the immunohistochemical analysis of the samples. KBdO participated in the statistical analysis and data interpretation. PEF made the sample collection possible. IMdSC participated in the design of the study and reviewed the manuscript for important intellectual content. RLG participated in the design of the study, interpretation of data, and gave final approval of the version to be published. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This study was approved by the Institutional Ethics Committee Involving Humans at State University of Londrina, Londrina—Paraná (PR), Brazil (CEP/UEL 176/2013; CAAE 19769913.0.0000.5231, in accordance with Resolution 466/12 of the National Research Ethics Commission).
Consent to participate
The study purpose and procedures were explained to all the patients and written informed consent was obtained from all the individual participants included in the study.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pereira, É.R., Pinheiro, L.C.L., Francelino, A.L. et al. Tissue immunostaining of candidate prognostic proteins in metastatic and non-metastatic prostate cancer. J Cancer Res Clin Oncol 149, 567–577 (2023). https://doi.org/10.1007/s00432-022-04274-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04274-w