Abstract
Introduction
Lung cancer with extrathoracic metastases is classified as M1c. However, extrathoracic metastases can be further classified into different patterns. The purpose of this study was to analyze the survival differences between different patterns of extrathoracic metastases in patients with stage M1c lung adenocarcinoma after receiving immunotherapy.
Materials and methods
This study included 160 stage M1c lung adenocarcinoma patients and treated with immunotherapy. The enrolled patients were divided into two groups: those with multiple extrathoracic metastases alone (EM group) and those with simultaneous multiple extrathoracic and intrathoracic metastases (EIM group). Progression-free survival (PFS) and overall survival (OS) were evaluated.
Results
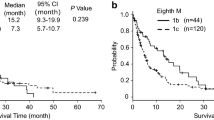
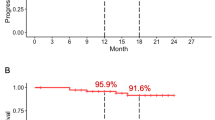
The median PFS and OS in the whole group were 7.7 months and 25.4 months, respectively. The patients in the EM group show better PFS (13.0 months vs. 5.0 months; hazard ratio [HR] = 0.462, 95% confidence interval [CI] 0.317–0.673, P < 0.0001) and OS (35.0 months vs. 18.9 months; HR 0.592, 95% CI 0.380–0.922, P = 0.019) compared with the EIM group. Furthermore, in patients with lung adenocarcinoma with simultaneous extrathoracic and intrathoracic metastases who received immunotherapy, immunotherapy combined with chemotherapy has better PFS and OS than immunotherapy alone. There was no difference between immunotherapy alone or combined with chemotherapy in patients with lung adenocarcinoma with extrathoracic metastasis alone.
Conclusion
The different patterns of extrathoracic metastasis were related to the efficacy and prognosis of immunotherapy in M1c cohort. In addition, patients with simultaneous extrathoracic and intrathoracic metastases were more recommended to choose immunotherapy in combination with chemotherapy rather than immunotherapy alone.






Similar content being viewed by others
Data availability
The data of the current study are available from the corresponding author and first author on reasonable request.
References
Altorki NK, Markowitz GJ, Gao D, Port JL, Saxena A, Stiles B et al (2019) The lung microenvironment: an important regulator of tumour growth and metastasis. Nat Rev Cancer 19(1):9–31. https://doi.org/10.1038/s41568-018-0081-9
Carter BW, Lichtenberger JP 3rd, Benveniste MK, de Groot PM, Wu CC, Erasmus JJ et al (2018) Revisions to the TNM staging of lung cancer: rationale, significance, and clinical application. Radiographics 38(2):374–391. https://doi.org/10.1148/rg.2018170081
Chansky K, Detterbeck FC, Nicholson AG, Rusch VW, Vallières E, Groome P, et al. (2017) The IASLC lung cancer staging project: external validation of the revision of the TNM stage groupings in the eighth edition of the TNM classification of lung Cancer. J Thorac Oncol 12(7):1109–1121. https://doi.org/10.1016/j.jtho.2017.04.011
Chardin D, Paquet M, Schiappa R, Darcourt J, Bailleux C, Poudenx M, et al. (2020) Baseline metabolic tumor volume as a strong predictive and prognostic biomarker in patients with non-small cell lung cancer treated with PD1 inhibitors: a prospective study. J Immunother Cancer. https://doi.org/10.1136/jitc-2020-000645.
Chen Z, Fillmore CM, Hammerman PS, Kim CF, Wong KK (2014) Non-small-cell lung cancers: a heterogeneous set of diseases. Nat Rev Cancer 14(8):535–546. https://doi.org/10.1038/nrc3775
Chen YJ, Roumeliotis TI, Chang YH, Chen CT, Han CL, Lin MH et al (2020) Proteogenomics of non-smoking lung cancer in East Asia delineates molecular signatures of pathogenesis and progression. Cell 182(1):226–44.e17. https://doi.org/10.1016/j.cell.2020.06.012
Sánchez de Cos Escuín J, Abal Arca J, Melchor Íñiguez R, Miravet Sorribes L, Núñez Ares A, Hernández Hernández JR, et al. (2014) Tumor, node and metastasis classification of lung cancer—M1a versus M1b—analysis of M descriptors and other prognostic factors. Lung Cancer 84(2):182–189. https://doi.org/10.1016/j.lungcan.2014.02.006.
Duraiswamy J, Freeman GJ, Coukos G (2014) Dual blockade of PD-1 and CTLA-4 combined with tumor vaccine effectively restores T-cell rejection function in tumors–response. Cancer Res 74(2):633–634; discussion 5. https://doi.org/10.1158/0008-5472.Can-13-2752.
Eberhardt WE, Mitchell A, Crowley J, Kondo H, Kim YT, Turrisi A, 3rd, et al. (2015) The IASLC lung cancer staging project: proposals for the revision of the M descriptors in the forthcoming eighth edition of the TNM classification of lung cancer. J Thorac Oncol 10(11):1515–1522. https://doi.org/10.1097/jto.0000000000000673.
Goldstraw P, Chansky K, Crowley J, Rami-Porta R, Asamura H, Eberhardt WE et al (2016) The IASLC lung cancer staging project: proposals for revision of the TNM stage groupings in the forthcoming (eighth) edition of the TNM classification for lung cancer. J Thorac Oncol 11(1):39–51. https://doi.org/10.1016/j.jtho.2015.09.009
Guisier F, Cousse S, Jeanvoine M, Thiberville L, Salaun M (2019) A rationale for surgical debulking to improve anti-PD1 therapy outcome in non small cell lung cancer. Sci Rep 9(1):16902. https://doi.org/10.1038/s41598-019-52913-z
Hanna NH, Robinson AG, Temin S, Baker S Jr, Brahmer JR, Ellis PM et al (2021) Therapy for stage IV non-small-cell lung cancer with driver alterations: ASCO and OH (CCO) joint guideline update. J Clin Oncol 39(9):1040–1091. https://doi.org/10.1200/jco.20.03570
He YY, Zhang XC, Yang JJ, Niu FY, Zeng Z, Yan HH et al (2014) Prognostic significance of genotype and number of metastatic sites in advanced non-small-cell lung cancer. Clin Lung Cancer 15(6):441–447. https://doi.org/10.1016/j.cllc.2014.06.006
Hu F, Zhang B, Li C, Xu J, Wang H, Gu P et al (2019) Prognosis of EGFR-mutant advanced lung adenocarcinoma patients with different intrathoracic metastatic patterns. J Cancer 10(5):1254–1262. https://doi.org/10.7150/jca.28601
Jiang C, Zhang N, Hu X, Wang H (2021) Tumor-associated exosomes promote lung cancer metastasis through multiple mechanisms. Mol Cancer 20(1):117. https://doi.org/10.1186/s12943-021-01411-w
Kim SI, Cassella CR, Byrne KT (2020) Tumor burden and immunotherapy: impact on immune infiltration and therapeutic outcomes. Front Immunol 11:629722. https://doi.org/10.3389/fimmu.2020.629722
Lambrechts D, Wauters E, Boeckx B, Aibar S, Nittner D, Burton O et al (2018) Phenotype molding of stromal cells in the lung tumor microenvironment. Nat Med 24(8):1277–1289. https://doi.org/10.1038/s41591-018-0096-5
Liu Y, Chen P, Wang H, Wu S, Zhao S, He Y et al (2021) The landscape of immune checkpoints expression in non-small cell lung cancer: a narrative review. Transl Lung Cancer Res 10(2):1029–1038. https://doi.org/10.21037/tlcr-20-1019
Mazieres J, Drilon A, Lusque A, Mhanna L, Cortot AB, Mezquita L et al (2019) Immune checkpoint inhibitors for patients with advanced lung cancer and oncogenic driver alterations: results from the IMMUNOTARGET registry. Ann Oncol 30(8):1321–1328. https://doi.org/10.1093/annonc/mdz167
Memmott RM, Wolfe AR, Carbone DP, Williams TM (2021) Predictors of response, progression-free survival, and overall survival in patients with lung cancer treated with immune checkpoint inhibitors. J Thorac Oncol 16(7):1086–1098. https://doi.org/10.1016/j.jtho.2021.03.017
Obara P, Pu Y (2013) Prognostic value of metabolic tumor burden in lung cancer. Chin J Cancer Res 25(6):615–622. https://doi.org/10.3978/j.issn.1000-9604.2013.11.10
Qu J, Jiang M, Wang L, Zhao D, Qin K, Wang Y et al (2020) Mechanism and potential predictive biomarkers of immune checkpoint inhibitors in NSCLC. Biomed Pharmacother 127:109996. https://doi.org/10.1016/j.biopha.2020.109996
Rami-Porta R (2021) Future perspectives on the TNM staging for lung cancer. Cancers (Basel). https://doi.org/10.3390/cancers13081940.
Schakenraad A, Hashemi S, Twisk J, Houda I, Ulas E, Daniels JMA et al (2021) The effect of tumor size and metastatic extent on the efficacy of first line pembrolizumab monotherapy in patients with high PD-L1 expressing advanced NSCLC tumors. Lung Cancer 162:36–41. https://doi.org/10.1016/j.lungcan.2021.10.002
Thai AA, Solomon BJ, Sequist LV, Gainor JF, Heist RS (2021) Lung cancer. Lancet 398(10299):535–554. https://doi.org/10.1016/s0140-6736(21)00312-3
Walters S, Maringe C, Coleman MP, Peake MD, Butler J, Young N et al (2013) Lung cancer survival and stage at diagnosis in Australia, Canada, Denmark, Norway, Sweden and the UK: a population-based study, 2004–2007. Thorax 68(6):551–564. https://doi.org/10.1136/thoraxjnl-2012-202297
Wood SL, Pernemalm M, Crosbie PA, Whetton AD (2014) The role of the tumor-microenvironment in lung cancer-metastasis and its relationship to potential therapeutic targets. Cancer Treat Rev 40(4):558–566. https://doi.org/10.1016/j.ctrv.2013.10.001
Yang CY, Yang JC, Yang PC (2020) Precision management of advanced non-small cell lung cancer. Annu Rev Med 71:117–136. https://doi.org/10.1146/annurev-med-051718-013524
Acknowledgements
This study was supported in part by the Chinese Society of Clinical Oncology (CSCO) Tumor Research Fund (No. Y-2019AZZD-0038), the Beijing Medical and health public welfare foundation project (No. YWJKJJHKYJ), and the National Natural Science Foundation of China (No. 82150005). The funding agencies played no role in the design, analysis or publication of the results of the study. The authors are grateful to all patients and their families for their participation in this study.
Author information
Authors and Affiliations
Contributions
Conception and design of study: Fang Hu, Liyan Jiang; Acquisition of data: Fang Hu, Jin Peng, Yanjie Niu, Meili Ma, Yizhuo Zhao, Aiqin Gu; Analysis and interpretation of data: Fang Hu, Jin Peng, Xiaowei Mao; All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflict of interest to disclose.
Consent to participate
Informed consent was obtained from all patients before the collection of information.
Ethics approval
This study was approved by the institutional review board of the Shanghai Chest Hospital (Shanghai, China; approval number: IS21127), and carried out in accordance with the Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hu, F., Peng, J., Mao, X. et al. Prognosis of different extrathoracic metastasis patterns in patients with M1c lung adenocarcinoma receiving immunotherapy. J Cancer Res Clin Oncol 149, 3171–3184 (2023). https://doi.org/10.1007/s00432-022-04182-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04182-z