Abstract
Purpose
Our objectives were to analyze the use of complementary and alternative medicine (CAM) in cancer patients and to describe the incidence and characteristics of interactions between CAM and antineoplastic agents.
Methods
We performed an observational study in cancer outpatients at a university hospital. Variables were collected through a 22-item questionnaire. Potential interactions between CAM and antineoplastic agents were analyzed using the Lexicomp®, the About Herbs®, and the summary of product characteristics. Mechanism of action, reliability, and the potential clinical effect of interactions were analyzed.
Results
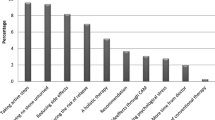
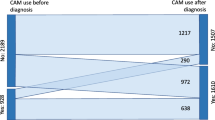
The study population comprised 937 patients, of whom 65% used CAM (70.6% herbal products, 25.8% dietary supplements, and 3.6% homeopathy). Female sex, younger age, and breast cancer were associated with more frequent use of CAM. The primary source of information about CAM was friends and family (43.5%). A total of 335 (57.1%) patients did not tell their doctor that they took CAM. The five most common CAM were chamomile, green tea, pennyroyal mint, linden, and rooibos. At least one interaction between CAM and antineoplastic agents was reported by 65.0% of CAM users (33.9% of all patients). Depending on the mechanism of action, 80% of CAM diminished the metabolism of the antineoplastic agents.
Conclusion
Our results reveal a high incidence of interactions between CAM and antineoplastic agents. The most frequent CAM were herbal products. Family and friends were the primary sources of information that led patients to start taking CAM, and more than half of the patients did not tell their doctor that they were taking CAM.
Similar content being viewed by others
Data availability
The data can be obtained upon a reasonable request from the corresponding author.
References
Asher GN, Corbett AH, Hawke RL (2017) Common herbal dietary supplement-drug interactions. Am Fam Physician 96(2):101–107
Bahall M (2017) Prevalence, patterns, and perceived value of complementary and alternative medicine among HIV patients: a descriptive study. BMC Complement Altern Med 17(1):422
Ben-Arye E, Samuels N, Goldstein LH, Mutafoglu K, Omran S, Schiff E, Charalambous H, Dweikat T, Ghrayeb I, Bar-Sela G, Turker I, Hassan A, Hassan E, Saad B, Nimri O, Kebudi R, Silbermann M (2016) Potential risks associated with traditional herbal medicine use in cancer care: a study of middle eastern oncology health care professionals. Cancer 122(4):598–610
Benoist GE, van Oort IM, Smeenk S et al (2018) Drug–drug interaction potential in men treated with enzalutamide: mind the gap. Br J Clin Pharmacol 84(1):122–129
Brooks SL, Rowan G, Michael M (2018) Potential issues with complementary medicines commonly used in the cancer population: a retrospective review of a tertiary cancer center’s experience. Asia Pac J Clin Oncol 14(5):e535–e542
Cao L, Wang X, Zhu G, Li S, Wang H, Wu J, Lu T, Li J (2021) Traditional Chinese medicine therapy for esophageal cancer: a literature review. Integr Cancer Ther 20:15347354211061720
Cassileth BR, Vickers AJ (2005) High prevalence of complementary and alternative medicine use among cancer patients: implications for research and clinical care. J Clin Oncol 23(12):2590–2592
Cheng YY, Hsieh CH, Tsai TH (2018) Concurrent administration of anticancer chemotherapy drug and herbal medicine on the perspective of pharmacokinetics. J Food Drug Ana 26(2S):S88–S95
Ciarlo G, Ahmadi E, Welter S, Hübner J (2019) Factors influencing the usage of complementary and alternative medicine by patients with cancer. Complement Ther Clin Pract 44:101389
Clement YN, Mahase V, Jagroop A, Kissoon K, Maharaj A, Mathura P, Quan CM, Ramadhin D, Mohammed C (2016) Herbal remedies and functional foods used by cancer patients attending specialty oncology clinics in Trinidad. BMC Complement Altern Med 16(1):399
Collado-Borrell R, Escudero-Vilaplana V, Calles A, Garcia-Martin E, Marzal-Alfaro B, Gonzalez-Haba E, Herranz-Alonso A, Sanjurjo-Saez M (2018) Oncology patient interest in the use of new technologies to manage their disease: cross-sectional survey. J Med Internet Res 20(10):e11006
Crichton M, Strike K, Isenring E, McCarthy AL, Marx W, Lohning A, Marshall S (2021) “It’s natural so it shouldn’t hurt me”: chemotherapy patients’ perspectives, experiences, and sources of information of complementary and alternative medicines. Complement Ther Clin Pract 43:101362
Davis EL, Oh B, Butow PN, Mullan BA, Clarke S (2012) Cancer patient disclosure and patient-doctor communication of complementary and alternative medicine use: a systematic review. Oncologist 17(11):1475–1481
Engdal S, Klepp O, Nilsen OG (2009) Identification and exploration of herb-drug combinations used by cancer patients. Integr Cancer Ther 8(1):29–36
Escudero-Vilaplana V, Collado-Borrell R, Hoyo-Muñoz A, Gimenez-Manzorro A, Calles A, Osorio S, Herranz-Alonso A, Sanjurjo-Sáez M (2020) Potential drug interactions between targeted oral antineoplastic agents and concomitant medication in clinical practice. Expert Opin Drug Saf 19(8):1041–1048
European Public Assessment Reports. Amsterdam: European Medicines Agency. Available at: https://www.ema.europa.eu/en/medicines. Accessed 25 Oct 2021
Fasinu PS, Rapp GK (2019) Herbal interaction with chemotherapeutic drugs-a focus on clinically significant findings. Front Oncol 9:1356
Firkins R, Eisfeld H, Keinki C, Buentzel J, Hochhaus A, Schmidt T, Huebner J (2018) The use of complementary and alternative medicine by patients in routine care and the risk of interactions. J Cancer Res Clin Oncol 144(3):551–557
Fritz H, Seely D, Kennedy DA, Fernandes R, Cooley K, Fergusson D (2013) Green tea and lung cancer: a systematic review. Integr Cancer Ther 12(1):7–24
Ge J, Tan BX, Chen Y, Yang L, Peng XC, Li HZ, Lin HJ, Zhao Y, Wei M, Cheng K, Li LH, Dong H, Gao F, He JP, Wu Y, Qiu M, Zhao YL, Su JM, Hou JM, Liu JY (2011) Interaction of green tea polyphenol epigallocatechin-3-gallate with sunitinib: potential risk of diminished sunitinib bioavailability. J Mol Med (berl) 89(6):595–602
Huebner J, Prott FJ, Micke O, Muecke R, Senf B, Dennert G, Muenstedt K (2014) PRIO (Working Group Prevention and Integrative Oncology - German Cancer Society) online survey of cancer patients on complementary and alternative medicine. Oncol Res Treat 37(6):304–308
Jazieh AR, Abuelgasim KA, Ardah HI, Alkaiyat M, Da’ar OB (2021) The trends of complementary alternative medicine use among cancer patients. BMC Complement Med Ther 21(1):167
Kanimozhi T, Hindu K, Maheshvari Y, Khushnidha YG, Kumaravel M, Srinivas KS, Manickavasagam M, Mangathayaru K (2021) Herbal supplement usage among cancer patients: a questionnaire-based survey. J Cancer Res Ther 17(1):136–141
Keene MR, Heslop IM, Sabesan SS, Glass BD (2019) Complementary and alternative medicine use in cancer: a systematic review. Complement Ther Clin Pract 35:33–47
Lapidari P, Djehal N, Havas J, Gbenou A, Martin E, Charles C, Dauchy S, Pistilli B, Cadeau C, Bertaut A, Everhard S, Martin AL, Coutant C, Cottu P, Menvielle G, Dumas A, Andre F, Michiels S, Vaz-Luis I, Di Meglio A (2021) Determinants of use of oral complementary-alternative medicine among women with early breast cancer: a focus on cancer-related fatigue. Breast Cancer Res Treat 190(3):517–529
Lexicomp. Drug interactions. Wolters Kluwer Clinical Drug Information. Hudson, Ohio: Lexi-Comp, Inc. www.lexi.com/online. Accessed 15 Nov 2021
Lyman GH, Greenlee H, Bohlke K, Bao T, DeMichele AM, Deng GE, Fouladbakhsh JM, Gil B, Hershman DL, Mansfield S, Mussallem DM, Mustian KM, Price E, Rafte S, Cohen L (2018) Integrative therapies during and after breast cancer treatment: ASCO endorsement of the SIO clinical practice guideline. J Clin Oncol 36(25):2647–2655
Mao JJ, Pillai GG, Andrade CJ, Ligibel JA, Basu P, Cohen L, Khan IA, Mustian KM, Puthiyedath R, Dhiman KS, Lao L, Ghelman R, Caceres Guido P, Lopez G, Gallego-Perez DF, Salicrup LA (2022) Integrative oncology: addressing the global challenges of cancer prevention and treatment. CA Cancer J Clin 72(2):144–164
Memorial Sloan Kettering Cancer Center’s About Herbs database. Memorial Sloan Kettering Cancer Center, New York. https://www.mskcc.org/cancer-care/diagnosis-treatment/symptom-management/integrative-medicine/herbs/search. Accessed 7 Oct 2021
Mohamed ME, Frye RF (2011) Effects of herbal supplements on drug glucuronidation. Review of clinical, animal, and in vitro studies. Planta Med 77(4):311–321
Molassiotis A, Fernández-Ortega P, Pud D, Ozden G, Scott JA, Panteli V, Margulies A, Browall M, Magri M, Selvekerova S, Madsen E, Milovics L, Bruyns I, Gudmundsdottir G, Hummerston S, Ahmad AM, Platin N, Kearney N, Patiraki E (2005) Use of complementary and alternative medicine in cancer patients: a European survey. Ann Oncol 16(4):655–663
Pezzani R, Salehi B, Vitalini S, Iriti M, Zuñiga FA, Sharifi-Rad J, Martorell M, Martins N (2019) Synergistic effects of plant derivatives and conventional chemotherapeutic agents: an update on the cancer perspective. Medicina (kaunas) 55(4):110
Ramos-Esquivel A, Víquez-Jaikel Á, Fernández C (2017) Potential drug-drug and herb-drug interactions in patients with cancer: a prospective study of medication surveillance. J Oncol Pract 13(7):e613–e622
Sáez-Garrido M, Espuny-Miró A, Ruiz-Gómez A, Díaz-Carrasco MS (2021) Drug-drug interactions in patients undergoing hematopoietic stem cell transplantation: systematic review. Farm Hosp 45(4):184–192
Scripture CD, Figg WD (2006) Drug interactions in cancer therapy. Nat Rev Cancer 6(7):546–558
Segal R, Pilote L (2016) Warfarin interaction with Matricaria chamomilla. Can Med Assoc J 174(9):1281–1282
Simpson E, Bernaitis N, Khan S, Grant G, Forster K, Anoopkumar-Dukie S (2022) An education on pharmacologically active complementary and alternative medicine and its effects on cancer treatment: literature review. Support Care Cancer 30(4):3057–3072
Teschke R, Xuan TD (2019) How can green tea polyphenols affect drug metabolism and should we be concerned? Expert Opin Drug Metab Toxicol 15(12):989–991
Theuser AK, Hack CC, Fasching PA, Antoniadis S, Grasruck K, Wasner S, Knoll S, Sievers H, Beckmann MW, Thiel FC (2021) Patterns and trends of herbal medicine use among patients with gynecologic cancer. Geburtshilfe Frauenheilkd 81(6):699–707
Tuna S, Dizdar O, Calis M (2013) The prevalence of usage of herbal medicines among cancer patients. J BUON 18(4):1048–1051
Vogel J, Zomorodbakhsch B, Stauch T, Josfeld L, Hübner J (2022) The role of the general practitioner in cancer care in general and with respect to complementary and alternative medicine for patients with cancer. Eur J Cancer Care (engl) 31(1):e13533
Wolf CPJG, Rachow T, Ernst T, Hochhaus A, Zomorodbakhsch B, Foller S, Rengsberger M, Hartmann M, Hübner J (2022) Interactions in cancer treatment considering cancer therapy, concomitant medications, food, herbal medicine and other supplements. J Cancer Res Clin Oncol 148(2):461–473
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
VEV, RCB, YJG, BMA, and MM: contributed to the study conception and design. Material preparation, data collection and analysis were performed by VEV, RCB, PGMS, ÁH-M, CVB, and JRH. The first draft of the manuscript was written by VEV and RCB, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest related to the research.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Escudero-Vilaplana, V., Collado-Borrell, R., Gómez Martínez-Sagrera, P. et al. Complementary and alternative medicine in cancer patients: characteristics of use and interactions with antineoplastic agents. J Cancer Res Clin Oncol 149, 2855–2882 (2023). https://doi.org/10.1007/s00432-022-04172-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04172-1