Abstract
Purpose
Define the impact of socio-demographic co-variates on outcomes of persons with newly-diagnosed chronic phase chronic myeloid leukaemia (CML).
Methods
Data of 961 consecutive subjects with newly-diagnosed CML were integrated for these outcomes in multi-variable Cox regression analyses after adjusting for confounders and interactions.
Results
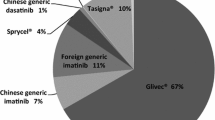
Elder age was associated with less use of a 2nd generation TKI as initial therapy. Household registration, comorbidity(ies) and education level were associated with use of a generic rather than branded TKI as initial therapy. Subjects with lower education level were more likely to be diagnosed with CML because of leukaemia-related symptoms. Rural registration and lower education level were also associated with a greater likelihood of switching TKI-therapy. Lower education level was associated with lower likelihood of achieving MMR [HR = 0.8 (0.7, 0.9), p = 0.002], MR4.5 [HR = 0.8 (0.7, 1.0), p = 0.055], and poor FFS [HR = 1.7 (1.3, 2.5); p < 0.001], PFS [HR = 2.0 (1.1, 5.0); p = 0.014], CML-related survival [HR = 2.5 (1.0, 10.0); p = 0.060] and survival [HR = 2.5 (1.0, 10.0); p = 0.043]. Males had lower rates of MMR and MR4.5 and worse FFS, but not survival compared with females. Being married was associated with a higher rate of MR4.5, fewer failures, progressions, and deaths.
Conclusion
Socio-demographic co-variates have a strong impact on therapy choice and responses in persons with newly-diagnosed CML, including circumstances of diagnosis, risk category and prognosis, use of initial TKI, switching TKIs, response to TKI-therapy, and outcomes.



Similar content being viewed by others
Data availability
Please contact author for data requests.
References
Baccarani M, Saglio G, Goldman J, Hochhaus A, Simonsson B, Appelbaum F et al (2006) Evolving concepts in the management of chronic myeloid leukemia: recommendations from an expert panel on behalf of the European LeukemiaNet. Blood 108(6):1809–1820. https://doi.org/10.1182/blood-2006-02-005686
Baccarani M, Cortes J, Pane F, Niederwieser D, Saglio G, Apperley J et al (2009) Chronic myeloid leukemia: an update of concepts and management recommendations of European LeukemiaNet. J Clin Oncol 27(35):6041–6051. https://doi.org/10.1200/JCO.2009.25.0779
Baccarani M, Deininger MW, Rosti G, Hochhaus A, Soverini S, Apperley JF et al (2013) European LeukemiaNet recommendations for the management of chronic myeloid leukemia: 2013. Blood 122(6):872–884. https://doi.org/10.1182/blood-2013-05-501569
Bhayat F, Das-Gupta E, Smith C, McKeever T, Hubbard R (2009) The incidence of and mortality from leukaemias in the UK: a general population-based study. BMC Cancer 9:252. https://doi.org/10.1186/1471-2407-9-252
Branford S, Yeung DT, Ross DM, Prime JA, Field CR, Altamura HK et al (2013) Early molecular response and female sex strongly predict stable undetectable BCR-ABL1, the criteria for imatinib discontinuation in patients with CML. Blood 121(19):3818–3824. https://doi.org/10.1182/blood-2012-10-462291
de Almeida MH, Pagnano KB, Vigorito AC, Lorand-Metze I, de Souza CA (2013) Adherence to tyrosine kinase inhibitor therapy for chronic myeloid leukemia: a Brazilian single-center cohort. Acta Haematol 130(1):16–22. https://doi.org/10.1159/000345722
Everist MM, Howard LE, Aronson WJ, Kane CJ, Amling CL, Cooperberg MR et al (2019) Socioeconomic status, race, and long-term outcomes after radical prostatectomy in an equal access health system: results from the SEARCH database. Urol Oncol 37(4):211–289. https://doi.org/10.1016/j.urolonc.2018.12.004
Experts in Chronic Myeloid Leukemia (2013) The price of drugs for chronic myeloid leukemia (CML) is a reflection of the unsustainable prices of cancer drugs: from the perspective of a large group of CML experts. Blood 121(22):4439–4442. https://doi.org/10.1182/blood-2013-03-490003
Ganesan P, Sagar TG, Dubashi B, Rajendranath R, Kannan K, Cyriac S et al (2011) Nonadherence to imatinib adversely affects event free survival in chronic phase chronic myeloid leukemia. Am J Hematol 86(6):471–474. https://doi.org/10.1002/ajh.22019
Geissler J, Sharf G, Bombaci F, Daban M, De Jong J, Gavin T et al (2017) Factors influencing adherence in CML and ways to improvement: results of a patient-driven survey of 2546 patients in 63 countries. J Cancer Res Clin Oncol 143(7):1167–1176. https://doi.org/10.1007/s00432-017-2372-z
Hochhaus A, Baccarani M, Silver RT, Schiffer C, Apperley JF, Cervantes F et al (2020) European LeukemiaNet 2020 recommendations for treating chronic myeloid leukemia. Leukemia 34(4):966–984. https://doi.org/10.1038/s41375-020-0776-2
Ibrahim AR, Eliasson L, Apperley JF, Milojkovic D, Bua M, Szydlo R et al (2011) Poor adherence is the main reason for loss of CCyR and imatinib failure for chronic myeloid leukemia patients on long-term therapy. Blood 117(14):3733–3736. https://doi.org/10.1182/blood-2010-10-309807
Jiang Q, Xu LP, Liu DH, Liu KY, Gale RP, Zhang MJ et al (2013) Imatinib results in better outcomes than HLA-identical sibling transplants in young persons with newly diagnosed chronic-phase chronic myelogenous leukemia. Leukemia 27(12):2410–2413. https://doi.org/10.1038/leu.2013.159
Kalmanti L, Saussele S, Lauseker M, Müller MC, Dietz CT, Heinrich L et al (2015) Safety and efficacy of imatinib in CML over a period of 10 years: data from the randomized CML-study IV. Leukemia 29(5):1123–1132. https://doi.org/10.1038/leu.2015.36
Keegan TH, Grogan RH, Parsons HM, Tao L, White MG, Onel K et al (2015) Sociodemographic disparities in differentiated thyroid cancer survival among adolescents and young adults in California. Thyroid 25(6):635–648. https://doi.org/10.1089/thy.2015.0021
Larfors G, Sandin F, Richter J, Själander A, Stenke L, Lambe M et al (2017) The impact of socio-economic factors on treatment choice and mortality in chronic myeloid leukaemia. Eur J Haematol 98(4):398–406. https://doi.org/10.1111/ejh.12845
Larson RA, Druker BJ, Guilhot F, O’Brien SG, Riviere GJ, Krahnke T et al (2008) Imatinib pharmacokinetics and its correlation with response and safety in chronic-phase chronic myeloid leukemia: a subanalysis of the IRIS study. Blood 111(8):4022–4028. https://doi.org/10.1182/blood-2007-10-116475
Lee JP, Birnstein E, Masiello D, Yang D, Yang AS (2009) Gender and ethnic differences in chronic myelogenous leukemia prognosis and treatment response: a single-institution retrospective study. J Hematol Oncol 2:30. https://doi.org/10.1186/1756-8722-2-30
Levine PH, Ajmera K, Neill OB, Venkatesh V, Garcia-Gonzalez P, Hoffman HJ (2016) Demographic factors related to young age at diagnosis of chronic myeloid leukemia in India. Clin Epidemiol Global Health 4(4):188–192. https://doi.org/10.1016/j.cegh.2016.06.001
Marin D, Bazeos A, Mahon FX, Eliasson L, Milojkovic D, Bua M et al (2010) Adherence is the critical factor for achieving molecular responses in patients with chronic myeloid leukemia who achieve complete cytogenetic responses on imatinib. J Clin Oncol 28(14):2381–2388. https://doi.org/10.1200/JCO.2009.26.3087
Patel MI, Schupp CW, Gomez SL, Chang ET, Wakelee HA (2013) How do social factors explain outcomes in non-small-cell lung cancer among Hispanics in California? Explaining the Hispanic paradox. J Clin Oncol 31(28):3572–3578. https://doi.org/10.1200/JCO.2012.48.6217
Perry AM, Brunner AM, Zou T, McGregor KL, Amrein PC, Hobbs GS et al (2017) Association between insurance status at diagnosis and overall survival in chronic myeloid leukemia: a population-based study. Cancer 123(13):2561–2569. https://doi.org/10.1002/cncr.30639
Pfirrmann M, Baccarani M, Saussele S, Guilhot J, Cervantes F, Ossenkoppele G et al (2016) Prognosis of long-term survival considering disease-specific death in patients with chronic myeloid leukemia. Leukemia 30(1):48–56. https://doi.org/10.1038/leu.2015.261
Qin YZ, Jiang Q, Jiang H, Li JL, Li LD, Zhu HH et al (2013) Which method better evaluates the molecular response in newly diagnosed chronic phase chronic myeloid leukemia patients with imatinib treatment, BCR-ABL(IS) or log reduction from the baseline level? Leuk Res 37(9):1035–1040. https://doi.org/10.1016/j.leukres.2013.06.003
Rego MN, Metze K, Lorand-Metze I (2015) Low educational level but not low income impairs the achievement of cytogenetic remission in chronic myeloid leukemia patients treated with imatinib in Brazil. Clinics (Sao Paulo) 70(5):322–325. https://doi.org/10.6061/clinics/2015(05)03
Sasaki K, Strom SS, O’Brien S, Jabbour E, Ravandi F, Konopleva M et al (2015) Relative survival in patients with chronic-phase chronic myeloid leukaemia in the tyrosine-kinase inhibitor era: analysis of patient data from six prospective clinical trials. Lancet Haematol 2(5):e186–e193. https://doi.org/10.1016/S2352-3026(15)00048-4
Singh GK, Jemal A (2017) Socioeconomic and racial/ethnic disparities in cancer mortality, incidence, and survival in the United States, 1950–2014: over six decades of changing patterns and widening inequalities. J Environ Public Health 2017:2819372. https://doi.org/10.1155/2017/2819372
Smith AG, Painter D, Howell DA, Evans P, Smith G, Patmore R et al (2014) Determinants of survival in patients with chronic myeloid leukaemia treated in the new era of oral therapy: findings from a UK population-based patient cohort. BMJ Open 4(1):e4266. https://doi.org/10.1136/bmjopen-2013-004266
Thein HH, Anyiwe K, Jembere N, Yu B, De P, Earle CC (2017) Effects of socioeconomic status on esophageal adenocarcinoma stage at diagnosis, receipt of treatment, and survival: a population-based cohort study. PLoS ONE 12(10):e186350. https://doi.org/10.1371/journal.pone.0186350
Tsai YF, Huang WC, Cho SF, Hsiao HH, Liu YC, Lin SF et al (2018) Side effects and medication adherence of tyrosine kinase inhibitors for patients with chronic myeloid leukemia in Taiwan. Medicine (Baltimore) 97(26):e11322. https://doi.org/10.1097/MD.0000000000011322
Utuama O, Mukhtar F, Pham YT, Dabo B, Manani P, Moser J et al (2019) Racial/ethnic, age and sex disparities in leukemia survival among adults in the United States during 1973–2014 period. PLoS ONE 14(8):e220864. https://doi.org/10.1371/journal.pone.0220864
Yu L, Wang H, Milijkovic D, Huang X, Jiang Q (2018) Achieving optimal response at 12 months is associated with a better health-related quality of life in patients with chronic myeloid leukemia: a prospective, longitudinal, single center study. BMC Cancer 18(1):782. https://doi.org/10.1186/s12885-018-4699-5
Acknowledgements
RPG acknowledges support from the National Institute of Health Research (NIHR) Biomedical Research Centre funding scheme.
Funding
Funded by the National Nature Science Foundation of China (No. 81770161; No. 81970140).
Author information
Authors and Affiliations
Contributions
LY: conceptualization, data curation, formal analysis, investigation, writing—original draft, and writing—review and editing. HW: conceptualization, data curation, formal analysis, investigation, writing—original draft, and writing—review and editing. RPG: conceptualization, methodology, supervision, writing—review and editing..YQ: investigation, writing—review and editing. YL: investigation, writing—review and editing. HS: investigation, writing—review and editing. XD: investigation, writing—review and editing. XH: conceptualization, methodology, writing—review and editing. QJ: conceptualization, data curation, formal analysis, funding acquisition, investigation, methodology, project administration, resources, supervision, writing—original draft, and writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
RPG is a consultant to BeiGene Ltd., Fusion Pharma LLC, LaJolla NanoMedical Inc., Mingsight Parmaceuticals Inc. and CStone Pharmaceuticals; advisor to Antegene Biotech LLC, Medical Director, FFF Enterprises Inc.; partner, AZAC Inc.; Board of Directors, Russian Foundation for Cancer Research Support; and Scientific Advisory Board: StemRad Ltd.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethics standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yu, L., Wang, H., Gale, R.P. et al. Impact of socio-demographic co-variates on prognosis, tyrosine kinase-inhibitor use and outcomes in persons with newly-diagnosed chronic myeloid leukaemia. J Cancer Res Clin Oncol 148, 449–459 (2022). https://doi.org/10.1007/s00432-021-03624-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-021-03624-4