Abstract
Purpose
SBRT demonstrated to increase survival in oligometastatic patients. Nevertheless, little is known regarding the natural history of oligometastatic disease (OMD) and how SBRT may impact the transition to the polymetastatic disease (PMD).
Methods
97 liver metastases in 61 oligometastatic patients were treated with SBRT. Twenty patients (33%) had synchronous oligometastases, 41 (67%) presented with metachronous oligometastases. Median number of treated metastases was 2 (range 1–5).
Results
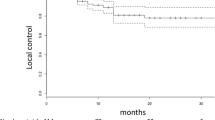
Median follow-up was 24 months. Median tPMC was 11 months (range 4–17 months). Median overall survival (OS) was 23 months (range 16–29 months). Cancer-specific survival predictive factors were having further OMD after SBRT (21 months versus 15 months; p = 0.00), and local control of treated metastases (27 months versus 18 months; p = 0.031). Median PFS was 7 months (range 4–12 months). Patients with 1 metastasis had longer median PFS as compared to those with 2–3 and 4–5 metastases (14.7 months versus 5.3 months versus 6.5 months; p = 0.041). At the last follow-up, 50/61 patients (82%) progressed, 16 of which (26.6%) again as oligometastatic and 34 (56%) as polymetastatic.
Conclusion
In the setting of oligometastatic disease, SBRT is able to delay the transition to the PMD. A proportion of patients relapse as oligometastatic and can be eventually evaluated for a further SBRT course. Interestingly, those patients retain a survival benefit as compared to those who had PMD. Further studies are needed to explore the role of SBRT in OMD and to identify treatment strategies able to maintain the oligometastatic state.




Similar content being viewed by others
References
Abdalla EK, Vauthey JN, Ellis LM et al (2004) Recurrence and outcomes following hepatic resection, radiofrequency ablation, and combined resection/ablation for colorectal liver metastases. Ann Surg 239(6):818–825
Adam R, Pascal G, Azoulay D, Tanaka K, Castaing D, Bismuth H (2003) Liver resection for colorectal metastases: the third hepatectomy. Ann Surg 238:871–883 (discussion: 83–84)
Alongi F, Arcangeli S, Filippi AR, Ricardi U, Scorsetti M (2012) Review and uses of stereotactic body radiation therapy for oligometastases. Oncologist 17(8):1100–1107. https://doi.org/10.1634/theoncologist.2012-0092
Alongi F, Mazzola R, Figlia V, Guckenberger M (2018) Stereotactic body radiotherapy for lung oligometastases: literature review according to PICO criteria. Tumori 104(3):148–156. https://doi.org/10.1177/0300891618766820
Al-Shafa F, Arifin AJ, Rodrigues GB, Palma DA, Louie AV (2019) A review of ongoing trials of stereotactic ablative radiotherapy for oligometastatic cancers: where will the evidence lead? Front Oncol 9:543. https://doi.org/10.3389/fonc.2019.00543
Arneth B (2018) Comparison of Burnet's clonal selection theory with tumor cell-clone development. Theranostics 8(12):3392–3399. https://doi.org/10.7150/thno.24083
Campbell PJ, Yachida S, Mudie LJ, Stephens PJ, Pleasance ED, Stebbings LA, Morsberger LA, Latimer C, McLaren S, Lin M-L, McBride DJ, Varela I, Nik-Zainal SA, Leroy C, Jia M, Menzies A, Butler AP, Teague JW, Griffin CA, Burton J, Swerdlow H, QuailMA SMR, Iacobuzio-Donahue C, Futreal PA (2010) Thepatterns and dynamics of genomic instability in metastatic pancreatic cancer. Nature 467:1109–1113. https://doi.org/10.1038/nature0946017
Clerici E, Comito T, Franzese C, Di Brina L, Tozzi A, Iftode C, Navarria P, Mancosu P, Reggiori G, Tomatis S, Scorsetti M (2019) Role of stereotactic body radiation therapy in the treatment of liver metastases: clinical results and prognostic factors. Strahlenther Onkol. https://doi.org/10.1007/s00066-019-01524-8
Eisenhauer E, Therasse P, Bogaerts J et al (2009) New response evaluation criteria in solid tumors: revised RECIST guideline (version 1.1). Eur J Cancer 45:228–247
Franzese C, Comito T, Toska E, Tozzi A, Clerici E, De Rose F, Franceschini D, Navarria P, Reggiori G, Tomatis S, Scorsetti M (2019) Predictive factors for survival of oligometastatic colorectal cancer treated with stereotactic body radiation therapy. Radiother Oncol 133:220–226. https://doi.org/10.1016/j.radonc.2018.10.024
Greco C, Pares O, Pimentel N, Louro V, Morales J, Nunes B, Castanheira J, Oliveira C, Silva A, Vaz S, Costa D, Zelefsky M, Kolesnick R, Fuks Z (2019) Phenotype-oriented ablation of oligometastatic cancer with single dose radiation therapy. Int J Radiat Oncol Biol Phys 104(3):593–603. https://doi.org/10.1016/j.ijrobp.2019.02.033
Gundem G, Loo P, Kremeyer B, Alexandrov LB, Tubio JMC, Papaemmanuil E, Brewer DS, Kallio HML, Högnäs G, Annala M, Kivinummi K, Goody V, Latimer C, Omeara S, Dawson KJ, Isaacs W, Emmert-Buck MR, Nykter M, Foster C, Kote-Jarai Z, Easton D, Whitaker HC, Neal DE, Cooper CS, Eeles RA, Visakorpi T, Campbell PJ, Mcdermott U, Wedge DC, Bova GS (2015) The evolutionary history of lethal metastatic prostate cancer. Nature 520(7547):353–357. https://doi.org/10.1038/nature14347
Hellman S, Weichselbaum RR (1995) Oligometastases. J Clin Oncol 13:8–10
Hoyer M, Roed D, Traberg Hansen A et al (2006) Phase II study on stereotactic body radiotherapy of colorectal metastases. Acta Oncol 45:823–830
Iijima Y, Hirotsu Y, Mochizuki H, Amemiya K, Oyama T, Uchida Y, Kobayashi Y, Tsutsui T, Kakizaki Y, Miyashita Y, Omata M (2018) Dynamic changes and drug-induced selection of resistant clones in a patient with EGFR-mutated adenocarcinoma that acquired T790M mutation and transformed to small-cell lung cancer. Clin Lung Cancer 19(6):e843–e847. https://doi.org/10.1016/j.cllc.2018.07.002
Kim MY, Oskarsson T, Acharyya S, Nguyen DX (2009) Tumor self-seeding by circulating cancer cells. Cell 139(7):1315–1326
Klein CA (2013) Selection and adaptation during metastatic cancer progression. Nature 501:365–372. https://doi.org/10.1038/nature12628
Klement RJ, Abbasi-Senger N, Adebahr S, Alheid H, Allgaeuer M, Becker G, Blanck O, Boda-Heggemann J, Brunner T, Duma M, Eble MJ, Ernst I, Gerum S, Habermehl D, Hass P, Henkenberens C, Hildebrandt G, Imhoff D, Kahl H, Klass ND, Krempien R, Lewitzki V, Lohaus F, Ostheimer C, Papachristofilou A, Petersen C, Rieber J, Schneider T, Schrade E, Semrau R, Wachter S, Wittig A, Guckenberger M, Andratschke N (2019) The impact of local control on overall survival after stereotactic body radiotherapy for liver and lung metastases from colorectal cancer: a combined analysis of 388 patients with 500 metastases. BMC Cancer 19(1):173. https://doi.org/10.1186/s12885-019-5362-5
Mazzola R, Fersino S, Alongi P, Di Paola G, Gregucci F, Aiello D, Tebano U, Pasetto S, Ruggieri R, Salgarello M, Alongi F (2018a) Stereotactic body radiation therapy for liver oligometastases: predictive factors of local response by (18)F-FDG-PET/CT. Br J Radiol 91(1088):20180058. https://doi.org/10.1259/bjr.20180058
Mazzola R, Fersino S, Ferrera G, Targher G, Figlia V, Triggiani L, Pasinetti N, Lo Casto A, Ruggieri R, Magrini SM, Alongi F (2018b) Stereotactic body radiotherapy for lung oligometastases impacts on systemic treatment-free survival: a cohort study. Med Oncol 35(9):121. https://doi.org/10.1007/s12032-018-1190-8
Meijerink MR, Puijk RS, van Tilborg AAJM, Henningsen KH, Fernandez LG, Neyt M, Heymans J, Frankema JS, de Jong KP, Richel DJ, Prevoo W, Vlayen J (2018) Radiofrequency and microwave ablation compared to systemic chemotherapy and to partial hepatectomy in the treatment of colorectal liver metastases: a systematic review and meta-analysis. Cardiovasc Intervent Radiol 41(8):1189–1204. https://doi.org/10.1007/s00270-018-1959-3
Mihai A, Mu Y, Armstrong J, Dunne M, Beriwal S, Rock L, Thirion P, Heron DE, Bird BH, Westrup J, Murphy CG, Huq MS, McDermott R (2017) Patients with colorectal lung oligometastases (L-OMD) treated by dose adapted SABR at diagnosis of oligometastatic disease have better outcomes than patients previously treated for their metastatic disease. J Radiosurg SBRT 5(1):43–53
Milano MT, Philip A, Okunieff P (2009) Analysis of patients with oligometastases undergoing two or more curative-intent stereotactic radiotherapy courses. Int J Radiat Oncol Biol Phys 73:832–837
Milano MT, Katz AW, Zhang H, Okunieff P (2012) Oligometastases treated with stereotactic body radiotherapy: long-term follow-up of prospective study. Int J Radiat Oncol Biol Phys 83:878–886
Nicosia L, Franzese C, Mazzola R, Franceschini D, Rigo M, Dagostino G, Corradini S, Alongi F, Scorsetti M (2019) Recurrence pattern of stereotactic body radiotherapy in oligometastatic prostate cancer: a multi-institutional analysis. Strahlenther Onkol. https://doi.org/10.1007/s00066-019-01523-9
Osti MF, Agolli L, Valeriani M, Reverberi C, Bracci S, Marinelli L, De Sanctis V, Cortesi E, Martelli M, De Dominicis C, Minniti G, Nicosia L (2018) 30 Gy single dose stereotactic body radiation therapy (SBRT): report on outcome in a large series of patients with lung oligometastatic disease. Lung Cancer 122:165–170. https://doi.org/10.1016/j.lungcan.2018.06.018
Palma DA, Olson R, Harrow S, Gaede S, Louie AV, Haasbeek C, Mulroy L, Lock M, Rodrigues GB, Yaremko BP, Schellenberg D, Ahmad B, Griffioen G, Senthi S, Swaminath A, Kopek N, Liu M, Moore K, Currie S, Bauman GS, Warner A, Senan S (2019) Stereotactic ablative radiotherapy versus standard of care palliative treatment in patients with oligometastatic cancers (SABR-COMET): a randomised, phase 2, open-label trial. Lancet 393(10185):2051–2058. https://doi.org/10.1016/S0140-6736(18)32487-5
Petrelli F, Comito T, Barni S, Pancera G, Scorsetti M, Ghidini A (2018) SBRT for CRC liver metastases. Stereotactic body radiotherapy for colorectal cancer liver metastases: a systematic review. Radiother Oncol. 129(3):427–434. https://doi.org/10.1016/j.radonc.2018.06.035
Pinker K, Riedl C, Weber WA (2017) Evaluating tumor response with FDG PET: updates on PERCIST, comparison with EORTC criteria and clues to future developments. Eur J Nucl Med Mol Imaging 44(Suppl 1):55–66. https://doi.org/10.1007/s00259-017-3687-3
Robin TP, Raben D, Schefter TE (2018) A contemporary update on the role of stereotactic body radiation therapy (SBRT) for liver metastases in the evolving landscape of oligometastatic disease management. Semin Radiat Oncol 28(4):288–294. https://doi.org/10.1016/j.semradonc.2018.06.009
Rusthoven KE, Kavanagh BD, Cardenes H et al (2009) Multiinstitutional phase I/II trial of stereotactic body radiation therapy for liver metastases. J Clin Oncol 27:1572–1578
Scorsetti M, Arcangeli S, Tozzi A, Comito T, Alongi F, Navarria P, Mancosu P, Reggiori G, Fogliata A, Torzilli G, Tomatis S, Cozzi L (2013) Is stereotactic body radiation therapy an attractive option for unresectable liver metastases? A preliminary report from a phase 2 trial. Int J Radiat Oncol Biol Phys 86(2):336–342. https://doi.org/10.1016/j.ijrobp.2012.12.021
Triggiani L, Alongi F, Buglione M, Detti B, Santoni R, Bruni A, Maranzano E, Lohr F, D'Angelillo R, Magli A, Bonetta A, Mazzola R, Pasinetti N, Francolini G, Ingrosso G, Trippa F, Fersino S, Borghetti P, Ghirardelli P, Magrini SM (2017) Efficacy of stereotactic body radiotherapy in oligorecurrent and in oligoprogressive prostate cancer: new evidence from a multicentric study. Br J Cancer 116(12):1520–1525. https://doi.org/10.1038/bjc.2017.103
Valentí V, Ramos J, Pérez C, Capdevila L, Ruiz I, Tikhomirova L, Sánchez M, Juez I, Llobera M, Sopena E, Rubió J, Salazar R (2019) Increased survival time or better quality of life? Trade-off between benefits and adverse events in the systemic treatment of cancer. Clin Transl Oncol. https://doi.org/10.1007/s12094-019-02216-6
Yachida S, Jones S, Bozic I, Antal T, Leary R, Fu B, KamiyamaM HRH, Eshleman JR, Nowak MA, Velculescu VE, Kinzler KW, Vogelstein B, Iacobuzio-Donahue CA (2010) Distant metastasis occurs late during the genetic evolution of pan-creatic cancer. Nature 467:1114–1117. https://doi.org/10.1038/nature09515
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nicosia, L., Cuccia, F., Mazzola, R. et al. Stereotactic body radiotherapy (SBRT) can delay polymetastatic conversion in patients affected by liver oligometastases. J Cancer Res Clin Oncol 146, 2351–2358 (2020). https://doi.org/10.1007/s00432-020-03223-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-020-03223-9