Abstract
Purpose
To evaluate the influence of overall treatment time (OTT) in disease control, acute, and long-term side effects with moderate hypofractionated external beam radiotherapy (RT) for prostate cancer (PCa) delivered either twice- or thrice-a-week.
Methods
157 patients with localized PCa were treated consecutively with 56 Gy in 4 Gy/fraction delivered either twice (86 patients, from 2003 to 2010, group-1) or thrice a week (71 patients, from 2010 to 2017, group-2) using IMRT or VMAT techniques. Gastrointestinal (GI) and genitourinary (GU) toxicities were scored according to the CTCAE v3.0 grading scale. Median follow-up was 110 and 56 months for groups 1 and 2, respectively.
Results
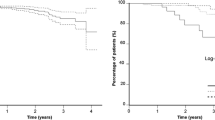
At 6 weeks, patients treated thrice-a-week experienced higher acute ≥ grade-2 GU toxicity compared to those treated twice a week (25.4% vs 5.8%, p = 0.001) even though none presented ≥ grade-3 GU or GI toxicity in the thrice-a-week group. The 5-year ≥ grade-2 late GU toxicity-free survival was higher in group-1 (95.9 ± 2.3%) than in group-2 (81.5 ± 4.9%, p = 0.003), while no differences in ≥ grade-2 late GI toxicity-free survival were observed between both groups (97.5 ± 1.7% vs. 97 ± 2.1% for groups 1 and 2, respectively). The 5-year biochemical relapse-free survival (bRFS) was not different for patients treated twice compared to those treated thrice-a-week (80.6 ± 4.5% vs. 85.3 ± 4.8%, respectively, p = 0.441), as much as for patients treated in > 5 weeks vs. those treated in ≤ 5 weeks (81.3 ± 4.4% vs. 84.4 ± 5.1%, respectively, p = 0.584).
Conclusions
In this retrospective hypothesis-generating analysis, less vs. more than 5 weeks OTT may increase acute and late GU toxicities without significantly improving bRFS in patients treated to high effective doses (> 80 Gy) with moderate hypofractionated RT. Prospective trials evaluating the impact of OTT on hypofractionated schedules for PCa are warranted.



Similar content being viewed by others
References
Amdur RJ, Parsons JT, Fitzgerald LT, Million RR (1990) The effect of overall treatment time on local control in patients with adenocarcinoma of the prostate treated with radiation therapy. Int J Radiat Oncol Biol Phys 19(6):1377–1382
D’Ambrosio DJ, Li T, Horwitz EM, Chen DY, Pollack A, Buyyounouski MK (2008) Does treatment duration affect outcome after radiotherapy for prostate cancer? Int J Radiat Oncol Biol Phys 72(5):1402–1407. https://doi.org/10.1016/j.ijrobp.2008.03.011
Dearnaley D, Syndikus I, Mossop H, Khoo V, Birtle A, Bloomfield D, Graham J, Kirkbride P, Logue J, Malik Z, Money-Kyrle J, O’Sullivan JM, Panades M, Parker C, Patterson H, Scrase C, Staffurth J, Stockdale A, Tremlett J, Bidmead M, Mayles H, Naismith O, South C, Gao A, Cruickshank C, Hassan S, Pugh J, Griffin C, Hall E, Investigators CH (2016) Conventional versus hypofractionated high-dose intensity-modulated radiotherapy for prostate cancer: 5-year outcomes of the randomised, non-inferiority, phase 3 CHHiP trial. Lancet Oncol 17(8):1047–1060. https://doi.org/10.1016/S1470-2045(16)30102-4
Diaz A, Roach M IIIrd, Marquez C, Coleman L, Pickett B, Wolfe JS, Carroll P, Narayan P (1994) Indications for and the significance of seminal vesicle irradiation during 3D conformal radiotherapy for localized prostate cancer. Int J Radiat Oncol Biol Phys 30(2):323–329
Dong Y, Zaorsky NG, Li T, Churilla TM, Viterbo R, Sobczak ML, Smaldone MC, Chen DY, Uzzo RG, Hallman MA, Horwitz EM (2018) Effects of interruptions of external beam radiation therapy on outcomes in patients with prostate cancer. J Med Imaging Radiat Oncol 62(1):116–121. https://doi.org/10.1111/1754-9485.12675
Fonteyne V, Sarrazyn C, Swimberghe M, De Meerleer G, Rammant E, Vanderstraeten B, Vanpachtenbeke F, Lumen N, Decaestecker K, Colman R, Villeirs G, Ost P (2018) 4 weeks versus 5 weeks of hypofractionated high-dose radiation therapy as primary therapy for prostate cancer: interim safety analysis of a randomized phase 3 trial. Int J Radiat Oncol Biol Phys 100(4):866–870. https://doi.org/10.1016/j.ijrobp.2017.12.016
Gao M, Mayr NA, Huang Z, Zhang H, Wang JZ (2010) When tumor repopulation starts? The onset time of prostate cancer during radiation therapy. Acta Oncol 49(8):1269–1275. https://doi.org/10.3109/0284186X.2010.509737
Graf R, Wust P, Hildebrandt B, Gogler H, Ullrich R, Herrmann R, Riess H, Felix R (2003) Impact of overall treatment time on local control of anal cancer treated with radiochemotherapy. Oncology 65(1):14–22. https://doi.org/10.1159/000071200
Haustermans KM, Hofland I, Van Poppel H, Oyen R, Van de Voorde W, Begg AC, Fowler JF (1997) Cell kinetic measurements in prostate cancer. Int J Radiat Oncol Biol Phys 37(5):1067–1070
Horwitz EM, Vicini FA, Ziaja EL, Dmuchowski CF, Stromberg JS, Gustafson GS, Martinez AA (1997) An analysis of clinical and treatment related prognostic factors on outcome using biochemical control as an end-point in patients with prostate cancer treated with external beam irradiation. Radiother Oncol J Eur Soc Ther Radiol Oncol 44(3):223–228
Incrocci L, Wortel RC, Alemayehu WG, Aluwini S, Schimmel E, Krol S, van der Toorn PP, Jager H, Heemsbergen W, Heijmen B, Pos F (2016) Hypofractionated versus conventionally fractionated radiotherapy for patients with localised prostate cancer (HYPRO): final efficacy results from a randomised, multicentre, open-label, phase 3 trial. Lancet Oncol 17(8):1061–1069. https://doi.org/10.1016/S1470-2045(16)30070-5
King CR, Brooks JD, Gill H, Pawlicki T, Cotrutz C, Presti JC Jr (2009) Stereotactic body radiotherapy for localized prostate cancer: interim results of a prospective phase II clinical trial. Int J Radiat Oncol Biol Phys 73(4):1043–1048. https://doi.org/10.1016/j.ijrobp.2008.05.059
Koukourakis M, Hlouverakis G, Kosma L, Skarlatos J, Damilakis J, Giatromanolaki A, Yannakakis D (1996) The impact of overall treatment time on the results of radiotherapy for nonsmall cell lung carcinoma. Int J Radiat Oncol Biol Phys 34(2):315–322
Kountouri M, Zilli T, Rouzaud M, Dubouloz A, Linero D, Escude L, Jorcano S, Miralbell R (2016) Moderate hypofractionated protracted radiation therapy and dose escalation for prostate cancer: do dose and overall treatment time matter? Int J Radiat Oncol Biol Phys 94(2):272–279. https://doi.org/10.1016/j.ijrobp.2015.10.055
Lai PP, Perez CA, Shapiro SJ, Lockett MA (1990) Carcinoma of the prostate stage B and C: lack of influence of duration of radiotherapy on tumor control and treatment morbidity. Int J Radiat Oncol Biol Phys 19(3):561–568
Lai PP, Pilepich MV, Krall JM, Asbell SO, Hanks GE, Perez CA, Rubin P, Sause WT, Cox JD (1991) The effect of overall treatment time on the outcome of definitive radiotherapy for localized prostate carcinoma: the Radiation Therapy Oncology Group 75-06 and 77-06 experience. Int J Radiat Oncol Biol Phys 21(4):925–933
Lee WR, Dignam JJ, Amin MB, Bruner DW, Low D, Swanson GP, Shah AB, D’Souza DP, Michalski JM, Dayes IS, Seaward SA, Hall WA, Nguyen PL, Pisansky TM, Faria SL, Chen Y, Koontz BF, Paulus R, Sandler HM (2016) Randomized phase III noninferiority study comparing two radiotherapy fractionation schedules in patients with low-risk prostate cancer. J Clin Oncol 34(20):2325–2332. https://doi.org/10.1200/JCO.2016.67.0448
Leyh-Bannurah SR, Karakiewicz PI, Pompe RS, Preisser F, Zaffuto E, Dell’Oglio P, Briganti A, Nafez O, Fisch M, Steuber T, Graefen M, Budaus L (2018) Inverse stage migration patterns in North American patients undergoing local prostate cancer treatment: a contemporary population-based update in light of the 2012 USPSTF recommendations. World J Urol. https://doi.org/10.1007/s00345-018-2396-2
Miralbell R, Roberts SA, Zubizarreta E, Hendry JH (2012) Dose-fractionation sensitivity of prostate cancer deduced from radiotherapy outcomes of 5,969 patients in seven international institutional datasets: alpha/beta = 1.4 (0.9–2.2) Gy. Int J Radiat Oncol Biol Phys 82(1):e17–e24. https://doi.org/10.1016/j.ijrobp.2010.10.075
Murphy CT, Galloway TJ, Handorf EA, Egleston BL, Wang LS, Mehra R, Flieder DB, Ridge JA (2016) Survival impact of increasing time to treatment initiation for patients with head and neck cancer in the United States. J Clin Oncol 34(2):169–178. https://doi.org/10.1200/JCO.2015.61.5906
Perez CA, Grigsby PW, Castro-Vita H, Lockett MA (1995) Carcinoma of the uterine cervix. I. Impact of prolongation of overall treatment time and timing of brachytherapy on outcome of radiation therapy. Int J Radiat Oncol Biol Phys 32(5):1275–1288. https://doi.org/10.1016/0360-3016(95)00220-S
Perez CA, Michalski J, Mansur D, Lockett MA (2004) Impact of elapsed treatment time on outcome of external-beam radiation therapy for localized carcinoma of the prostate. Cancer J 10(6):349–356
Quon HC, Ong A, Cheung P, Chu W, Chung HT, Vesprini D, Chowdhury A, Panjwani D, Pang G, Korol R, Davidson M, Ravi A, McCurdy B, Zhang L, Mamedov A, Deabreu A, Loblaw A (2018) Once-weekly versus every-other-day stereotactic body radiotherapy in patients with prostate cancer (PATRIOT): a phase 2 randomized trial. Radiother Oncol J Eur Soc Ther Radiol Oncol 127(2):206–212. https://doi.org/10.1016/j.radonc.2018.02.029
Reis Ferreira M, Khan A, Thomas K, Truelove L, McNair H, Gao A, Parker CC, Huddart R, Bidmead M, Eeles R, Khoo V, van As NJ, Hansen VN, Dearnaley DP (2017) Phase 1/2 dose-escalation study of the use of intensity modulated radiation therapy to treat the prostate and pelvic nodes in patients with prostate cancer. Int J Radiat Oncol Biol Phys 99(5):1234–1242. https://doi.org/10.1016/j.ijrobp.2017.07.041
Roach M IIIrd, Marquez C, Yuo HS, Narayan P, Coleman L, Nseyo UO, Navvab Z, Carroll PR (1994) Predicting the risk of lymph node involvement using the pre-treatment prostate specific antigen and Gleason score in men with clinically localized prostate cancer. Int J Radiat Oncol Biol Phys 28(1):33–37
Roach M IIIrd, Hanks G, Thames H Jr, Schellhammer P, Shipley WU, Sokol GH, Sandler H (2006) Defining biochemical failure following radiotherapy with or without hormonal therapy in men with clinically localized prostate cancer: recommendations of the RTOG-ASTRO Phoenix Consensus Conference. Int J Radiat Oncol Biol Phys 65(4):965–974. https://doi.org/10.1016/j.ijrobp.2006.04.029
Thames HD, Kuban D, Levy LB, Horwitz EM, Kupelian P, Martinez A, Michalski J, Pisansky T, Sandler H, Shipley W, Zelefsky M, Zietman A (2010) The role of overall treatment time in the outcome of radiotherapy of prostate cancer: an analysis of biochemical failure in 4839 men treated between 1987 and 1995. Radiother Oncol J Eur Soc Ther Radiol Oncol 96(1):6–12. https://doi.org/10.1016/j.radonc.2010.03.020
Vogelius IR, Bentzen SM (2018) Dose response and fractionation sensitivity of prostate cancer after external beam radiation therapy: a meta-analysis of randomized trials. Int J Radiat Oncol Biol Phys 100(4):858–865. https://doi.org/10.1016/j.ijrobp.2017.12.011
Withers HR, Taylor JM, Maciejewski B (1988) The hazard of accelerated tumor clonogen repopulation during radiotherapy. Acta Oncol 27(2):131–146
Zilli T, Jorcano S, Rouzaud M, Dipasquale G, Nouet P, Toscas JI, Casanova N, Wang H, Escude L, Molla M, Linero D, Weber DC, Miralbell R (2011) Twice-weekly hypofractionated intensity-modulated radiotherapy for localized prostate cancer with low-risk nodal involvement: toxicity and outcome from a dose escalation pilot study. Int J Radiat Oncol Biol Phys 81(2):382–389. https://doi.org/10.1016/j.ijrobp.2010.05.057
Acknowledgements
This study has been funded by a research grant from the “Fundació Privada Cellex”, Spain and the “Fondation pour la lutte contre le cancer et pour des recherches médico-biologiques”, Geneva, Switzerland.
Author information
Authors and Affiliations
Contributions
All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Achard, V., Jorcano, S., Rouzaud, M. et al. Twice- vs. thrice-weekly moderate hypofractionated radiotherapy for prostate cancer: does overall treatment time matter?. J Cancer Res Clin Oncol 145, 1581–1588 (2019). https://doi.org/10.1007/s00432-019-02893-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-019-02893-4