Abstract
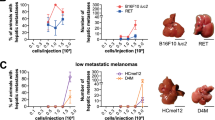
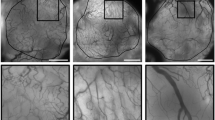
Tumour angiogenesis is defined by an anarchic vasculature and irregularities in alignment of endothelial cells. These structural abnormalities could explain the variability in distribution of nanomedicines in various tumour models. Then, the main goal of this study was to compare and to characterize the tumour vascular structure in different mouse models of melanoma tumours (B16F10 and SK-Mel-28) and in human melanomas from different patients. Tumours were obtained by subcutaneous injection of 106 B16F10 and 3.106 SK-Mel-28 melanoma cells in C57BL/6 and nude mice, respectively. Tumour growth was evaluated weekly, while vasculature was analysed through fluorescent labelling via CD31 and desmin. Significant differences in tumour growth and mice survival were evidenced between the two melanoma models. A fast evolution of tumours was observed for B16F10 melanoma, reaching a tumour size of 100 mm3 in 7 days compared to SK-Mel-28 which needed 21 days to reach the same volumes. Important differences in vascularization were exposed between the melanoma models, characterized by a significant enhancement of vascular density and a significant lumen size for mice melanoma models compared to human. Immunostaining revealed irregularities in endothelium structure for both melanoma models, but structural differences of vasculature were observed, characterized by a stronger expression of desmin in SK-Mel-28 tumours. While human melanoma mainly develops capillaries, structural irregularities are also observed on the samples of this tumour model. Our study revealed an impact of cell type and tumour progression on the structural vasculature of melanoma, which could impact the distribution of drugs in the tumour environment.




Similar content being viewed by others
References
Armulik A, Genove G, Betsholtz C (2011) Pericytes: developmental, physiological, and pathological perspectives, problems, and promises. Dev Cell 21:193–215. https://doi.org/10.1016/j.devcel.2011.07.001
Baluk P, Hashizume H, McDonald DM (2005) Cellular abnormalities of blood vessels as targets in cancer. Curr Opin Genet Dev 15:102–111. https://doi.org/10.1016/j.gde.2004.12.005
Barenholz Y (2012) Doxil®--the first FDA-approved nano-drug: lessons learned. J Control Release 160:117–134. https://doi.org/10.1016/j.jconrel.2012.03.020
Bolkestein M, de Blois E, Koelewijn SJ, Eggermont AM, Grosveld F, de Jong M, Koning GA (2016) Investigation of factors determining the enhanced permeability and retention effect in subcutaneous Xenografts. J Nucl Med 57:601–607. https://doi.org/10.2967/jnumed.115.166173
Carmeliet P, Jain RK (2000) Angiogenesis in cancer and other diseases Nature 407:249–257. https://doi.org/10.1038/35025220
Chan RC, Babbs CF, Vetter RJ, Lamar CH (1984) Abnormal response of tumor vasculature to vasoactive drugs. J Natl Cancer Inst 72:145–150. https://doi.org/10.1093/jnci/72.1.145
Choi YP, Shim HS, Gao MQ, Kang S, Cho NH (2011) Molecular portraits of intratumoral heterogeneity in human ovarian cancer. Cancer Lett 307:62–71. https://doi.org/10.1016/j.canlet.2011.03.018
Clere N et al (2010) Deficiency or blockade of angiotensin II type 2 receptor delays tumorigenesis by inhibiting malignant cell proliferation and angiogenesis. Int J Cancer 127:2279–2291. https://doi.org/10.1002/ijc.25234
Danciu C et al (2013) A characterization of four B16 murine melanoma cell sublines molecular fingerprint and proliferation behavior. Cancer Cell Int 13:75. https://doi.org/10.1186/1475-2867-13-75
Danciu C et al (2015) Behaviour of four different B16 murine melanoma cell sublines: C57BL/6J skin Int. J Exp Pathol 96:73–80. https://doi.org/10.1111/iep.12114
Danhier F (2016) To exploit the tumor microenvironment: since the EPR effect fails in the clinic, what is the future of nanomedicine? J Control Release 244:108–121. https://doi.org/10.1016/j.jconrel.2016.11.015
Danhier F et al (2015) Paclitaxel-loaded micelles enhance transvascular permeability and retention of nanomedicines in tumors. Int J Pharm 479:399–407. https://doi.org/10.1016/j.ijpharm.2015.01.009
Danquah MK, Zhang XA, Mahato RI (2011) Extravasation of polymeric nanomedicines across tumor vasculature Adv Drug Deliv Rev 63:623–639. https://doi.org/10.1016/j.addr.2010.11.005
De Bock K, De Smet F, Leite De Oliveira R, Anthonis K, Carmeliet P (2009) Endothelial oxygen sensors regulate tumor vessel abnormalization by instructing phalanx endothelial cells. J Mol Med (Berl) 87:561–569. https://doi.org/10.1007/s00109-009-0482-z
De Bock K, Cauwenberghs S, Carmeliet P (2011) Vessel abnormalization: another hallmark of cancer? Molecular mechanisms and therapeutic implications. Curr Opin Genet Dev 21:73–79. https://doi.org/10.1016/j.gde.2010.10.008
Dudley AC (2012) Tumor endothelial cells Cold Spring. Harb Perspect Med 2:a006536. https://doi.org/10.1101/cshperspect.a006536
Duncan R, Sat-Klopsch YN, Burger AM, Bibby MC, Fiebig HH, Sausville EA (2013) Validation of tumour models for use in anticancer nanomedicine evaluation: the EPR effect and cathepsin B-mediated drug release rate. Cancer Chemother Pharmacol 72:417–427. https://doi.org/10.1007/s00280-013-2209-7
Egeblad M, Nakasone ES, Werb Z (2010) Tumors as organs: complex tissues that interface with the entire organism. Dev Cell 18:884–901. https://doi.org/10.1016/j.devcel.2010.05.012
Elder DE, Van Belle P, Elenitsas R, Halpern A, Guerry D (1996) Neoplastic progression and prognosis in melanoma Semin Cutan Med Surg 15:336–348. https://doi.org/10.1016/s1085-5629(96)80047-2
Fleming C, Morrissey S, Cai Y, Yan J (2017) γδ T cells: unexpected regulators of cancer development and progression Trends Cancer 3:561–570. https://doi.org/10.1016/j.trecan.2017.06.003
Folkman J (2002) Role of angiogenesis in tumor growth and metastasis Semin Oncol 29:15–8 https://doi.org/10.1053/sonc.2002.37263
Hanahan D, Weinberg RA (2000) The hallmarks of cancer Cell 100:57–70. https://doi.org/10.1016/S0092-8674(00)81683-9
Hanahan D, Weinberg RA (2011) Hallmarks of cancer: the next generation Cell 144:646–674. https://doi.org/10.1016/j.cell.2011.02.013
Hansen S, Sørensen FB, Vach W, Grabau DA, Bak M, Rose C (2004) Microvessel density compared with the Chalkley count in a prognostic study of angiogenesis in breast cancer patients Histopathology 44:428–436. https://doi.org/10.1111/j.1365-2559.2004.01848.x
Hashizume H et al (2000) Openings between defective endothelial cells explain tumor vessel leakiness. Am J Pathol 156:1363–1380. https://doi.org/10.1016/s0002-9440(10)65006-7
Hollis CP, Weiss HL, Leggas M, Evers BM, Gemeinhart RA, Li T (2013) Biodistribution and bioimaging studies of hybrid paclitaxel nanocrystals: lessons learned of the EPR effect and image-guided drug delivery. J Control Release 172:12–21. https://doi.org/10.1016/j.jconrel.2013.06.039
Hori K, Suzuki M, Tanda S, Saito S, Shinozaki M, Zhang QH (1991) Fluctuations in tumor blood flow under normotension and the effect of angiotensin II-induced hypertension Jpn. J Cancer Res 82:1309–1316. https://doi.org/10.1111/j.1349-7006.1991.tb01797.x
Hori K, Saito S, Takahashi H, Sato H, Maeda H, Sato Y (2000) Tumor-selective blood flow decrease induced by an angiotensin converting enzyme inhibitor, temocapril hydrochloride Jpn J Cancer Res 91:261–269. https://doi.org/10.1111/j.1349-7006.2000.tb00940.x
Jain RK (2001) Delivery of molecular medicine to solid tumors: lessons from in vivo imaging of gene expression and function. J Control Release 74:7–25. https://doi.org/10.1016/s0168-3659(01)00306-6
Jain RK (2005) Normalization of tumor vasculature: an emerging concept in antiangiogenic therapy Science 307:58–62. https://doi.org/10.1126/science.1104819
Jain RK, Baxter LT (1988) Mechanisms of heterogeneous distribution of monoclonal antibodies and other macromolecules in tumors: significance of elevated interstitial pressure. Cancer Res 48:7022–7032
Jain RK, Stylianopoulos T (2010) Delivering nanomedicine to solid tumors. Nat Rev Clin Oncol 7:653–664. https://doi.org/10.1038/nrclinonc.2010.139
Kashani-Sabet M, Sagebiel RW, Ferreira CM, Nosrati M, Miller JR (2002) Tumor vascularity in the prognostic assessment of primary cutaneous melanoma. J Clin Oncol 20:1826–1831. https://doi.org/10.1200/JCO.2002.07.082
Kim R, Emi M, Tanabe K (2007) Cancer immunoediting from immune surveillance to immune escape Immunology 121:1–14. https://doi.org/10.1111/j.1365-2567.2007.02587.x
Kim JY et al (2009) The expression of VEGF receptor genes is concurrently influenced by epigenetic gene silencing of the genes and VEGF activation Epigenetics 4:313–321
Lammers T, Kiessling F, Hennink WE, Storm G (2012) Drug targeting to tumors: principles, pitfalls and (pre-) clinical progress. J Control Release 161:175–187. https://doi.org/10.1016/j.jconrel.2011.09.063
Matsumura Y, Maeda H (1986) A new concept for macromolecular therapeutics in cancer chemotherapy: mechanism of tumoritropic accumulation of proteins and the antitumor agent smancs. Cancer Res 46:6387–6392
McDonald DM, Thurston G, Baluk P (1999) Endothelial gaps as sites for plasma leakage in inflammation Microcirculation 6:7–22. https://doi.org/10.1080/713773924
Nagy JA, Chang SH, Dvorak AM, Dvorak HF (2009) Why are tumour blood vessels abnormal and why is it important to know? Br J Cancer 100:865–869. https://doi.org/10.1038/sj.bjc.6604929
Palazon A et al (2017) An HIF-1α/VEGF-A axis in cytotoxic T cells regulates tumor progression Cancer Cell 32:669–683.e665. https://doi.org/10.1016/j.ccell.2017.10.003
Pasquali S et al (2015) Lymphatic and blood vasculature in primary cutaneous melanomas of the scalp and neck. Head Neck 37:1596–1602. https://doi.org/10.1002/hed.23801
Simonetti O et al (2013) Microvessel density and VEGF, HIF-1α expression in primary oral melanoma: correlation with prognosis. Oral Dis 19:620–627. https://doi.org/10.1111/odi.12048
Stirland DL, Nichols JW, Miura S, Bae YH (2013) Mind the gap: a survey of how cancer drug carriers are susceptible to the gap between research and practice. J Control Release 172:1045–1064. https://doi.org/10.1016/j.jconrel.2013.09.026
Stylianopoulos T, Jain RK (2013) Combining two strategies to improve perfusion and drug delivery in solid tumors. Proc Natl Acad Sci U S A 110:18632–18637. https://doi.org/10.1073/pnas.1318415110
Stylianopoulos T, Jain RK (2015) Design considerations for nanotherapeutics in oncology Nanomedicine 11:1893–1907. https://doi.org/10.1016/j.nano.2015.07.015
Taniguchi M, Seino K, Nakayama T (2003) The NKT cell system: bridging innate and acquired immunity. Nat Immunol 4:1164–1165. https://doi.org/10.1038/ni1203-1164
Tuthill RJ, Reed RJ (2007) Failure of senescence in the dysplasia-melanoma sequence: demonstration using a tissue microarray and a revised paradigm for melanoma. Semin Oncol 34:467–475. https://doi.org/10.1053/j.seminoncol.2007.09.014
Vakoc BJ et al (2009) Three-dimensional microscopy of the tumor microenvironment in vivo using optical frequency domain imaging. Nat Med 15:1219–1223. https://doi.org/10.1038/nm.1971
Wahl ML et al (2002) Regulation of intracellular pH in human melanoma: potential therapeutic implications. Mol Cancer Ther 1:617–628
Acknowledgements
The authors thank the “service commun imagerie et analyse microscopique” and particularly Dr. Mabilleau and Dr. Perrot for their expertise. We are also grateful to Ms. Dumez and Ms. Viau for their technical support.
Funding
The authors thank the “comité départemental du Maine et Loire de la Ligue contre le Cancer” for its financial support for the realization of this project. Furthermore, the authors would like to thank the “Région Pays de la Loire” and the “Erasmus Mundus” program for the financing of the phD program of VP.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Pautu, V., Mellinger, A., Resnier, P. et al. Melanoma tumour vasculature heterogeneity: from mice models to human. J Cancer Res Clin Oncol 145, 589–597 (2019). https://doi.org/10.1007/s00432-018-2809-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-018-2809-z