Abstract
Purpose
This study aimed to investigate the prognostic value of different organs metastases in patients with non-small cell lung cancer (NSCLC) and its most common subtypes.
Methods
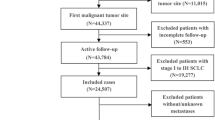
We identified 45,423 NSCLC cases (25,129 men and 20,294 women) between 2010 and 2013 with distant metastases, with complete clinical information obtained from the surveillance, epidemiology, and end results (SEER) database.
Results
Bone and liver were the most and the least common metastatic sites with rates of 37.1 and 16.8%, respectively. The mortality rates associated with bone, brain, liver, lung metastases, and multiorgan metastases (MOM) were 73.2, 72.7, 78.3, 65.4, and 77.5%, respectively. Kaplan–Meier analyses demonstrated that patients with MOM and liver metastasis had the worst survival. Compared with NSCLC cases with other organ metastasis, but without the four organs metastasis, hazard ratios (HRs) for lung, bone, brain, and liver metastases, and MOM were 0.906 (95% CI 0.866–0.947), 1.276 (95% CI 1.225–1.330), 1.318 (95% CI 1.260–1.379), 1.481 (95% CI 1.388–1.580), and 1.647 (95% CI 1.587–1.709), respectively. Similar results were obtained for adenocarcinoma (AD) cases.
Conclusions
The mortality risk is highest with MOM and liver metastasis followed by bone, brain, other organ, and lung metastases in NSCLC and AD which is the most common variant for NSCLC. These results will be helpful for pre-treatment evaluation regarding the prognosis of NSCLC patients.



Similar content being viewed by others
References
Bray F, Jemal A, Grey N, Ferlay J, Forman D (2012) Global cancer transitions according to the Human Development Index (2008–2030): a population-based study. Lancet Oncol 13:790–801. https://doi.org/10.1016/S1470-2045(12)70211-5
Brodowicz T, O’Byrne K, Manegold C (2012) Bone matters in lung cancer. Ann Oncol 23:2215–2222. https://doi.org/10.1093/annonc/mds009
Chang YP et al (2017) The impact of de novo liver metastasis on clinical outcome in patients with advanced non-small-cell lung cancer. PLoS ONE 12:e0178676. https://doi.org/10.1371/journal.pone.0178676
D’Antonio C et al (2014) Bone and brain metastasis in lung cancer: recent advances in therapeutic strategies. Ther Adv Med Oncol 6:101–114. https://doi.org/10.1177/1758834014521110
Detterbeck FC, Boffa DJ, Kim AW, Tanoue LT (2017) The eighth edition lung cancer stage classification. Chest 151:193–203. https://doi.org/10.1016/j.chest.2016.10.010
Eberhardt WE et al (2015) The IASLC lung cancer staging project: proposals for the revision of the M descriptors in the forthcoming eighth edition of the TNM classification of lung cancer. J Thorac Oncol 10:1515–1522. https://doi.org/10.1097/JTO.0000000000000673
Goldstraw P et al (2007) The IASLC Lung Cancer Staging Project: proposals for the revision of the TNM stage groupings in the forthcoming (seventh) edition of the TNM Classification of malignant tumours. J Thorac Oncol 2:706–714. https://doi.org/10.1097/JTO.0b013e31812f3c1a
Ichinose Y et al (2000) The prognosis of patients with non-small cell lung cancer found to have carcinomatous pleuritis at thoracotomy. Surg Today 30:1062–1066
Iida T et al (2015) Surgical intervention for non-small-cell lung cancer patients with pleural carcinomatosis: results from the Japanese Lung Cancer Registry in 2004. J Thorac Oncol 10:1076–1082. https://doi.org/10.1097/JTO.0000000000000554
Jett JR, Scott WJ, Rivera MP, Sause WT, American College of Chest P (2003) Guidelines on treatment of stage IIIB non-small cell lung cancer. Chest 123:221S–225S
Morgensztern D, Waqar S, Subramanian J, Gao F, Govindan R (2009) Improving survival for stage IV non-small cell lung cancer: a surveillance, epidemiology, and end results survey from 1990 to 2005. J Thorac Oncol 4:1524–1529. https://doi.org/10.1097/JTO.0b013e3181ba3634
Morgensztern D, Ng SH, Gao F, Govindan R (2010) Trends in stage distribution for patients with non-small cell lung cancer: a National Cancer Database survey. J Thorac Oncol 5:29–33. https://doi.org/10.1097/JTO.0b013e3181c5920c
Nakazawa K, Kurishima K, Tamura T, Kagohashi K, Ishikawa H, Satoh H, Hizawa N (2012) Specific organ metastases and survival in small cell lung cancer. Oncol Lett 4:617–620. https://doi.org/10.3892/ol.2012.792
Ohta Y, Shimizu Y, Matsumoto I, Tamura M, Oda M, Watanabe G (2005) Retrospective review of lung cancer patients with pleural dissemination after limited operations combined with parietal pleurectomy. J Surg Oncol 91:237–242. https://doi.org/10.1002/jso.20333
Rami-Porta R, Asamura H, Travis WD, Rusch VW (2017) Lung cancer—major changes in the American Joint Committee on Cancer eighth edition cancer staging manual. CA Cancer J Clin 67:138–155. https://doi.org/10.3322/caac.21390
Ren Y et al (2016) Prognostic effect of liver metastasis in lung cancer patients with distant metastasis. Oncotarget 7:53245–53253. https://doi.org/10.18632/oncotarget.10644
Riihimaki M, Hemminki A, Fallah M, Thomsen H, Sundquist K, Sundquist J, Hemminki K (2014) Metastatic sites and survival in lung cancer. Lung Cancer 86:78–84. https://doi.org/10.1016/j.lungcan.2014.07.020
Sanchez de Cos Escuin J et al (2014) Tumor, node and metastasis classification of lung cancer—M1a versus M1b—analysis of M descriptors and other prognostic factors. Lung Cancer 84:182–189. https://doi.org/10.1016/j.lungcan.2014.02.006
Siegel RL, Miller KD, Jemal A (2017) Cancer statistics, 2017. CA Cancer J Clin 67:7–30. https://doi.org/10.3322/caac.21387
Sugiura S, Ando Y, Minami H, Ando M, Sakai S, Shimokata K (1997) Prognostic value of pleural effusion in patients with non-small cell lung cancer. Clin Cancer Res 3:47–50
Sugiura H, Yamada K, Sugiura T, Hida T, Mitsudomi T (2008) Predictors of survival in patients with bone metastasis of lung cancer. Clin Orthop Relat Res 466:729–736. https://doi.org/10.1007/s11999-007-0051-0
Tamura T, Kurishima K, Nakazawa K, Kagohashi K, Ishikawa H, Satoh H, Hizawa N (2015) Specific organ metastases and survival in metastatic non-small-cell lung cancer. Mol Clin Oncol 3:217–221. https://doi.org/10.3892/mco.2014.410
Waqar SN et al (2015) Brain metastases at presentation in patients with non-small cell lung cancer. Am J Clin Oncol 41(1):36–40. https://doi.org/10.1097/COC.0000000000000230
Acknowledgements
We would like to thank all the staff of National Cancer Institute for their efforts toward the SEER program.
Funding
This work was supported by National Natural Science Foundation of China, No. 81600052 (J.Y.) and 81500052 (Y.Z.). This work was also supported by Shanghai Tenth Hospital’s improvement plan for National Natural Science Foundation of China, No. SYGZRPY (Y.H.).
Author information
Authors and Affiliations
Contributions
Conception and design: Y.H., J.Y., and G.J.; acquisition, statistical analysis or interpretation of the data: all authors; drafting of the manuscript: Y.H., J.Y., Y.Z. and X.S.; all authors reviewed and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors disclose no potential conflicts of interest related to this study.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study formal consent is waived.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yang, J., Zhang, Y., Sun, X. et al. The prognostic value of multiorgan metastases in patients with non-small cell lung cancer and its variants: a SEER-based study. J Cancer Res Clin Oncol 144, 1835–1842 (2018). https://doi.org/10.1007/s00432-018-2702-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-018-2702-9