Abstract
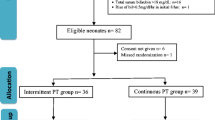
Phototherapy (PT) is a widely used treatment for neonatal jaundice, yet the ideal model of application remains controversial. In this study, the effects of continuous phototherapy (CPT) and intermittent phototherapy (IPT) models were compared in the treatment of neonatal indirect hyperbilirubinemia (IHB) and whether IPT is a superior modality is investigated. Single-centre parallel randomized controlled open label trial. A computer-based table of random numbers was used to allocate treatments. Newborns ≥ 34 weeks’ gestation who received phototherapy in our neonatal intensive care unit (NICU) between July 2022 and April 2023 were included. CPT was applied continuously for 6 h, and IPT was applied as 2 cycles of 1 h on and 2 h off in a 6-h session. Rebound TSB was measured 8 h after phototherapy was stopped in both groups. Phototherapy duration, TSB reduction rate and rebound bilirubin rate were compared between intervention groups. One hundered and four neonates met the inclusion criteria during the study period. CPT and IPT were each used in 52 newborns. Demographic characteristics of the study groups, including sex, mode of delivery, birth weight, admission weight, age at postnatal presentation, diet, discharge weight, and history of PT in siblings, were similar (p > 0.05). The most common cause of IHB in both groups was ABO incompatibility. The median phototherapy time was 12 h (6–15) in the CPT group and 4 h (2–4) in the IPT group (p < 0.001). The mean rate of bilirubin decrease was 1.12 ± 0.73 mg/dl/h in those who underwent IPT and 0.51 ± 0.33 mg/dl/h in those who underwent CPT (p < 0.001). The mean rebound bilirubin rate 8 h after phototherapy was 0.08 ± 0.28 mg/dl/h in the CPT group, and −0.01 ± 0.17 mg/dl/h in the IPT group (p = 0.039). The length of hospital stay was longer in the CPT group (p = 0.032). Skin rash, diarrhoea and increased body temperature were less frequent in the IPT group (p < 0.001).
Conclusions: In this study, IPT was found to be at least as effective as CPT in reducing total serum bilirubin. Even though the duration of PT is shorter in IPT, the slower rate of rebound bilirubin, shorter hospital stays and lower incidence of side effects indicated that intermittent phototherapy is superior to continuous phototherapy. Choosing IPT over CPT is a more rational approach in neonatal jaundice.
ClinicalTrials.gov Identifier: NCT 06386731 (registered retrospectively on 23/04/2024)
What is Known: • PT is common used in the treatment of neonatal jaundice. • There is no standard model of application for PT. |
What is New: • The IPT model is as effective as CPT. • Newborns are discharged faster with IPT. |

Similar content being viewed by others
Data availability
No datasets were generated or analyzed during the current study.
Abbreviations
- CPT:
-
Continuous phototherapy
- IHB:
-
Indirect hyperbilirubinemia
- IPT:
-
Intermittent phototherapy
- i Ca:
-
Ionized calcium
- NICU:
-
Neonatal intensive care unit
- LED:
-
Light emitting diode
- PT:
-
Phototherapy
- STB:
-
Serum total bilirubin
References
Battersby C, Michaelides S, Upton M, Rennie JM, Jaundice Working Group of the Atain (2017) (Avoiding term admissions into neonatal units) programme, led by the patient safety term admissions to neonatal units in England: a role for transitional care? A retrospective cohort study. BMJ Open 7(5):e016050. https://doi.org/10.1136/bmjopen-2017-016050
Mreihil K, Benth JŠ, Stensvold HJ, Nakstad B, Hansen TWR, Norwegian NICU, Phototherapy Study Group, & Norwegian Neonatal Network (2018) Phototherapy is commonly used for neonatal jaundice but greater control is needed to avoid toxicity in the most vulnerable infants. Acta Paediatr 107(4):611–619. https://doi.org/10.1111/apa
Geiger AM, Petitti DB, Yao JF (2001) Rehospitalisation for neonatal jaundice: risk factors and outcomes. Paediatr Perinat Epidemiol 15(4):352–358. https://doi.org/10.1046/j.1365-3016.2001.00374.x
Amsalu R, Oltman SP, Baer RJ, Medvedev MM, Rogers EE, Jelliffe-Pawlowski L (2022) Incidence, risk factors, and reasons for 30-Day hospital readmission among healthy late preterm infants. Hosp Pediatr 12(7):639–649. https://doi.org/10.1542/hpeds.2021-006215
Hansen TW (2001) Bilirubin brain toxicity. J Perinatol Off J Calif Perinat Assoc 21(Suppl 1):S48–S62. https://doi.org/10.1038/sj.jp.7210634
Bhutani VK, Wong R (2015) Bilirubin-induced neurologic dysfunction (BIND). Semin Fetal Neonatal Med 20(1):1. https://doi.org/10.1016/j.siny.2014.12.010
Kasirer Y, Kaplan M, Hammerman C (2023) Kernicterus on the spectrum. NeoReviews 24(6):e329–e342. https://doi.org/10.1542/neo.24-6-e329
Slusher TM, Zipursky A, Bhutani VK (2011) A global need for affordable neonatal jaundice technologies. Semin Perinatol 35(3):185–191. https://doi.org/10.1053/j.semperi.2011.02.014
Kaplan M, Bromiker R, Hammerman C (2011) Severe neonatal hyperbilirubinemia and kernicterus: are these still problems in the third millennium? Neonatology 100(4):354–362. https://doi.org/10.1159/000330055
Vidavalur R, Devapatla S (2022) Trends in hospitalizations of newborns with hyperbilirubinemia and kernicterus in United States: an epidemiological study. J Maternal-Fetal Neonatal Med Off J Eur Assoc Perinat Med Fed Asia Oceania Perinat Soc Int Soc Perinat Obstet 35(25):7701–7706. https://doi.org/10.1080/14767058.2021.1960970
Maisels MJ, McDonagh AF (2008) Phototherapy for neonatal jaundice. N Engl J Med 358(9):920–928. https://doi.org/10.1056/NEJMct0708376
Stoll J B, Kliegman M R (2000) Nelson Textbook of pediatrics. In: Behrman ER (ed) Jaundice and Hyperbilirubinemia in the Newborn, 16rd edn. W.B. Saunders Company, Philadelphia, pp 513–519
Madan A (2005) Phototherapy: old questions, new answers. Acta Paediatr 94(10):1360–1362. https://doi.org/10.1111/j.1651-2227.2005.tb01804.x
Hansen TWR, Maisels MJ, Ebbesen F, Vreman HJ, Stevenson DK, Wong RJ, Bhutani VK (2020) Sixty years of phototherapy for neonatal jaundice - from serendipitous observation to standardized treatment and rescue for millions. J Perinatol Off J Calif Perinat Assoc 40(2):180–193. https://doi.org/10.1038/s41372-019-0439-1
Faulhaber FRS, Procianoy RS, Silveira RC (2019) Side effects of phototherapy on neonates. Am J Perinatol 36(3):252–257. https://doi.org/10.1055/s-0038-1667379
Hansen TW (2012) Let there be light-but should there be less? J Perinatol J Perinatol Off J Calif Perinat Assoc 32(9):649–651. https://doi.org/10.1038/jp.2012.80
Maisels MJ (2018) Phototherapy in the neonatal intensive care unit - quantity and quality. Acta Paediatr (Oslo, Norway: 1992) 107(4):551–553. https://doi.org/10.1111/apa.14241
Shoris I, Gover A, Toropine A, Iofe A, Zoabi-Safadi R, Tsuprun S, Riskin A (2023) Light on phototherapy-complications and strategies for shortening its duration, a review of the literature. Child (Basel Switzerland) 10(10):1699. https://doi.org/10.3390/children10101699
Brown AK, McDonagh AF (1980) Phototherapy for neonatal hyperbilirubinemia: efficacy, mechanism and toxicity. Adv Pediatr 27:341–389 PMID: 7194571
Mreihil K, McDonagh AF, Nakstad B, Hansen TW (2010) Early isomerization of bilirubin in phototherapy of neonatal jaundice. Pediatr Res 67(6):656–659. https://doi.org/10.1203/PDR.0b013e3181dcedc0
American Academy of Pediatrics Subcommittee on Hyperbilirubinemia (2004) Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics 114(1):297–316. https://doi.org/10.1542/peds.114.1.297
Gutta S, Shenoy J, Kamath SP, Mithra P, Baliga BS, Sarpangala M, Srinivasan M (2019) Light emitting diode (LED) phototherapy versus conventional phototherapy in neonatal hyperbilirubinemia: a single blinded randomized control trial from coastal India. BioMed Res Int 2019:6274719. https://doi.org/10.1155/2019/6274719
Sachdeva M, Murki S, Oleti TP, Kandraju H (2015) Intermittent versus continuous phototherapy for the treatment of neonatal non-hemolytic moderate hyperbilirubinemia in infants more than 34 weeks of gestational age: a randomized controlled trial. Eur J Pediatr 174(2):177–181. https://doi.org/10.1007/s00431-014-2373-8
Zhou S, Wu X, Ma A, Zhang M, Liu Y (2019) Analysis of therapeutic effect of intermittent and continuous phototherapy on neonatal hemolytic jaundice. Exp Ther Med 17(5):4007–4012. https://doi.org/10.3892/etm.2019.7432
Sharma P, Mukthapuram S (2023) What is the minimum duration of cycled phototherapy that is still effective in treating hyperbilirubinemia? J Perinatol Off J Calif Perinat Assoc 43(11):1449–1451. https://doi.org/10.1038/s41372-023-01759-5
Chu L, Xue X, Qiao J (2021) Efficacy of intermittent phototherapy versus continuous phototherapy for treatment of neonatal hyperbilirubinaemia: a systematic review and meta-analysis. J Adv Nurs 77(1):12–22. https://doi.org/10.1111/jan.14535
Gottimukkala SB, Sethuraman G, Kitchanan S, Pathak S (2021) Comparison of efficacy, safety & satisfaction of intermittent versus continuous phototherapy in hyperbilirubinaemic newborns ≥ 35 week gestation: a randomized controlled trial. Indian J Med Res 153(4):446–452. https://doi.org/10.4103/ijmr.IJMR_2156_18
Gottimukkala SB, Lobo L, Gautham KS, Bolisetty S, Fiander M, Schindler T (2023) Intermittent phototherapy versus continuous phototherapy for neonatal jaundice. Cochrane Database Syst Rev 3(3):CD008168. https://doi.org/10.1002/14651858.CD008168.pub2
Hooman N, Honarpisheh A (2005) The effect of phototherapy on urinary calcium excretion in newborns. Pediatr Nephrol (Berlin Germany) 20(9):1363–1364. https://doi.org/10.1007/s00467-005-1951-4
Hakanson DO, Penny R, Bergstrom WH (1987) Calcemic responses to photic and pharmacologic manipulation of serum melatonin. Pediatr Res 22(4):414–416. https://doi.org/10.1203/00006450-198710000-00010
Karamifar H, Pishva N, Amirhakimi GH (2002) Prevalence of phototherapy-induced hypocalcemia. Iran J Med Sci 27(4):166–8
Wang J, Guo G, Li A, Cai WQ, Wang X (2021) Challenges of phototherapy for neonatal hyperbilirubinemia (review). Exp Ther Med 21(3):231. https://doi.org/10.3892/etm.2021.9662
Kumar P, Chawla D, Deorari A (2011) Light-emitting diode phototherapy for unconjugated hyperbilirubinaemia in neonates. Cochrane Database Syst Rev (12):CD007969. https://doi.org/10.1002/14651858.CD007969.pub2
Aydemir O, Soysaldı E, Kale Y, Kavurt S, Bas AY, Demirel N (2014) Body temperature changes of newborns under fluorescent versus LED phototherapy. Indian J Pediatr 81(8):751–754. https://doi.org/10.1007/s12098-013-1209-2
Kurt A, Aygun AD, Kurt AN, Godekmerdan A, Akarsu S, Yilmaz E (2009) Use of phototherapy for neonatal hyperbilirubinemia affects cytokine production and lymphocyte subsets. Neonatology 95(3):262–266. https://doi.org/10.1159/000171216
Xiong T, Qu Y, Cambier S, Mu D (2011) The side effects of phototherapy for neonatal jaundice: what do we know? What should we do? Eur J Pediatr 170(10):1247–1255. https://doi.org/10.1007/s00431-011-1454-1
Zecca E, Barone G, De Luca D, Marra R, Tiberi E, Romagnoli C (2009) Skin bilirubin measurement during phototherapy in preterm and term newborn infants. Early Hum Dev 85(8):537–540. https://doi.org/10.1016/j.earlhumdev.2009.05.010
De Luca D, Zecca E, de Turris P, Barbato G, Marras M, Romagnoli C (2007) Using BiliCheck for preterm neonates in a sub-intensive unit: diagnostic usefulness and suitability. Early Hum Dev 83(5):313–317. https://doi.org/10.1016/j.earlhumdev.2006.06.006
De Luca D, Dell’Orto V (2017) Patched skin bilirubin assay to monitor neonates born extremely preterm undergoing phototherapy. J Pediatr 188:122–127. https://doi.org/10.1016/j.jpeds.2017.05.080
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
H N. D. and S S. O. prepared the materials and collected the data. S S. O. and H F. O. analyzed the data, interpreted them and created figures. H N. D. and S S.O. wrote the first draft of the article. H F. O. made criticisms. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the local ethics board in concordance with the Declaration of Helsinki. Ethics committee approval was obtained from the Istanbul Medeniyet University Göztepe Training and Research Hospital Clinical Research Ethics Committee dated 15 June 2022 (decision number 2022/0387).
Consent to participate
Written informed consent was obtained from the parents of newborns.
Competing interests
The authors declare no competing interests.
Additional information
Communicated by Daniele De Luca
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Demirel, H.N., Ozumut, S.S. & Ovalı, H.F. Continuous versus intermittent phototherapy in treatment of neonatal jaundice: a randomized controlled trial. Eur J Pediatr (2024). https://doi.org/10.1007/s00431-024-05610-7
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00431-024-05610-7