Abstract
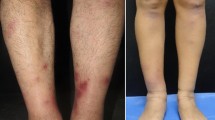
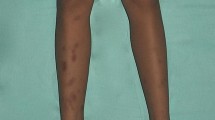
Erythema nodosum (EN), although relatively uncommon in the pediatric population, is the most frequent type of panniculitis in children. The present study aimed to report all the cases of children admitted to our tertiary pediatric hospital with the diagnosis of EN to evaluate the epidemiology, clinical manifestations, etiology, treatment, and the course of this disease in the pediatric age. This observational study retrospectively considered all children evaluated to the emergency room (ER) of Meyer Children’s University Hospital, Florence, Italy, discharged with a diagnosis of EN over a 12-year period (from January 2009 to December 2021). Clinical and laboratory data were recorded using a standardized report form. Sixty-eight patients with EN were included. The etiologic diagnosis of EN was made in 38 children (55.9%): 29 (42.6%) had infection-related EN (in particular EBV and β-hemolytic streptococcus), 6 (8.8%) had Crohn’s disease, 1 celiac disease, 1 Sjogren syndrome, and 1 Hodgkin lymphoma. In 30 patients (45%), no definitive diagnosis was reached, and they were defined as having idiopathic EN. Most of the laboratory tests were nonspecific. No statistical differences were found in the demographic and clinical data, and the main diagnostic laboratory parameters between patients with idiopathic EN versus those with secondary EN.
Conclusion: Since EN can be isolated or the first manifestation of heterogeneous underlying pathologies, some of which can be severe and life-threatening, it is important to recognize it and carry out all the necessary etiological diagnostic investigations to understand its etiology and start the specific treatment.
What is Known: |
• Erythema nodosum (EN) is the most frequent type of panniculitis in children. |
• It has been associated with a wide spectrum of disorders, such as different types of infection, malignancies, chronic inflammations, and drugs. |
What is New: |
• No statistical differences can be found in clinical features as well as laboratory data, between patients with idiopathic EN versus those with secondary EN. |
• A broad spectrum of investigations and a proper follow-up should be taken into account in order to prevent a delayed or missed secondary EN diagnosis. |

Similar content being viewed by others
Availability of data and material
Materials described in the manuscript, including all relevant raw data, will be freely available to any researcher and reader.
Change history
02 March 2024
A Correction to this paper has been published: https://doi.org/10.1007/s00431-024-05452-3
Abbreviations
- ANA:
-
Antinuclear antibodies
- ANCA:
-
Anti-neutrophil cytoplasmic antibodies
- ASCA:
-
Anti-Saccharomyces cerevisiae antibodies
- ASO:
-
Anti-streptolysin O
- CBC:
-
Complete blood cell count
- CD:
-
Crohn’s disease
- CRP:
-
C-reactive protein
- EBV:
-
Epstein-Barr virus
- EN:
-
Erythema nodosum
- ESR:
-
Erythrocyte sedimentation rate
- IBD:
-
Inflammatory bowel disease
- IQR:
-
Interquartile range
- NSAIDs:
-
Nonsteroidal anti-inflammatories
- PCR:
-
Polymerase chain reaction
- pSS:
-
Pediatric Sjogren syndrome
- QuantiFERON test:
-
Interferon-gamma release test
- SD:
-
Standard deviation
- SS:
-
Sjogren syndrome
References
Garty BZ, Poznanski O (2014) Erythema nodosum in Israeli children. Isr Med Assoc J 2:145–146
Blake T, Manahan M, Rodins K (2014) Erythema nodosum – a review of an uncommon panniculitis. Dermatol Online J 20:22376
Calista D, Schianchi S, Morri M (2001) Erythema nodosum induced by kerion celsi of the scalp. Pediatr Dermatol 18:114–116. https://doi.org/10.1046/j.1525-1470.2001.018002114.x
Hassink RI, Pasquinelli-Egli CE, Jacomella V, Laux-End R, Bianchetti MG (1997) Conditions currently associated with erythema nodosum in Swiss children. Eur J Pediatr 156:851–853. https://doi.org/10.1007/s004310050728
Trapani S, Rubino C, Lodi L, Resti M, Indolfi G (2022) Erythema nodosum in children: a narrative review and a practical approach. Children 9:511. https://doi.org/10.3390/children9040511
Porges T, Shafat T, Sagy I et al (2018) Clinical, epidemiological, and etiological changes in erythema nodosum. Isr Med Assoc J 20:770–772
Mana J, Marcoval J (2007) Erythema nodosum. Clin Dermat 25:288–294. https://doi.org/10.1016/j.clindermatol.2007.03.006
Arnold J, Leung AKC, Lam JM (2020) Violaceous tender nodules symmetrically distributed over the pretibial area. Paediatr Child Health 25:201–202. https://doi.org/10.1093/pch/pxz030
Litwin L, Machura E (2014) The etiology and clinical manifestation of erythema nodosum in hospitalized children – analysis of 12 cases. Preliminary report Dev Period Med 18:506–512
Polcari IC, Stein SL (2010) Panniculitis in childhood. Dermatol Ther 23:356–367. https://doi.org/10.1111/j.1529-8019.2010.01336.x
Labbe L, Perel Y, Maleville J, Taieb A (1996) Erythema nodosum in children: a study of 27 patients. Pediatr Dermatol 13:447–450. https://doi.org/10.1111/j.1525-1470.1996.tb00722.x
Picco P, Gattorno M, Vignola S et al (1999) Clinical and biological characteristics of immunopathological disease-related erythema nodosum in children. Scand J Rheumatol 28:27–32
Bartyik K, Varkonyi A, Kirschner A, Endreffy E, Turi S, King E (2004) Erythema nodosum in association with celiac disease. Pediatr Dermatol 21:227–230. https://doi.org/10.1111/j.0736-8046.2004.21307.x
Leung AKC, Leong KF, Lam JM (2018) Erythema nodosum. World J Pediatr 14:548–554. https://doi.org/10.1007/s12519-018-0191-1
Kakourou T, Drosatou P, Psychou F, Aroni K, Nicolaidou P (2001) Erythema nodosum in children: a prospective study. J Am Acad Dermatol 44:17–21. https://doi.org/10.1067/mjd.2001.110877
Wallis P, Starr M, Phillips RJ (2016) An uncommon cause of erythema nodosum. J Paediatr Child Health 52:961–963. https://doi.org/10.1111/jpc.13267
Schwartz RA, Nervi SJ (2007) Erythema nodosum: a sign of systemic disease. Am Fam Physician 75:695–700
Aydin-Teke T, Tanir G, Bayhan GI, Metin O, Oz N (2014) Erythema nodosum in children: evaluation of 39 patients. Turk J Pediatr 56:144–149
Mert A, Kumbasar H, Ozaras R et al (2007) Erythema nodosum: an evaluation of 100 cases. Clin Exp Rheumatol 25:563–570
Lins K, Drummond M, Velho PE (2019) Cutaneous manifestations of bartonellosis. An Bras Dermatol 94:594–602. https://doi.org/10.1016/j.abd.2019.09.024
Carithers HA (1985) Cat-scratch disease. an overview based on a study of 1,200 patients. Am J Dis Child 139:1124–1133. https://doi.org/10.1001/archpedi.1985.02140130062031
Laborada J, Cohen PR (2021) Tuberculosis-associated erythema nodosum. Cureus 13:e20184. https://doi.org/10.7759/cureus.20184
Mantadakis E, Arvanitidou V, Tsalkidis A, Thomaidis S, Chatzimichael A (2010) Erythema nodosum associated with Salmonella enteritidis. Hippokratia 14:51–53
Su CG, Judge TA, Lichtenstein GR (2002) Extraintestinal manifestations of inflammatory bowel disease. Gastroenterol Clin North Am 31:307–327. https://doi.org/10.1016/s0889-8553(01)00019-x
He S, Zhen X, Hu Y (2021) Juvenile primary Sjogren’s syndrome with cutaneous involvement. Clin Rheumatol 40:3687–3694. https://doi.org/10.1007/s10067-021-05656-0
Bonci A, Di Lernia V, Merli F, Lo Scocco G (2001) Erythema nodosum and Hodgkin’s disease. Clin Exp Dermatol 26:408–411. https://doi.org/10.1046/j.1365-2230.2001.00847.x
La Spina M, Russo G (2007) Presentation of childhood acute myeloid leukemia with erythema nodosum. J Clin Oncol 25:4011–4012. https://doi.org/10.1200/JCO.2007.12.0022
Lin JT, Chen PM, Huang DF, Kwang WK, Lo K, Wang WS (2004) Erythema nodosum associated with carcinoid tumour. Clin Exp Dermatol 29:426–427. https://doi.org/10.1111/j.1365-2230.2004.01544.x
Perez NB, Bernad B, Narváez J, Valverde J (2006) Erythema nodosum and lung cancer. Joint Bone Spine 73:336–337. https://doi.org/10.1016/j.jbspin.2005.10.009
Alvarez-Lario B, Piney E, Rodriguez-Valverde V, Pena-Sagredo JL, Peiro-Callizo E (1987) Erythema nodosum: study of 103 cases. Med Clin (Barc) 88:5–8
Author information
Authors and Affiliations
Contributions
S.A.R and F.B made substantial contributions to conception and acquisition of data and wrote the main manuscript text. G.I. revised it critically for important intellectual content. S.T. made contribution on design and final approbation. All authors approved the final manuscript as submitted and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. As the study has an observational retrospective design, for this type of study, formal consent was not required.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Communicated by Peter de Winter.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Abu-Rumeileh, S., Barbati, F., Indolfi, G. et al. Erythema nodosum in children: a cohort study from a tertiary pediatric hospital in Italy. Eur J Pediatr 182, 1803–1810 (2023). https://doi.org/10.1007/s00431-023-04872-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-023-04872-x