Abstract
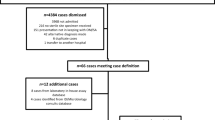
Diagnostic tools for the management of acute osteomyelitis (OM) and septic arthritis (SA) have improved over the last decade. To investigate the influence and availability of magnetic resonance imaging (MRI) and nucleic acid testing (NAT), a retrospective cohort study was done. Patients admitted with acute OM or SA between 2005 and 2014 were identified using ICD-10 discharge codes. Ninety-six children were identified: OM, n = 45; SA, n = 42; and OM + SA, n = 9. Diagnostic imaging was performed in 100% of OM or OM + SA and 95% of SA patients. MRI was performed in 85% of OM patients, 26% of SA patients and 100% OM + SA patients. In patients with OM or SA, concomitant joint/bone involvement was detected in 24 and 36% of patients, respectively. In 58% of patients, a pathogen was detected (Staphylococcus aureus, Streptococcus pyogenes and Streptococcus pneumoniae being most common). Blood and tissue culture were positive in 41 and 86% for OM patients and in 14 and 41%, respectively, for SA patients. In 42% of patients, no pathogen was identified, of which 40% had no material for blood or tissue culture/NAT taken.
Conclusion: Optimal use of imaging modalities including MRI and systematic pathogen detection including NAT should be advocated to limit use of broad spectrum antibiotics and treatment duration.
What is Known: • Magnetic resonance imaging and sonography have the best sensitivity for detection of acute osteomyelitis and septic arthritis in children. • Systematic use of blood cultures, tissue cultures and nucleic acid testing improves pathogen detection in children with acute osteomyelitis and septic arthritis. | |
What is New: • The added value of imaging modalities other than magnetic resonance and sonography for detection of osteomyelitis and septic arthritis is limited, and their routine use should be questioned. • Despite availability of optimal pathogen detection methods, missed opportunities to improve pathogen detection are frequent. |



Similar content being viewed by others
Abbreviations
- CRP:
-
C-reactive protein
- ESR:
-
Erythrocyte sedimentation rate
- Hib:
-
H. influenzae serotype b
- ICD:
-
International Classification of Diseases
- MRI:
-
Magnetic resonance imaging
- NAT:
-
Nucleic acid testing
- OM:
-
Osteomyelitis
- OM + SA:
-
Osteomyelitis and septic arthritis
- SA:
-
Septic arthritis
- WBC:
-
White blood count
References
Arnold SR, Elias D, Buckingham SC, Thomas ED, Novais E, Arkader A, Howard C (2006) Changing patterns of acute hematogenous osteomyelitis and septic arthritis: emergence of community-associated methicillin-resistant Staphylococcus aureus. J Pediatr Orthop 26:703–708
Bonhoeffer J, Haeberle B, Schaad UB, Heininger U (2001) Diagnosis of acute haematogenous osteomyelitis and septic arthritis: 20 years experience at the University Children’s Hospital Basel. Swiss Med Wkly 131:575–581
Brischetto A, Leung G, Marshall CS, Bowen AC (2016) A retrospective case-series of children with bone and joint infection from northern Australia. Medicine 95:e2885
Calvo C, Nunez E, Camacho M, Clemente D, Fernandez-Cooke E, Alcobendas R, Mayol L, Soler-Palacin P, Oscoz M, Saavedra-Lozano J (2016) Epidemiology and management of acute, uncomplicated septic arthritis and osteomyelitis: Spanish multicenter study. Pediatr Infect Dis J 35:1288–1293
Calvo C, Nunez E, Camacho M, Clemente D, Fernandez-Cooke E, Alcobendas R, Mayol L, Soler P, Oscoz M, Saavedra-Lozano J (2016) Epidemiology and management of acute uncomplicated septic arthritis and osteomyelitis, Spanish Multicenter Study. Pediatr Infect Dis J
Carter K, Doern C, Jo CH, Copley LA (2016) The clinical usefulness of polymerase chain reaction as a supplemental diagnostic tool in the evaluation and the treatment of children with septic arthritis. J Pediatr Orthop 36:167–172
Ceroni D, Cherkaoui A, Ferey S, Kaelin A, Schrenzel J (2010) Kingella kingae osteoarticular infections in young children: clinical features and contribution of a new specific real-time PCR assay to the diagnosis. J Pediatr Orthop 30:301–304
Ceroni D, Dubois-Ferriere V, Anderson R, Combescure C, Lamah L, Cherkaoui A, Schrenzel J (2012) Small risk of osteoarticular infections in children with asymptomatic oropharyngeal carriage of Kingella kingae. Pediatr Infect Dis J 31:983–985
Ceroni D, Kampouroglou G, Valaikaite R, Anderson della Llana R, Salvo D (2014) Osteoarticular infections in young children: what has changed over the last years? Swiss Med Wkly 144:w13971
Chiappini E, Camposampiero C, Lazzeri S, Indolfi G, De Martino M, Galli L (2017) Epidemiology and management of acute haematogenous osteomyelitis in a tertiary paediatric center. Int J Environ Res Public Health 14
Chometon S, Benito Y, Chaker M, Boisset S, Ploton C, Berard J, Vandenesch F, Freydiere AM (2007) Specific real-time polymerase chain reaction places Kingella kingae as the most common cause of osteoarticular infections in young children. Pediatr Infect Dis J 26:377–381
Gafur OA, Copley LA, Hollmig ST, Browne RH, Thornton LA, Crawford SE (2008) The impact of the current epidemiology of pediatric musculoskeletal infection on evaluation and treatment guidelines. J Pediatr Orthop 28:777–785
Gesundheit Bf (2013) Invasive H. influenzae. Erkrankungen 1988–2011
Ilharreborde B, Bidet P, Lorrot M, Even J, Mariani-Kurkdjian P, Liguori S, Vitoux C, Lefevre Y, Doit C, Fitoussi F, Pennecot G, Bingen E, Mazda K, Bonacorsi S (2009) New real-time PCR-based method for Kingella kingae DNA detection: application to samples collected from 89 children with acute arthritis. J Clin Microbiol 47:1837–1841
Islam G, Tomlinson J, Darton T, Townsend R (2013) Bone and joint infections. Surgery (Oxford) 31:187–192
Kaplan SL (2014) Recent lessons for the management of bone and joint infections. J Infect 68(Supplement 1):S51–S56
Lyon RM, Evanich JD (1999) Culture-negative septic arthritis in children. J Pediatr Orthop 19:655–659
Monsalve J, Kan JH, Schallert EK, Bisset GS, Zhang W, Rosenfeld SB (2015) Septic arthritis in children: frequency of coexisting unsuspected osteomyelitis and implications on imaging work-up and management. AJR Am J Roentgenol 204:1289–1295
Morel AS, Dubourg G, Prudent E, Edouard S, Gouriet F, Casalta JP, Fenollar F, Fournier PE, Drancourt M, Raoult D (2015) Complementarity between targeted real-time specific PCR and conventional broad-range 16S rDNA PCR in the syndrome-driven diagnosis of infectious diseases. Eur J Clin Microbiol Infect Dis : Off Publ Eur Soc Clin Microbiol 34:561–570
Ogden JA (1979) Pediatric osteomyelitis and septic arthritis: the pathology of neonatal disease. Yale J Biol Med 52:423–448
Peltola H, Paakkonen M, Kallio P, Kallio MJ (2009) Prospective, randomized trial of 10 days versus 30 days of antimicrobial treatment, including a short-term course of parenteral therapy, for childhood septic arthritis. Clin Infect Dis : Off Publ Infect Dis Soc Am 48:1201–1210
Peltola H, Paakkonen M, Kallio P, Kallio MJ (2010) Short- versus long-term antimicrobial treatment for acute hematogenous osteomyelitis of childhood: prospective, randomized trial on 131 culture-positive cases. Pediatr Infect Dis J 29:1123–1128
Peltola H, Paakkonen M (2014) Acute osteomyelitis in children. N Engl J Med 370:352–360
Perlman MH, Patzakis MJ, Kumar PJ, Holtom P (2000) The incidence of joint involvement with adjacent osteomyelitis in pediatric patients. J Pediatr Orthop 20:40–43
Riise OR, Handeland KS, Cvancarova M, Wathne KO, Nakstad B, Abrahamsen TG, Kirkhus E, Flato B (2008) Incidence and characteristics of arthritis in Norwegian children: a population-based study. Pediatrics 121:e299–e306
Riise OR, Kirkhus E, Handeland KS, Flato B, Reiseter T, Cvancarova M, Nakstad B, Wathne KO (2008) Childhood osteomyelitis—incidence and differentiation from other acute onset musculoskeletal features in a population-based study. BMC Pediatr 8:45
Saavedra-Lozano J, Falup-Pecurariu O, Faust SN, Girschick H, Hartwig N, Kaplan S, Lorrot M, Mantadakis E, Peltola H, Rojo P, Zaoutis T, LeMair A (2017) Bone and joint infections. Pediatr Infect Dis J 36:788–799
Schallert EK, Kan JH, Monsalve J, Zhang W, Bisset GS 3rd, Rosenfeld S (2015) Metaphyseal osteomyelitis in children: how often does MRI-documented joint effusion or epiphyseal extension of edema indicate coexisting septic arthritis? Pediatr Radiol 45:1174–1181
Section J, Gibbons SD, Barton T, Greenberg DE, Jo CH, Copley LA (2015) Microbiological culture methods for pediatric musculoskeletal infection: a guideline for optimal use. J Bone Joint Surg Am 97:441–449
Weichert S, Sharland M, Clarke NM, Faust SN (2008) Acute haematogenous osteomyelitis in children: is there any evidence for how long we should treat? Curr Opin Infect Dis 21:258–262
Yagupsky P (2004) Kingella kingae: from medical rarity to an emerging paediatric pathogen. Lancet Infect Dis 4:358–367
Yagupsky P, Porsch E, St Geme JW 3rd (2011) Kingella kingae: an emerging pathogen in young children. Pediatrics 127:557–565
Author information
Authors and Affiliations
Contributions
Nora Manz carried out the data analysis, drafted the initial manuscript and approved the final manuscript as submitted. Andreas Krieg reviewed the manuscript and approved the final manuscript as submitted. Ulrich Heininger conceived the study, reviewed the manuscript and approved the final manuscript as submitted. Nicole Ritz conceived the study, supervised the analysis, reviewed and revised the manuscript and approved the final manuscript as submitted.
Corresponding author
Ethics declarations
Financial disclosure
The authors have no financial relationships relevant to this article to disclose.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval/informed consent
Due to the retrospective, descriptive study design, no patient consent was obtained. The study was approved by the ethics committee of North-West-Switzerland (EKBB, number 2014/184).
Additional information
Communicated by Piet Leroy
Ulrich Heininger and Nicole Ritz had shared authorship
Rights and permissions
About this article
Cite this article
Manz, N., Krieg, A.H., Heininger, U. et al. Evaluation of the current use of imaging modalities and pathogen detection in children with acute osteomyelitis and septic arthritis. Eur J Pediatr 177, 1071–1080 (2018). https://doi.org/10.1007/s00431-018-3157-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-018-3157-3